Sick sinus syndrome (SSS), also known as sinus node dysfunction Sinus node dysfunction A condition caused by dysfunctions related to the sinoatrial node including impulse generation (cardiac sinus arrest) and impulse conduction (sinoatrial exit block). It is characterized by persistent bradycardia, chronic atrial fibrillation, and failure to resume sinus rhythm following cardioversion. This syndrome can be congenital or acquired, particularly after surgical correction for heart defects. Bradyarrhythmias, is characterized by degeneration of the sinoatrial (SA) node, the heart’s primary pacemaker Pacemaker A device designed to stimulate, by electric impulses, contraction of the heart muscles. It may be temporary (external) or permanent (internal or internal-external). Bradyarrhythmias. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship with SSS may be asymptomatic or may present with tachycardia Tachycardia Abnormally rapid heartbeat, usually with a heart rate above 100 beats per minute for adults. Tachycardia accompanied by disturbance in the cardiac depolarization (cardiac arrhythmia) is called tachyarrhythmia. Sepsis in Children or bradycardia Bradycardia Bradyarrhythmia is a rhythm in which the heart rate is less than 60/min. Bradyarrhythmia can be physiologic, without symptoms or hemodynamic change. Pathologic bradyarrhythmia results in reduced cardiac output and hemodynamic instability causing syncope, dizziness, or dyspnea. Bradyarrhythmias. In cases of bradycardia Bradycardia Bradyarrhythmia is a rhythm in which the heart rate is less than 60/min. Bradyarrhythmia can be physiologic, without symptoms or hemodynamic change. Pathologic bradyarrhythmia results in reduced cardiac output and hemodynamic instability causing syncope, dizziness, or dyspnea. Bradyarrhythmias, patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship can experience fatigue Fatigue The state of weariness following a period of exertion, mental or physical, characterized by a decreased capacity for work and reduced efficiency to respond to stimuli. Fibromyalgia, light-headedness, and syncope Syncope Syncope is a short-term loss of consciousness and loss of postural stability followed by spontaneous return of consciousness to the previous neurologic baseline without the need for resuscitation. The condition is caused by transient interruption of cerebral blood flow that may be benign or related to a underlying life-threatening condition. Syncope. Diagnosis is made by physical exam and ECG ECG An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG). Management can include a pacemaker Pacemaker A device designed to stimulate, by electric impulses, contraction of the heart muscles. It may be temporary (external) or permanent (internal or internal-external). Bradyarrhythmias.
Last updated: Dec 15, 2025
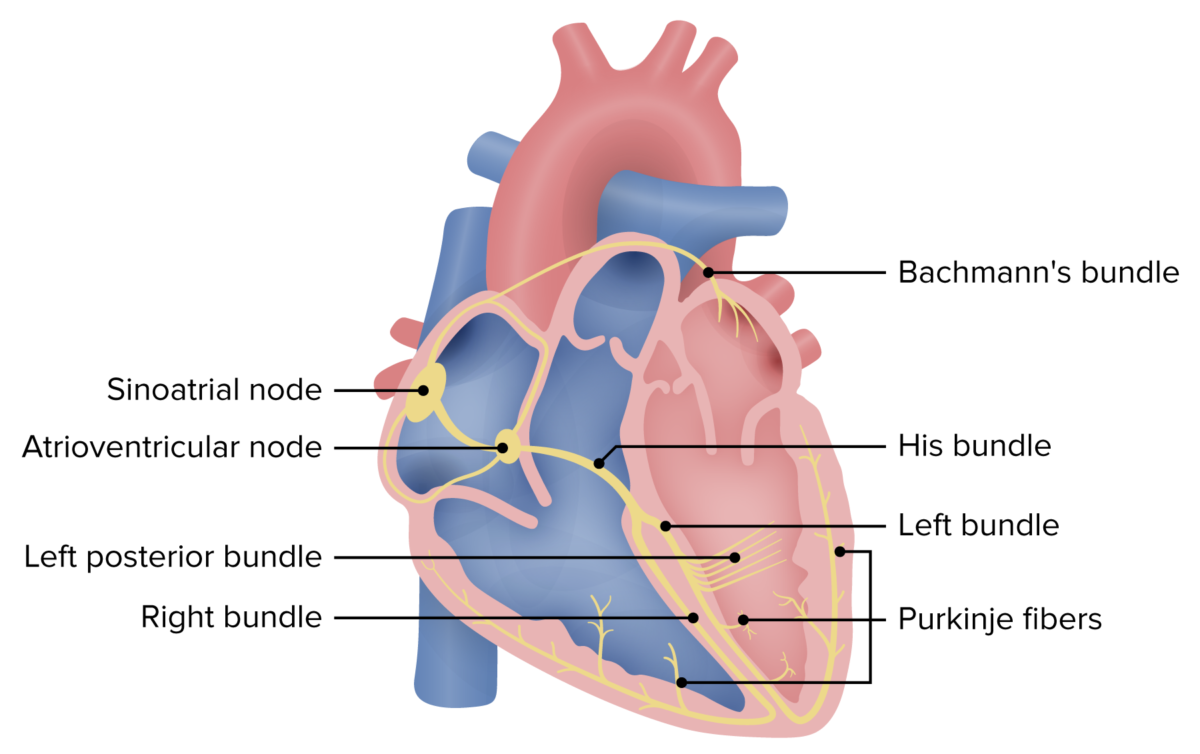
Conduction system of the heart
Image by Lecturio.Degeneration of the SA node:
Symptoms of bradycardia Bradycardia Bradyarrhythmia is a rhythm in which the heart rate is less than 60/min. Bradyarrhythmia can be physiologic, without symptoms or hemodynamic change. Pathologic bradyarrhythmia results in reduced cardiac output and hemodynamic instability causing syncope, dizziness, or dyspnea. Bradyarrhythmias or tachycardia Tachycardia Abnormally rapid heartbeat, usually with a heart rate above 100 beats per minute for adults. Tachycardia accompanied by disturbance in the cardiac depolarization (cardiac arrhythmia) is called tachyarrhythmia. Sepsis in Children– bradycardia Bradycardia Bradyarrhythmia is a rhythm in which the heart rate is less than 60/min. Bradyarrhythmia can be physiologic, without symptoms or hemodynamic change. Pathologic bradyarrhythmia results in reduced cardiac output and hemodynamic instability causing syncope, dizziness, or dyspnea. Bradyarrhythmias syndrome include:
The following heart rhythm abnormalities may be seen as a part of SSS:
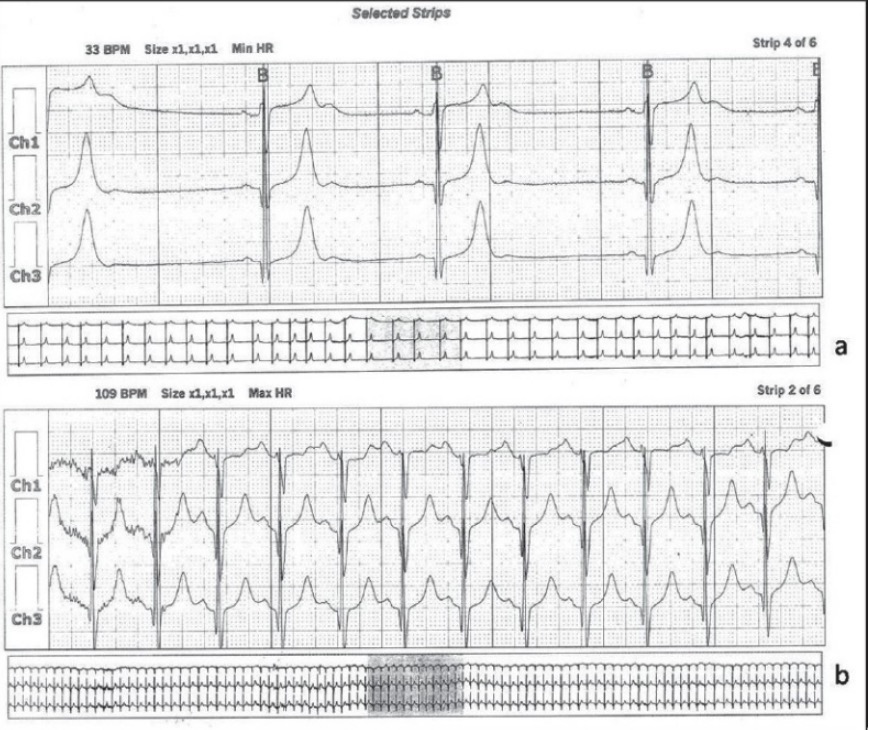
24-Hour Holter monitor recording demonstrating both bradycardia (panel a) and tachycardia (panel b); bradycardia–tachycardia syndrome
Image: “24-Hour Holter” by Department of Pediatrics, Seth G.S. Medical College and KEM Hospital, Mumbai, India. License: CC BY 2.0The following conditions may predispose to SSS.
The following conditions are included in the differential diagnosis for SSS.