Penetrating abdominal injuries are created by an object puncturing the abdominal wall Abdominal wall The outer margins of the abdomen, extending from the osteocartilaginous thoracic cage to the pelvis. Though its major part is muscular, the abdominal wall consists of at least seven layers: the skin, subcutaneous fat, deep fascia; abdominal muscles, transversalis fascia, extraperitoneal fat, and the parietal peritoneum. Surgical Anatomy of the Abdomen. Injuries can be high velocity, like gunshot wounds Gunshot wounds Disruption of structural continuity of the body as a result of the discharge of firearms. Penetrating Chest Injury, or low velocity, like stab wounds. Different structures can be injured, including the duodenum Duodenum The shortest and widest portion of the small intestine adjacent to the pylorus of the stomach. It is named for having the length equal to about the width of 12 fingers. Small Intestine: Anatomy, spleen Spleen The spleen is the largest lymphoid organ in the body, located in the LUQ of the abdomen, superior to the left kidney and posterior to the stomach at the level of the 9th-11th ribs just below the diaphragm. The spleen is highly vascular and acts as an important blood filter, cleansing the blood of pathogens and damaged erythrocytes. Spleen: Anatomy, liver Liver The liver is the largest gland in the human body. The liver is found in the superior right quadrant of the abdomen and weighs approximately 1.5 kilograms. Its main functions are detoxification, metabolism, nutrient storage (e.g., iron and vitamins), synthesis of coagulation factors, formation of bile, filtration, and storage of blood. Liver: Anatomy, kidneys Kidneys The kidneys are a pair of bean-shaped organs located retroperitoneally against the posterior wall of the abdomen on either side of the spine. As part of the urinary tract, the kidneys are responsible for blood filtration and excretion of water-soluble waste in the urine. Kidneys: Anatomy, and pelvic organs. The extent and specific type of abdominal traumatic injury can be identified by a proper history and physical exam and supported by appropriate imaging studies. Management, which can be laparotomy Laparotomy Incision into the side of the abdomen between the ribs and pelvis. Laparotomy and Laparoscopy or a conservative approach, is dependent on the patient’s hemodynamic stability and specific type of injury.
Last updated: Dec 15, 2025
A penetrating abdominal injury is the result of trauma from an object puncturing the skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions, entering the body, and creating a wound.
Because of the wide variety and severity of injuries associated with penetrating abdominal trauma, a prompt but careful history and physical exam are necessary to direct investigation with imaging studies.
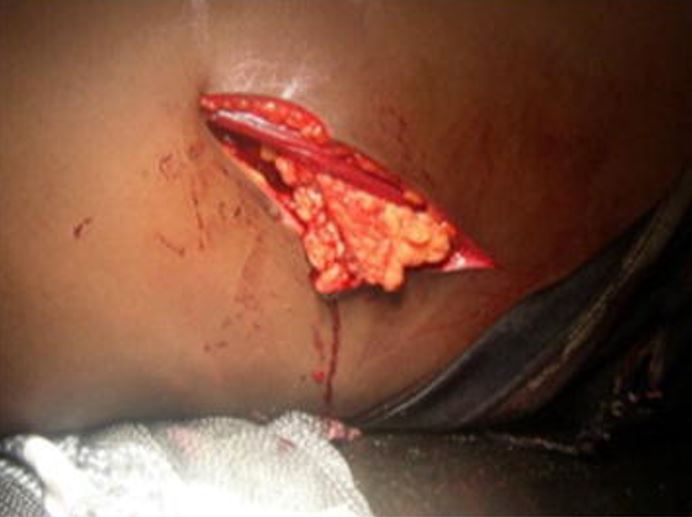
Penetrating injury: large left thoracoabdominal wound with epiplocele
Image: “Large left thoraco-abdominal wound with epiplocele” by SpringerPlus. License: CC BY 4.0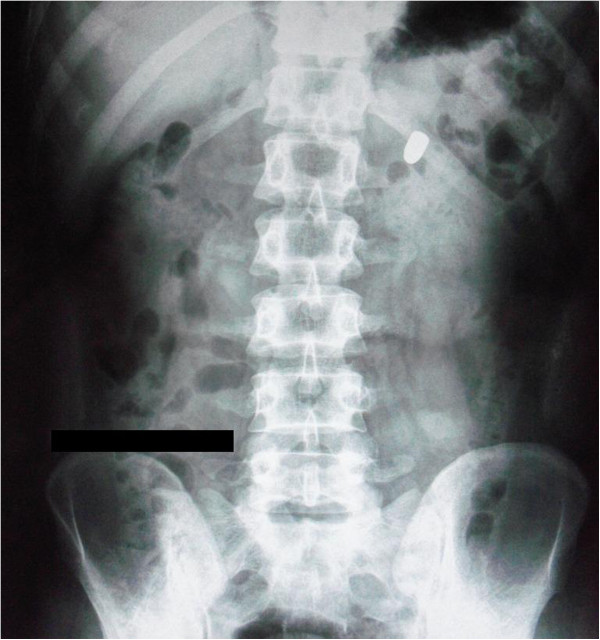
Erect abdominal radiograph:
Radiograph showing bullet in the upper left quadrant of the abdomen
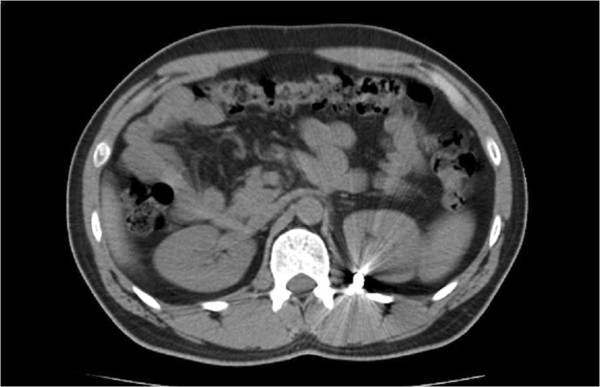
Transverse view of CT scan:
This view shows the bullet to be lodged posteromedially to the left kidney.
Penetrating injuries Penetrating injuries Wounds caused by objects penetrating the skin. Genitourinary Trauma may affect more than just the area that is obviously injured externally, and damage to the adjacent structures needs to be investigated.
Historical and standard management of penetrating abdominal trauma is laparotomy Laparotomy Incision into the side of the abdomen between the ribs and pelvis. Laparotomy and Laparoscopy. Recent improvements in imaging and better understanding of injury patterns have resulted in more-conservative strategies.
Assessment of patient stability, correlation Correlation Determination of whether or not two variables are correlated. This means to study whether an increase or decrease in one variable corresponds to an increase or decrease in the other variable. Causality, Validity, and Reliability with diagnostic tests Diagnostic tests Diagnostic tests are important aspects in making a diagnosis. Some of the most important epidemiological values of diagnostic tests include sensitivity and specificity, false positives and false negatives, positive and negative predictive values, likelihood ratios, and pre-test and post-test probabilities. Epidemiological Values of Diagnostic Tests, and determination of the need for immediate surgery:
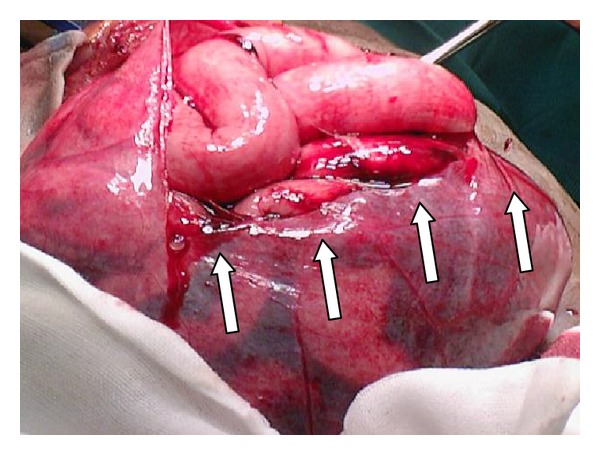
Stab wound injury: On laparotomy, multiple small bowel perforations (arrows) were evident.
Image: “Multiple small bowel perforations (indicated by arrows)” by Naidoo K, Mewa Kinoo S, Singh B. License: CC BY 3.0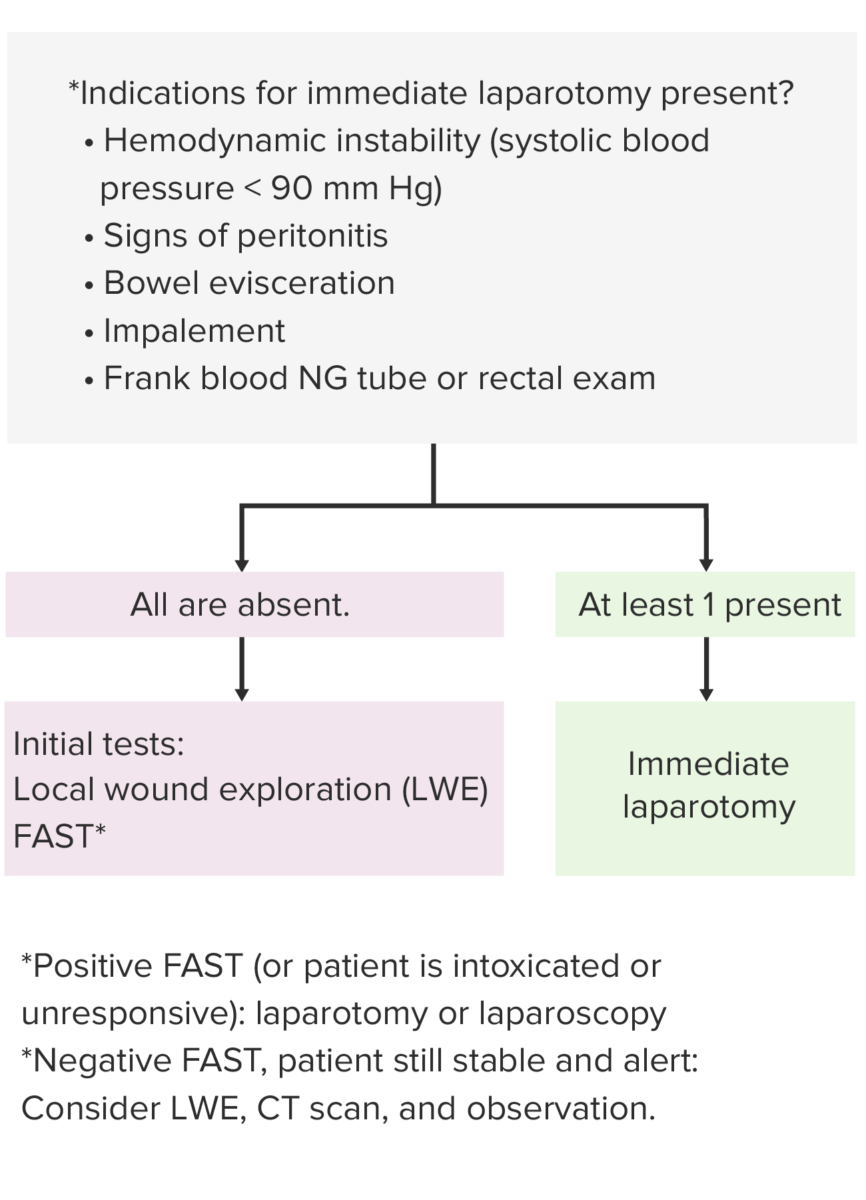
Algorithm of management of penetrating abdominal injury
Abbreviations: BP: blood pressure; FAST: Focused Assessment with Sonography for Trauma; LWE: local wound exploration; CT: computed tomography