Nuclear imaging is the radiologic examination using radiopharmaceuticals, which are radioactive substances taken up by specific types of cells. Nuclear medicine is more concerned with the functional and molecular aspects of the organ or pathology being investigated rather than the structure. Radiopharmaceuticals are administered to the patient and in vivo distribution is recorded. Nuclear imaging has been widely used to diagnose and follow up certain diseases. Multiple organ systems can be evaluated, including the cardiovascular system, where ischemia Ischemia A hypoperfusion of the blood through an organ or tissue caused by a pathologic constriction or obstruction of its blood vessels, or an absence of blood circulation. Ischemic Cell Damage is detected; endocrine system, where thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy activity is evaluated; hepatobiliary system, where cystic Cystic Fibrocystic Change duct obstruction can be seen; and skeletal system where tumors/ metastasis Metastasis The transfer of a neoplasm from one organ or part of the body to another remote from the primary site. Grading, Staging, and Metastasis or fractures are localized.
Last updated: Dec 15, 2025
Equipment:
Imaging techniques:
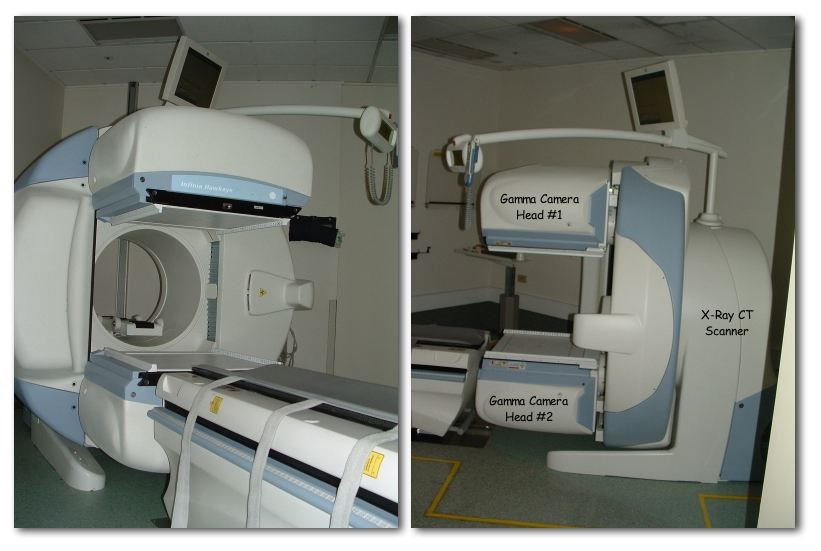
A SPECT/CT system with relevant components labeled in the photograph on the right
Image: “NM19 290” by Kieran Maher. License: Public Domain| Imaging finding | Interpretation |
|---|---|
| Bile Bile An emulsifying agent produced in the liver and secreted into the duodenum. Its composition includes bile acids and salts; cholesterol; and electrolytes. It aids digestion of fats in the duodenum. Gallbladder and Biliary Tract: Anatomy ducts visible | Normal hepatic function |
| Filling of the gallbladder Gallbladder The gallbladder is a pear-shaped sac, located directly beneath the liver, that sits on top of the superior part of the duodenum. The primary functions of the gallbladder include concentrating and storing up to 50 mL of bile. Gallbladder and Biliary Tract: Anatomy | Patent cystic Cystic Fibrocystic Change duct |
| Radiotracer is seen in the duodenum Duodenum The shortest and widest portion of the small intestine adjacent to the pylorus of the stomach. It is named for having the length equal to about the width of 12 fingers. Small Intestine: Anatomy | Patent common bile Bile An emulsifying agent produced in the liver and secreted into the duodenum. Its composition includes bile acids and salts; cholesterol; and electrolytes. It aids digestion of fats in the duodenum. Gallbladder and Biliary Tract: Anatomy duct |
| No radiotracer is seen in the gallbladder Gallbladder The gallbladder is a pear-shaped sac, located directly beneath the liver, that sits on top of the superior part of the duodenum. The primary functions of the gallbladder include concentrating and storing up to 50 mL of bile. Gallbladder and Biliary Tract: Anatomy | Obstructed gallbladder Gallbladder The gallbladder is a pear-shaped sac, located directly beneath the liver, that sits on top of the superior part of the duodenum. The primary functions of the gallbladder include concentrating and storing up to 50 mL of bile. Gallbladder and Biliary Tract: Anatomy ( acute cholecystitis Acute cholecystitis Acute inflammation of the gallbladder wall. It is characterized by the presence of abdominal pain; fever; and leukocytosis. Gallstone obstruction of the cystic duct is present in approximately 90% of the cases. Cholecystitis) |
| No radiotracer is seen in the duodenum Duodenum The shortest and widest portion of the small intestine adjacent to the pylorus of the stomach. It is named for having the length equal to about the width of 12 fingers. Small Intestine: Anatomy | Biliary atresia Atresia Hypoplastic Left Heart Syndrome (HLHS) |
| Radiotracer outside the biliary system | Biliary leak |

Hepatobiliary iminodiacetic acid scan
Image by Lecturio.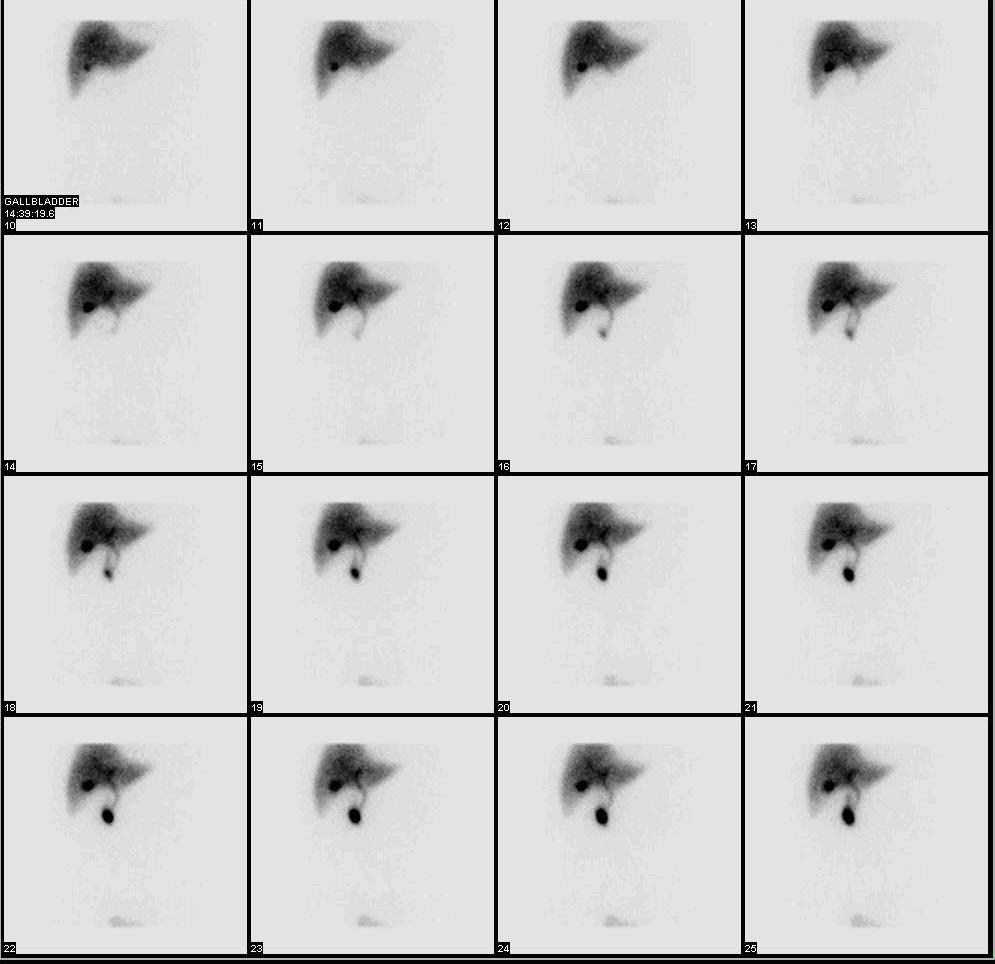
Normal hepatobiliary iminodiacetic acid scan showing the radioactive substance moving through the biliary system
Image: “HIDA” by Myohan. License: CC BY 3.0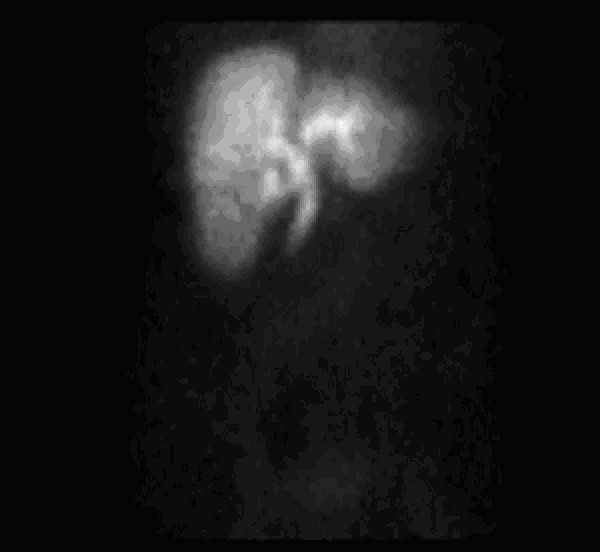
Hepatobiliary iminodiacetic acid scan in a patient with gallbladder pathology:
Demonstration of uptake of tracer in liver without visualization of the gallbladder. Delayed images show excretion of tracer into the small bowel.
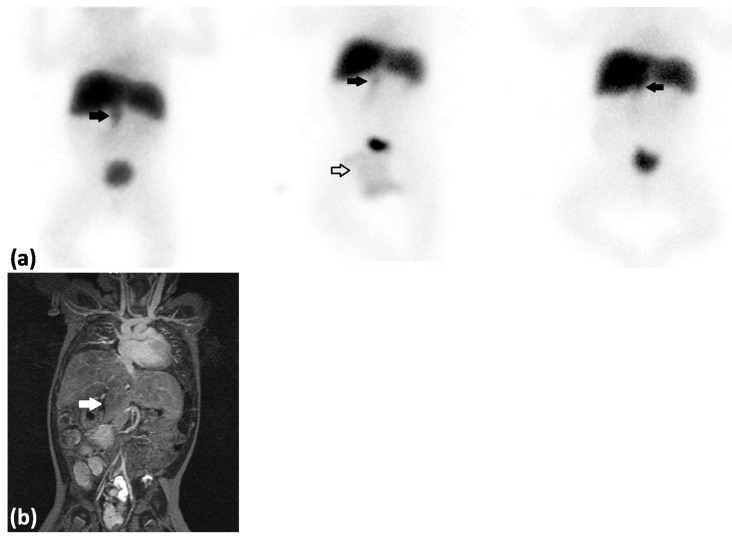
(a) Cholescintigraphy anterior view: left: 52–56 min after tracer injection; middle: 2 hours after tracer injection; right: 5 hours after tracer injection. Biliary atresia (BA) was suspected and the patient was referred for a technetium-99m trimethyl bromo-iminodiacetic acid hepatobiliary scintigraphy (99mTc-mebrofenin hepatobiliary scintigraphy), which showed rapid extraction of tracer by the liver with no excretion to the small bowel but with suspicion of visualization of the gallbladder (thick black arrows). The tracer was physiologically excreted in the urine and localized in a diaper (white arrow).
(b) MRI, coronal view (T2 weighted), demonstrating that the liver is separated into several lobes, indicating a false positive on the hepatobiliary iminodiacetic acid scan for gallbladder visualization. This was a confirmed case of biliary atresia.
| Category | Findings |
|---|---|
| High probability Probability Probability is a mathematical tool used to study randomness and provide predictions about the likelihood of something happening. There are several basic rules of probability that can be used to help determine the probability of multiple events happening together, separately, or sequentially. Basics of Probability of pulmonary embolism Pulmonary Embolism Pulmonary embolism (PE) is a potentially fatal condition that occurs as a result of intraluminal obstruction of the main pulmonary artery or its branches. The causative factors include thrombi, air, amniotic fluid, and fat. In PE, gas exchange is impaired due to the decreased return of deoxygenated blood to the lungs. Pulmonary Embolism | More than 2 large mismatched segmental defects |
| Intermediate probability Probability Probability is a mathematical tool used to study randomness and provide predictions about the likelihood of something happening. There are several basic rules of probability that can be used to help determine the probability of multiple events happening together, separately, or sequentially. Basics of Probability of pulmonary embolism Pulmonary Embolism Pulmonary embolism (PE) is a potentially fatal condition that occurs as a result of intraluminal obstruction of the main pulmonary artery or its branches. The causative factors include thrombi, air, amniotic fluid, and fat. In PE, gas exchange is impaired due to the decreased return of deoxygenated blood to the lungs. Pulmonary Embolism |
|
| Low probability Probability Probability is a mathematical tool used to study randomness and provide predictions about the likelihood of something happening. There are several basic rules of probability that can be used to help determine the probability of multiple events happening together, separately, or sequentially. Basics of Probability for pulmonary embolism Pulmonary Embolism Pulmonary embolism (PE) is a potentially fatal condition that occurs as a result of intraluminal obstruction of the main pulmonary artery or its branches. The causative factors include thrombi, air, amniotic fluid, and fat. In PE, gas exchange is impaired due to the decreased return of deoxygenated blood to the lungs. Pulmonary Embolism |
|
| Normal | No matched or mismatched defects |

Normal pulmonary ventilation and perfusion (VQ) scan. The nuclear medicine VQ scan is useful in the evaluation of pulmonary embolism.
Image: “Ventperf” by Myohan. License: CC BY 3.0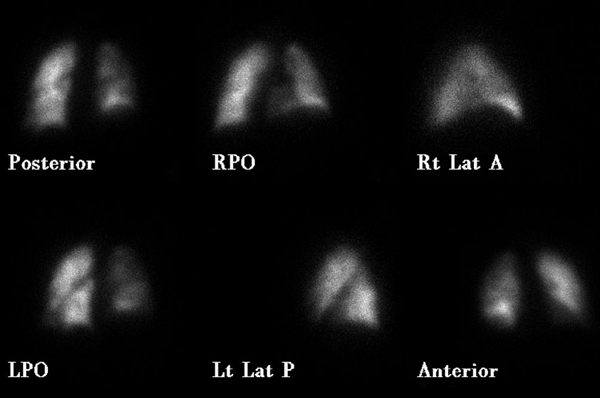
High probability for pulmonary embolism:
Decreased perfusion is seen to the right lung and is particularly evident in the right lower lobe on the right posterior oblique (RPO) image (perfusion scan was performed using Tc-99m macroaggregated albumin).
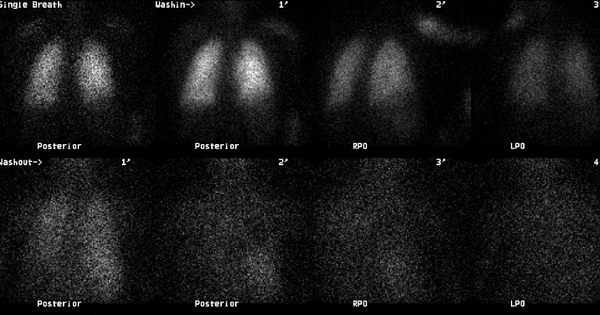
High probability for pulmonary embolism:
No significant ventilation defect (ventilation scan performed using Xe-133 gas)
High probability for pulmonary embolism:
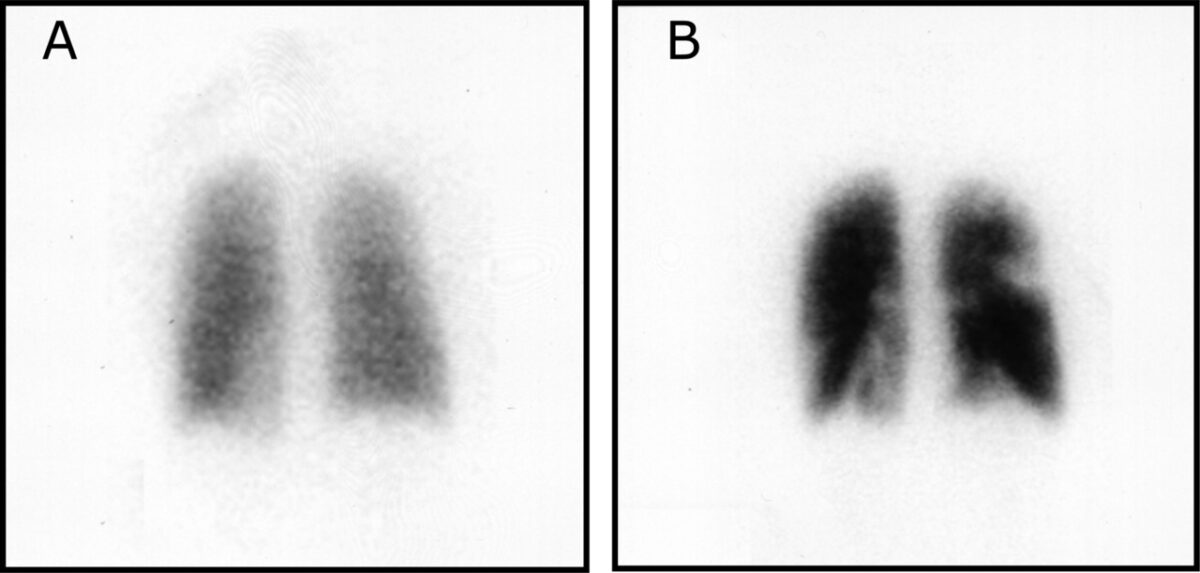
Ventilation-perfusion scintigraphy in a woman taking oral contraceptives and valdecoxib
A: Ventilation phase: uniform ventilation to lungs
B: Perfusion phase: This and other views show decreased activity in the apical segment of right upper lobe, anterior segment of right upper lobe, superior segment of right lower lobe, posterior basal segment of right lower lobe, anteromedial basal segment of left lower lobe, and lateral basal segment of left lower lobe.
| Results | Description | Accuracy | Examples |
|---|---|---|---|
| Normal |
|
True negative | False negative False negative An FN test result indicates a person does not have the disease when, in fact, they do. Epidemiological Values of Diagnostic Tests |
| Normal skeleton | Purely lytic metastasis Metastasis The transfer of a neoplasm from one organ or part of the body to another remote from the primary site. Grading, Staging, and Metastasis | ||
| Abnormal | Asymmetric increased uptake | True positive | False positive False positive An FP test result indicates that a person has the disease when they do not. Epidemiological Values of Diagnostic Tests |
|
|
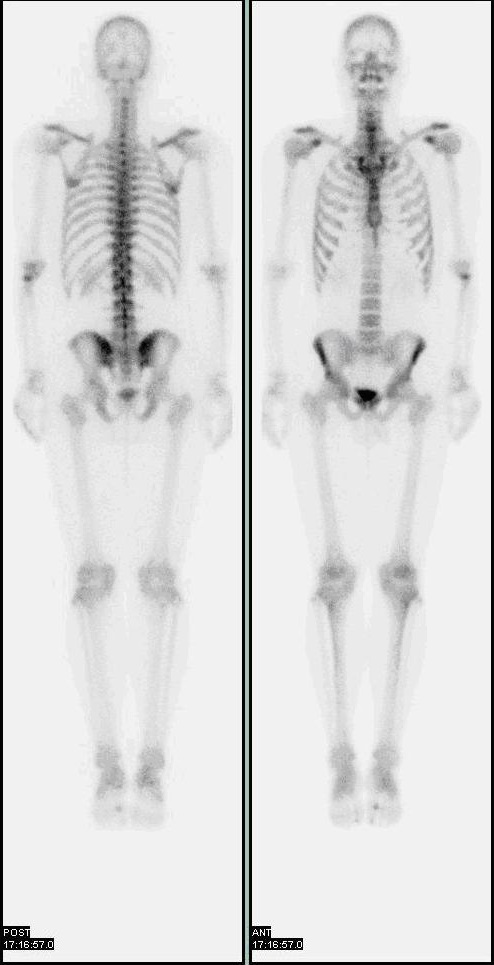
Normal bone scan with 2 views and no asymmetric increased uptake
Image: “Nl bone scan2” by Myohan. License: CC BY 3.0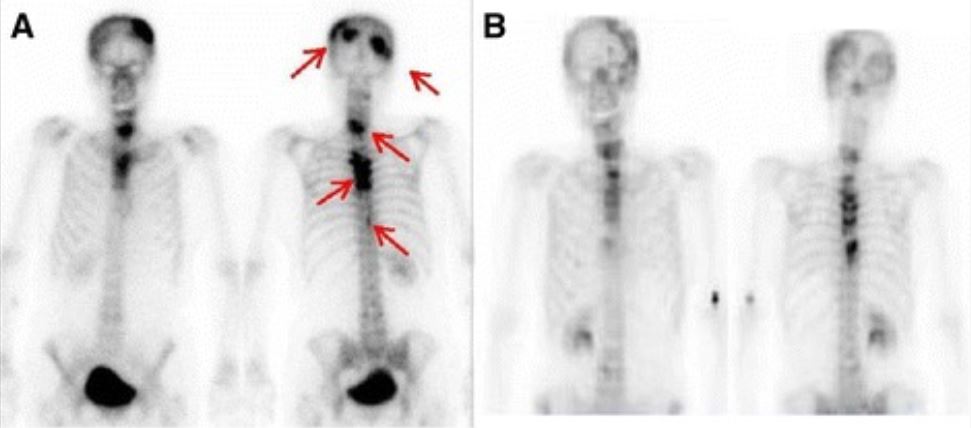
A: Bone scintigraphy during interferon-α treatment: Multiple bone metastases are visible (red arrows).
B: Bone scintigraphy at present state: Abnormal accumulations are less visible.
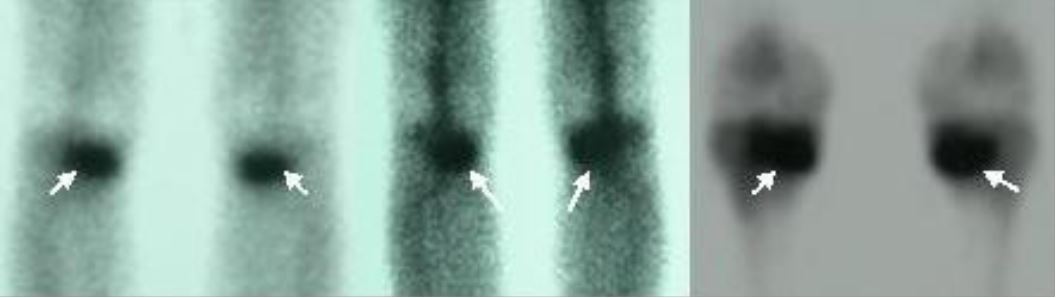
Oval-shaped increased osteoblastic activity on the metaphyseal region of both tibias (arrows) (stress fractures due to marathon running)
Image: “Stress fracture of bilateral tibial metaphysis due to ceremonial march training: A case report” by Kurklu M, Ozboluk S, Kilic E, Tatar O, Ozkan H, Basbozkurt M. License: CC BY 2.0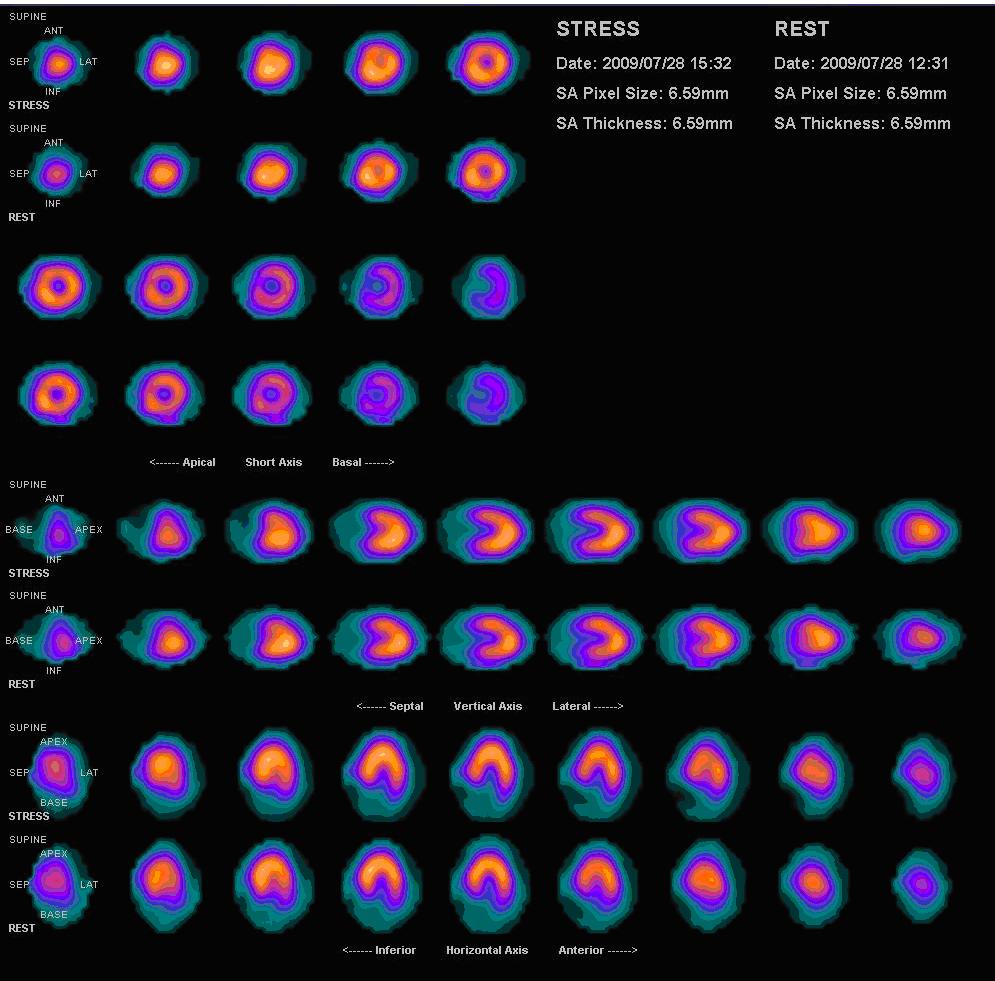
Normal myocardial perfusion scan with thallium-201 for the rest images (bottom rows) and technetium-sestamibi for the stress images (top rows)
Image: “Nl mpi2” by Myohan. License: CC BY 3.0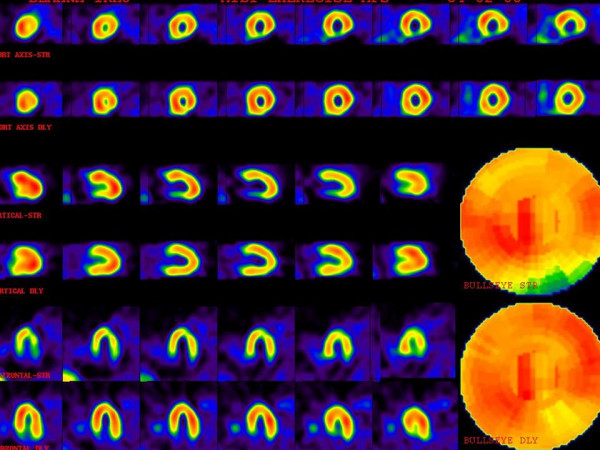
A patient with multiple perfusion defects with different degrees of severity.
The upper images are stress phase and lower images are rest or delayed images. There is moderate ischemia in the mid anterolateral and mid inferolateral walls.
There also is severe ischemia in the basal inferior wall. Mild ischemia in the apex, apical septal, and basal anterolateral regions are also noted.
| Uptake | Pattern | Diagnosis |
|---|---|---|
| Increased | Nodular (hot nodule Nodule Chalazion) | Toxic adenoma Toxic Adenoma Thyrotoxicosis and Hyperthyroidism |
| Diffuse | Graves’ disease Graves’ disease A common form of hyperthyroidism with a diffuse hyperplastic goiter. It is an autoimmune disorder that produces antibodies against the thyroid stimulating hormone receptor. These autoantibodies activate the TSH receptor, thereby stimulating the thyroid gland and hypersecretion of thyroid hormones. These autoantibodies can also affect the eyes (Graves ophthalmopathy) and the skin (Graves dermopathy). Thyrotoxicosis and Hyperthyroidism | |
| Normal | Symmetric uptake with no defects | |
| Decreased | Nodular (cold nodule Nodule Chalazion) | Thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy cancer |
| Diffuse | Hashimoto thyroiditis Thyroiditis Thyroiditis is a catchall term used to describe a variety of conditions that have inflammation of the thyroid gland in common. It includes pathologies that cause an acute illness with severe thyroid pain (e.g., subacute thyroiditis and infectious thyroiditis) as well as conditions in which there is no clinically evident inflammation and the manifestations primarily reflect thyroid dysfunction or a goiter (e.g., painless thyroiditis and fibrous Riedel’s thyroiditis). Thyroiditis |

Normal thyroid scan
Image: “Thyroid scan” by Myohan. License: CC BY 3.0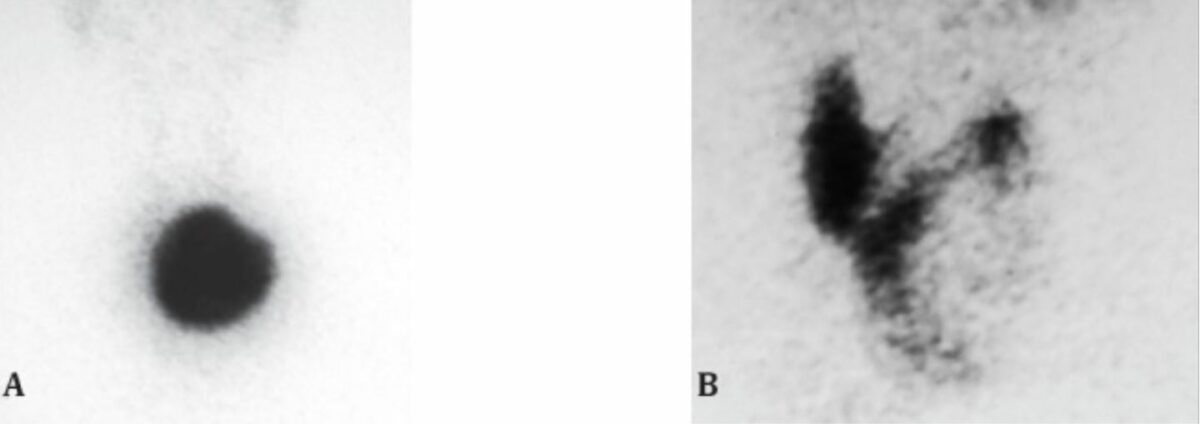
Technetium-99 pertechnetate (99mTcO4) thyroid scan:
A: A large hot nodule with suppression of the rest of the thyroid
B: A large cold nodule in the left lobe of the thyroid
On cytology, the hot nodule was reported as a “follicular neoplasm” and the cold nodule was reported as a “colloid nodule.”
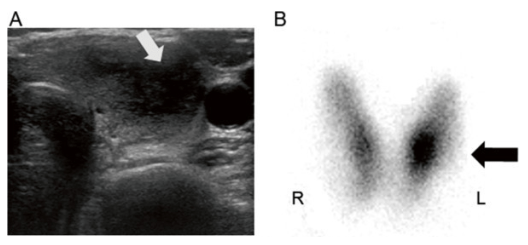
Initial thyroid ultrasound scanning and 99m-Technetium scintiscan
A: Thyroid ultrasonography reveals an ill-defined, solid, hypoechoic nodule (15 × 0.8 mm) with an irregular border in the left thyroid lobe (indicated by a white arrow).
B: Thyroid scintigraphy with 99m-Tc shows focal accumulation of radiotracer uptake in the lower lobe of the left thyroid, which represents the palpable tender nodule (indicated by a black arrow).