Melasma is a benign Benign Fibroadenoma skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions condition characterized by hyperpigmentation Hyperpigmentation Excessive pigmentation of the skin, usually as a result of increased epidermal or dermal melanin pigmentation, hypermelanosis. Hyperpigmentation can be localized or generalized. The condition may arise from exposure to light, chemicals or other substances, or from a primary metabolic imbalance. Malassezia Fungi of sun-exposed regions due to excess melanin Melanin Insoluble polymers of tyrosine derivatives found in and causing darkness in skin (skin pigmentation), hair, and feathers providing protection against sunburn induced by sunlight. Carotenes contribute yellow and red coloration. Seborrheic Keratosis production and deposition. The condition mainly affects women during their reproductive years, particularly those with darker skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions tones. Hyperpigmented patches Patches Vitiligo typically occur on the face, especially the cheeks, chin, forehead, and upper lip. The diagnosis is clinical. Management includes sun protection and topical depigmenting agents.
Last updated: Nov 24, 2024
Melasma, also known as chloasma, is a benign Benign Fibroadenoma condition of the skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions characterized by hyperpigmentation Hyperpigmentation Excessive pigmentation of the skin, usually as a result of increased epidermal or dermal melanin pigmentation, hypermelanosis. Hyperpigmentation can be localized or generalized. The condition may arise from exposure to light, chemicals or other substances, or from a primary metabolic imbalance. Malassezia Fungi in sun-exposed areas.
Hyperactive melanocytes Melanocytes Mammalian pigment cells that produce melanins, pigments found mainly in the epidermis, but also in the eyes and the hair, by a process called melanogenesis. Coloration can be altered by the number of melanocytes or the amount of pigment produced and stored in the organelles called melanosomes. The large non-mammalian melanin-containing cells are called melanophores. Skin: Structure and Functions deposit excess melanin Melanin Insoluble polymers of tyrosine derivatives found in and causing darkness in skin (skin pigmentation), hair, and feathers providing protection against sunburn induced by sunlight. Carotenes contribute yellow and red coloration. Seborrheic Keratosis in the epidermis Epidermis The external, nonvascular layer of the skin. It is made up, from within outward, of five layers of epithelium: (1) basal layer (stratum basale epidermidis); (2) spinous layer (stratum spinosum epidermidis); (3) granular layer (stratum granulosum epidermidis); (4) clear layer (stratum lucidum epidermidis); and (5) horny layer (stratum corneum epidermidis). Skin: Structure and Functions and dermis Dermis A layer of vascularized connective tissue underneath the epidermis. The surface of the dermis contains innervated papillae. Embedded in or beneath the dermis are sweat glands; hair follicles; and sebaceous glands. Skin: Structure and Functions of the skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions.
Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship develop hyperpigmented lesions.
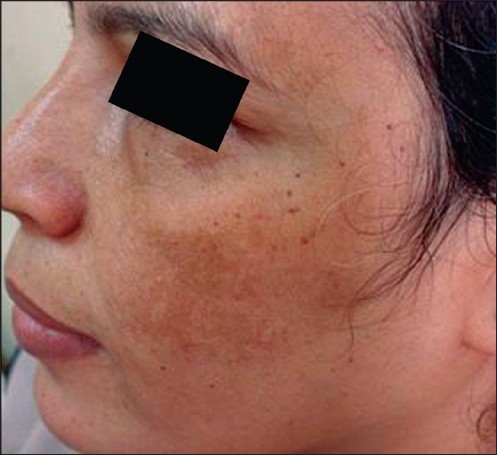
Hyperpigmentation on the cheeks due to melasma
Image: “A study comparing chemical peeling using modified Jessner’s solution and 15% trichloroacetic Acid versus 15% trichloroacetic acid in the treatment of melasma” by Safoury OS, Zaki NM, El Nabarawy EA, Farag EA. License: CC BY 2.0
Hyperpigmentation on the cheeks of a patient with melasma
Image: “A study comparing chemical peeling using modified Jessner’s solution and 15% trichloroacetic Acid versus 15% trichloroacetic acid in the treatment of melasma” by Safoury OS, Zaki NM, El Nabarawy EA, Farag EA. License: CC BY 2.0The diagnosis of melasma is clinical.