Rhabdomyolysis is characterized by muscle necrosis and the release of toxic intracellular contents, especially myoglobin, into the circulation. Rhabdomyolysis can result from trauma or direct muscle injuries; however, non-exertional and non-traumatic etiologies (heatstroke, immobilization, medication side effects) can also lead to muscle breakdown. The classic triad of symptoms includes myalgia, weakness, and tea-colored urine, but the presentation can be nonspecific. The diagnosis is clinical, based on history, exam, and lab findings, typically including elevated creatine kinase levels, abnormal electrolytes with possible renal failure, and dark urine without RBCs (indicating myoglobinuria). Management of rhabdomyolysis involves aggressive IV fluid resuscitation and appropriately managing electrolyte abnormalities, triggering events, and acute kidney injury (if present).
Last updated: Mar 4, 2024
Rhabdomyolysis Rhabdomyolysis Rhabdomyolysis is characterized by muscle necrosis and the release of toxic intracellular contents, especially myoglobin, into the circulation. Rhabdomyolysis is a syndrome marked by muscle necrosis Muscle Necrosis Rhabdomyolysis, resulting in the release of toxic intracellular muscle constituents into the circulation Circulation The movement of the blood as it is pumped through the cardiovascular system. ABCDE Assessment (especially myoglobin Myoglobin A conjugated protein which is the oxygen-transporting pigment of muscle. It is made up of one globin polypeptide chain and one heme group. Rhabdomyolysis).
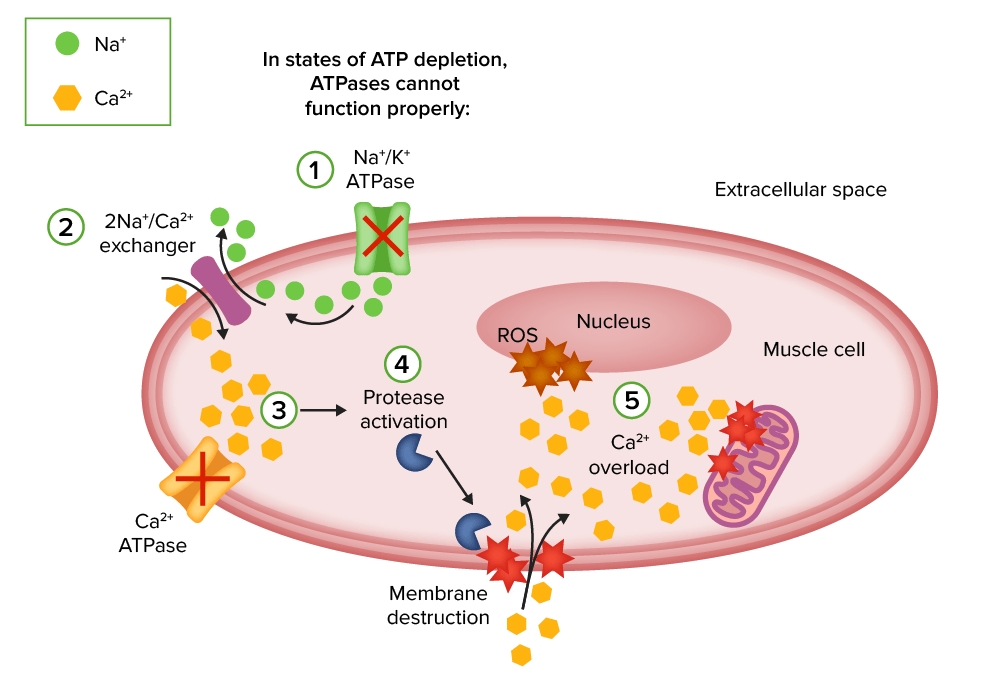
Injury mechanisms of rhabdomyolysis:
1. Energy (ATP) depletion inhibits Na+/K+ ATPase function and increases intracellular sodium.
2. The 2Na+/Ca2+ exchanger increases intracellular calcium.
3. Ca2+ ATPase is not able to pump out intracellular calcium due to energy depletion.
4. Intracellular calcium activates proteases such as phospholipase 2 (PLA2), which destroy the structural components of cell membranes and allow the entry of more calcium.
5. Calcium overload disrupts mitochondrial integrity and induces apoptosis, leading to necrosis of muscle cells.
ROS: reactive oxygen species
Renal injury is the most common systemic complication of rhabdomyolysis Rhabdomyolysis Rhabdomyolysis is characterized by muscle necrosis and the release of toxic intracellular contents, especially myoglobin, into the circulation. Rhabdomyolysis. Factors contributing to renal failure Renal failure Conditions in which the kidneys perform below the normal level in the ability to remove wastes, concentrate urine, and maintain electrolyte balance; blood pressure; and calcium metabolism. Renal insufficiency can be classified by the degree of kidney damage (as measured by the level of proteinuria) and reduction in glomerular filtration rate. Crush Syndrome include:
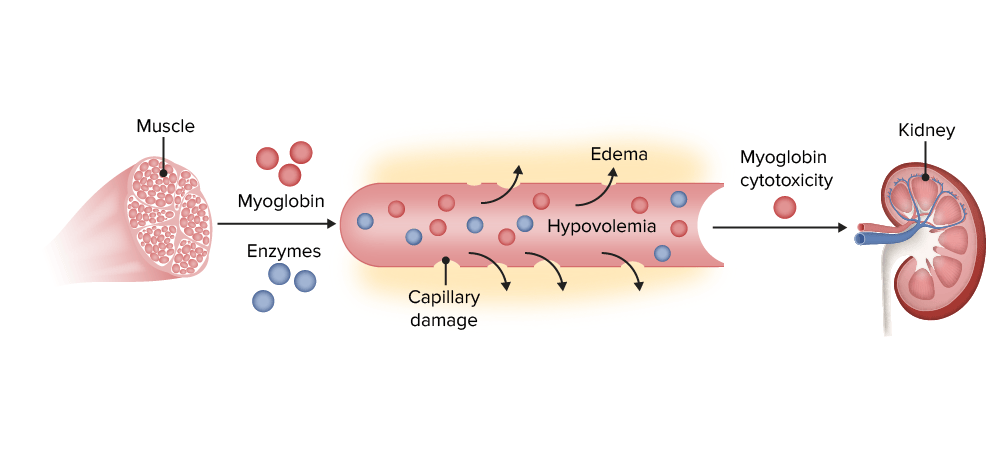
Acute kidney injury (AKI) in rhabdomyolysis (enzymes: creatine kinase, aldolase, lactate dehydrogenase):
After muscle destruction, myoglobin and enzymes are released into the circulation, damaging capillaries and leading to leakage and edema. Hypovolemia and reduced renal blood flow are associated with AKI. Myoglobin cytotoxicity affects the kidney due to lipid peroxidation and production of reactive oxygen species. Tubular obstruction by myoglobin is also associated with AKI.
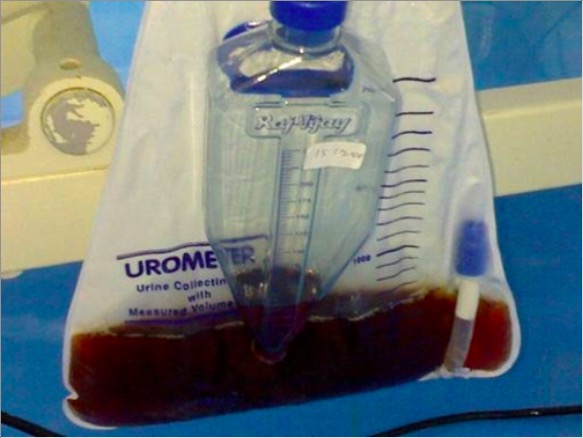
Tea-colored urine of a patient being treated for rhabdomyolysis
Image: “Urine appearance” by the Department of General Medicine, Sri Ramachandra University Chennai, Tamil Nadu, India. License: CC BY 3.0Laboratory abnormalities[2,4,5]
Additional labs to consider during workup[2,4,5]
Electrocardiography Electrocardiography Recording of the moment-to-moment electromotive forces of the heart as projected onto various sites on the body’s surface, delineated as a scalar function of time. The recording is monitored by a tracing on slow moving chart paper or by observing it on a cardioscope, which is a cathode ray tube display. Electrocardiogram (ECG) ( ECG ECG An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG))[4]
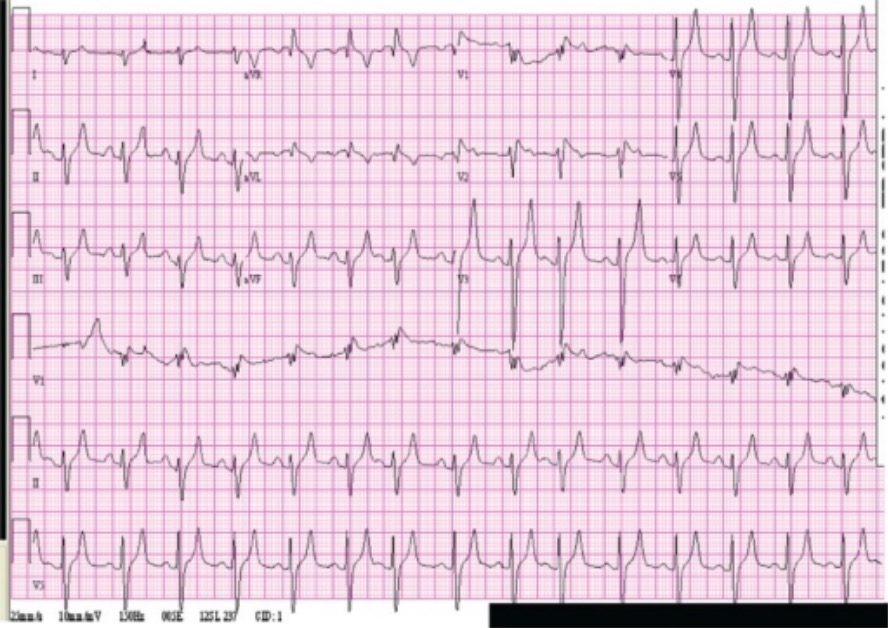
Patient with rhabdomyolysis and hyperkalemia:
Electrocardiogram of a patient treated for rhabdomyolysis, showing peaked T waves and wide QRS. The patient had a serum potassium level of 8 mEq/L.
Local protocols may vary from location to location. The following information is based on current US and UK guidelines.
Initial approach[2,4]
Aggressive intravenous fluid resuscitation Resuscitation The restoration to life or consciousness of one apparently dead. . Neonatal Respiratory Distress Syndrome[2,5‒7]
Other therapies
Correction of electrolyte abnormalities[5,7]
Monitoring[7]
Renal replacement therapy (RRT)[2,5,7]
Analgesia Analgesia Methods of pain relief that may be used with or in place of analgesics. Anesthesiology: History and Basic Concepts ( crush injury Crush injury Excessive compression of parts of the body that causes muscle swelling, fracture, and/or neurological disturbances in the affected areas. Crush injury with systemic manifestations is referred to as crush syndrome. Crush Syndrome)[7]
Management algorithm
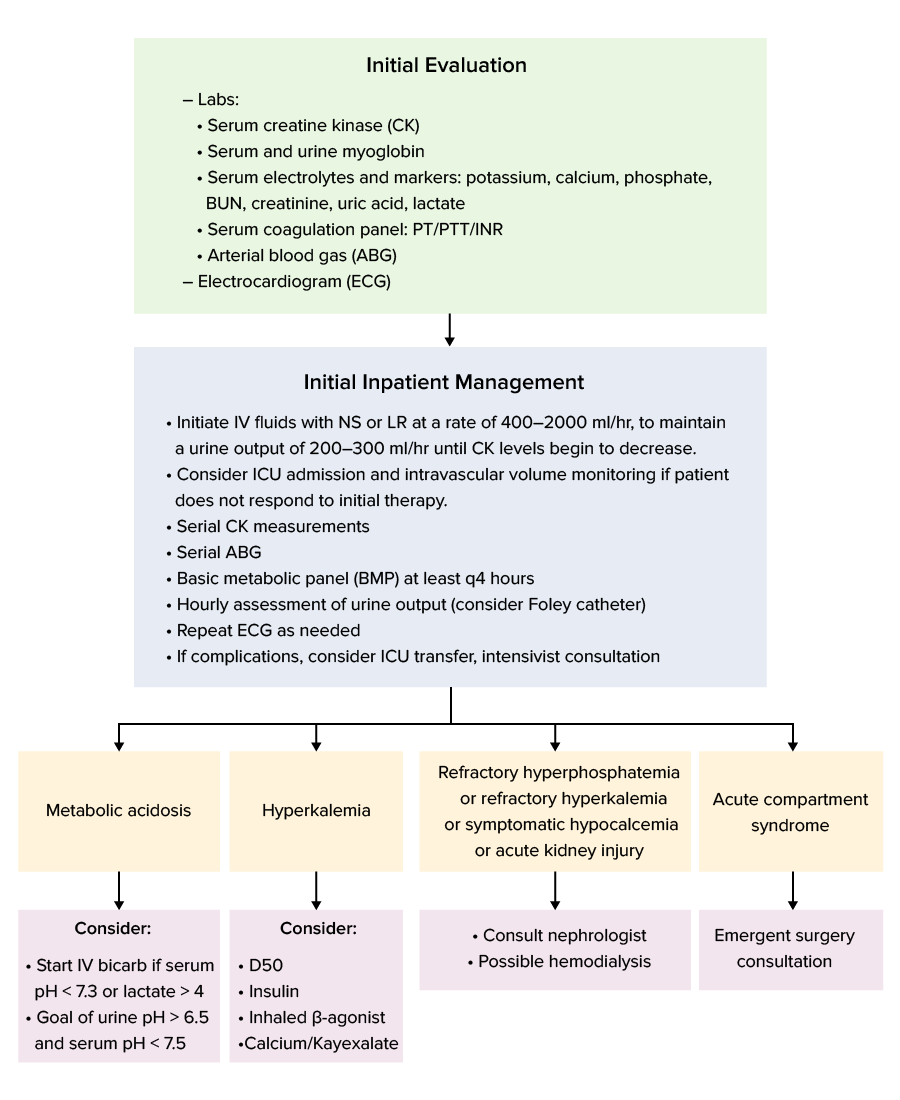
Management algorithm for rhabdomyolysis
Image by Lecturio.