Giardiasis is caused by Giardia Giardia A genus of flagellate intestinal eukaryotes parasitic in various vertebrates, including humans. Characteristics include the presence of four pairs of flagella arising from a complicated system of axonemes and cysts that are ellipsoidal to ovoidal in shape. Nitroimidazoles lamblia (G. lamblia), a flagellated protozoan that can infect the intestinal tract. Giardia Giardia A genus of flagellate intestinal eukaryotes parasitic in various vertebrates, including humans. Characteristics include the presence of four pairs of flagella arising from a complicated system of axonemes and cysts that are ellipsoidal to ovoidal in shape. Nitroimidazoles transmission occurs most commonly through consumption of cysts Cysts Any fluid-filled closed cavity or sac that is lined by an epithelium. Cysts can be of normal, abnormal, non-neoplastic, or neoplastic tissues. Fibrocystic Change in contaminated water or through the fecal-oral route Fecal-oral route Echovirus. Excystation occurs in the gastrointestinal (GI) tract, and trophozoites Trophozoites Cells or feeding stage in the life cycle of sporozoan protozoa. In the malarial parasite, the trophozoite develops from the merozoite and then splits into the schizont. Trophozoites that are left over from cell division can go on to form gametocytes. Amebicides attach to the intestinal wall villi and cause malabsorption Malabsorption General term for a group of malnutrition syndromes caused by failure of normal intestinal absorption of nutrients. Malabsorption and Maldigestion. The hallmark symptom of giardiasis is foul-smelling steatorrhea Steatorrhea A condition that is characterized by chronic fatty diarrhea, a result of abnormal digestion and/or intestinal absorption of fats. Diarrhea. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship who develop chronic infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease may experience weight loss Weight loss Decrease in existing body weight. Bariatric Surgery, failure to thrive Failure to Thrive Failure to thrive (FTT), or faltering growth, describes suboptimal weight gain and growth in children. The majority of cases are due to inadequate caloric intake; however, genetic, infectious, and oncological etiologies are also common. Failure to Thrive, and vitamin deficiencies as a result of malabsorption Malabsorption General term for a group of malnutrition syndromes caused by failure of normal intestinal absorption of nutrients. Malabsorption and Maldigestion. The diagnosis is made through detection of Giardia Giardia A genus of flagellate intestinal eukaryotes parasitic in various vertebrates, including humans. Characteristics include the presence of four pairs of flagella arising from a complicated system of axonemes and cysts that are ellipsoidal to ovoidal in shape. Nitroimidazoles organisms, antigens, or deoxyribonucleic acid Deoxyribonucleic acid A deoxyribonucleotide polymer that is the primary genetic material of all cells. Eukaryotic and prokaryotic organisms normally contain DNA in a double-stranded state, yet several important biological processes transiently involve single-stranded regions. DNA, which consists of a polysugar-phosphate backbone possessing projections of purines (adenine and guanine) and pyrimidines (thymine and cytosine), forms a double helix that is held together by hydrogen bonds between these purines and pyrimidines (adenine to thymine and guanine to cytosine). DNA Types and Structure ( DNA DNA A deoxyribonucleotide polymer that is the primary genetic material of all cells. Eukaryotic and prokaryotic organisms normally contain DNA in a double-stranded state, yet several important biological processes transiently involve single-stranded regions. DNA, which consists of a polysugar-phosphate backbone possessing projections of purines (adenine and guanine) and pyrimidines (thymine and cytosine), forms a double helix that is held together by hydrogen bonds between these purines and pyrimidines (adenine to thymine and guanine to cytosine). DNA Types and Structure) in the stool. Management includes supportive treatment and antimicrobial therapy with metronidazole Metronidazole A nitroimidazole used to treat amebiasis; vaginitis; trichomonas infections; giardiasis; anaerobic bacteria; and treponemal infections. Pyogenic Liver Abscess, tinidazole Tinidazole A nitroimidazole alkylating agent that is used as an antitrichomonal agent against trichomonas vaginalis; entamoeba histolytica; and giardia lamblia infections. It also acts as an antibacterial agent for the treatment of bacterial vaginosis and anaerobic bacterial infections. Nitroimidazoles, or nitazoxanide. Prevention measures include proper handwashing and water treatment.
Last updated: Sep 19, 2022
Giardiasis is caused by the flagellated protozoan, Giardia Giardia A genus of flagellate intestinal eukaryotes parasitic in various vertebrates, including humans. Characteristics include the presence of four pairs of flagella arising from a complicated system of axonemes and cysts that are ellipsoidal to ovoidal in shape. Nitroimidazoles lamblia (G. lamblia, also known as G. duodenalis or G. intestinalis).
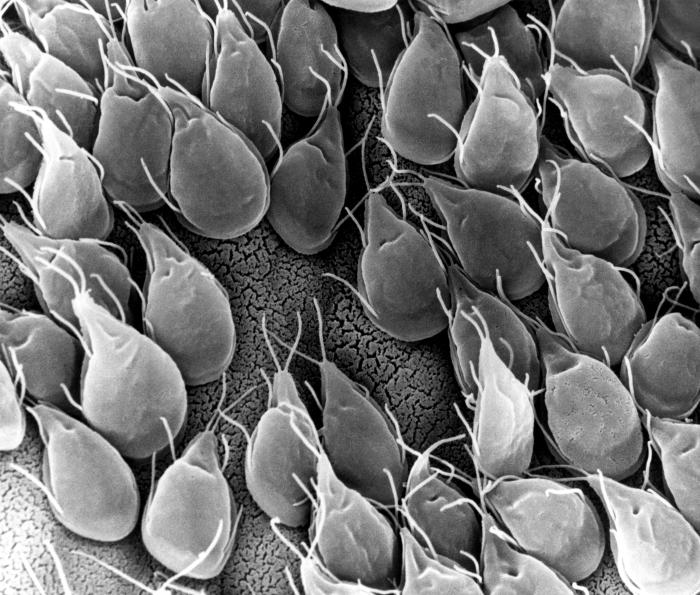
Scanning electron microscopic (SEM) image of G. lamblia trophozoites
Image: “SEM” by CDC/Dr. Stan Erlandsen. License: Public Domain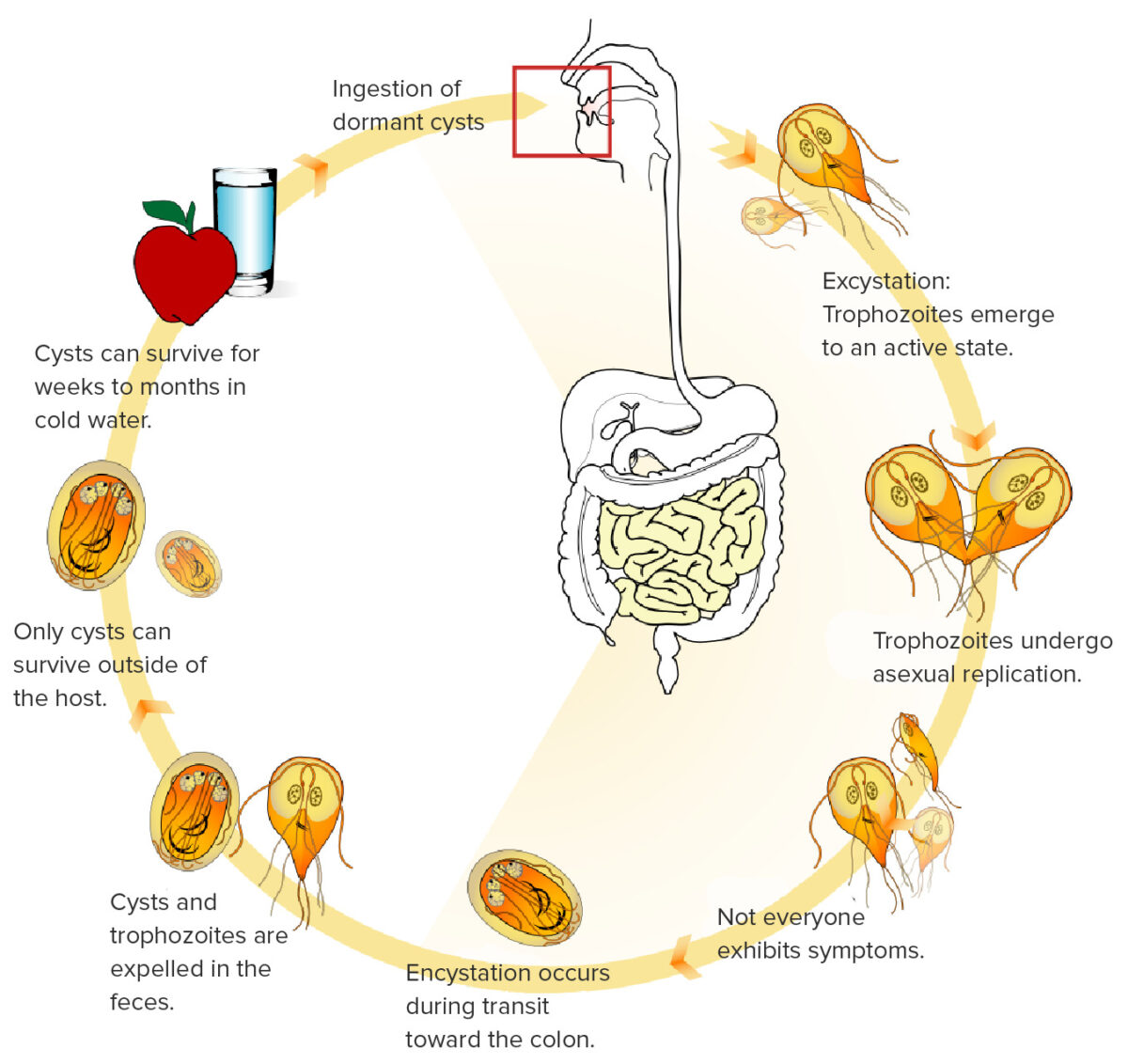
This image shows the life cycle of G. lamblia. Cysts can survive for long periods of time in cold water and then be inadvertently consumed. Once consumed, the cysts transform into trophozoite form, replicate, and infect the intestines. The trophozoites attach to the intestinal villi, resulting in symptoms.
Image: “Giardia life cycle” by LadyofHats. License: Public Domain, edited by Lecturio.While some patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship may be asymptomatic, the hallmark clinical feature of giardiasis is malabsorptive diarrhea Malabsorptive diarrhea Norovirus.
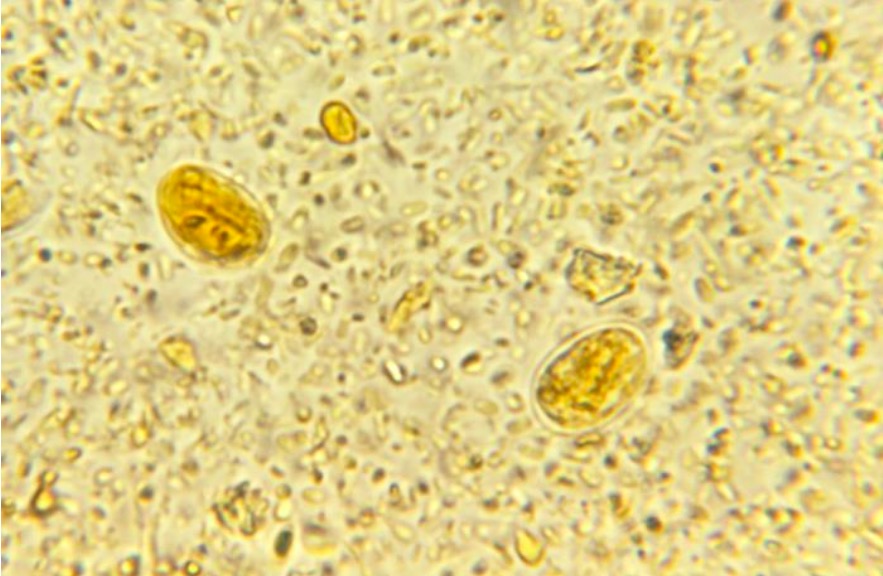
Stool microscopy revealing the presence of 2 G. lamblia cysts
Image: “ 21085” by CDC. License: Public Domain| Giardia Giardia A genus of flagellate intestinal eukaryotes parasitic in various vertebrates, including humans. Characteristics include the presence of four pairs of flagella arising from a complicated system of axonemes and cysts that are ellipsoidal to ovoidal in shape. Nitroimidazoles | Leishmania Leishmania Leishmania species are obligate intracellular parasites that are transmitted by an infected sandfly. The disease is endemic to Asia, the Middle East, Africa, the Mediterranean, and South and Central America. Clinical presentation varies, dependent on the pathogenicity of the species and the host’s immune response. Leishmania/Leishmaniasis | Trypanosoma | Trichomonas Trichomonas A genus of parasitic flagellate eukaryotes distinguished by the presence of four anterior flagella, an undulating membrane, and a trailing flagellum. Nitroimidazoles | |
|---|---|---|---|---|
| Characteristics |
|
|
|
|
| Forms |
|
|
|
|
| Transmission |
|
|
|
Sexually transmitted |
| Clinical | Giardiasis | Leishmaniasis Leishmaniasis Leishmania species are obligate intracellular parasites that are transmitted by an infected sandfly. The mildest form is cutaneous leishmaniasis (CL), characterized by painless skin ulcers. The mucocutaneous type involves more tissue destruction, causing deformities. Visceral leishmaniasis (VL), the most severe form, presents with hepatosplenomegaly, anemia, thrombocytopenia, and fever. Leishmania/Leishmaniasis |
|
Trichomoniasis |
| Diagnosis |
|
|
|
|
| Treatment |
|
Depends on the clinical syndrome:
|
Depends on the clinical disease:
|
|
| Prevention |
|
|
|
|
ELISA: enzyme-linked immunosorbent assay
DFA: direct immunofluorescence assay
NAAT: nucleic acid amplification assay
PCR: polymerase chain reaction
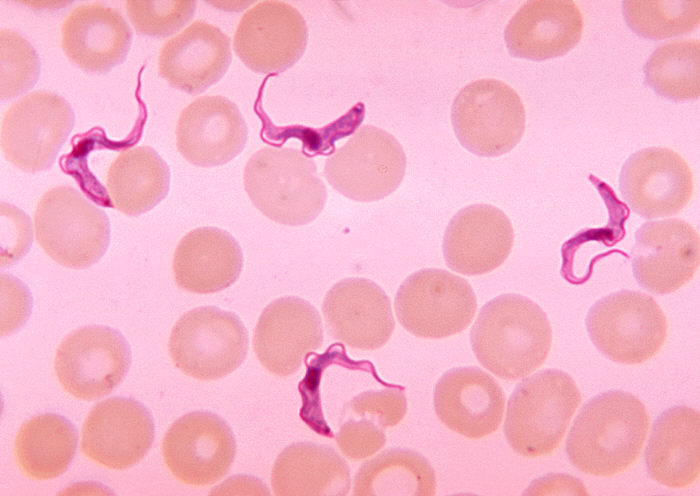
Blood smear demonstrating Trypanosoma trypomastigotes
Image: “Ms. Michaels forms” by CDC/Dr. Myron G. Schultz. License: Public Domain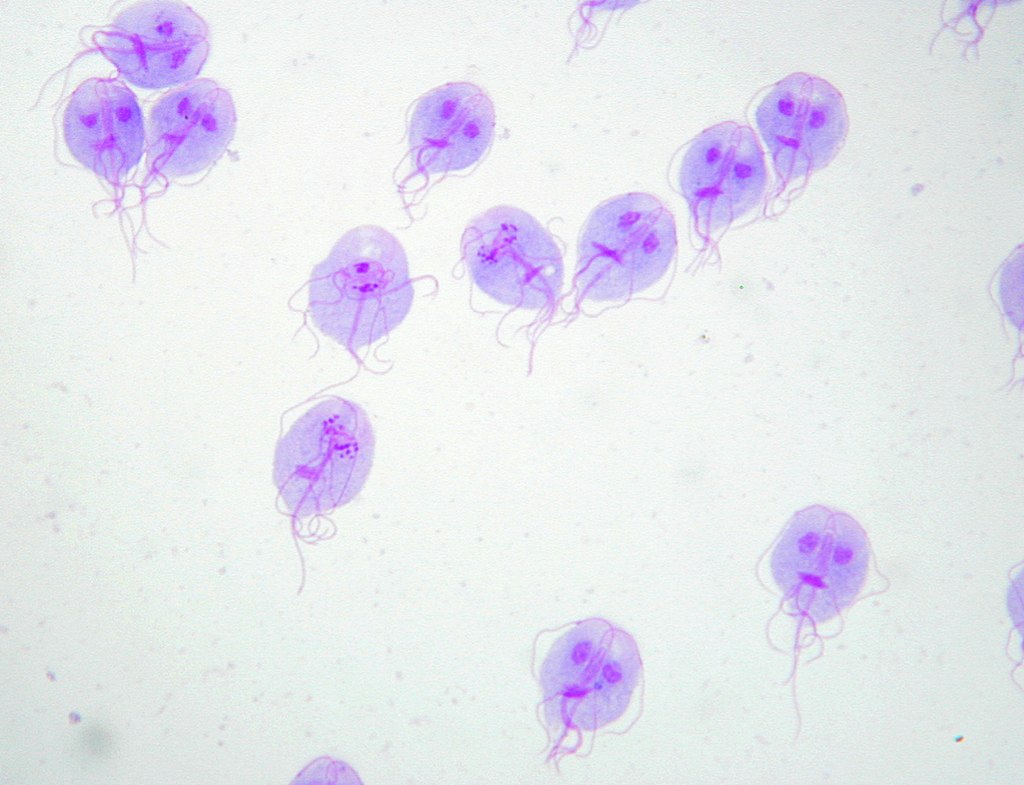
Giemsa’s stain of G. lamblia trophozoites
Image: “Trophozoites of Giardia lamblia” by Eva Nohýnková, Department of Tropical Medicine, 1st Faculty of Medicine, Charles University in Prague and Hospital Bulovka, Czech Republic. License: CC BY 4.0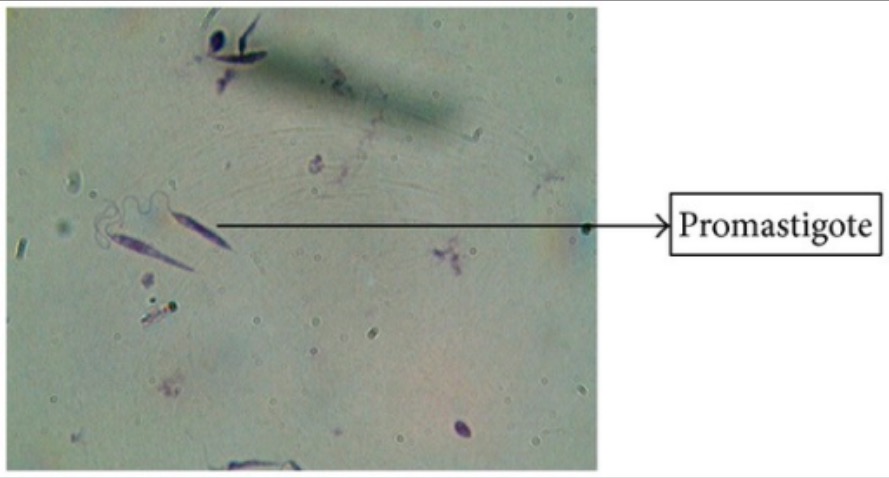
Giemsa’s stain of Leishmania promastigotes
Image: “Giemsa stain” by Arriyadh Community College, King Saud University, P.O. Box 28095, Riyadh 11437, Saudi Arabia. License: CC BY 3.0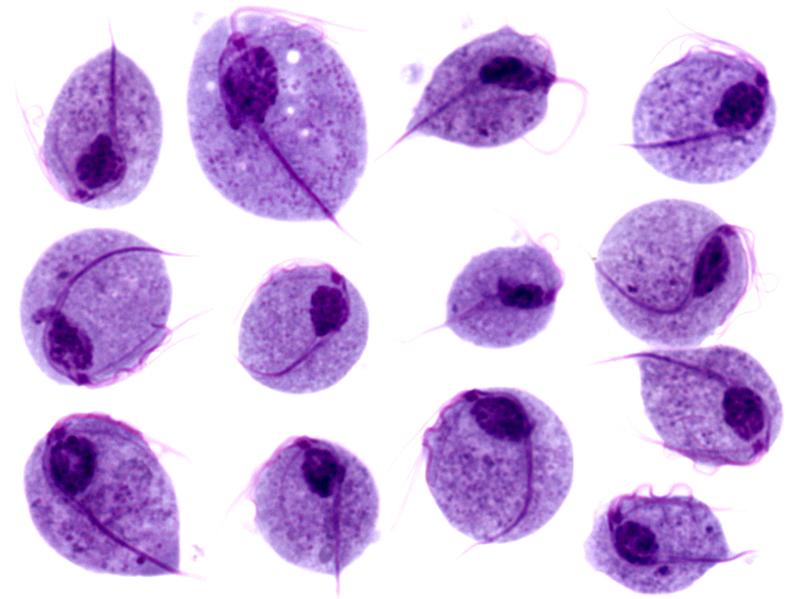
Microscopic images of Trichomonas vaginalis trophozoites
Image: “Trichomonas protozoa” by isis325. License: CC BY 2.0.