Corynebacteria are gram-positive Gram-Positive Penicillins, club-shaped bacilli Bacilli Shigella. Corynebacteria are commonly isolated on tellurite Tellurite Diphtheria or Loeffler media and have characteristic metachromatic granules. The major pathogenic species is Corynebacterium diphtheriae Corynebacterium diphtheriae Diphtheria is an infectious disease caused by corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria, which causes diphtheria Diphtheria Diphtheria is an infectious disease caused by Corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria—a severe upper respiratory infection Upper respiratory infection Rhinitis. The characteristic findings of diphtheria Diphtheria Diphtheria is an infectious disease caused by Corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria include pharyngeal pseudomembranes Pseudomembranes Raised yellow or off-white plaques up to 2 cm in diameter that form as a result of mucosal ulceration Pseudomembranous Colitis (grayish tonsillar exudates), severe pharyngitis Pharyngitis Pharyngitis is an inflammation of the back of the throat (pharynx). Pharyngitis is usually caused by an upper respiratory tract infection, which is viral in most cases. It typically results in a sore throat and fever. Other symptoms may include a runny nose, cough, headache, and hoarseness. Pharyngitis, and “bull’s neck Neck The part of a human or animal body connecting the head to the rest of the body. Peritonsillar Abscess” lymphadenopathy Lymphadenopathy Lymphadenopathy is lymph node enlargement (> 1 cm) and is benign and self-limited in most patients. Etiologies include malignancy, infection, and autoimmune disorders, as well as iatrogenic causes such as the use of certain medications. Generalized lymphadenopathy often indicates underlying systemic disease. Lymphadenopathy. Treatment is primarily through passive immunization Passive immunization Transfer of immunity from immunized to non-immune host by administration of serum antibodies, or transplantation of lymphocytes (adoptive transfer). Vaccination with antitoxin and antibiotics. Prevention is via the diphtheria Diphtheria Diphtheria is an infectious disease caused by Corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria toxoid Toxoid Preparations of pathogenic organisms or their derivatives made nontoxic and intended for active immunologic prophylaxis. They include deactivated toxins. Anatoxin toxoids are distinct from anatoxins that are tropanes found in cyanobacteria. Vaccination vaccine Vaccine Suspensions of killed or attenuated microorganisms (bacteria, viruses, fungi, protozoa), antigenic proteins, synthetic constructs, or other bio-molecular derivatives, administered for the prevention, amelioration, or treatment of infectious and other diseases. Vaccination.
Last updated: Dec 15, 2025
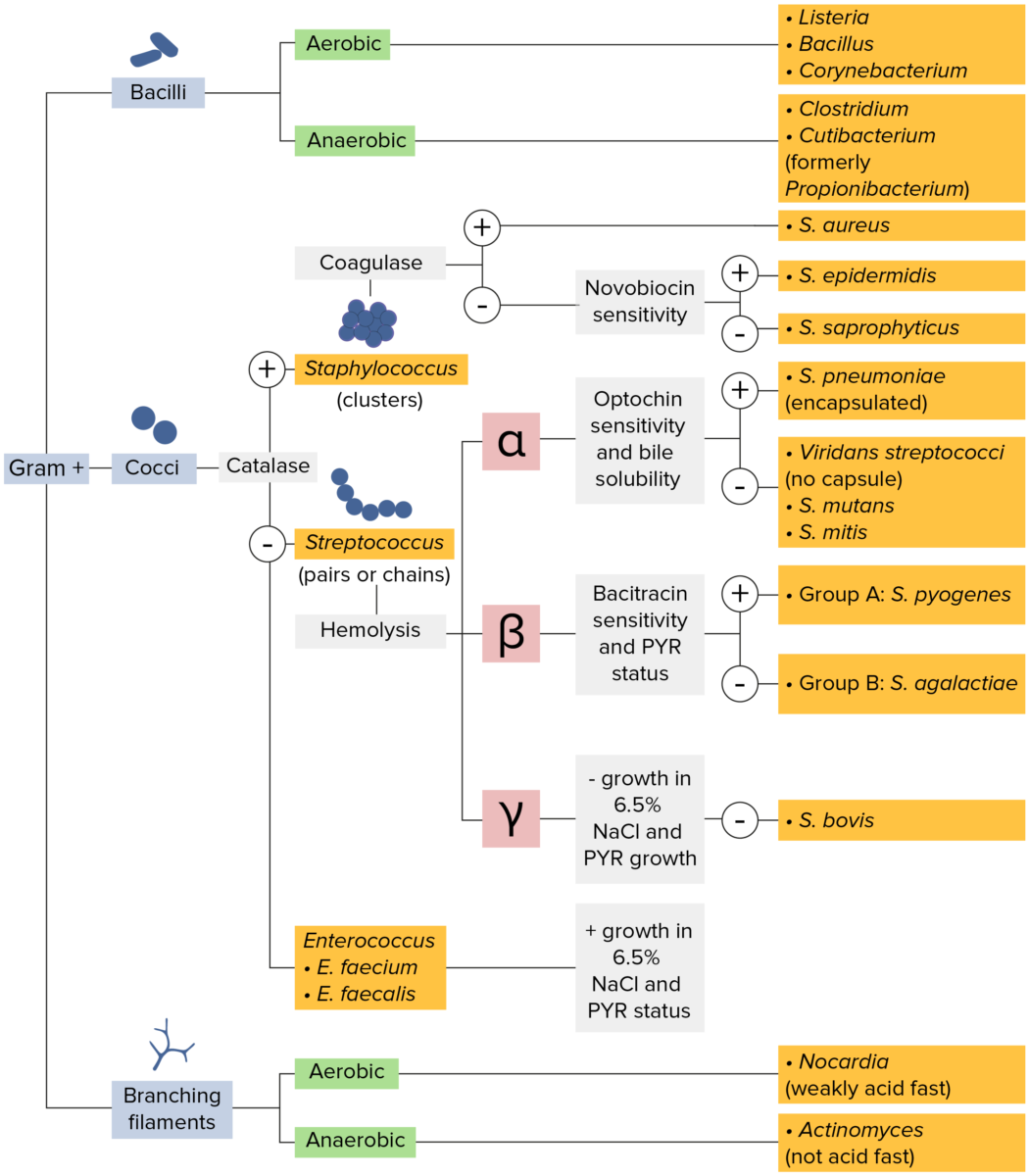
Gram-positive bacteria:
Most bacteria can be classified according to a lab procedure called Gram staining.
Bacteria with cell walls that have a thick layer of peptidoglycan retain the crystal violet stain utilized in Gram staining but are not affected by the safranin counterstain. These bacteria appear as purple-blue on the stain, indicating that they are gram positive. The bacteria can be further classified according to morphology (branching filaments, bacilli, and cocci in clusters or chains) and their ability to grow in the presence of oxygen (aerobic versus anaerobic). The cocci can also be further identified. Staphylococci can be narrowed down on the basis of the presence of the enzyme coagulase and on their sensitivity to the antibiotic novobiocin. Streptococci are grown on blood agar and classified on the basis of which form of hemolysis they employ (α, β, or γ). Streptococci are further narrowed on the basis of their response to the pyrrolidonyl-β-naphthylamide (PYR) test, their sensitivity to specific antimicrobials (optochin and bacitracin), and their ability to grow on sodium chloride (NaCl) media.
General characteristics of Corynebacterium species include:
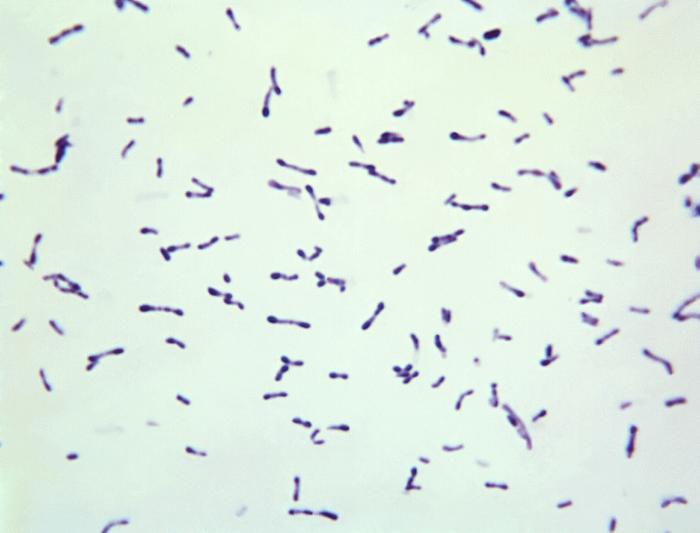
Micrograph of Corynebacterium diphtheriae
Image: “12163” by the CDC/Graham Heid. License: Public domain.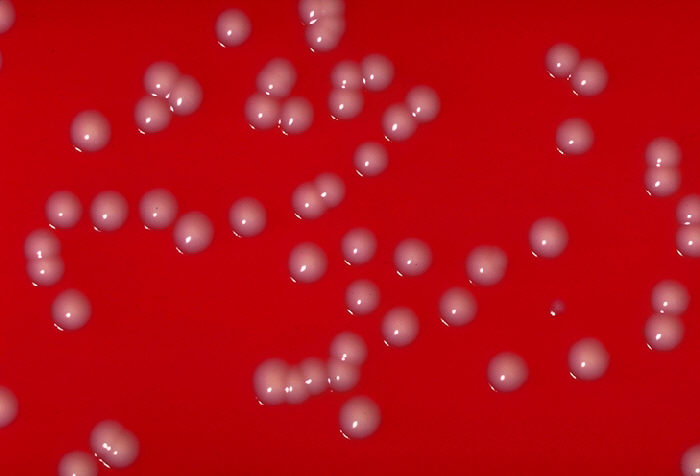
Corynebacterium ulcerans colonies on a blood agar plate
Image: “Corynebacterium ulcerans 01” by the CDC/Dr. W.A. Clark. License: Public domain.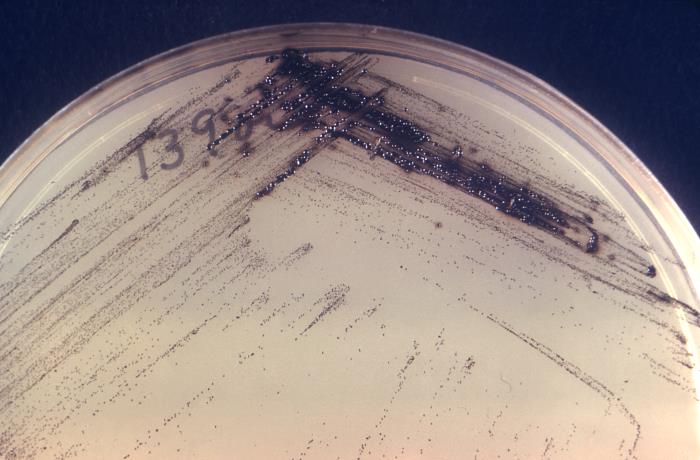
Corynebacterium diphtheriae on Tinsdale’s agar plate
Image: “16561” by the CDC. License: Public domain.Diphtheria Diphtheria Diphtheria is an infectious disease caused by Corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria (respiratory):
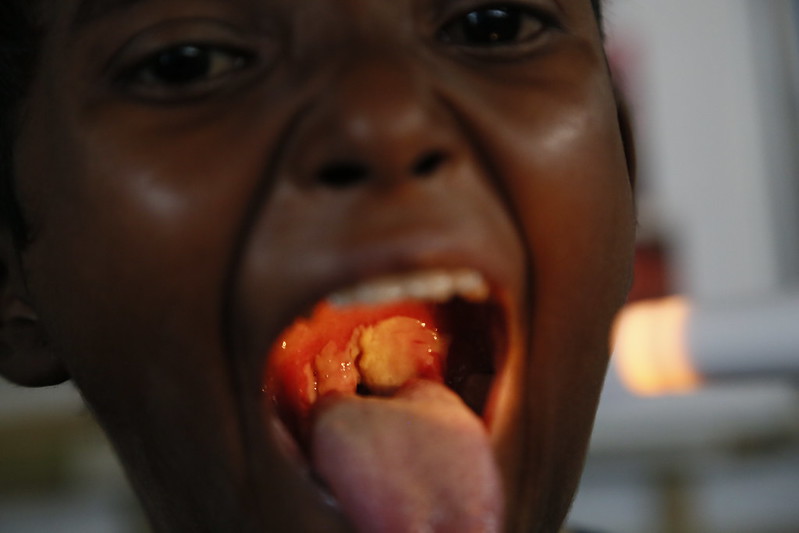
Diphtheria: pediatric patient with diphtheria presenting with the characteristic grayish-white membrane covering the posterior pharyngeal wall
Image: “39015940254_849c8705a0_c” by Russell Watkins/Department for International Development. License: CC BY 2.0.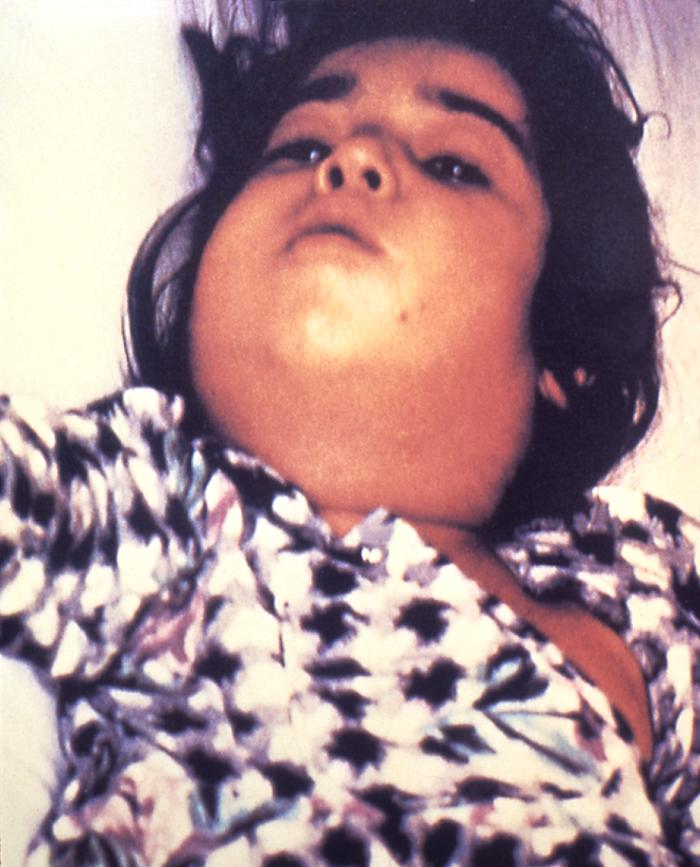
Patient infected by Corynebacterium: severe lymphadenopathy, known as “bull’s neck”
Image: “5325” by CDC. License: Public domain.Complications/systemic toxemia:
Cutaneous (wound) diphtheria Diphtheria Diphtheria is an infectious disease caused by Corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria:
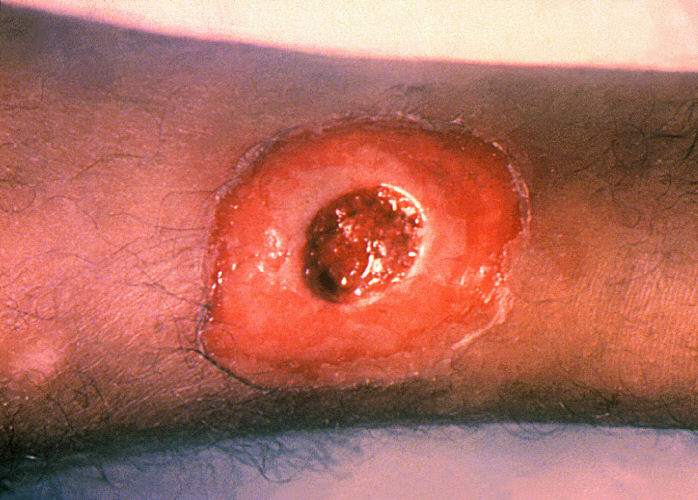
Cutaneous diphtheria: chronic non-healing ulcer
Image: “1941” by the CDC. License: Public domain.“ABCDEFGs of Corynebacterium diphtheriae Corynebacterium diphtheriae Diphtheria is an infectious disease caused by corynebacterium diphtheriae that most often results in respiratory disease with membranous inflammation of the pharynx, sore throat, fever, swollen glands, and weakness. The hallmark sign is a sheet of thick, gray material covering the back of the throat. Diphtheria”: