Human papillomavirus (HPV) is a nonenveloped, circular, double-stranded DNA DNA A deoxyribonucleotide polymer that is the primary genetic material of all cells. Eukaryotic and prokaryotic organisms normally contain DNA in a double-stranded state, yet several important biological processes transiently involve single-stranded regions. DNA, which consists of a polysugar-phosphate backbone possessing projections of purines (adenine and guanine) and pyrimidines (thymine and cytosine), forms a double helix that is held together by hydrogen bonds between these purines and pyrimidines (adenine to thymine and guanine to cytosine). DNA Types and Structure virus Virus Viruses are infectious, obligate intracellular parasites composed of a nucleic acid core surrounded by a protein capsid. Viruses can be either naked (non-enveloped) or enveloped. The classification of viruses is complex and based on many factors, including type and structure of the nucleoid and capsid, the presence of an envelope, the replication cycle, and the host range. Virology belonging to the Papillomaviridae family. Humans are the only reservoir Reservoir Animate or inanimate sources which normally harbor disease-causing organisms and thus serve as potential sources of disease outbreaks. Reservoirs are distinguished from vectors (disease vectors) and carriers, which are agents of disease transmission rather than continuing sources of potential disease outbreaks. Humans may serve both as disease reservoirs and carriers. Escherichia coli, and transmission occurs through close skin-to-skin or sexual contact. Human papillomaviruses infect basal epithelial cells and can affect cell-regulatory proteins Proteins Linear polypeptides that are synthesized on ribosomes and may be further modified, crosslinked, cleaved, or assembled into complex proteins with several subunits. The specific sequence of amino acids determines the shape the polypeptide will take, during protein folding, and the function of the protein. Energy Homeostasis to result in cell proliferation. There are > 200 genotypes that can cause several conditions, including cutaneous warts Warts Benign epidermal proliferations or tumors; some are viral in origin. Female Genitourinary Examination, anogenital warts Warts Benign epidermal proliferations or tumors; some are viral in origin. Female Genitourinary Examination, and neoplasms Neoplasms New abnormal growth of tissue. Malignant neoplasms show a greater degree of anaplasia and have the properties of invasion and metastasis, compared to benign neoplasms. Benign Bone Tumors.
Last updated: May 21, 2025
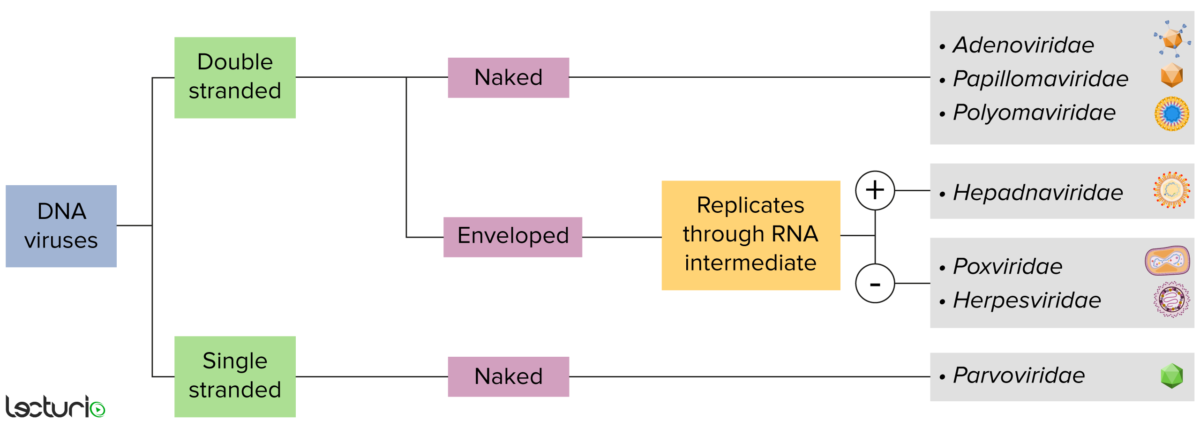
DNA virus identification:
Viruses can be classified in many ways. Most viruses, however, will either have a genome formed by DNA or RNA. Viruses with a DNA genome can be further characterized by whether that DNA is single or double stranded. If the viruses are covered by a thin coat of cell membrane (usually taken from the host cell), they are called “enveloped” viruses. If that coat is absent, the viruses are called “naked” viruses. Some of the enveloped viruses translate their DNA into RNA before it is incorporated into the host cell’s genome.
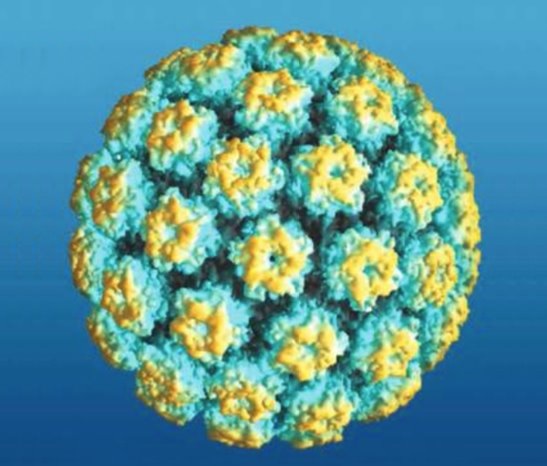
A scanning electron microscope model of the human papillomavirus
Image: “An atomic model of human papillomavirus” by Zhao et al; BioMed Central Ltd. License: CC BY 2.0There are > 200 HPV genotypes. The notable genotypes include:
Humans are the only reservoir Reservoir Animate or inanimate sources which normally harbor disease-causing organisms and thus serve as potential sources of disease outbreaks. Reservoirs are distinguished from vectors (disease vectors) and carriers, which are agents of disease transmission rather than continuing sources of potential disease outbreaks. Humans may serve both as disease reservoirs and carriers. Escherichia coli.
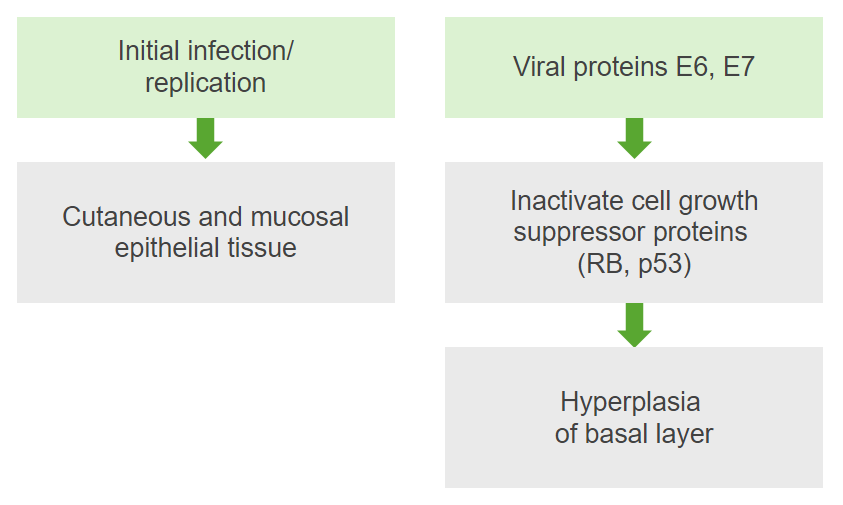
Diagram summarizing the pathophysiology of a human papillomavirus infection
Image by Lecturio. License: CC BY-NC-SA 4.0| Notable genotypes | Disease | Clinical features |
|---|---|---|
| 1, 2, 3, 4, 10, 27, 57 | Cutaneous
warts
Warts
Benign epidermal proliferations or tumors; some are viral in origin.
Female Genitourinary Examination:
|
|
| 6 and 11 | Anogenital warts Warts Benign epidermal proliferations or tumors; some are viral in origin. Female Genitourinary Examination ( condylomata acuminata Condylomata Acuminata Condylomata acuminata are a clinical manifestation of genital HPV infection. Condylomata acuminata are described as raised, pearly, flesh-colored, papular, cauliflower-like lesions seen in the anogenital region that may cause itching, pain, or bleeding. Condylomata Acuminata (Genital Warts)) |
|
| Laryngeal papillomatosis |
|
|
| 16 and 18 (31, 33, 45, 52, and 58 in immunocompromised immunocompromised A human or animal whose immunologic mechanism is deficient because of an immunodeficiency disorder or other disease or as the result of the administration of immunosuppressive drugs or radiation. Gastroenteritis individuals) |
Neoplasia:
|
|
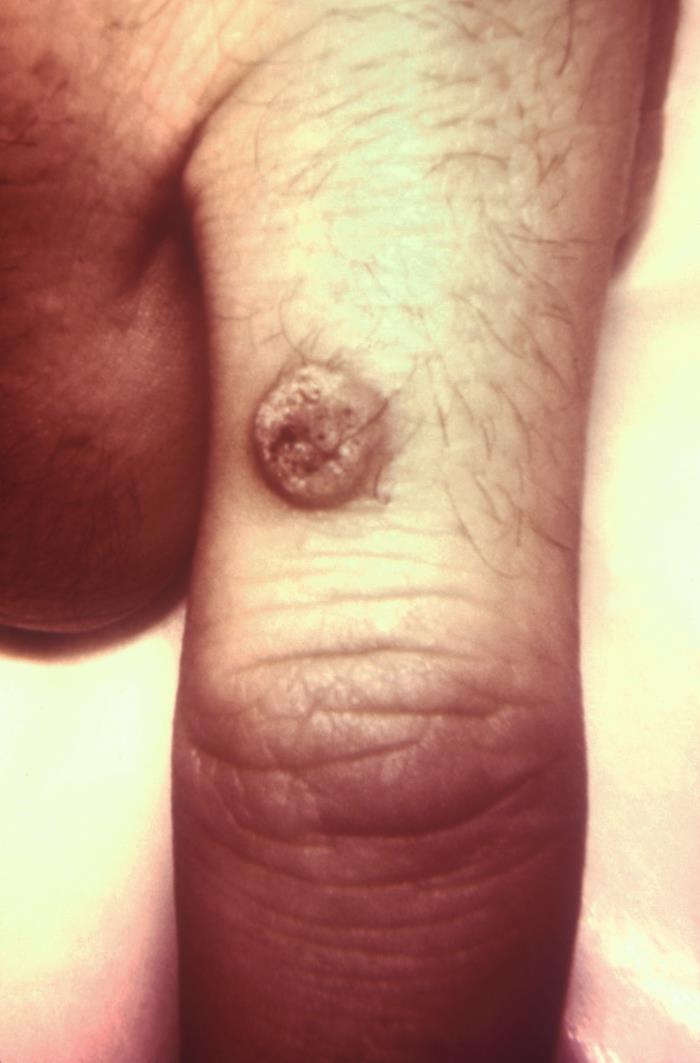
Verruca vulgaris (common wart) on a patient’s finger caused by human papillomavirus
Image: “This image depicts a close dorsal view of a patient’s right index finger, highlighting a proximal cutaneous lesion” by CDC/ Richard S. Hibbets. License: Public Domain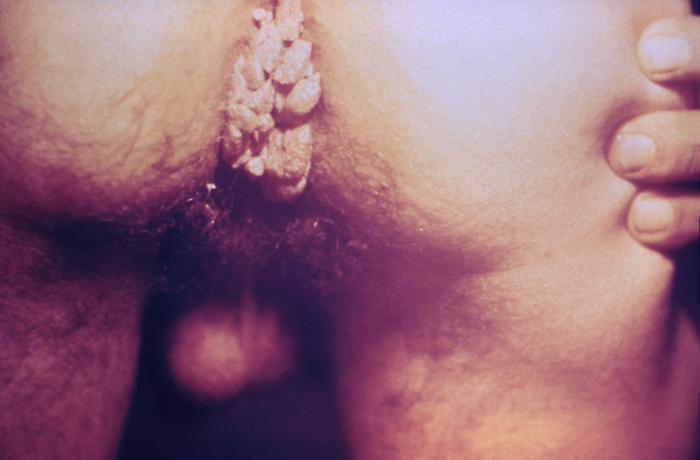
Multiple enlarged warts in the anal region of a patient
Image: “4151” by Dr. Wiesner. License: Public Domain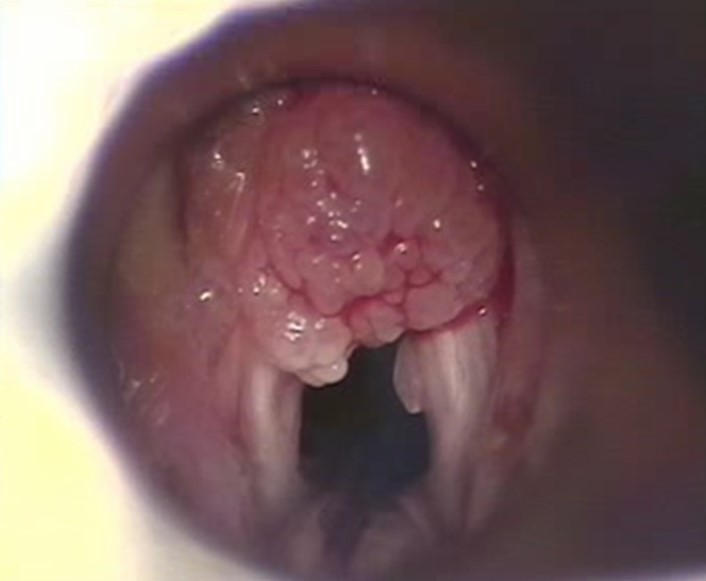
Laryngeal papillomatosis, a benign laryngeal tumor due to infection with human papillomavirus
Image: “Endoscopic view of laryngeal papilloma in a child with RRP” by Omland et al. License: CC BY 2.0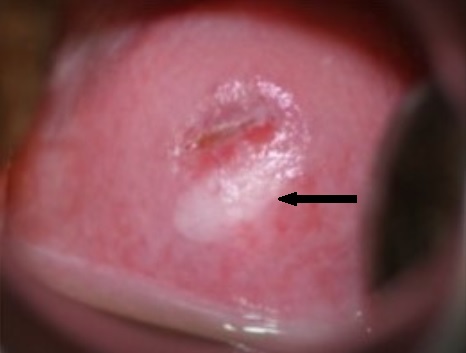
Squamous intraepithelial lesion of the cervix on colposcopy:
Ovoid squamous intraepithelial lesion (SIL) located in the 4‒8 o’clock area of the cervix (arrow), highlighted to a white color by the application of acetic acid. It is then called an “acetowhite” lesion. Note that the superior edge of the lesion is at the border of the deeper pink-colored endocervical glandular area (the transformation zone). The small exocervical os indicates that the woman has not given vaginal birth.
The following table compares 2 clinically similar double-stranded DNA viruses DNA Viruses Viruses whose nucleic acid is DNA. Virology:
| Organism | Human papillomavirus | Herpes simplex Herpes Simplex A group of acute infections caused by herpes simplex virus type 1 or type 2 that is characterized by the development of one or more small fluid-filled vesicles with a raised erythematous base on the skin or mucous membrane. It occurs as a primary infection or recurs due to a reactivation of a latent infection. Congenital TORCH Infections virus Virus Viruses are infectious, obligate intracellular parasites composed of a nucleic acid core surrounded by a protein capsid. Viruses can be either naked (non-enveloped) or enveloped. The classification of viruses is complex and based on many factors, including type and structure of the nucleoid and capsid, the presence of an envelope, the replication cycle, and the host range. Virology |
|---|---|---|
| Characteristics |
|
|
| Transmission |
|
|
| Clinical |
|
|
| Diagnosis |
|
|