Strabismus is the misalignment of the eyes while fixating the gaze on an object. Strabismus can be idiopathic Idiopathic Dermatomyositis, but it may also be caused by cerebral palsy Palsy paralysis of an area of the body, thus incapable of voluntary movement Cranial Nerve Palsies, uncorrected refractive errors Refractive errors By refraction, the light that enters the eye is focused onto a particular point of the retina. The main refractive components of the eye are the cornea and the lens. When the corneal curvature, the refractive power of the lens, does not match the size of the eye, ametropia or a refractive error occurs. Refractive Errors, and extraocular muscle or cranial nerve dysfunction. Clinical presentation may include vertical or horizontal diplopia Diplopia A visual symptom in which a single object is perceived by the visual cortex as two objects rather than one. Disorders associated with this condition include refractive errors; strabismus; oculomotor nerve diseases; trochlear nerve diseases; abducens nerve diseases; and diseases of the brain stem and occipital lobe. Myasthenia Gravis (double vision Vision Ophthalmic Exam). Diagnosis of strabismus is established clinically with the eye cover–uncover test. Management includes therapy with cycloplegic eye drops, eye patching, or surgery. Untreated strabismus can lead to amblyopia, which is reduced vision Vision Ophthalmic Exam with no structural defect.
Last updated: Jun 21, 2025
Strabismus is the misalignment of the eyes in any direction (vertical, horizontal). Colloquially, it is referred to as “crossed eyes.”
Strabismus can be classified as:
Medical terminology describes the direction of eye deviation:
Other considerations:
Most strabismus results from an abnormality of the neuromuscular control of eye movement. Less commonly, there is a problem with the extraocular muscles.
Strabismus presents as:

Esotropia (inward deviation) of the right eye:
The light reflex is central in the left eye (the nondeviated eye) but over the iris in the right eye (the deviated eye).

Exotropia (outward deviation) of the right eye
Image: “This boy’s right eye is deviated outwards, an example of exotropia” by Helveston, E.M. License: CC BY 2.0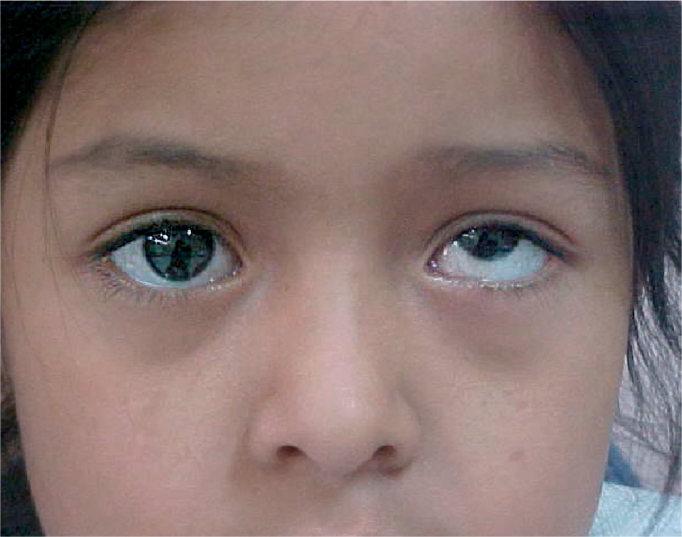
The left eye is higher in this girl with hypertropia, a vertical deviation
Image: “Understanding, detecting, and managing strabismus” by Helveston, E.M. License: CC BY 2.0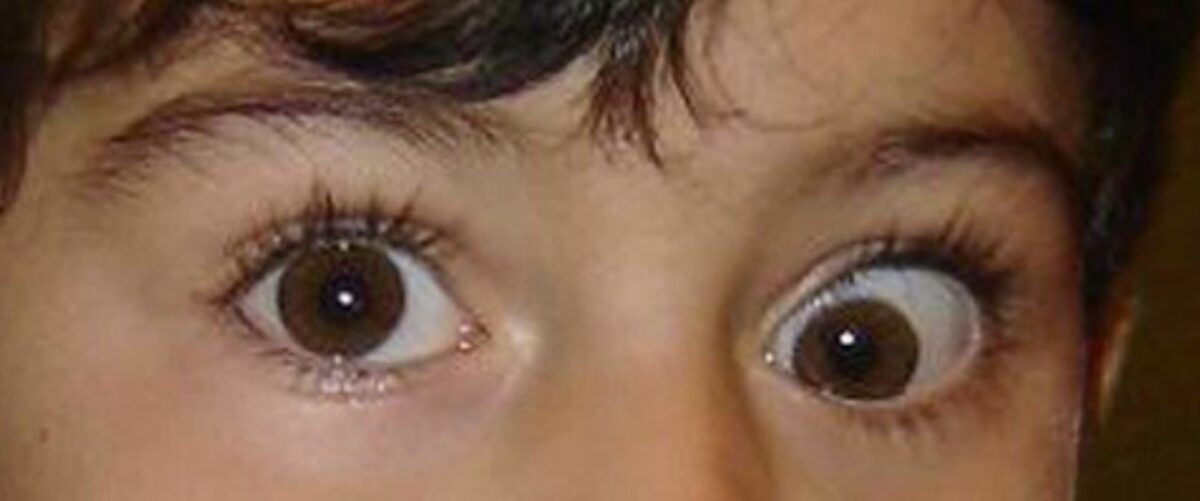
Hypotropia (downward deviation) of the right eye
Image: “Deficit of elevation in adduction of the LE” by Manzotti F, Menozzi C, Porta MR, Orsoni JG. License: CC BY 2.0There are several historical factors to consider in determining the cause and treatment of strabismus.
Abnormal eye examination or strabismus noted on testing in a child should be referred to a pediatric ophthalmologist.