Yersinia is a genus of bacteria Bacteria Bacteria are prokaryotic single-celled microorganisms that are metabolically active and divide by binary fission. Some of these organisms play a significant role in the pathogenesis of diseases. Bacteriology characterized as gram-negative bacilli Bacilli Shigella that are facultative anaerobic with bipolar Bipolar Nervous System: Histology staining. There are 2 enteropathogenic species that cause yersiniosis, Y. enterocolitica and Y. pseudotuberculosis. Infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease are manifested as pseudoappendicitis or mesenteric lymphadenitis Mesenteric Lymphadenitis Inflammation of lymph nodes in the mesentery. Pediatric Gastrointestinal Abnormalities, and enterocolitis. The bacteria Bacteria Bacteria are prokaryotic single-celled microorganisms that are metabolically active and divide by binary fission. Some of these organisms play a significant role in the pathogenesis of diseases. Bacteriology are transmitted through consumption of contaminated food products or water. Manifestations include fever Fever Fever is defined as a measured body temperature of at least 38°C (100.4°F). Fever is caused by circulating endogenous and/or exogenous pyrogens that increase levels of prostaglandin E2 in the hypothalamus. Fever is commonly associated with chills, rigors, sweating, and flushing of the skin. Fever, abdominal pain Abdominal Pain Acute Abdomen, and/or diarrhea Diarrhea Diarrhea is defined as ≥ 3 watery or loose stools in a 24-hour period. There are a multitude of etiologies, which can be classified based on the underlying mechanism of disease. The duration of symptoms (acute or chronic) and characteristics of the stools (e.g., watery, bloody, steatorrheic, mucoid) can help guide further diagnostic evaluation. Diarrhea. The gastrointestinal illness is usually self-limiting Self-Limiting Meningitis in Children. Antibiotics are given for severe infection and in immunocompromised immunocompromised A human or animal whose immunologic mechanism is deficient because of an immunodeficiency disorder or other disease or as the result of the administration of immunosuppressive drugs or radiation. Gastroenteritis patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship.
Last updated: Dec 15, 2025
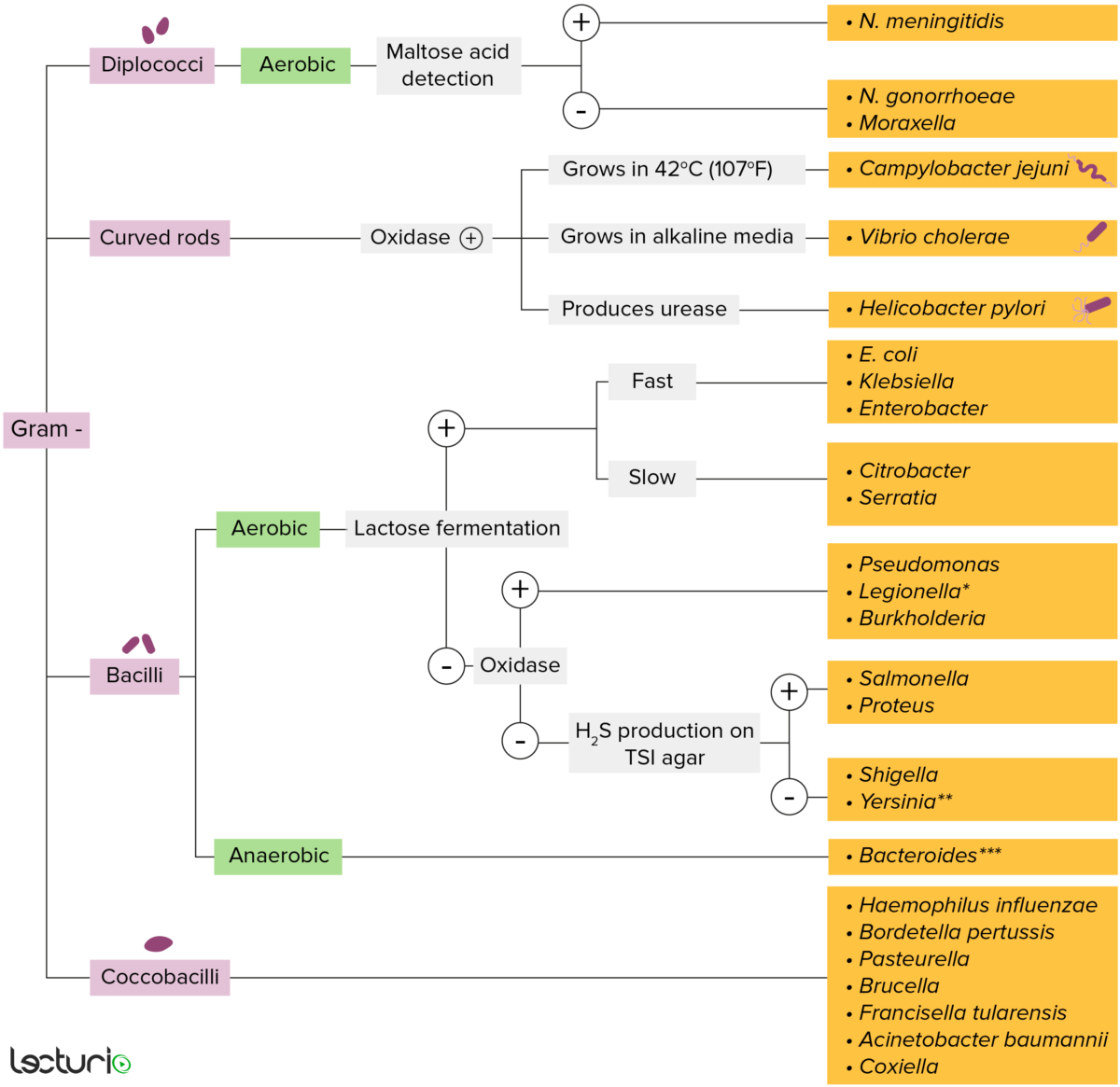
Gram-negative bacteria:
Most bacteria can be classified according to a lab procedure called Gram staining.
Bacteria with cell walls that have a thin layer of peptidoglycan do not retain the crystal violet stain utilized in Gram staining. These bacteria do, however, retain the safranin counterstain and thus appear as pinkish-red on the stain, making them gram negative. These bacteria can be further classified according to morphology (diplococci, curved rods, bacilli, and coccobacilli) and their ability to grow in the presence of oxygen (aerobic versus anaerobic). The bacteria can be more narrowly identified by growing them on specific media (triple sugar iron (TSI) agar) where their enzymes can be identified (urease, oxidase) and their ability to ferment lactose can be tested.
* Stains poorly on Gram stain
** Pleomorphic rod/coccobacillus
*** Require special transport media
Yersinia cause disease in animals Animals Unicellular or multicellular, heterotrophic organisms, that have sensation and the power of voluntary movement. Under the older five kingdom paradigm, animalia was one of the kingdoms. Under the modern three domain model, animalia represents one of the many groups in the domain eukaryota. Cell Types: Eukaryotic versus Prokaryotic; humans are usually incidental hosts. Three species are pathogenic to humans:
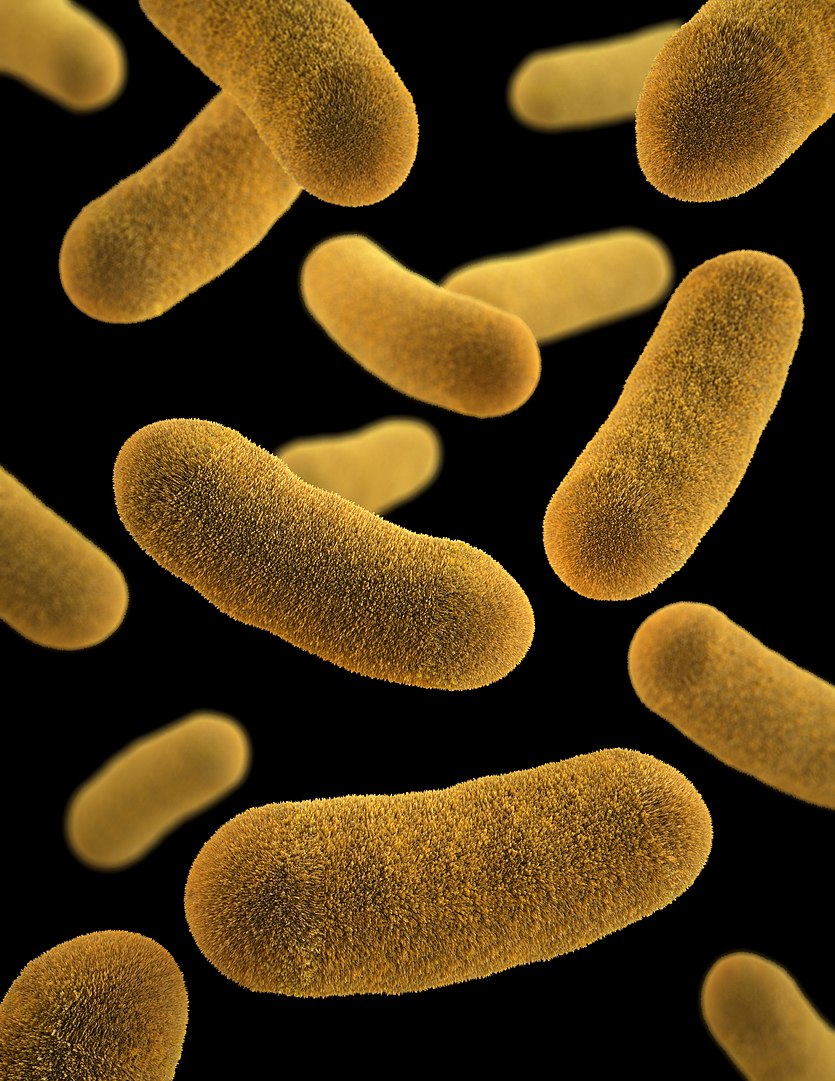
Three-dimensional (3D) computer-generated image of oblong-shaped Y. enterocolitica
Image: “3D computer generated image of Yersinia enterocolita” by Jennifer Oosthuizen. License: Public domain.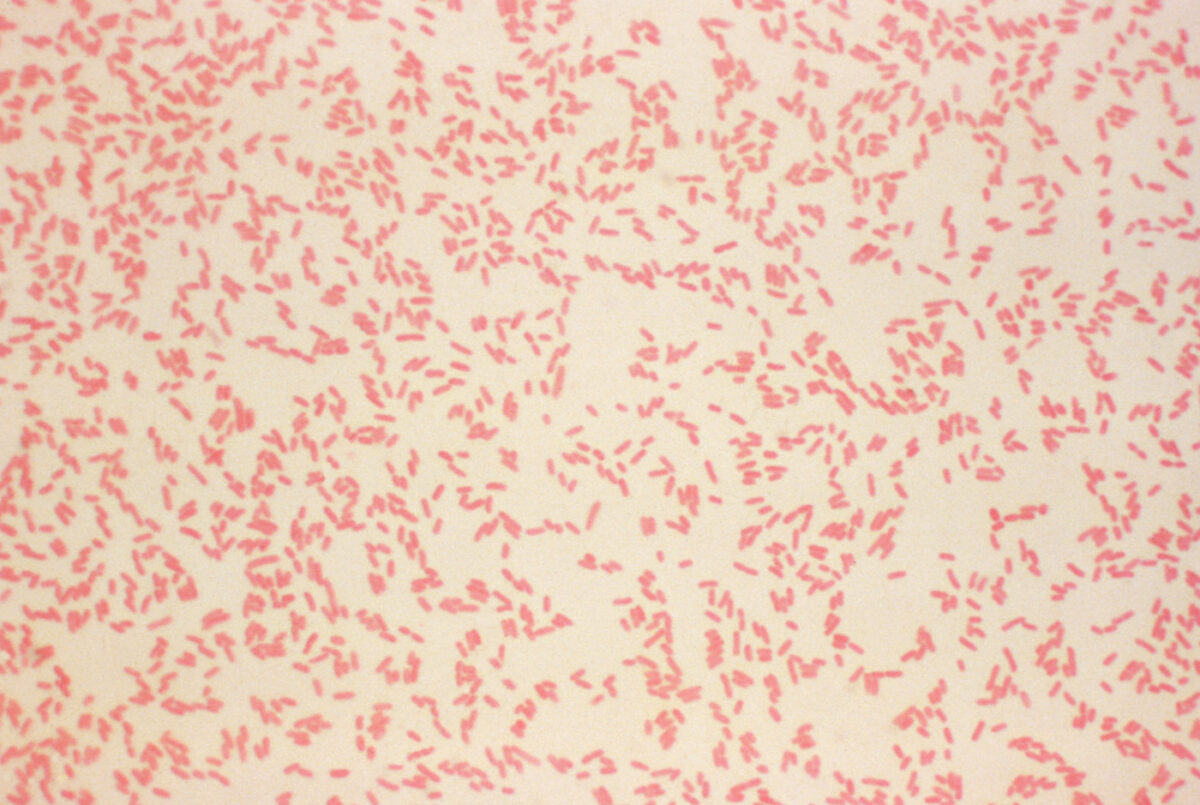
Yersinia enterocolitica: a photomicrograph of a gram-stained culture revealing the presence of numerous gram-negative Y. enterocolitica bacteria
Image: “Yersinia enterocolitica gram” by the CDC. License: Public domain.