The 2 primary thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types are triiodothyronine (T3) and thyroxine (T4). These hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types are synthesized and secreted by the thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy, and they are responsible for stimulating metabolism in most cells of the body. Their secretion Secretion Coagulation Studies is regulated primarily by thyroid-stimulating hormone (TSH), which is produced by the pituitary Pituitary A small, unpaired gland situated in the sella turcica. It is connected to the hypothalamus by a short stalk which is called the infundibulum. Hormones: Overview and Types gland. Thyroid-stimulating hormone is regulated by thyroid-releasing hormone (TRH; which is stimulatory) and somatostatin Somatostatin A 14-amino acid peptide named for its ability to inhibit pituitary growth hormone release, also called somatotropin release-inhibiting factor. It is expressed in the central and peripheral nervous systems, the gut, and other organs. SRIF can also inhibit the release of thyroid-stimulating hormone; prolactin; insulin; and glucagon besides acting as a neurotransmitter and neuromodulator. In a number of species including humans, there is an additional form of somatostatin, srif-28 with a 14-amino acid extension at the n-terminal. Gastrointestinal Secretions (which is inhibitory). Both of these hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types are produced by the hypothalamus Hypothalamus The hypothalamus is a collection of various nuclei within the diencephalon in the center of the brain. The hypothalamus plays a vital role in endocrine regulation as the primary regulator of the pituitary gland, and it is the major point of integration between the central nervous and endocrine systems. Hypothalamus. T3 is far more active than T4, so most T4 is converted to T3 in the periphery (e.g., liver Liver The liver is the largest gland in the human body. The liver is found in the superior right quadrant of the abdomen and weighs approximately 1.5 kilograms. Its main functions are detoxification, metabolism, nutrient storage (e.g., iron and vitamins), synthesis of coagulation factors, formation of bile, filtration, and storage of blood. Liver: Anatomy). T3 helps to maintain normal cellular metabolism, oxygen consumption, energy levels, heart rate Heart rate The number of times the heart ventricles contract per unit of time, usually per minute. Cardiac Physiology, thermoregulation Thermoregulation Body temperature can be divided into external temperature, which involves the skin, and core temperature, which involves the CNS and viscera. While external temperature can be variable, the core temperature is maintained within a narrow range of 36.5-37.5ºC (97.7-99.5ºF). Body Temperature Regulation, bowel movements, mental health, and neurologic function. Abnormalities in thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy hormone levels can lead to hyperthyroidism Hyperthyroidism Hypersecretion of thyroid hormones from the thyroid gland. Elevated levels of thyroid hormones increase basal metabolic rate. Thyrotoxicosis and Hyperthyroidism and hypothyroidism Hypothyroidism Hypothyroidism is a condition characterized by a deficiency of thyroid hormones. Iodine deficiency is the most common cause worldwide, but Hashimoto's disease (autoimmune thyroiditis) is the leading cause in non-iodine-deficient regions. Hypothyroidism.
Last updated: May 17, 2024
The primary hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types released from the thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy include:
Release Release Release of a virus from the host cell following virus assembly and maturation. Egress can occur by host cell lysis, exocytosis, or budding through the plasma membrane. Virology of T3 and T4 is regulated by hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types secreted by the hypothalamus Hypothalamus The hypothalamus is a collection of various nuclei within the diencephalon in the center of the brain. The hypothalamus plays a vital role in endocrine regulation as the primary regulator of the pituitary gland, and it is the major point of integration between the central nervous and endocrine systems. Hypothalamus and pituitary Pituitary A small, unpaired gland situated in the sella turcica. It is connected to the hypothalamus by a short stalk which is called the infundibulum. Hormones: Overview and Types gland. This complex interaction is known as the HPT axis Axis The second cervical vertebra. Vertebral Column: Anatomy:
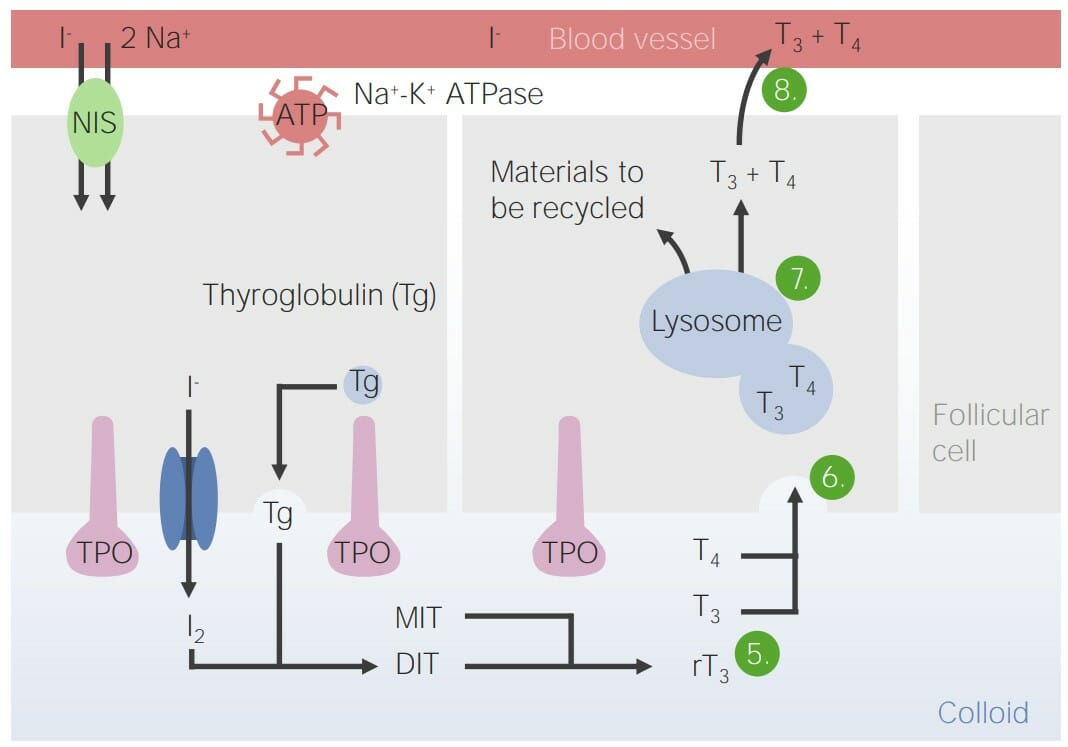
Steps for synthesis of thyroid hormones:
Through the sodium iodide symporter (NIS), odide (I‒) is brought into the thyroid follicular cells where the I‒ is oxidized into iodine (I2) and then secreted into colloid through pendrin channels. The follicular cells produce Tg, which is exocytosed into the colloid. Thyroid peroxidase (TPO) then combines the I2 and Tg molecules to form mono-iodotyrosine (MIT), or T1, and di-iodotyrosine (DIT), or T2. The TPO then uses the MIT and DIT to form triiodothyronine (T3), thyroxine (T4), and reverse triiodothyronine (rT3), an inactive metabolite. The thyroid hormones are endocytosed back into the follicular cells, processed in the lysosome, and then excreted into the blood.
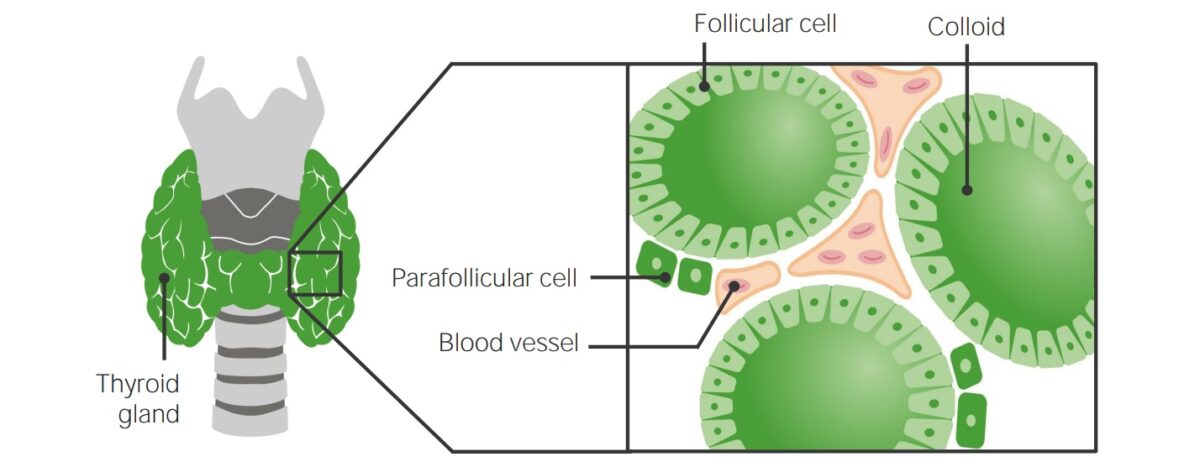
Histologic structure of the thyroid gland
Image by Lecturio.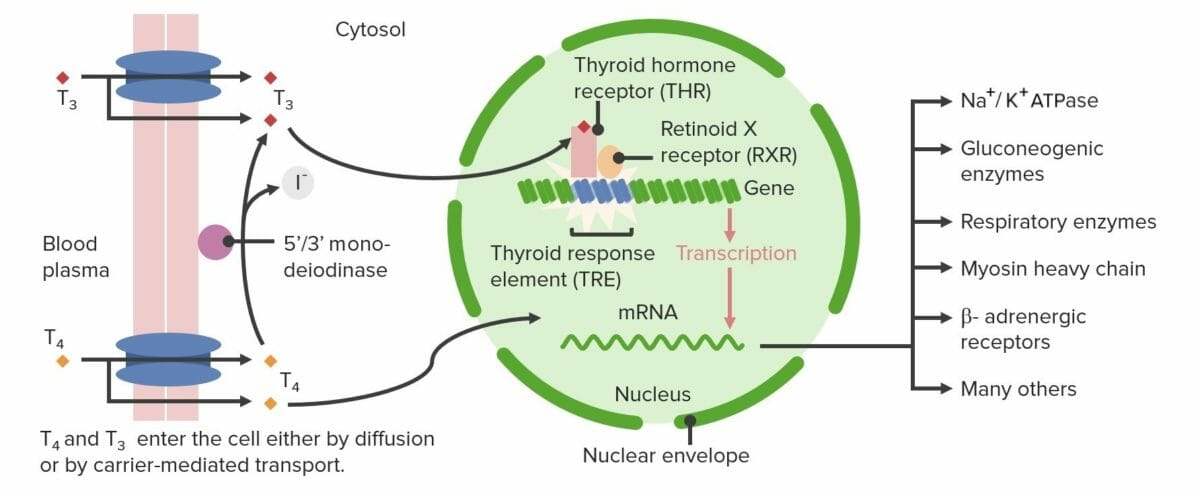
Peripheral conversion of T4 and T3:
Thyroid hormones exert their greatest influence over transcription as T3. Triiodothyronine moves into the nucleus where it binds to the THR. The T3-THR complex acts as a transcription factor and is able to bind directly to the DNA at sequences known as TREs. With the help of additional transcription-regulating proteins, transcription of messenger RNA (mRNA) occurs with mRNAs encoding a number of proteins involved in metabolism.
T4: thyroxine
T3: triiodothyronine
When thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types are produced at abnormal levels, symptoms can develop.
Hyperthyroidism Hyperthyroidism Hypersecretion of thyroid hormones from the thyroid gland. Elevated levels of thyroid hormones increase basal metabolic rate. Thyrotoxicosis and Hyperthyroidism is the inappropriate secretion Secretion Coagulation Studies of excessive amounts of thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy hormones Hormones Hormones are messenger molecules that are synthesized in one part of the body and move through the bloodstream to exert specific regulatory effects on another part of the body. Hormones play critical roles in coordinating cellular activities throughout the body in response to the constant changes in both the internal and external environments. Hormones: Overview and Types (T3 and T4), leading to an abnormal increase in the basal metabolic rate.
Hypothyroidism Hypothyroidism Hypothyroidism is a condition characterized by a deficiency of thyroid hormones. Iodine deficiency is the most common cause worldwide, but Hashimoto’s disease (autoimmune thyroiditis) is the leading cause in non-iodine-deficient regions. Hypothyroidism is the inadequate secretion Secretion Coagulation Studies of thyroid Thyroid The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck. Thyroid Gland: Anatomy hormone, leading to an abnormal decrease in the metabolic rate.