Enterobiasis is a helminth infection caused by Enterobius vermicularis, also known as a pinworm. This infection is typically seen in children and is transmitted through the fecal–oral route. The primary clinical feature is anal pruritus Pruritus An intense itching sensation that produces the urge to rub or scratch the skin to obtain relief. Atopic Dermatitis (Eczema), but patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship are often asymptomatic. Visualization of ova or worms on cellophane tape testing is often required for diagnosis. Anthelmintic medications are used for treatment. Prevention of reinfection and transmission requires frequent handwashing and bathing, as well as washing of clothes and linens.
Last updated: Dec 15, 2025
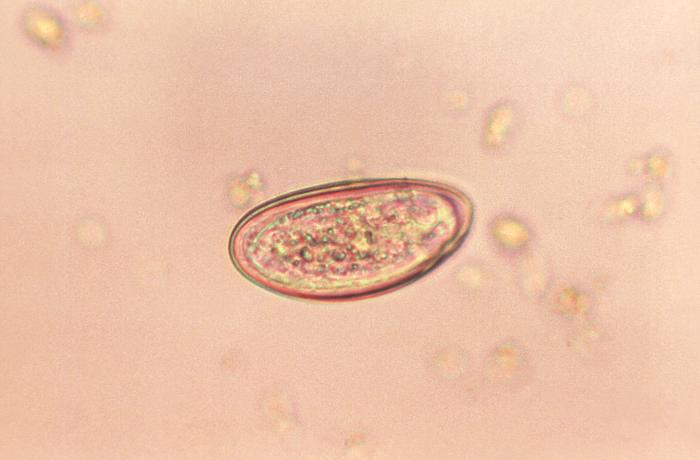
An Enterobius egg
Image: “Photomicrograph of an Enterobius vermicularis egg” by CDC. License: Public Domain
Posterior end of an Enterobius vermicularis adult worm
Image: “Posterior end of an Enterobius vermicularis adult worm” by Division of Parasitic Diseases and Malaria (DPDM). License: Public Domain
2 adult Enterobius vermicularis worms
Image: “Enterobius vermicularis or pinworm parasite” by Erich. License: Public DomainEnterobius vermicularis, or pinworm, causes enterobiasis.
Enterobiasis is the most common helminth infection in the United States and Western Europe.
Humans are the primary hosts of E. vermicularis.
The entire life cycle of E. vermicularis takes place in the human GI tract and lasts 2‒8 weeks.
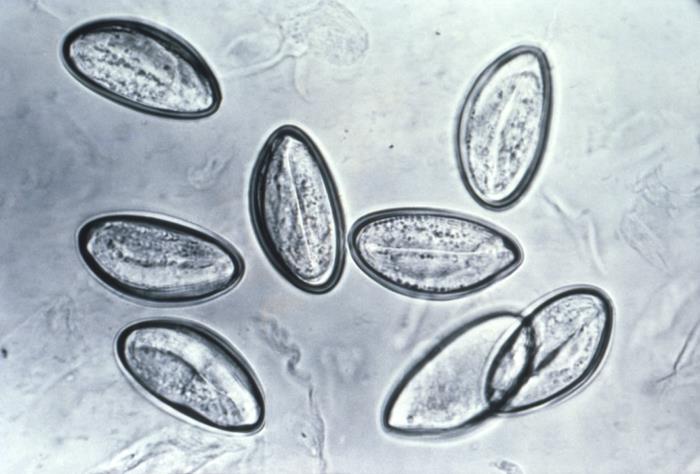
Photomicrograph of 8 Enterobius vermicularis eggs on cellophane tape
Image: Photomicrograph depicts eight eggs of the human pinworm, Enterobius vermicularis” by CDC. License: Public DomainMedical therapy:
Measures to reduce reinfection and spread:
| Organism | Enterobius vermicularis | Toxocara canis Toxocara canis A species of parasitic nematode found in the intestine of dogs. Lesions in the brain, liver, eye, kidney, and lung are caused by migrating larvae. In humans, these larvae do not follow normal patterns and may produce visceral larva migrans (larva migrans, visceral). Toxocariasis | Ascaris Ascaris Ascaris is a genus of parasitic nematodes. The infection, ascariasis, is most often caused by A. lumbricoides. Transmission occurs primarily via ingestion of water or food contaminated with Ascaris eggs. Most patients with ascariasis are asymptomatic. Ascaris/Ascariasis lumbricoides | Strongyloides stercoralis Strongyloides stercoralis A species of parasitic nematode widely distributed in tropical and subtropical countries. The females and their larvae inhabit the mucosa of the intestinal tract, where they cause ulceration and diarrhea. Strongyloidiasis | Schistosoma Schistosoma Schistosomiasis is an infection caused by Schistosoma, a trematode. Schistosomiasis occurs in developing countries with poor sanitation. Freshwater snails are the intermediate host and are transmitted to humans through skin contact with contaminated fresh water. The clinical presentation occurs as a result of the host’s immune response to antigens from the eggs. Schistosoma/Schistosomiasis mansoni |
|---|---|---|---|---|---|
| Characteristics | Nematode Nematode A phylum of unsegmented helminths with fundamental bilateral symmetry and secondary triradiate symmetry of the oral and esophageal structures. Many species are parasites. Toxocariasis | Nematode Nematode A phylum of unsegmented helminths with fundamental bilateral symmetry and secondary triradiate symmetry of the oral and esophageal structures. Many species are parasites. Toxocariasis | Nematode Nematode A phylum of unsegmented helminths with fundamental bilateral symmetry and secondary triradiate symmetry of the oral and esophageal structures. Many species are parasites. Toxocariasis | Nematode Nematode A phylum of unsegmented helminths with fundamental bilateral symmetry and secondary triradiate symmetry of the oral and esophageal structures. Many species are parasites. Toxocariasis | Trematode Trematode Class of parasitic flukes consisting of three subclasses, monogenea, aspidogastrea, and digenea. The digenetic trematodes are the only ones found in man. They are endoparasites and require two hosts to complete their life cycle. Schistosoma/Schistosomiasis |
| Reservoir Reservoir Animate or inanimate sources which normally harbor disease-causing organisms and thus serve as potential sources of disease outbreaks. Reservoirs are distinguished from vectors (disease vectors) and carriers, which are agents of disease transmission rather than continuing sources of potential disease outbreaks. Humans may serve both as disease reservoirs and carriers. Escherichia coli | Humans | Dogs | Humans |
|
Humans |
| Transmission | Fecal–oral | Fecal–oral | Fecal–oral | Skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions contact with contaminated soil | Skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions contact with contaminated water |
| Clinical |
|
|
|
|
|
| Diagnosis |
|
|
Stool analysis |
|
|
| Management |
|
|
|
|
Praziquantel Praziquantel An anthelmintic used in most schistosome and many cestode infestations. Anthelmintic Drugs |
| Prevention | Good hygiene |
|
|
|
|
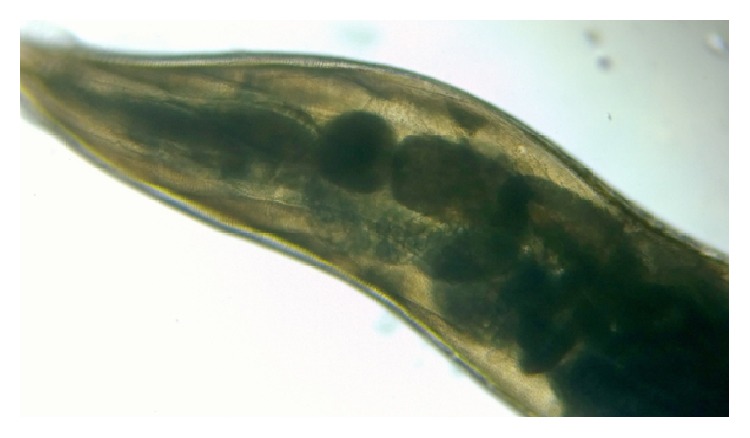
Low-power microscopic view of Enterobius vermicularis
Image: “Double bulb oesophagus of Enterobius vermicularis, under low power” by Kaniyarakkal V et al. License: CC BY 4.0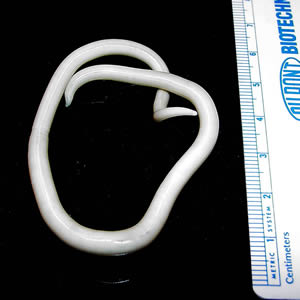
An adult Ascaris lumbricoides worm
Image: “An adult Ascaris lumbricoides worm” by CDC Division of Parasitic Diseases. License: Public Domain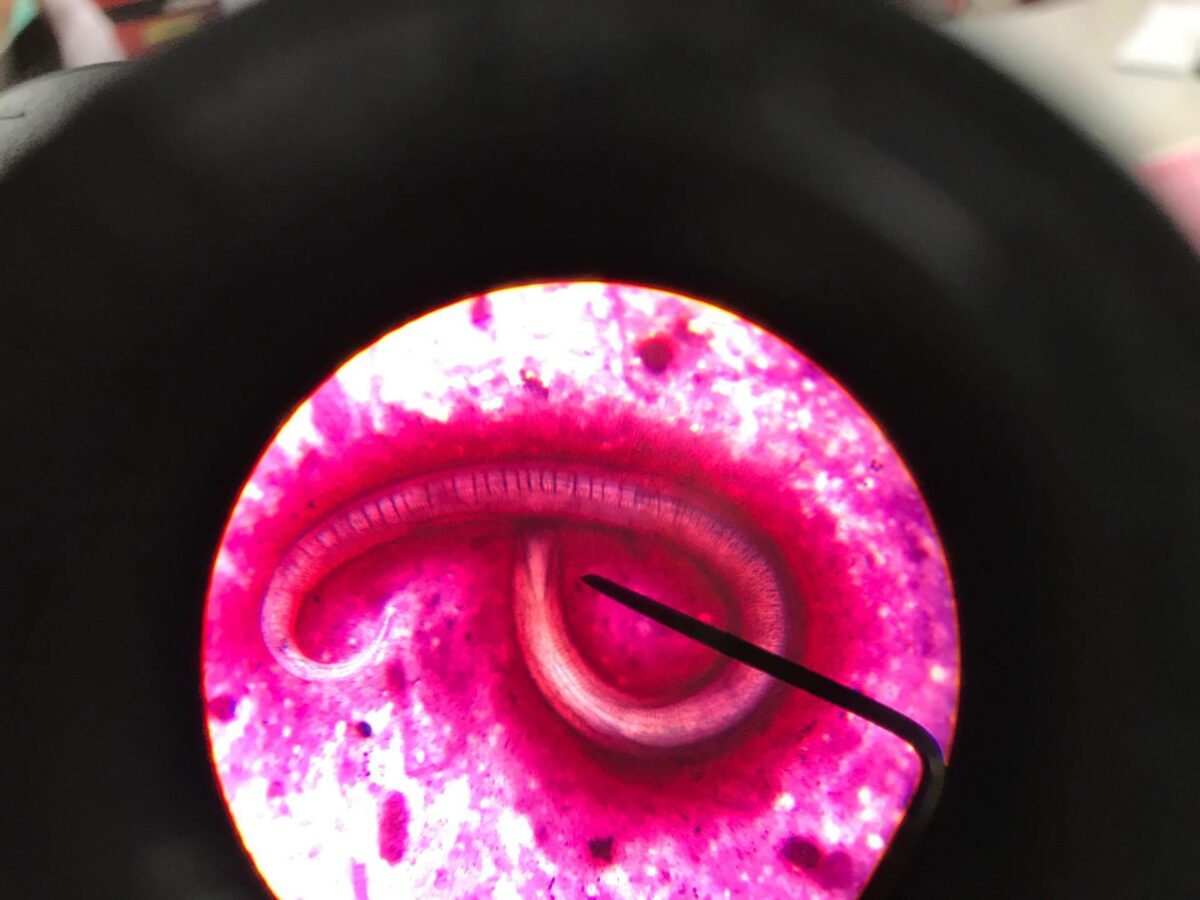
Strongyloides stercoralis parasite
Image: “Strongyloides Stercoralis in sputum” by CDC Division of Parasitic Diseases. License: CC BY 4.0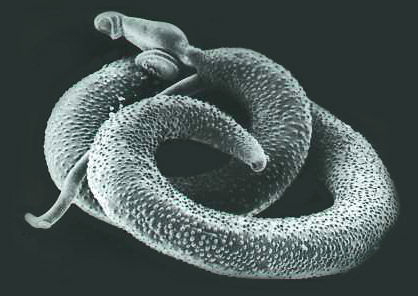
An adult Schistosoma mansoni seen on electron microscopy
Image: “Schistosoma mansoni, adult. SEM [Scanning electron microscopy] of worm, unstained” by Otis Historical Archives of “National Museum of Health & Medicine”. License: CC BY 2.0