Veins are tubular collections of cells, which transport deoxygenated blood and waste from the capillary beds Capillary beds Groups of 10–100 individual capillary vessels supplied by a single metarteriole. Capillaries: Histology back to the heart. Veins are classified into 3 types: small veins/venules, medium veins, and large veins. Each type contains 3 primary layers: tunica intima Tunica intima The innermost layer of an artery or vein, made up of one layer of endothelial cells and supported by an internal elastic lamina. Arteries: Histology, tunica media Tunica media The middle layer of blood vessel walls, composed principally of thin, cylindrical, smooth muscle cells and elastic tissue. It accounts for the bulk of the wall of most arteries. The smooth muscle cells are arranged in circular layers around the vessel, and the thickness of the coat varies with the size of the vessel. Arteries: Histology, and tunica adventitia Tunica adventitia The outermost covering of organs, blood vessels, and other such structures in the body. Arteries: Histology. The venous circulation Circulation The movement of the blood as it is pumped through the cardiovascular system. ABCDE Assessment is a low-pressure system with much lower amounts of smooth muscle and elastic Elastic Connective Tissue: Histology tissue, thinner walls, and larger lumens than arteries Arteries Arteries are tubular collections of cells that transport oxygenated blood and nutrients from the heart to the tissues of the body. The blood passes through the arteries in order of decreasing luminal diameter, starting in the largest artery (the aorta) and ending in the small arterioles. Arteries are classified into 3 types: large elastic arteries, medium muscular arteries, and small arteries and arterioles. Arteries: Histology. Veins are capacitance Capacitance The measure of a blood vessel's ability to increase the volume of blood it holds without a large increase in blood pressure. The vascular capacitance is equal to the change in volume divided by the change in pressure. Venous Function vessels with significant compliance and the ability to distend and hold up to 70%–80% of blood volume at rest.
Last updated: Dec 15, 2025
Veins are tubular collections of cells transporting deoxygenated blood and waste products from capillaries Capillaries Capillaries are the primary structures in the circulatory system that allow the exchange of gas, nutrients, and other materials between the blood and the extracellular fluid (ECF). Capillaries are the smallest of the blood vessels. Because a capillary diameter is so small, only 1 RBC may pass through at a time. Capillaries: Histology in the periphery of the body back to the heart.
Characteristics of veins and the venous system include:
All veins have the same basic structure and are made up of 3 primary layers: tunica intima Tunica intima The innermost layer of an artery or vein, made up of one layer of endothelial cells and supported by an internal elastic lamina. Arteries: Histology, tunica media Tunica media The middle layer of blood vessel walls, composed principally of thin, cylindrical, smooth muscle cells and elastic tissue. It accounts for the bulk of the wall of most arteries. The smooth muscle cells are arranged in circular layers around the vessel, and the thickness of the coat varies with the size of the vessel. Arteries: Histology, and tunica adventitia Tunica adventitia The outermost covering of organs, blood vessels, and other such structures in the body. Arteries: Histology.
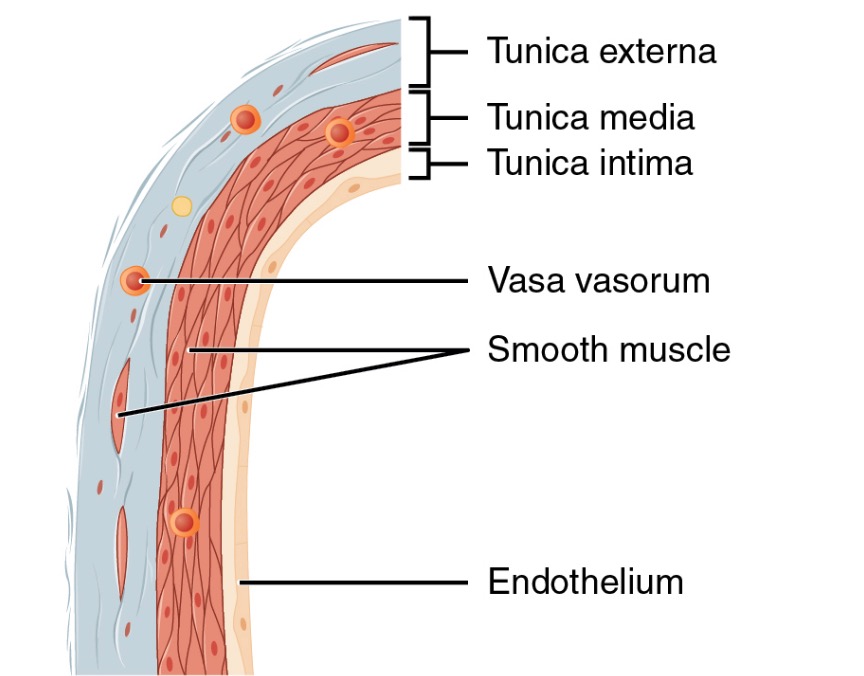
Structure of a vein wall
Image: “Structure of a vein wall” by Phil Schatz. License: CC BY 4.0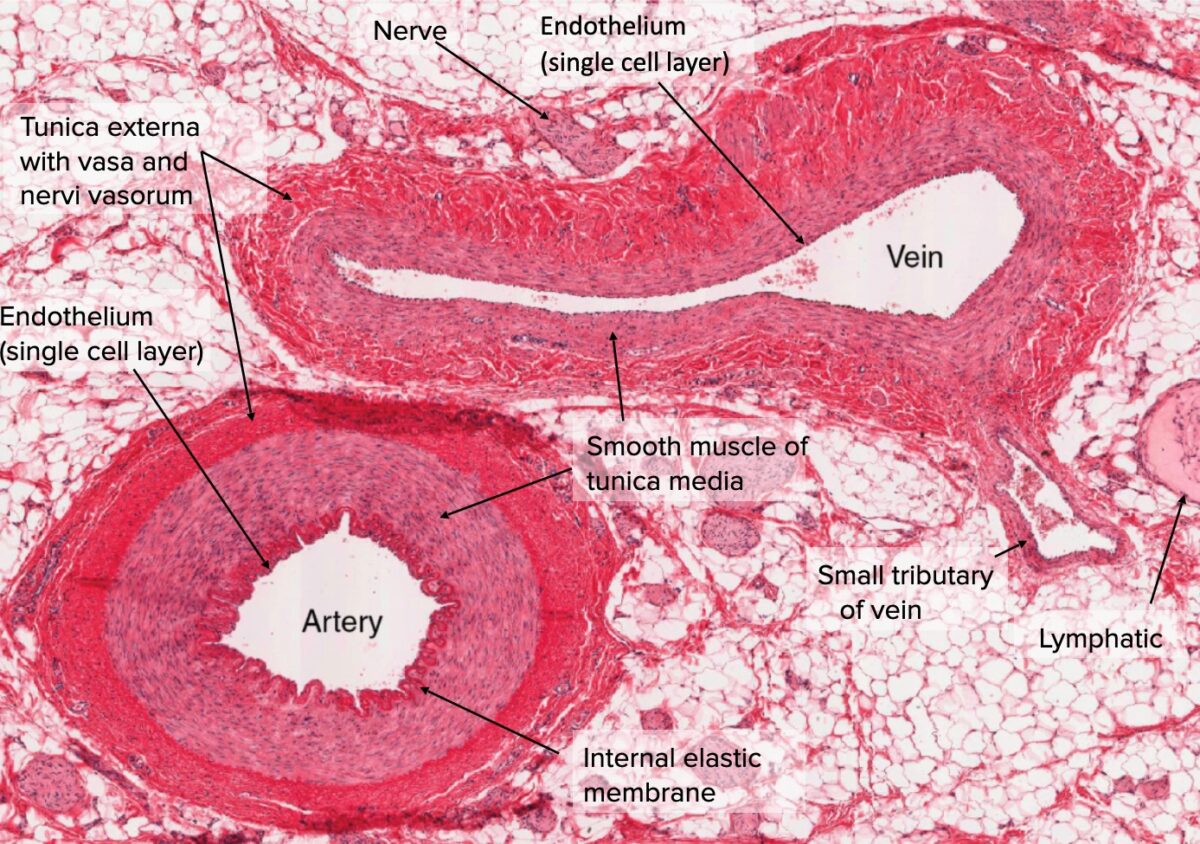
Cross-section of artery and vein
Image: “Types of Arteries and Arterioles” by Phil Schatz. License: CC BY 4.0, edited by Lecturio.Segmental differentiation distinguishes the 3 primary types of veins by overall size, function, and composition. Veins generally exist on a continuum with gradual changes in vessel morphology down the venous tree.
The 3 primary types of veins are:
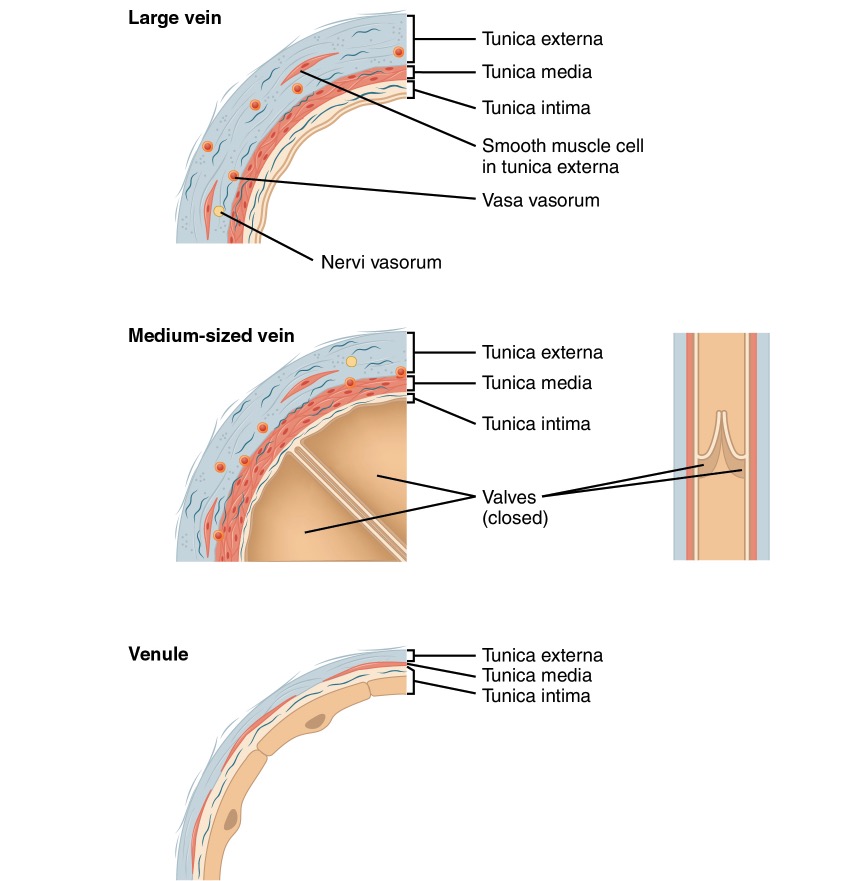
Comparison of large, medium, and small veins
Image: “Comparison of large, medium, and small veins” by Phil Schatz. License: CC BY 4.0
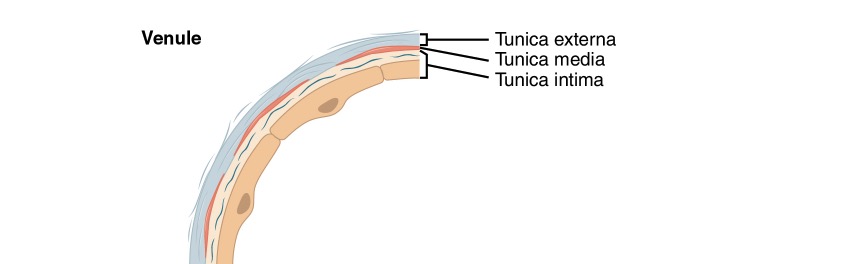
Diagram of a venule
Image: “Venule” by Phil Schatz. License: CC BY 4.0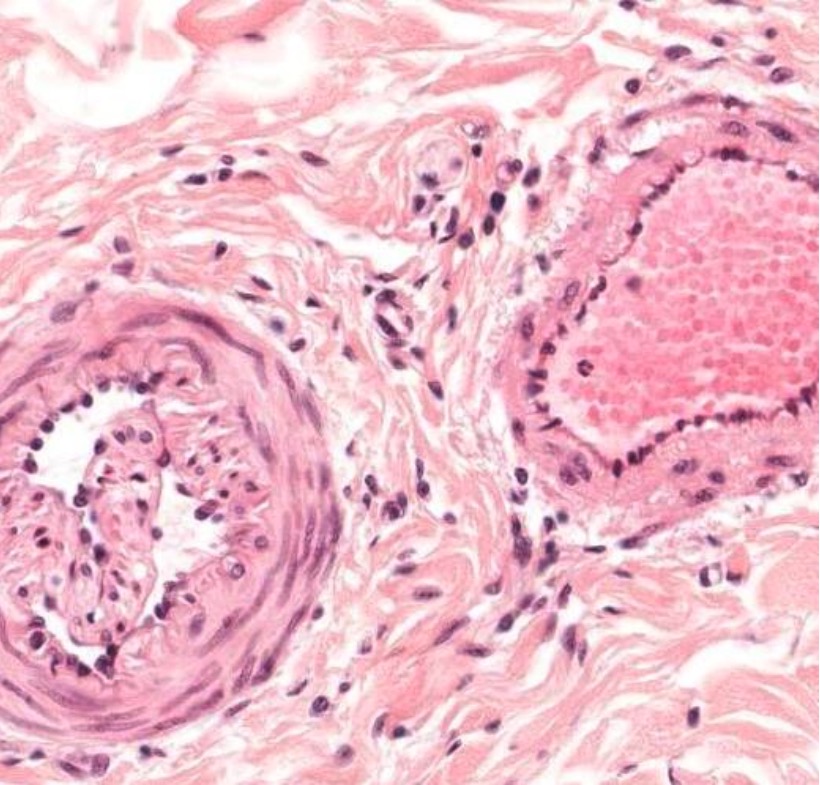
Cross-section of a small artery (left) and a small vein (right)
Image by Geoffrey Meyer, PhD.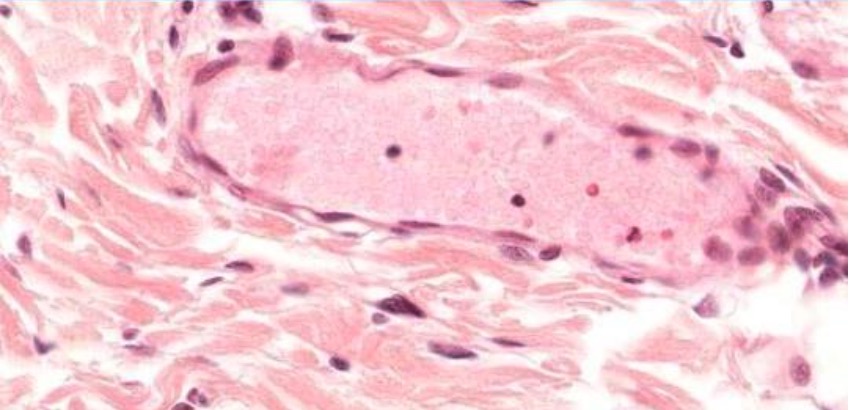
Postcapillary venule
Image by Geoffrey Meyer, PhD.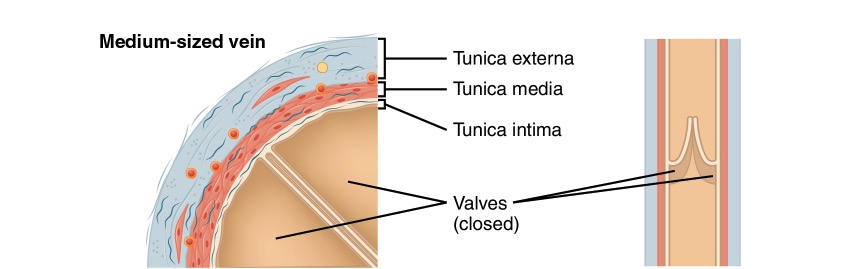
Diagram of a medium-sized vein
Image: “Medium-sized vein” by Phil Schatz. License: CC BY 4.0
Diagram of the muscle pump
Image: “The contraction of skeletal muscles” by Phil Schatz. License: CC BY 4.0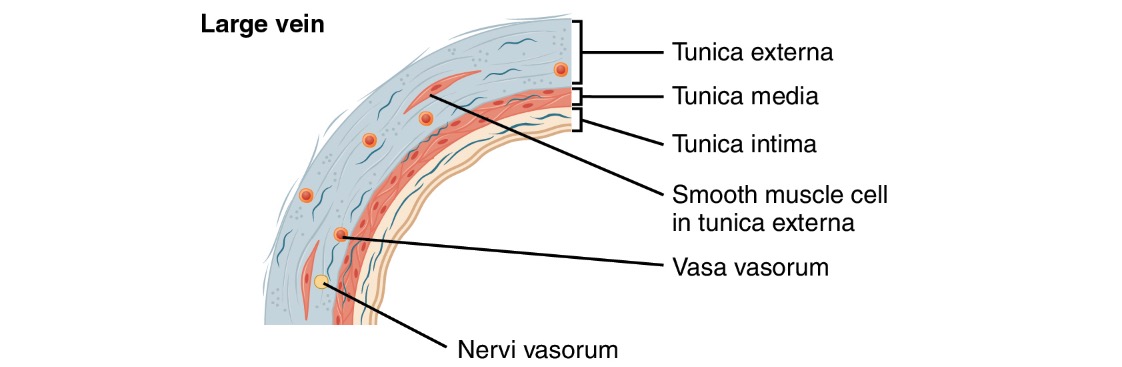
Diagram of a large vein
Image: “Large vein” by Phil Schatz. License: CC BY 4.0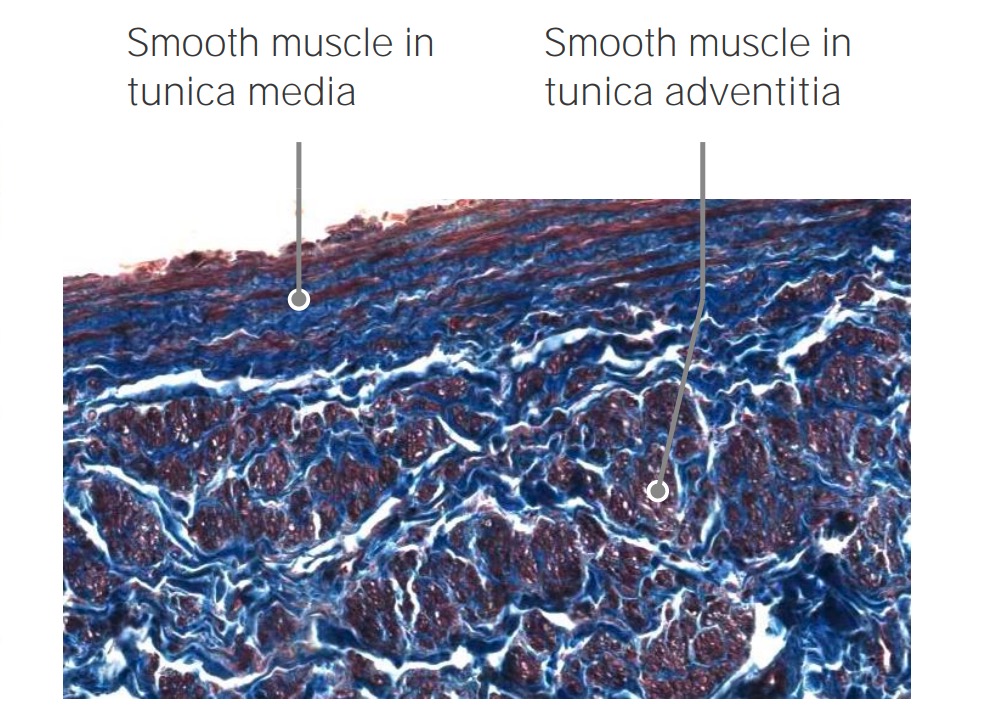
Longitudinal smooth muscles of the vena cava
Image by Geoffrey Meyer, PhD.