The stomach is a muscular sac in the upper left portion of the abdomen that plays a critical role in digestion Digestion Digestion refers to the process of the mechanical and chemical breakdown of food into smaller particles, which can then be absorbed and utilized by the body. Digestion and Absorption. The stomach develops from the foregut Foregut Development of the Abdominal Organs and connects the esophagus Esophagus The esophagus is a muscular tube-shaped organ of around 25 centimeters in length that connects the pharynx to the stomach. The organ extends from approximately the 6th cervical vertebra to the 11th thoracic vertebra and can be divided grossly into 3 parts: the cervical part, the thoracic part, and the abdominal part. Esophagus: Anatomy with the duodenum Duodenum The shortest and widest portion of the small intestine adjacent to the pylorus of the stomach. It is named for having the length equal to about the width of 12 fingers. Small Intestine: Anatomy. Structurally, the stomach is J-shaped and forms a greater and lesser curvature and is divided grossly into regions: the cardia, fundus, body, and pylorus. On a microscopic level, the stomach wall has several layers, including a mucosa, submucosa, muscularis, and serosa. The stomach is filled with glands that secrete a variety of substances involved in the digestive process. The arterial supply to the stomach is primarily from vessels originating from the celiac trunk.
Last updated: Nov 19, 2024
The stomach is a muscular sac in the upper abdomen that plays a critical role in digestion Digestion Digestion refers to the process of the mechanical and chemical breakdown of food into smaller particles, which can then be absorbed and utilized by the body. Digestion and Absorption.
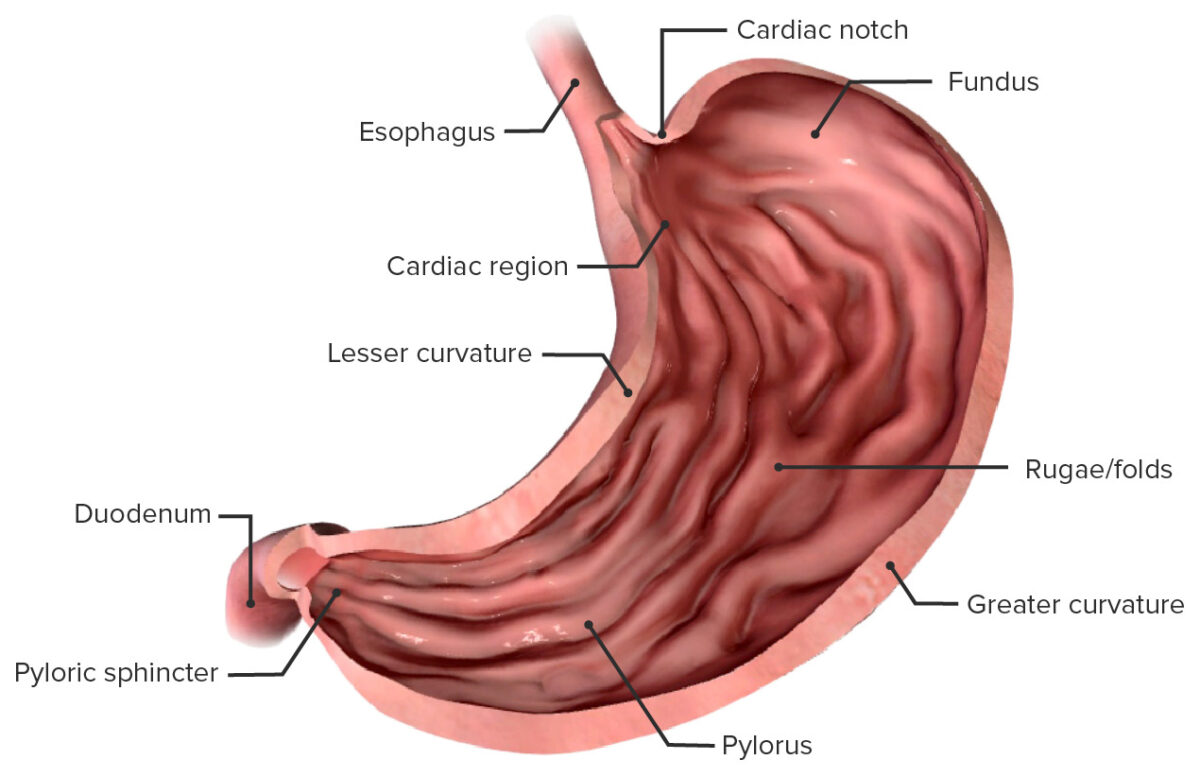
Anatomical components of the stomach
Image by BioDigital, edited by LecturioThe stomach is in direct contact with a number of other organs, including:
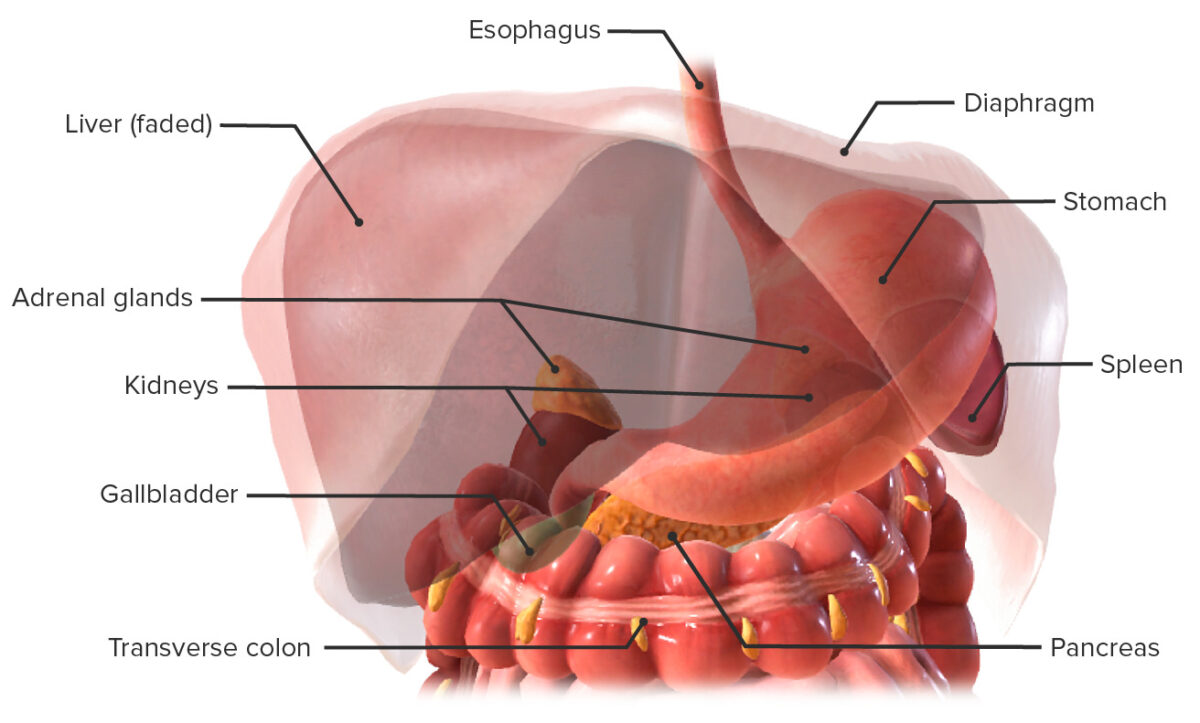
Stomach in situ and the relations to its neighboring structures
Image by BioDigital, edited by Lecturio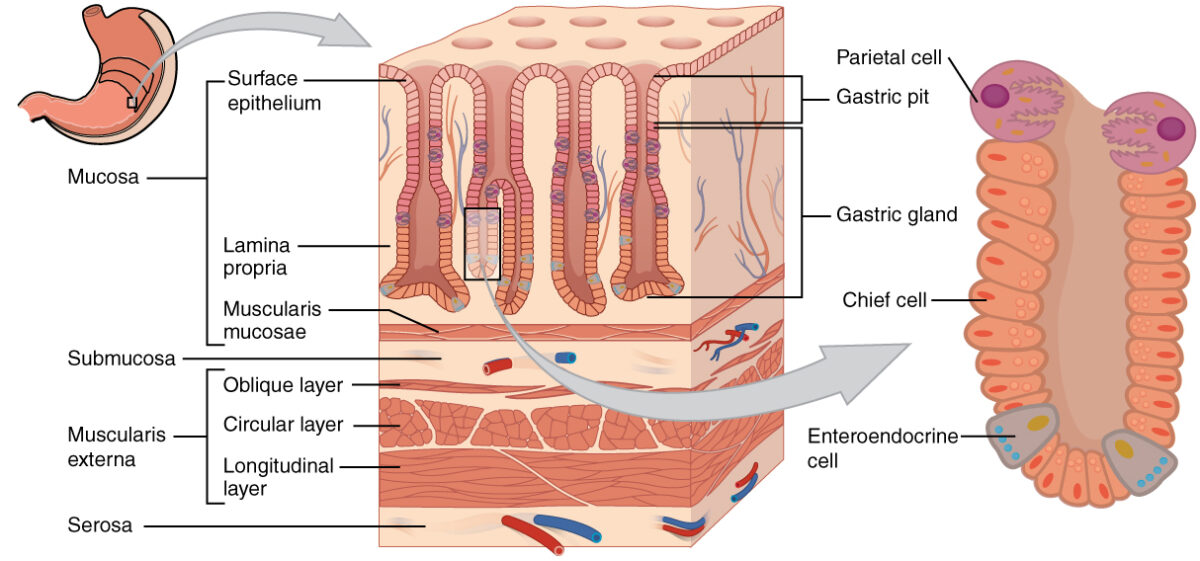
Layers of the stomach wall:
In the epithelium, gastric pits lead to gastric glands that secrete a variety of substances to aid in digestion.
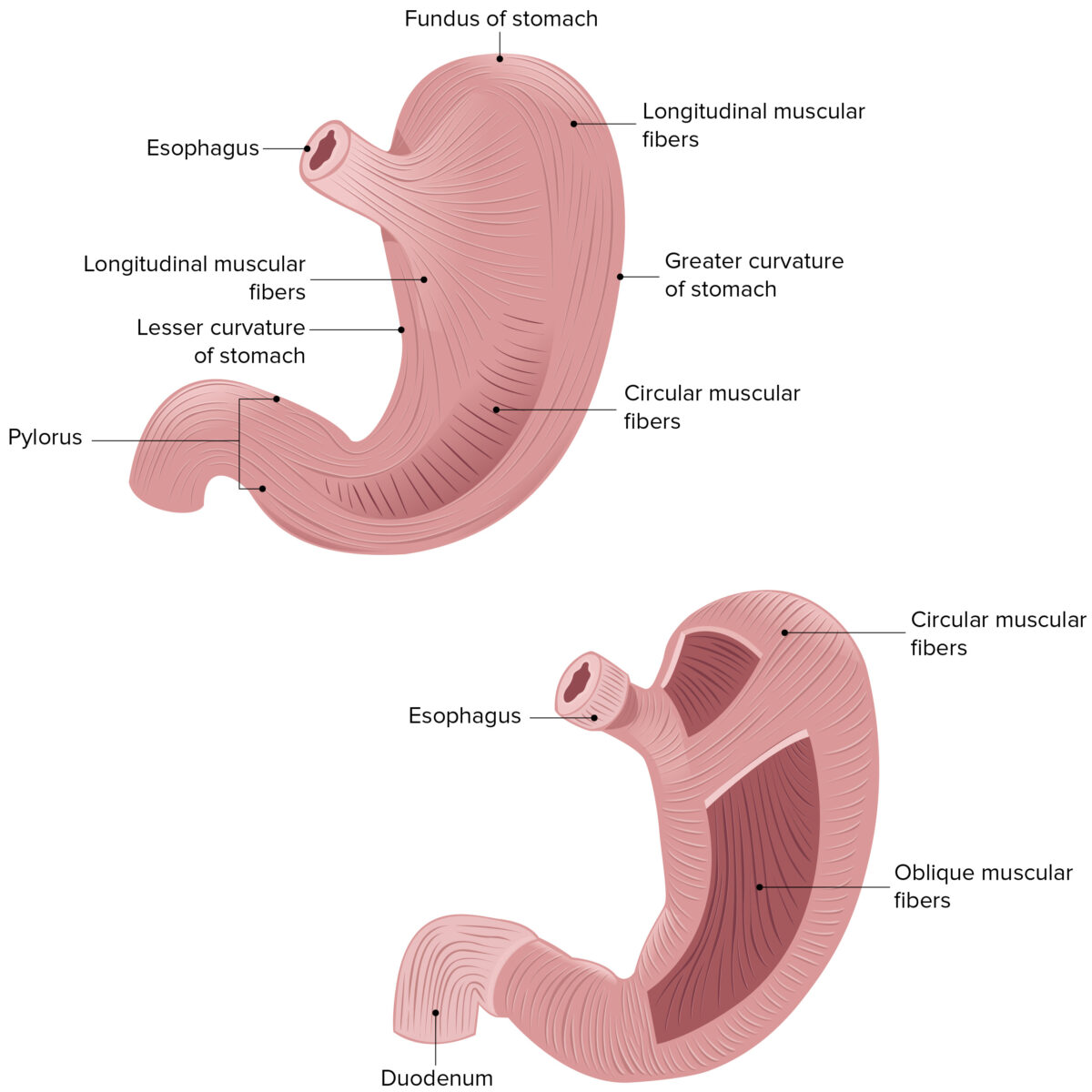
Image displaying the 3 muscular layers of the stomach wall
Image by Lecturio.General characteristics:
Types of glands:
Types of cells within the glands:
Comprises (from surface to deep):
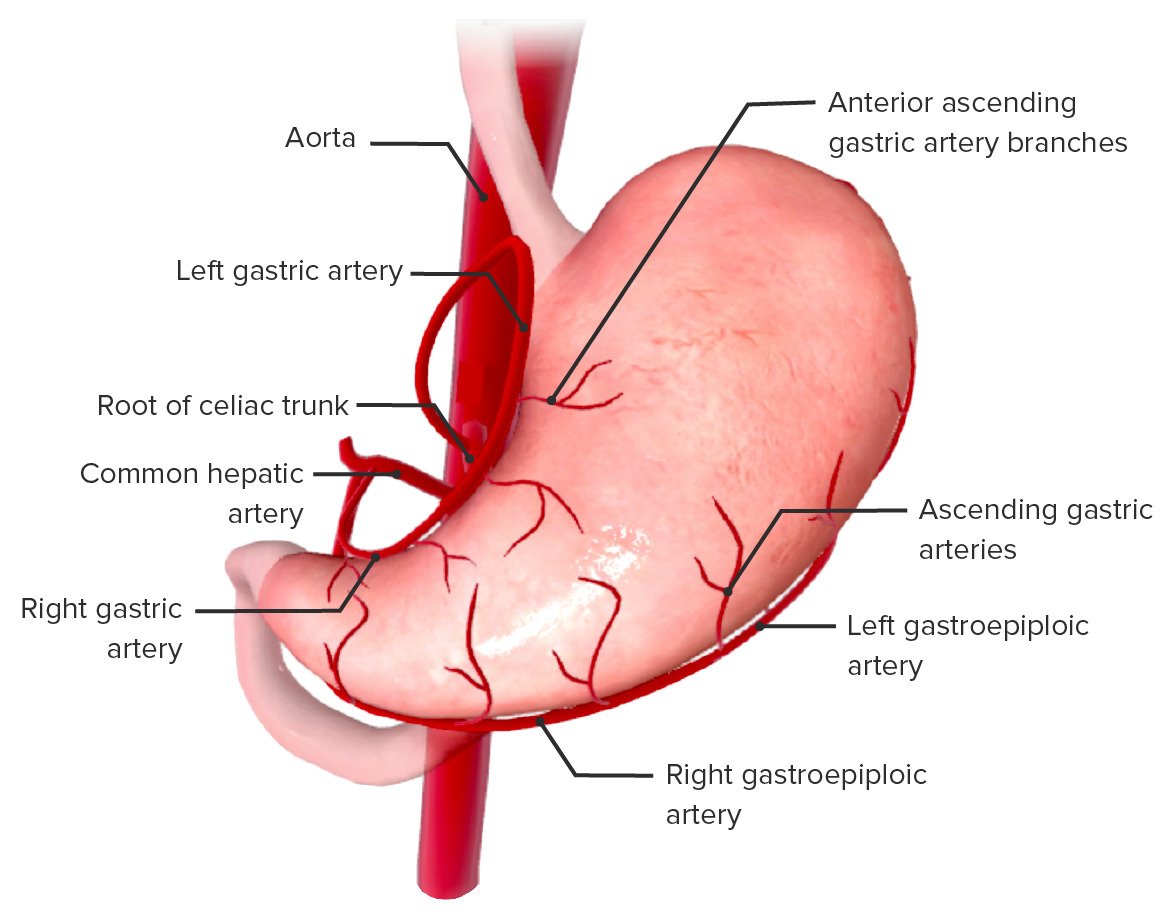
Image showing the blood supply of the stomach
Image by BioDigital, edited by Lecturio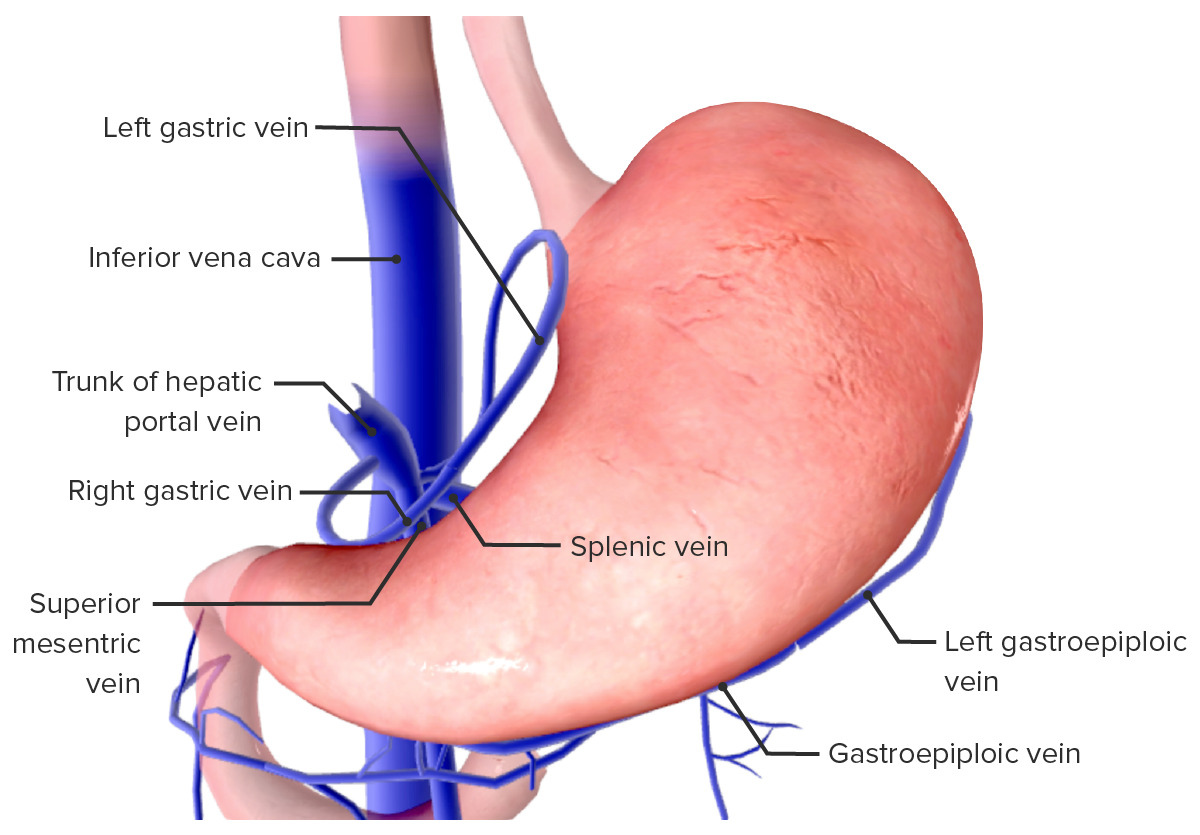
Venous drainage of the stomach
Image by BioDigital, edited by LecturioLymph nodes Lymph Nodes They are oval or bean shaped bodies (1 – 30 mm in diameter) located along the lymphatic system. Lymphatic Drainage System: Anatomy draining the stomach are arranged in a complex network.
The stomach is innervated by the autonomic nervous system Autonomic nervous system The ANS is a component of the peripheral nervous system that uses both afferent (sensory) and efferent (effector) neurons, which control the functioning of the internal organs and involuntary processes via connections with the CNS. The ANS consists of the sympathetic and parasympathetic nervous systems. Autonomic Nervous System: Anatomy.
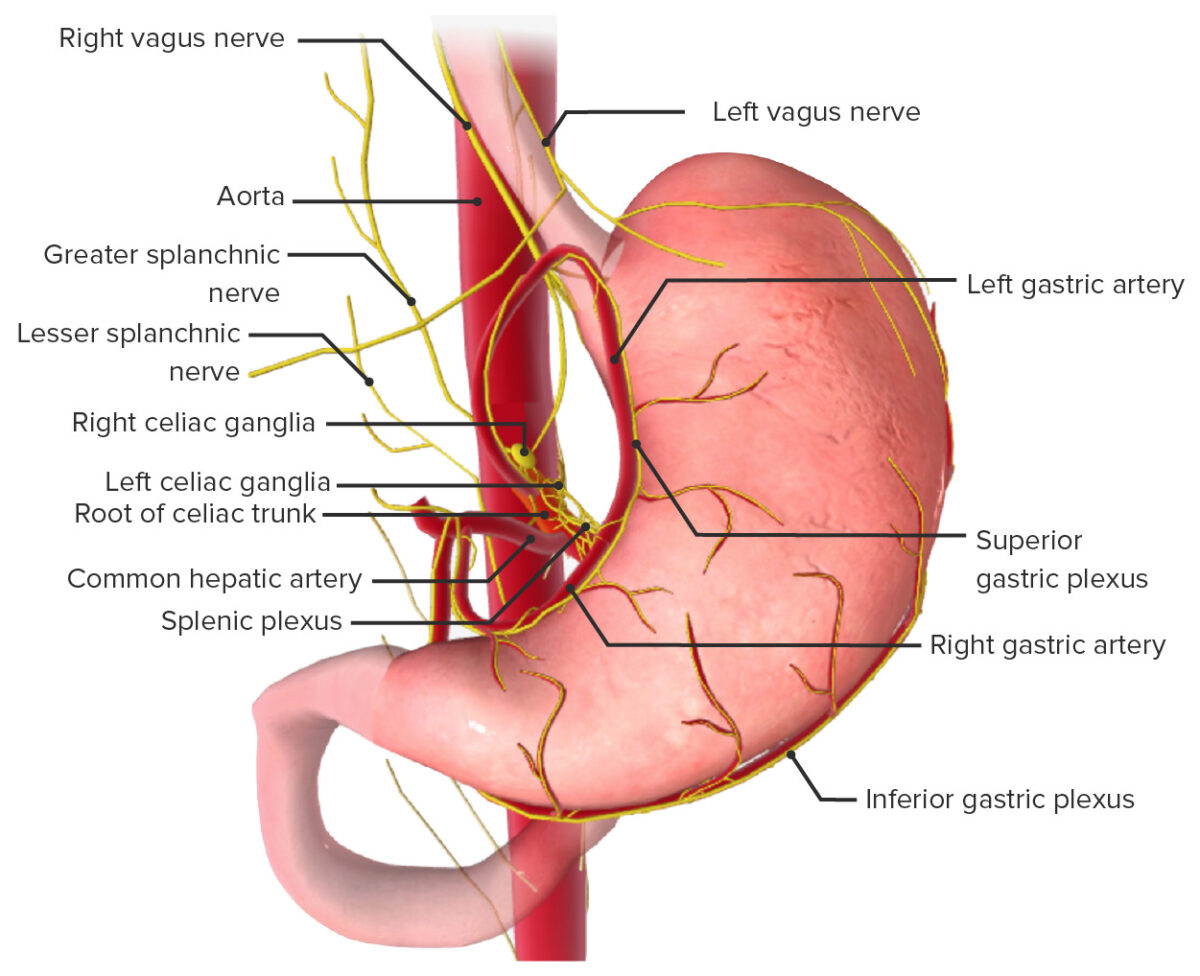
Innervation of the stomach
Image by BioDigital, edited by Lecturio