Level up to NP with online
Nurse Practitioner Courses
Created by NPs for NPs, Lecturio is your all-in-one companion for class prep, clinical rotations and exams.


- Master core clinical topics
- Pass your exams
- Smoothly transition to provider
Gain confidence for independent practice
with tailor-made NP courses
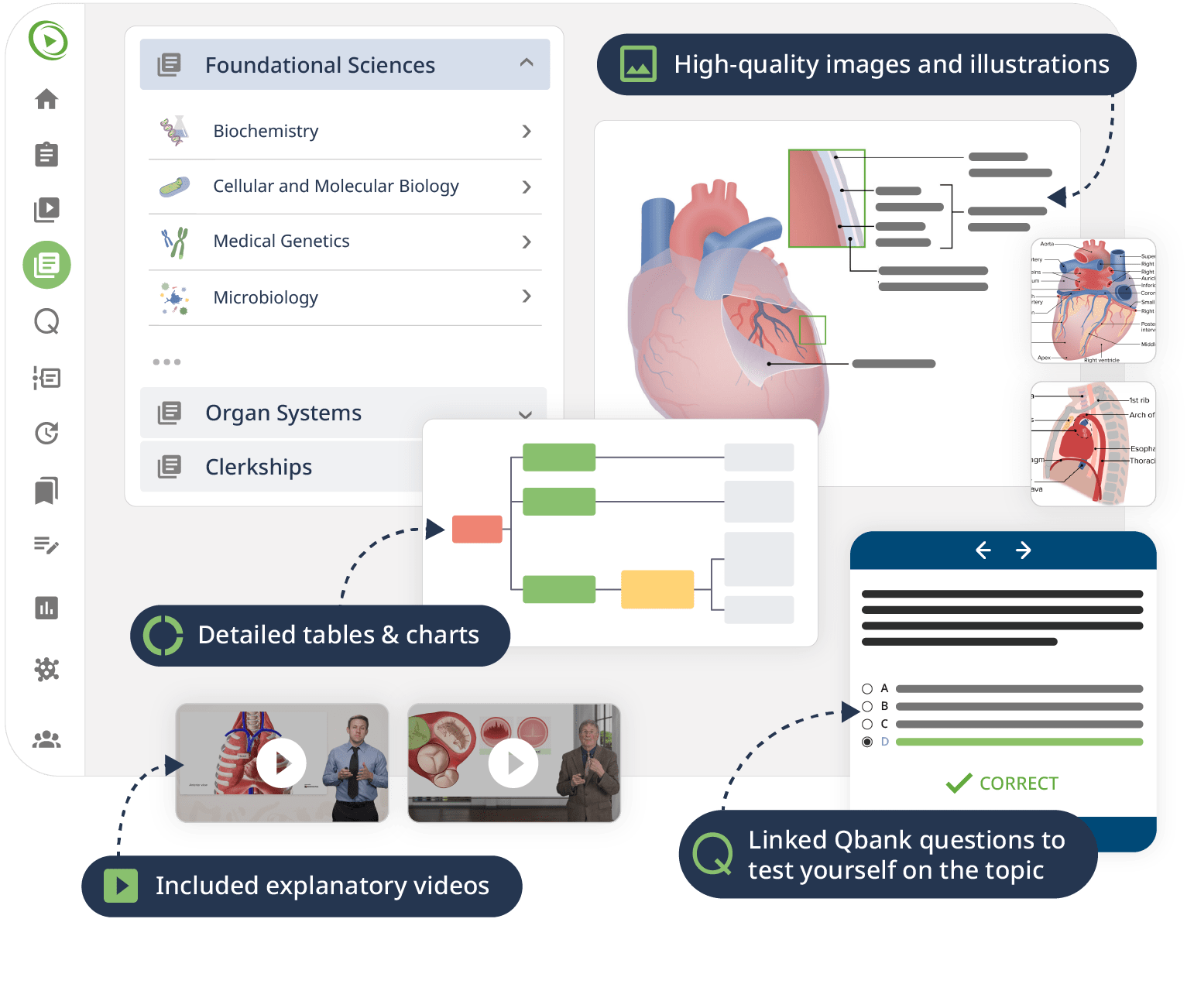
We cover all the topics that nurse practitioner students need to know
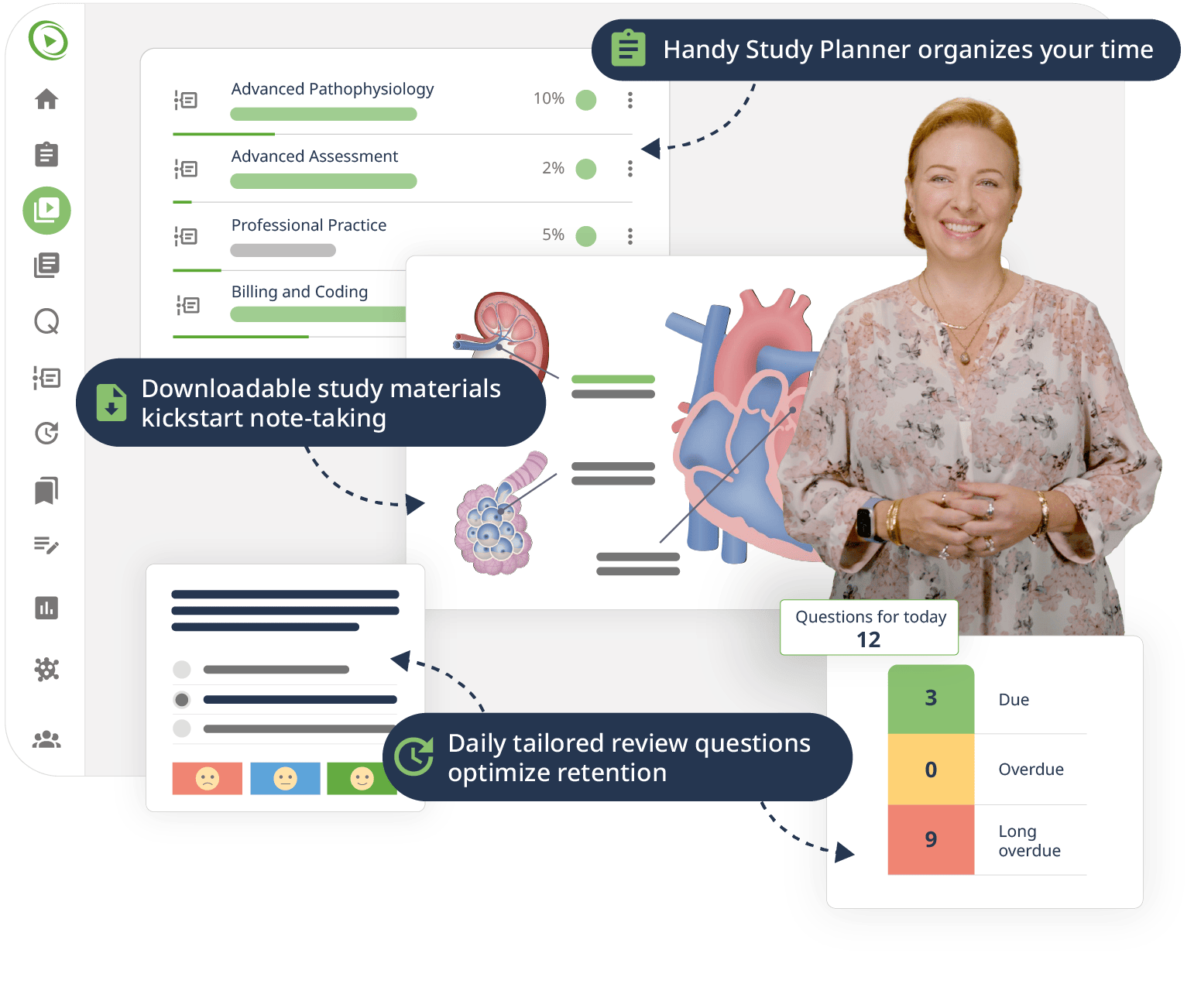
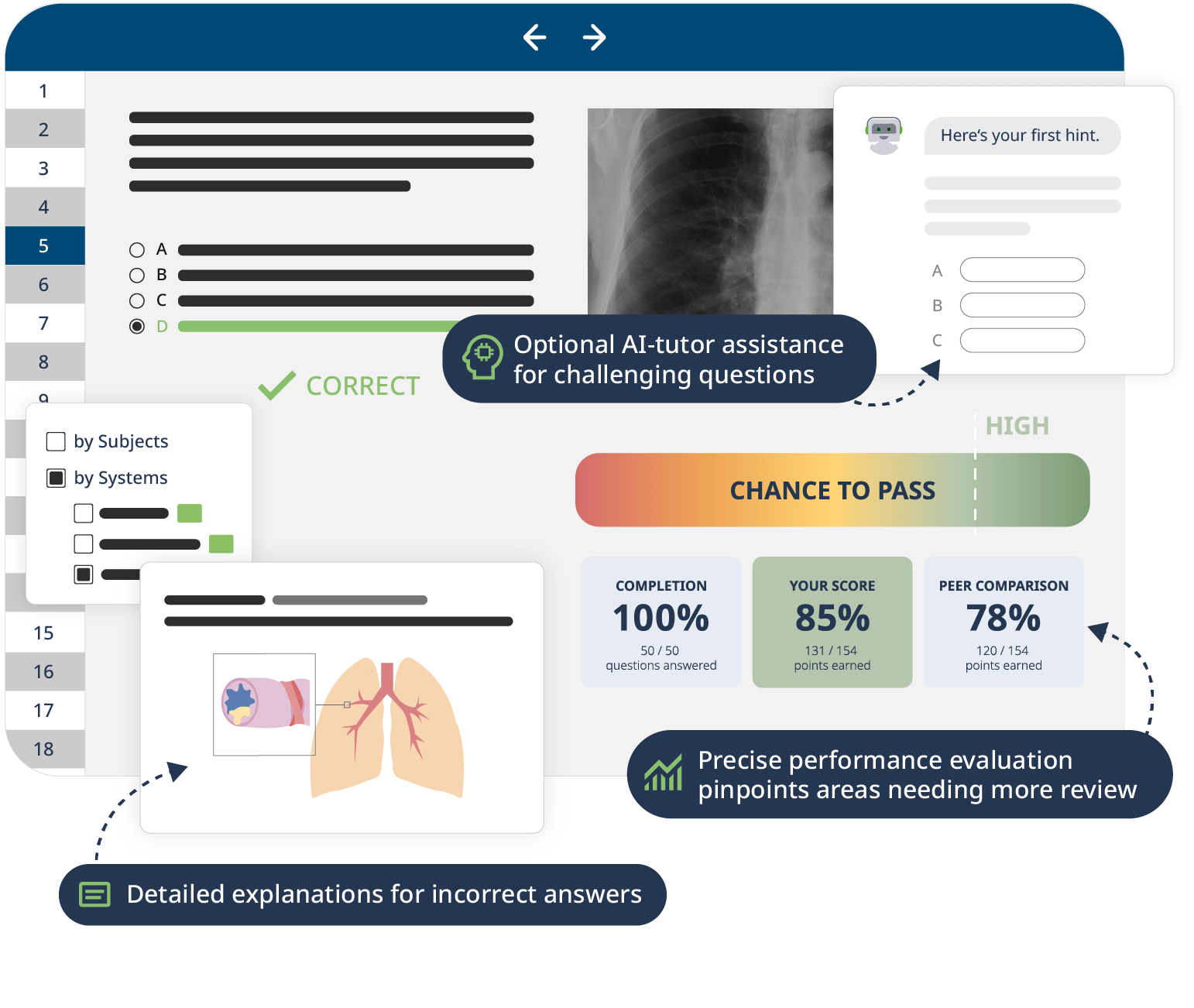
We streamline your study strategy with a set of smart learning tools built just for NP students



“I wish I'd discovered this site earlier. One of the biggest problems professors have in school is that they often forget that they're teaching people who don't already know the material. It can make what seems to the professor like a straightforward lecture into an unintelligible mess to their students. With Lecturio, I feel much better informed now, and I recommend this platform to everyone who felt like I did when listening to their school lectures.”
"Excellent review! I'm reviewing for my NP certification and this is a great resource."
Lean on our experience and guidance
Content created by nurse practitioners for nurse practitioners

Texas Christian University (TCU), USA

All Saints Medical Center, USA

Johns Hopkins University, USA

University of Birmingham, UK

Tucson, Arizona State University, USA

The Pathwayz Group

University of Washington, USA

Private practice

Rosalind Franklin University, USA

UCLA-affiliated hospital, USA

Georgia University, USA

University College London (UCL), UK

University of North Carolina, Chapel Hill, USA

LAC+USC Medical Center, Los Angeles, USA

Rush University, USA
Part of the platform is a dedicated video series filled with guidance and advice on becoming and practicing as Nurse Practitioner.
Including:
Liz Russ, FNP
Amy Howells, PhD, CPNP-AC/PC
David Warren, SRNA, NP

Join Lecturio Medical Today
First 7 Days Free
Medical Basic
Full library access
Videos + Concept Pages
without Qbank and smart exam prep features
Best exam & board prep
Medical Premium
Full library access
Videos + Concept Pages
Powerful Qbank
with AI-tutor + performance tracking
Structured study plans
Expert-built exam & board prep
AI Assistant
Get answers you can trust
Accredited Courses
starts at
$
299
Academic Diplomas and Certificates of Advanced Studies and single courses to earn formal ECTS credits
Medical Basic
Pay after 7 days, cancel anytime
Full library access
Videos + Concept Pages
without Qbank and smart exam prep features
Best exam & board prep
Medical Premium
Pay after 7 days, cancel anytime
Full library access
Videos + Concept Pages
Powerful Qbank
with AI-tutor + performance tracking
Structured study plans
Expert-built exam & board prep
AI Assistant
Get answers you can trust
Accredited Courses
starts at
$
299
Academic Diplomas and Certificates of Advanced Studies and single courses to earn formal ECTS credits
Medical Basic
Full library access
Videos + Concept Pages
without Qbank and smart exam prep features
Best exam & board prep
Medical Premium
Full library access
Videos + Concept Pages
Powerful Qbank
with AI-tutor + performance tracking
Structured study plans
Expert-built exam & board prep
AI Assistant
Get answers you can trust
Accredited Courses
starts at
$
299
Academic Diplomas and Certificates of Advanced Studies and single courses to earn formal ECTS credits
Medical Basic
Pay after 7 days, cancel anytime
Full library access
Videos + Concept Pages
without Qbank and smart exam prep features
Best exam & board prep
Medical Premium
Pay after 7 days, cancel anytime
Full library access
Videos + Concept Pages
Powerful Qbank
with AI-tutor + performance tracking
Structured study plans
Expert-built exam & board prep
AI Assistant
Get answers you can trust
Accredited Courses
starts at
$
299
Academic Diplomas and Certificates of Advanced Studies and single courses to earn formal ECTS credits
Medical Basic
Full library access
Videos + Concept Pages
without Qbank and smart exam prep features
Best exam & board prep
Medical Premium
Full library access
Videos + Concept Pages
Powerful Qbank
with AI-tutor + performance tracking
Structured study plans
Expert-built exam & board prep
AI Assistant
Get answers you can trust
Accredited Courses
starts at
$
299
Academic Diplomas and Certificates of Advanced Studies and single courses to earn formal ECTS credits
Medical Basic
Pay after 7 days, cancel anytime
Full library access
Videos + Concept Pages
without Qbank and smart exam prep features
Best exam & board prep
Medical Premium
Pay after 7 days, cancel anytime
Full library access
Videos + Concept Pages
Powerful Qbank
with AI-tutor + performance tracking
Structured study plans
Expert-built exam & board prep
AI Assistant
Get answers you can trust
Accredited Courses
starts at
$
299
Academic Diplomas and Certificates of Advanced Studies and single courses to earn formal ECTS credits
FAQs
RN vs NP: What is a nurse practitioner?
Registered nurses (RNs) are eligible to receive state licensure when successful on the NCLEX-RN national examination proctored by the National Council of State Boards of Nursing (NCSBN). Advanced practice registered nurses (APRNs) are eligible to receive state licensure when successful on a certification exam sponsored by an accrediting organization specific to the APRN track. NPs have a broader range of practice than RN, including diagnosing and treating illnesses, prescribing medications, and practicing with autonomy similar to that of a physician.
How to become a nurse practitioner
To transition from the role of RN to being an NP, you will need to pursue a graduate degree in nursing and choose a specialization. How long NP school takes depends on your previous qualifications and the number of clinical hours required. It may be between 2 and 4 years.
Lecturio has a full curriculum on the “three Ps of advanced practice academic preparation:” advanced pathophysiology, pharmacology, and physical assessment. Video Lessons, Concept Pages, Recall Quizzes, and Qbank items assist you to build a strong foundation for subsequent courses in primary care of families, adults, and geriatric populations.
Is this an NP board prep course?
The purpose of Lecturio’s NP curriculum is to provide students with support during their NP school program.
With Lecturio, you have access to over 3000 NP certification-style questions across the curriculum and over 3,100 Recall Quiz questions embedded within each video to help test knowledge and encourage repetition of major concepts, preparing you to be successful on your certification exams.
However, at this time, it is not designed to serve as a stand-alone board preparation program.
How does the medical content from Lecturio prepare me to be an Advanced Provider?
Advanced Practice Registered Nurses, Physician Assistants, and medical students are expected to acquire extensive knowledge of anatomy, pathophysiology, assessment, diagnosis, and treatment of disease. Lecturio’s curricula are designed to provide all advanced care providers with a strong foundation of medical knowledge.
I’m in an acute care NP program, is Lecturio a good fit for me?
In it’s entirety, Lecturio’s NP program best supports family nurse practitioners (FNPs) and adult gerontology primary care nurse practitioners (AGPCN). However, we do offer advanced pathophysiology, advanced pharmacology, and advanced health assessment courses that acute care nurse practitioner students take as well.
Can I try content for free?
You can register your Lecturio account for free, no obligations, no credit card required. Your free account gives you access to around 20% of the full content – no time limit. If you like, you can upgrade to a paid account with full access anytime. Additionally, our youtube channel has many examples of video lectures for you to browse and help you determine if Lecturio is a good fit for your education journey.



