Erythema Erythema Redness of the skin produced by congestion of the capillaries. This condition may result from a variety of disease processes. Chalazion infectiosum is an illness commonly identified by a characteristic rash Rash Rocky Mountain Spotted Fever; it is caused by parvovirus B19 Parvovirus B19 Primate erythroparvovirus 1 (generally referred to as parvovirus B19, B19 virus, or sometimes erythrovirus B19) ranks among the smallest DNA viruses. Parvovirus B19 is of the family Parvoviridae and genus Erythrovirus. In immunocompetent humans, parvovirus B19 classically results in erythema infectiosum (5th disease) or "slapped cheek syndrome." Parvovirus B19. Erythema Erythema Redness of the skin produced by congestion of the capillaries. This condition may result from a variety of disease processes. Chalazion infectiosum is also known as fifth disease, being 5th in the historical list of rash-causing childhood infectious diseases: measles Measles Measles (also known as rubeola) is caused by a single-stranded, linear, negative-sense RNA virus of the family Paramyxoviridae. It is highly contagious and spreads by respiratory droplets or direct-contact transmission from an infected person. Typically a disease of childhood, measles classically starts with cough, coryza, and conjunctivitis, followed by a maculopapular rash. Measles Virus (1st), scarlet fever Scarlet fever Infection with group a Streptococci that is characterized by tonsillitis and pharyngitis. An erythematous rash is commonly present. Scarlet Fever (2nd), rubella Rubella An acute infectious disease caused by the rubella virus. The virus enters the respiratory tract via airborne droplet and spreads to the lymphatic system. Rubella Virus (3rd), Dukes' disease (4th), and roseola (6th). Transmission is thought to be through contact with contaminated respiratory secretions. Diagnosis is generally clinical, suspected in patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship presenting with an erythematous malar rash Malar Rash Systemic Lupus Erythematosus with circumoral pallor (“slapped cheek”). A rash Rash Rocky Mountain Spotted Fever over the trunk and extremities occurs afterward. The illness is self-limited and has no specific therapy. Complications can occur, however, due to the viral tropism for erythrocyte precursors. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship with hemoglobinopathies Hemoglobinopathies A group of inherited disorders characterized by structural alterations within the hemoglobin molecule. Anemia: Overview and Types can experience aplastic crisis, while the immunocompromised immunocompromised A human or animal whose immunologic mechanism is deficient because of an immunodeficiency disorder or other disease or as the result of the administration of immunosuppressive drugs or radiation. Gastroenteritis may have chronic infection producing pure red cell aplasia Aplasia Cranial Nerve Palsies.
Last updated: Dec 28, 2024
The incubation Incubation The amount time between exposure to an infectious agent and becoming symptomatic. Rabies Virus period is 4–21 days.
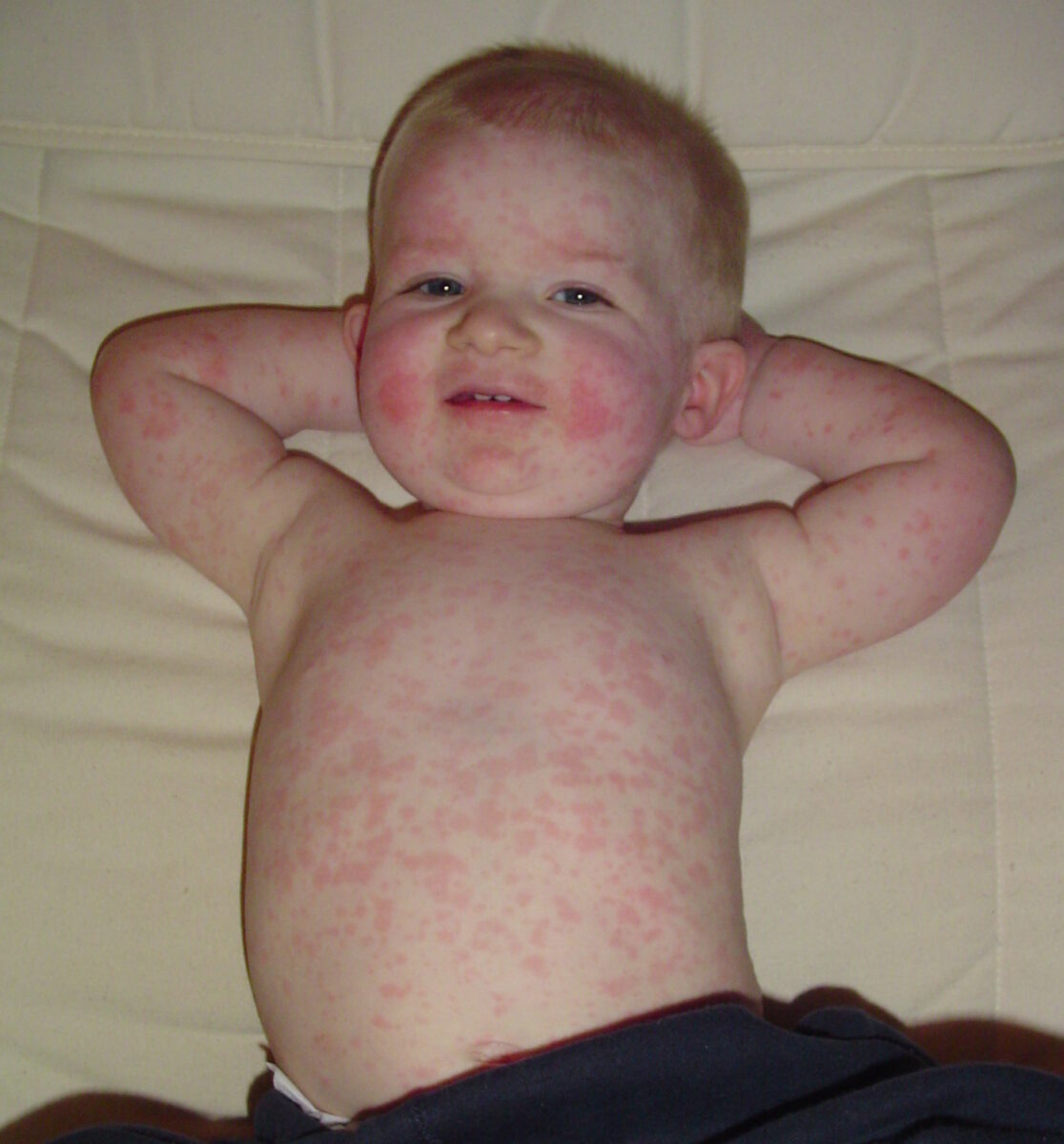
Pediatric patient with fifth disease: erythematous facial rash accompanied by rash on the torso and extremities
Image: “Fifth disease” by Andrew Kerr. License: Public Domain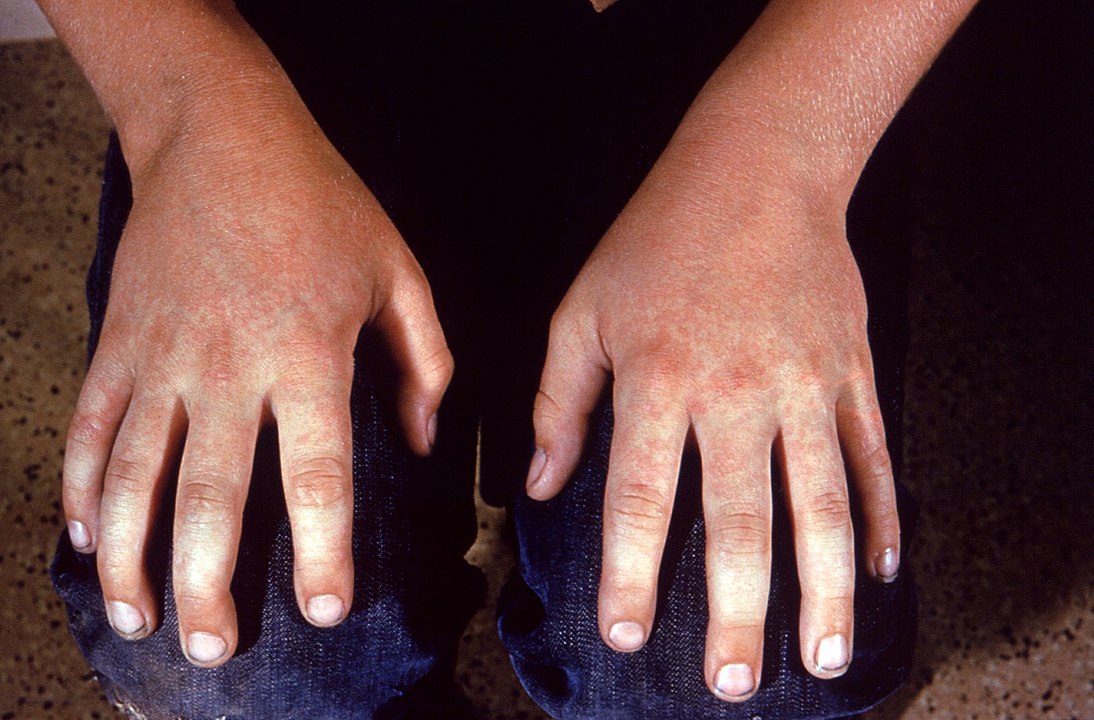
Erythema infectiosum: rash on the extremities
Image: “Fifth disease symptoms” by CDC. License: Public Domain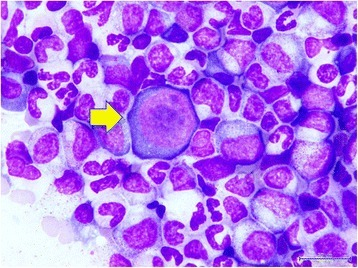
Transient aplastic crisis in parvovirus B19 infection
Image shows bone marrow cytology. Yellow arrow indicates a giant pronormoblast.
| Number | Other names for the disease | Etiology | Description |
|---|---|---|---|
| 1st disease 1st disease Measles (also known as rubeola) is caused by a single-stranded, linear, negative-sense RNA virus of the family Paramyxoviridae. It is highly contagious and spreads by respiratory droplets or direct-contact transmission from an infected person. Typically a disease of childhood, measles classically starts with cough, coryza, and conjunctivitis, followed by a maculopapular rash. Measles Virus |
|
Measles Measles Measles (also known as rubeola) is caused by a single-stranded, linear, negative-sense RNA virus of the family Paramyxoviridae. It is highly contagious and spreads by respiratory droplets or direct-contact transmission from an infected person. Typically a disease of childhood, measles classically starts with cough, coryza, and conjunctivitis, followed by a maculopapular rash. Measles Virus morbillivirus Morbillivirus A genus of the family paramyxoviridae (subfamily paramyxovirinae) where the virions of most members have hemagglutinin but not neuraminidase activity. All members produce both cytoplasmic and intranuclear inclusion bodies. Measles virus is the type species. Measles Virus |
|
| 2nd disease |
|
Streptococcus Streptococcus Streptococcus is one of the two medically important genera of gram-positive cocci, the other being Staphylococcus. Streptococci are identified as different species on blood agar on the basis of their hemolytic pattern and sensitivity to optochin and bacitracin. There are many pathogenic species of streptococci, including S. pyogenes, S. agalactiae, S. pneumoniae, and the viridans streptococci. Streptococcus pyogenes |
|
| 3rd disease 3rd disease An acute infectious disease caused by the rubella virus. The virus enters the respiratory tract via airborne droplet and spreads to the lymphatic system. Rubella Virus |
|
Rubella Rubella An acute infectious disease caused by the rubella virus. The virus enters the respiratory tract via airborne droplet and spreads to the lymphatic system. Rubella Virus virus Virus Viruses are infectious, obligate intracellular parasites composed of a nucleic acid core surrounded by a protein capsid. Viruses can be either naked (non-enveloped) or enveloped. The classification of viruses is complex and based on many factors, including type and structure of the nucleoid and capsid, the presence of an envelope, the replication cycle, and the host range. Virology |
|
| 4th disease |
|
Due to Staphylococcus aureus Staphylococcus aureus Potentially pathogenic bacteria found in nasal membranes, skin, hair follicles, and perineum of warm-blooded animals. They may cause a wide range of infections and intoxications. Brain Abscess strains that make epidermolytic (exfoliative) toxin |
|
| 5th disease | Erythema Erythema Redness of the skin produced by congestion of the capillaries. This condition may result from a variety of disease processes. Chalazion infectiosum | Erythrovirus or parvovirus B19 Parvovirus B19 Primate erythroparvovirus 1 (generally referred to as parvovirus B19, B19 virus, or sometimes erythrovirus B19) ranks among the smallest DNA viruses. Parvovirus B19 is of the family Parvoviridae and genus Erythrovirus. In immunocompetent humans, parvovirus B19 classically results in erythema infectiosum (5th disease) or “slapped cheek syndrome.” Parvovirus B19 (Primate erythroparvovirus Erythroparvovirus Parvovirus B19 1) |
|
| 6th disease |
|
Human herpesvirus 6B or human herpesvirus 7 |
|