Arteries are tubular collections of cells that transport oxygenated blood and nutrients from the heart to the tissues of the body. The blood passes through the arteries in order of decreasing luminal diameter, starting in the largest artery (the aorta Aorta The main trunk of the systemic arteries. Mediastinum and Great Vessels: Anatomy) and ending in the small arterioles. Arteries are classified into 3 types: large elastic Elastic Connective Tissue: Histology arteries, medium muscular arteries, and small arteries and arterioles. Each of these types of arteries contain 3 primary layers: the tunica intima, tunica media, and tunica adventitia. In particular, the tunica media contains smooth muscle cells (allowing for vasoconstriction Vasoconstriction The physiological narrowing of blood vessels by contraction of the vascular smooth muscle. Vascular Resistance, Flow, and Mean Arterial Pressure), and in the larger vessels, a significant amount of elastin (allowing these vessels to stretch and recoil in response to changes in pressure during systole Systole Period of contraction of the heart, especially of the heart ventricles. Cardiac Cycle and diastole Diastole Post-systolic relaxation of the heart, especially the heart ventricles. Cardiac Cycle).
Last updated: Dec 15, 2025
Arteries are tubular collections of cells that transport oxygenated blood and nutrients from the heart to the tissues of the body.
All arteries have the following characteristics:
All arteries have the same basic structure and are made up of three primary layers: the tunica intima, tunica media, and tunica adventitia (also known as tunica externa).
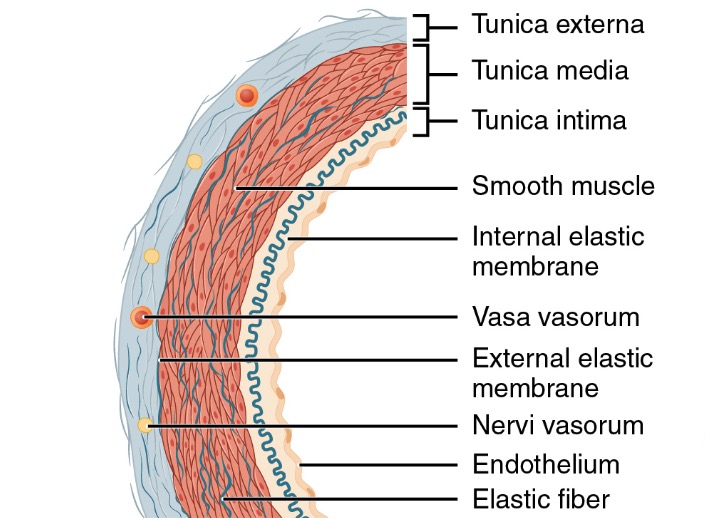
Structure of an artery wall
Image: “Structure of an artery wall” by Phil Schatz. License: CC BY 4.0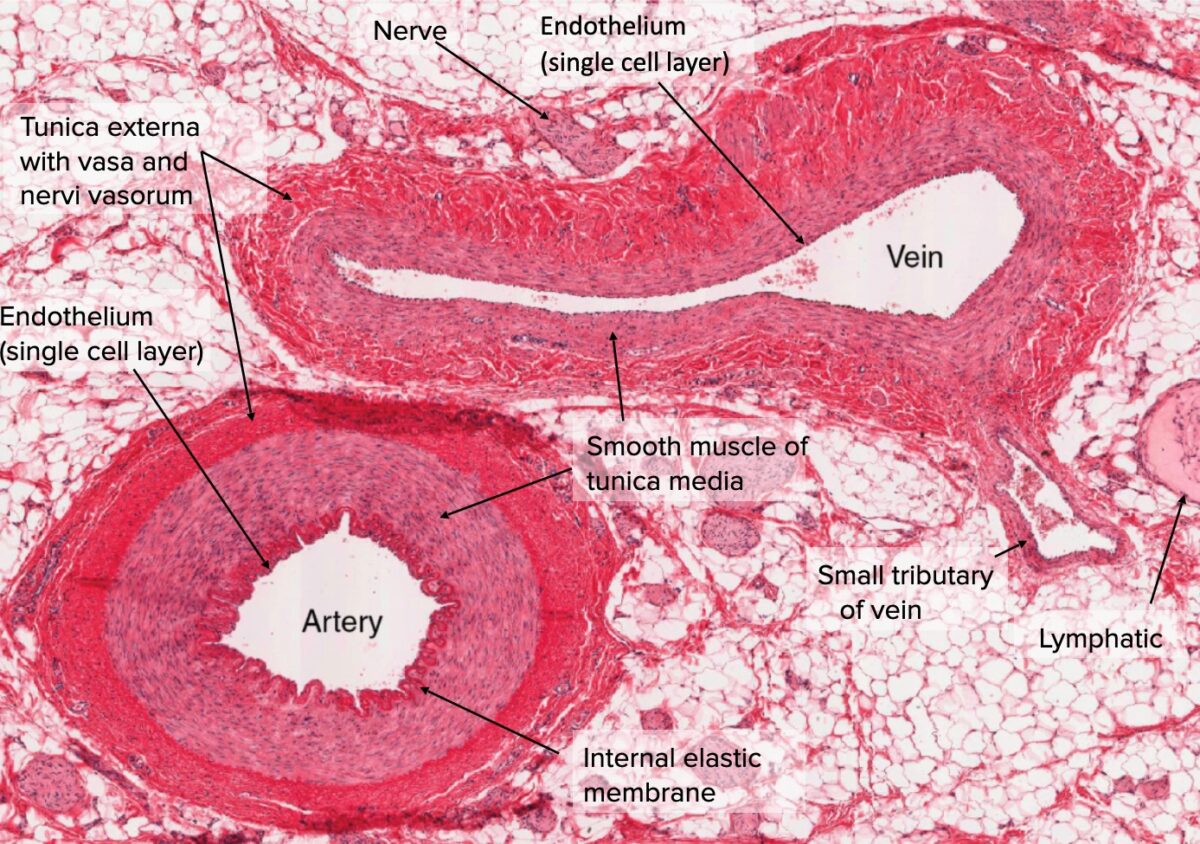
Cross section of artery and vein
Image: “Types of Arteries and Arterioles” by Phil Schatz. License: CC BY 4.0, edited by Lecturio.There are 3 primary types of arteries, based on their overall size, function, and composition (known as segmental differentiation). The arteries generally exist on a continuum, with gradual changes in vessel morphology moving down the arterial tree.
The 3 primary types of arteries are:
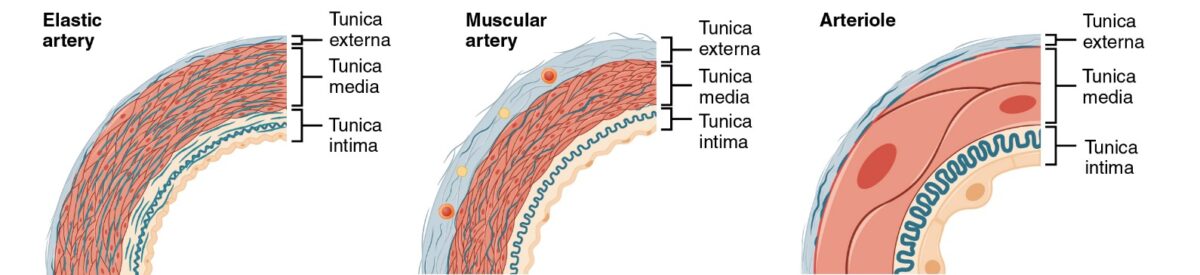
3 primary types of arteries
Image: “Types of Arteries and Arterioles” by Phil Schatz. License: CC BY 4.0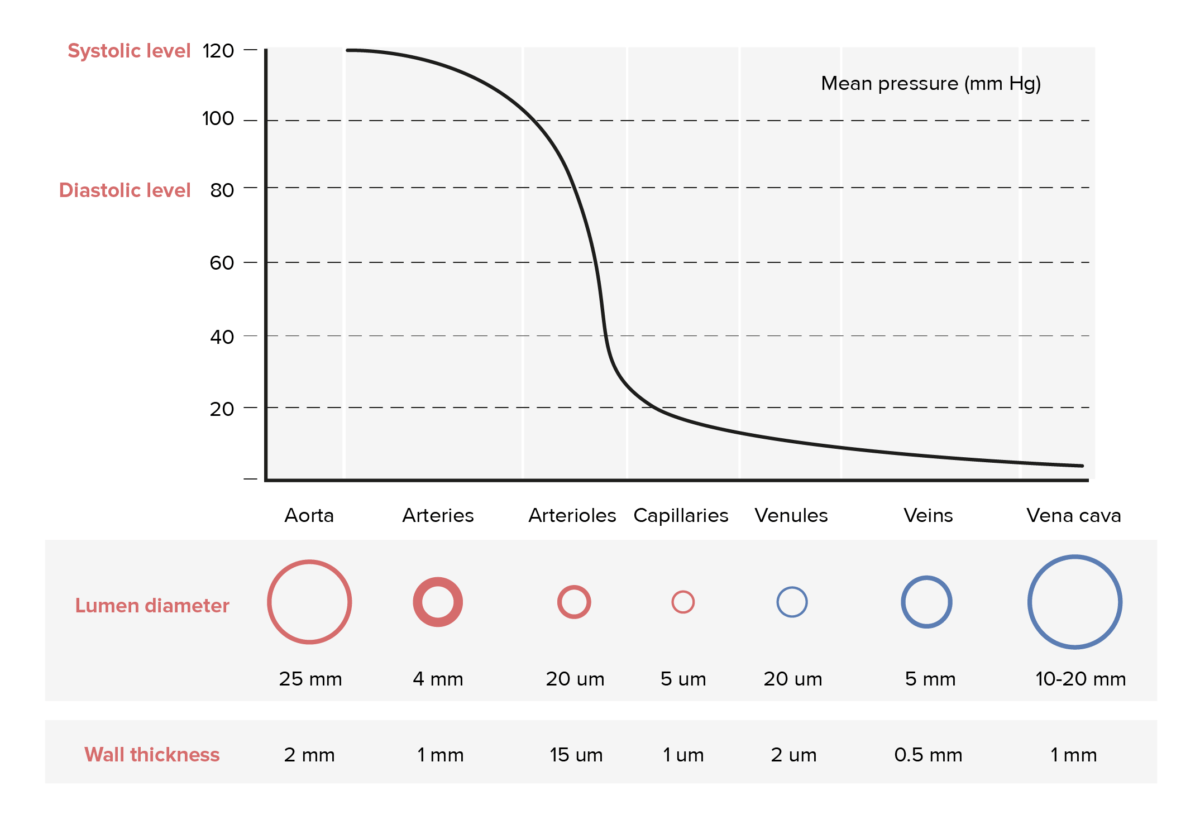
Intraluminal pressures of different vessels
Image by Lecturio.This group includes the largest arteries in the body; all large/ elastic Elastic Connective Tissue: Histology arteries are close to the heart. The aorta Aorta The main trunk of the systemic arteries. Mediastinum and Great Vessels: Anatomy is the largest artery in the body.
Large/ elastic Elastic Connective Tissue: Histology arteries include:
Characteristics:
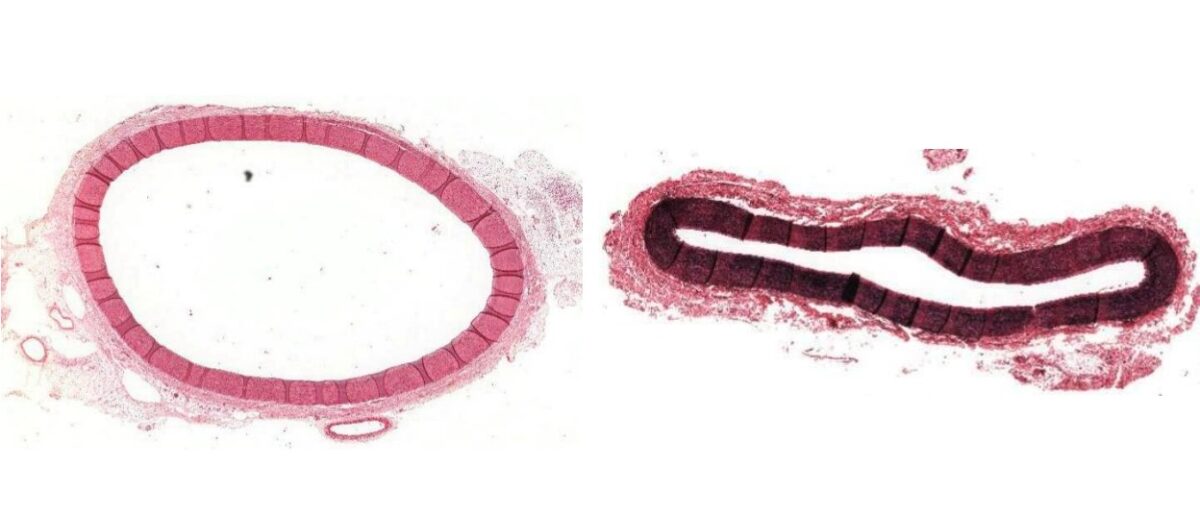
Histologic staining of the aorta:
Left: H&E stain of the aorta
Right: Stained for elastic tissue (darker color), demonstrating the significant amount of elastic tissue within the tunica media in the aorta
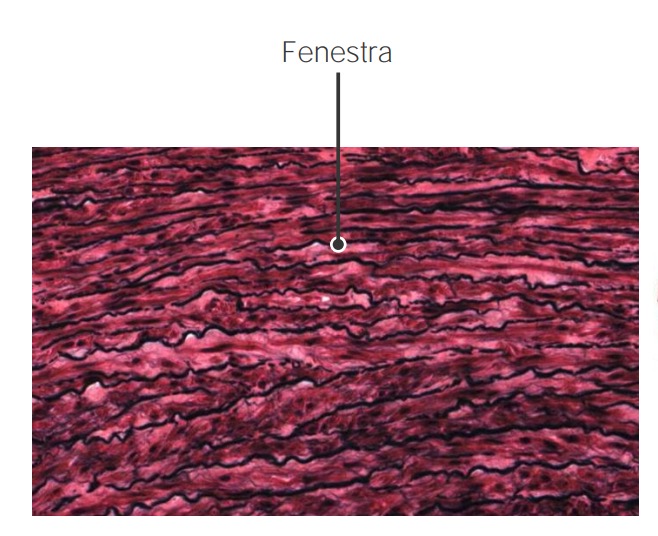
Fenestra (or “windows”) within the elastic fibers in the aortic wall
Image by Geoffrey Meyer, PhD.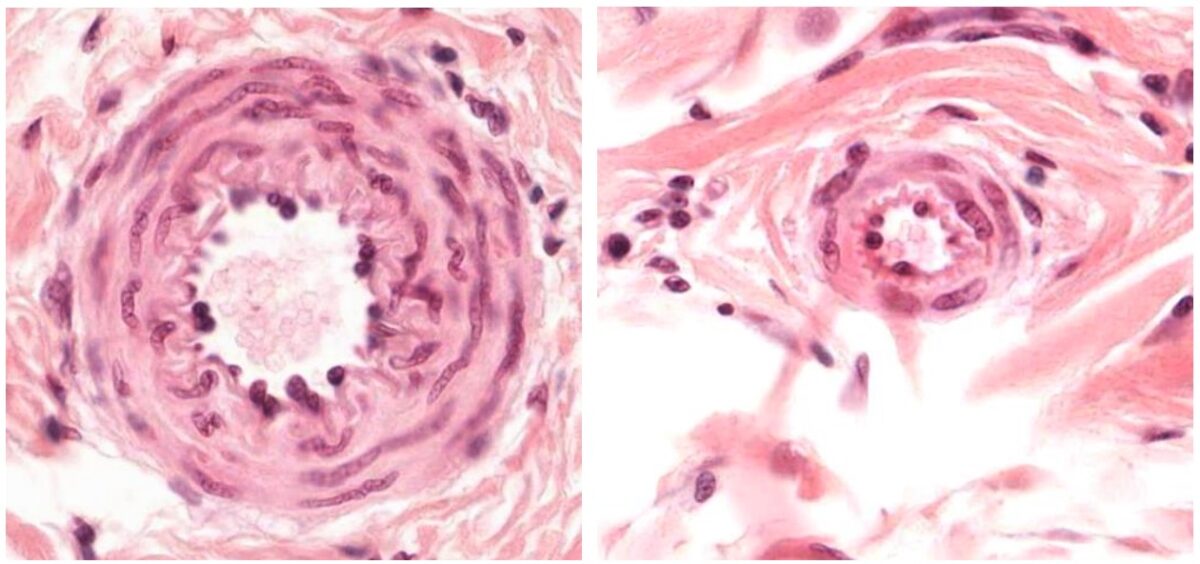
Cross sections of a small artery (left) and an arteriole (right)
Image by Geoffrey Meyer, PhD.
Capillary bed demonstrating an arteriole, a metarteriole, and precapillary sphincters
Image: “Capillary Bed” by OpenStax College. License: CC BY 3.0Vasculitides Vasculitides Vasculitides are a group of conditions characterized by vasculitis, ischemia, and damage to the organs supplied by the affected vessels. The affected arteries are of different sizes and locations and vary by the type of vasculitis. Vasculitides are a group of autoimmune conditions characterized by immune-mediated blood vessel inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body’s defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation and wall damage. Loss of vessel integrity can lead to bleeding, as well as to downstream ischemia Ischemia A hypoperfusion of the blood through an organ or tissue caused by a pathologic constriction or obstruction of its blood vessels, or an absence of blood circulation. Ischemic Cell Damage and necrosis Necrosis The death of cells in an organ or tissue due to disease, injury or failure of the blood supply. Ischemic Cell Damage. These processes can be primary or secondary, and they tend to affect only vessels of a specific type or in a specific location.
| Category of vasculitis Vasculitis Inflammation of any one of the blood vessels, including the arteries; veins; and rest of the vasculature system in the body. Systemic Lupus Erythematosus | Examples of conditions in each category |
|---|---|
| Large-vessel vasculitis Vasculitis Inflammation of any one of the blood vessels, including the arteries; veins; and rest of the vasculature system in the body. Systemic Lupus Erythematosus |
|
| Medium-vessel vasculitis Vasculitis Inflammation of any one of the blood vessels, including the arteries; veins; and rest of the vasculature system in the body. Systemic Lupus Erythematosus |
|
| Small-vessel vasculitis Small-Vessel Vasculitis Henoch-Schönlein Purpura |
|
| Variable-vessel vasculitis Vasculitis Inflammation of any one of the blood vessels, including the arteries; veins; and rest of the vasculature system in the body. Systemic Lupus Erythematosus |
|
| Single-organ vasculitis Vasculitis Inflammation of any one of the blood vessels, including the arteries; veins; and rest of the vasculature system in the body. Systemic Lupus Erythematosus |
|