Surgeons have used specialized tools to perform invasive procedures since Ancient Egypt. Throughout history, new techniques have been developed in close association with novel surgical instruments. Generally speaking, for any successful operation, a surgeon requires tools to cut open and access tissues (cutting, dissection, and retraction instruments), for bleeding control ( hemostasis Hemostasis Hemostasis refers to the innate, stepwise body processes that occur following vessel injury, resulting in clot formation and cessation of bleeding. Hemostasis occurs in 2 phases, namely, primary and secondary. Primary hemostasis involves forming a plug that stops the bleeding temporarily. Secondary hemostasis involves the activation of the coagulation cascade. Hemostasis instruments), and for anatomical restoration and closure of the surgical wound (sutures and needles).
Last updated: Jan 17, 2023
Suturing, also known as “stitching,” is a surgical maneuver carried out with the intent of joining together 2 selected tissues. For this purpose, the use of a needle and thread has proven to be the most cost-effective method up to modern times. Mechanical sutures (i.e., staples) are also available but are more expensive and have limited uses.
All sutures are classified according to their material as either absorbable or nonabsorbable. With absorbable sutures, the body will naturally degrade and absorb them over time. All suture materials are foreign bodies that set off an inflammatory response. Some materials are more likely to cause inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body’s defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation than others.
Absorbable:
Nonabsorbable:
According to shape:
According to tip (most common):
The size of a surgical needle is proportional to the caliber of the attached suture.
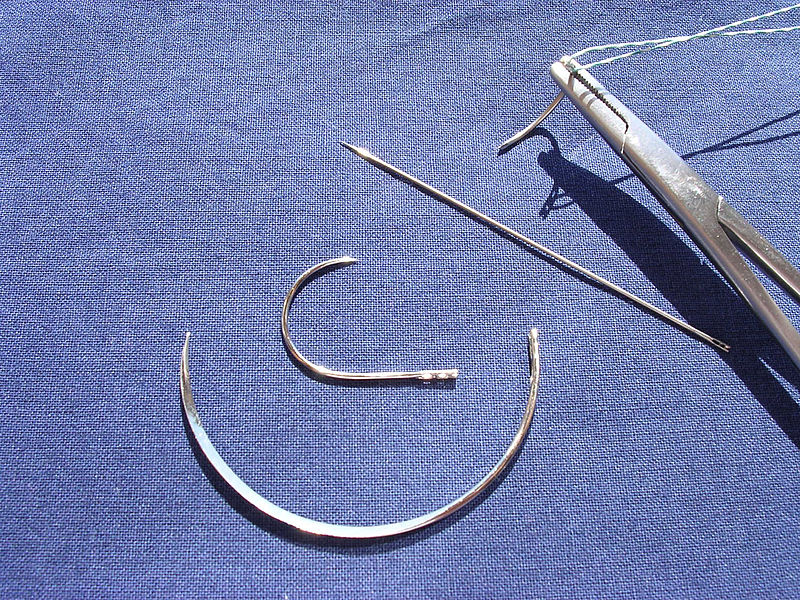
Curved and straight surgical needles
Image: “Surgical needles” by Rocco Cusari. License: Public DomainNeedle holders are specialized tools used to hold the needles for suturing. Needle holders are integrated clamps that lock the needle in place for as long as required. There are 2 main types of needle holders:
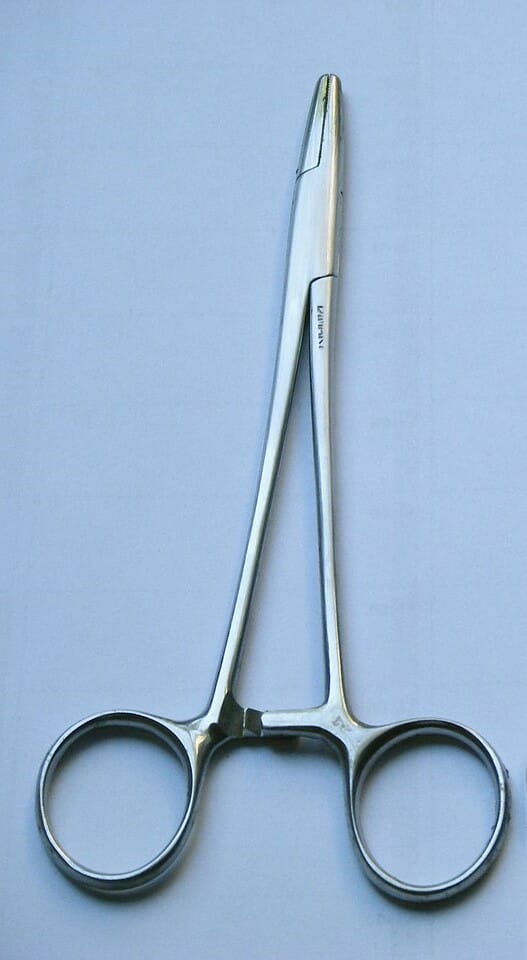
Mayo-Hegar needle holder
Image: “Pinza emostatica e portaghi” by Ricce. License: Public Domain, cropped by Lecturio.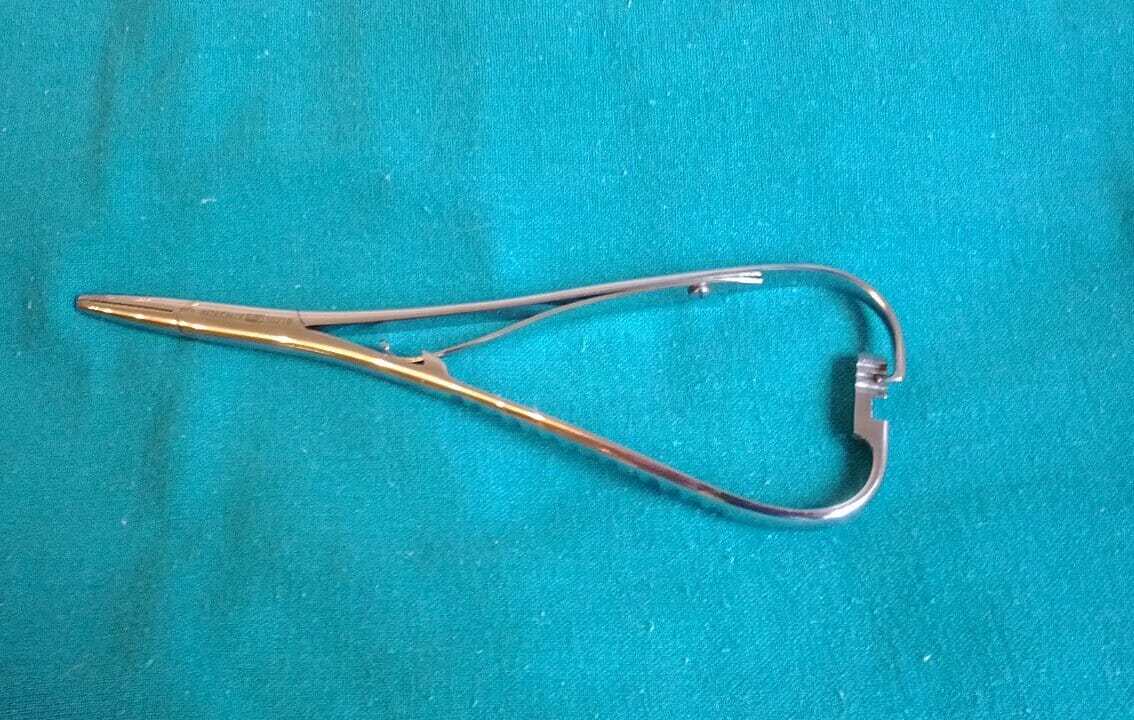
Mathieu needle holder
Image: “Mathieu needle holder” by MacPiek. License: CC BY 3.0Scalpel:

Scalpel handle
Image: “Scalpel” by Saltanat ebli. License: CC0 1.0Electric scalpel:
Laser scalpel:
Surgical scissors:
Types:

Metzenbaum scissors
Image: “Metzenbaum scissors” by Saltanat ebli. License: CC0 1.0
Mayo scissors
Image: “Mayo surgical scissors” by آرمین. License: Public Domain, cropped by Lecturio.Adequate bleeding control during a surgical procedure is key for reducing the likelihood of complications and reintervention. Hemostasis Hemostasis Hemostasis refers to the innate, stepwise body processes that occur following vessel injury, resulting in clot formation and cessation of bleeding. Hemostasis occurs in 2 phases, namely, primary and secondary. Primary hemostasis involves forming a plug that stops the bleeding temporarily. Secondary hemostasis involves the activation of the coagulation cascade. Hemostasis can be achieved via mechanical methods, such as rudimentary pressure, or hemostats, electrocautery, or hemostatic agents.
Mechanical hemostasis Hemostasis Hemostasis refers to the innate, stepwise body processes that occur following vessel injury, resulting in clot formation and cessation of bleeding. Hemostasis occurs in 2 phases, namely, primary and secondary. Primary hemostasis involves forming a plug that stops the bleeding temporarily. Secondary hemostasis involves the activation of the coagulation cascade. Hemostasis:
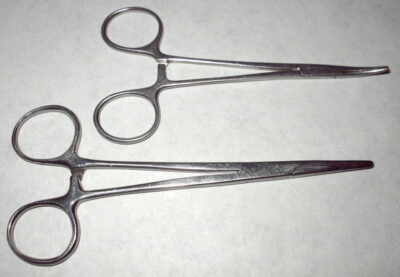
Hemostats with straight and curved tips
Image: “Hemostats” by Splarka. License: Public DomainElectrocautery:
Hemostatic agents:
Dissection instruments aid the surgeon in gaining depth in the tissues. Retraction instruments keep the surgical wound, or work area, open for further dissection.
Forceps:
Graspers and clamps:
Dissectors:
Numerous instruments are available to aid with tissue dissection. Some commonly used ones include:
Retractors:
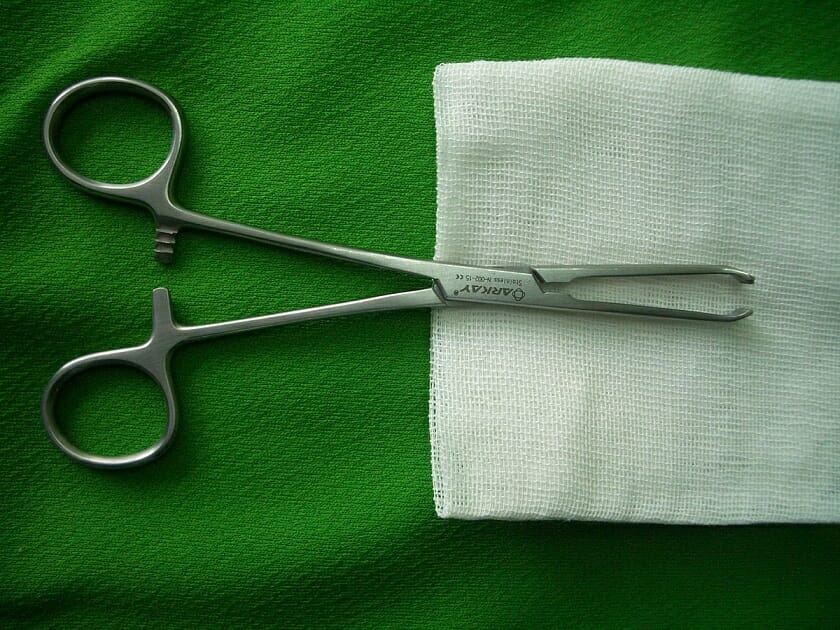
Allis clamp
Image: “Allis clamp” by آرمین. License: CC0 1.0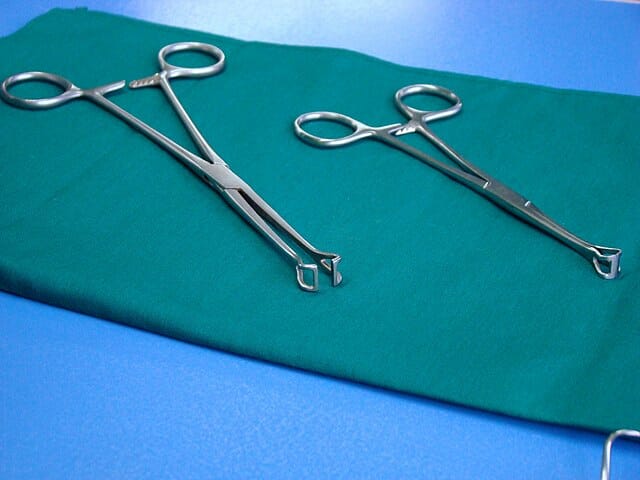
Babcock clamp
Image: “Babcock clamp” by آرمین. License: CC0 1.0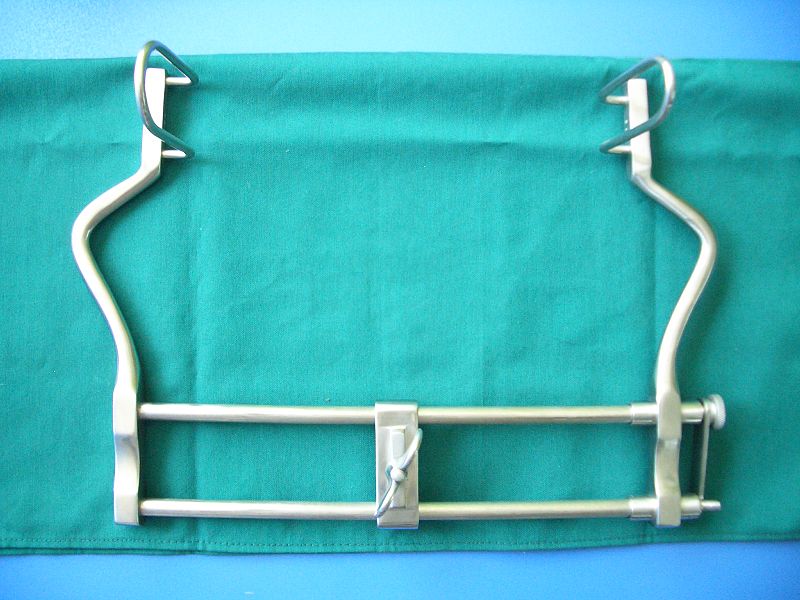
Self-retaining retractor
Image: “Surgical retractor” by Saltanat ebli. License: CC0 1.0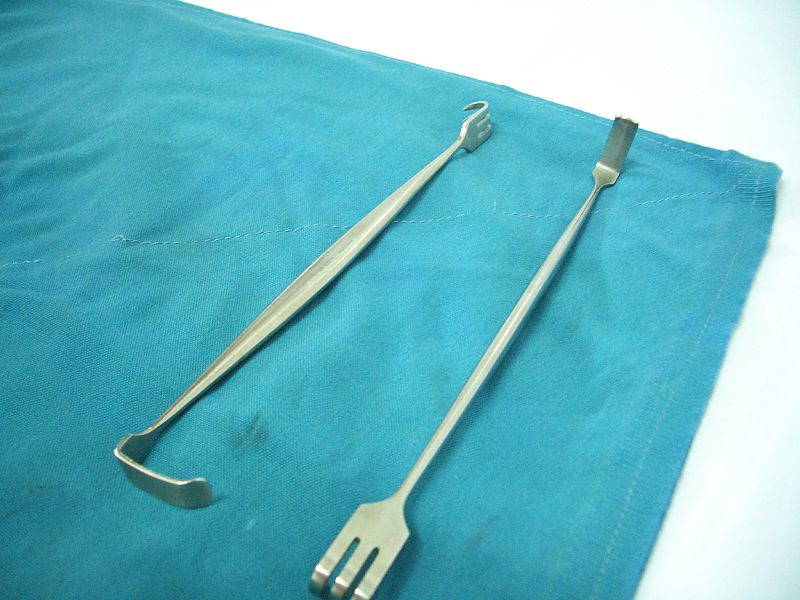
Miller-Senn retractors (manual)
Image: “Miler-Sen retractors” by آرمین. License: CC0 1.0
Deaver retractor (manual)
Image: “Deaver retractor” by Saltanat ebli. License: CC0 1.0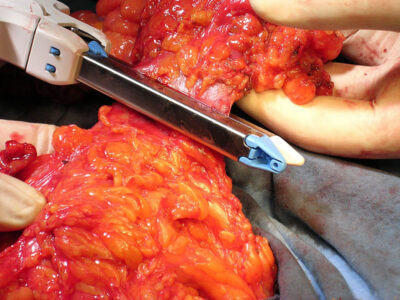
GIA (gastrointestinal anastomosis) stapler
Image: “Stapler GIA” by Rocco Cusari. License: Public Domain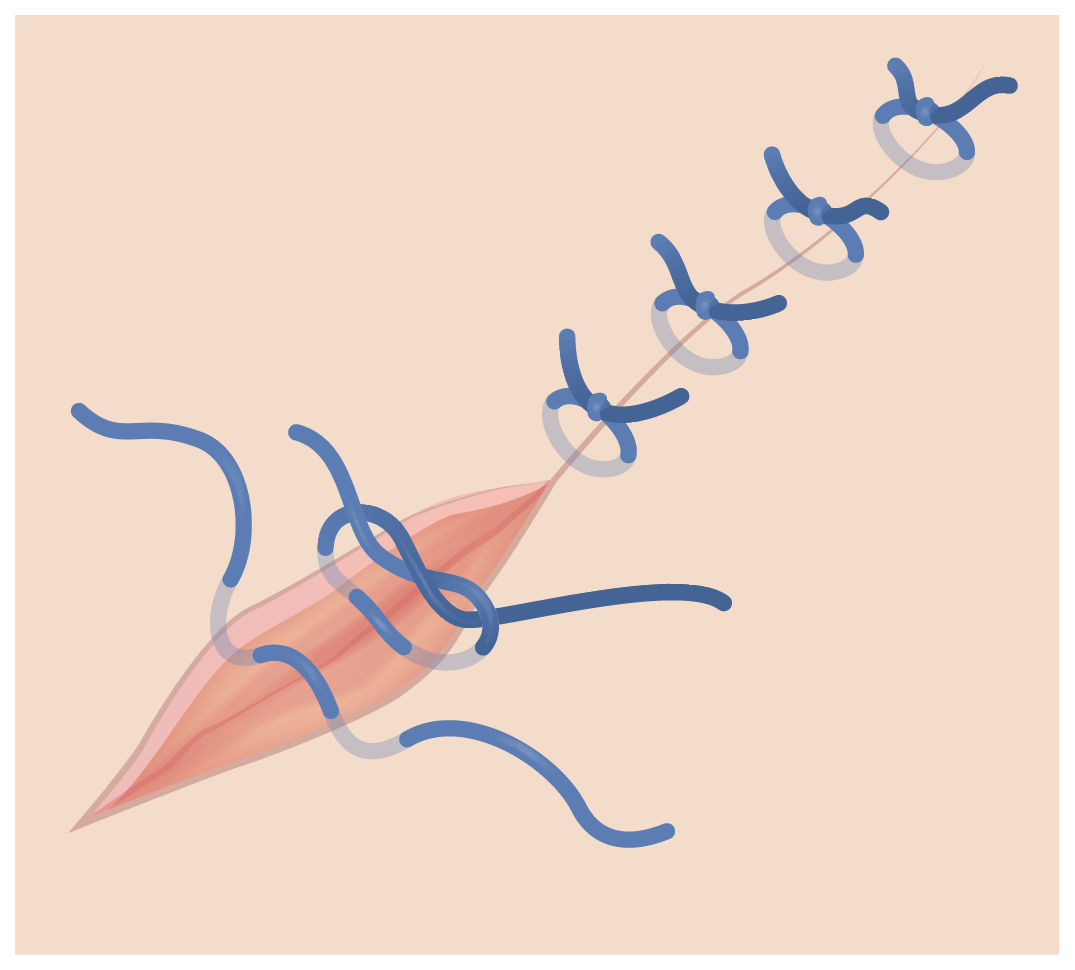
Simple interrupted suture
Image by Lecturio.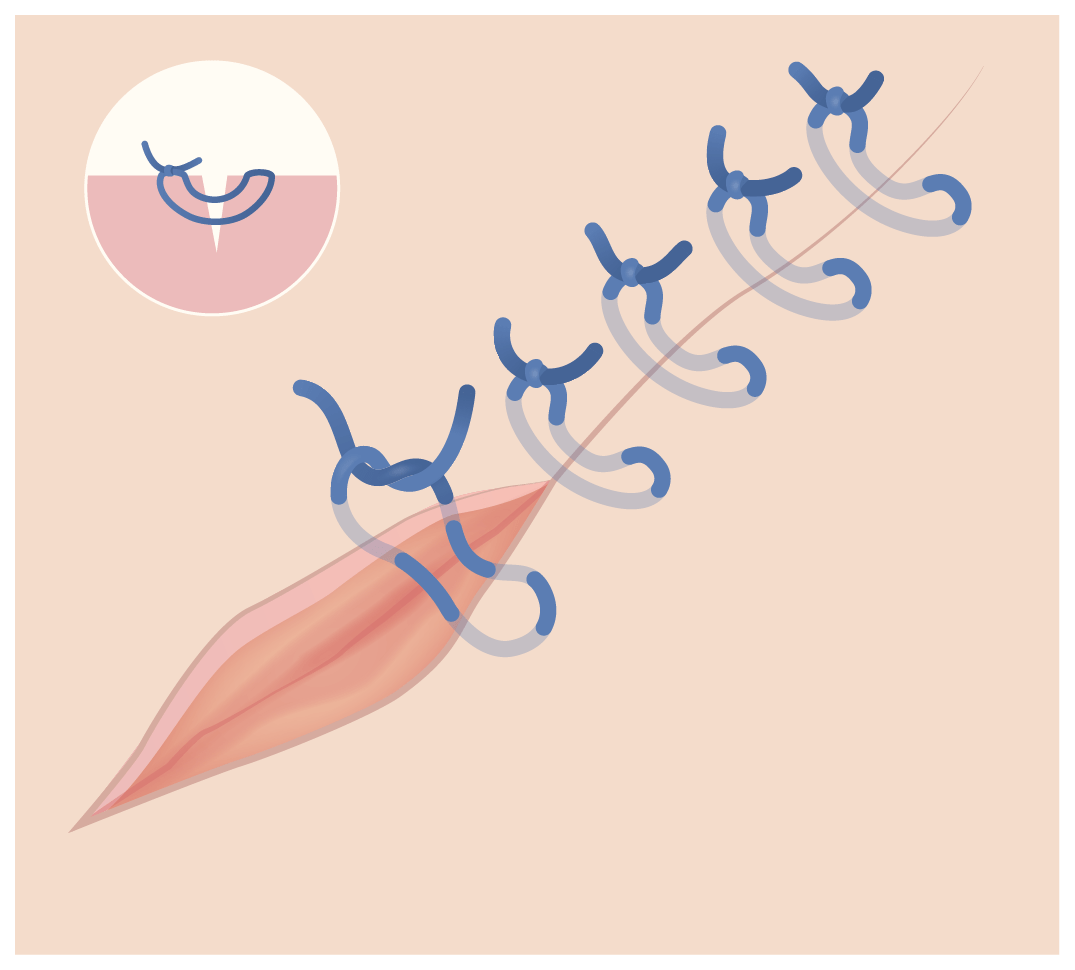
Vertical mattress suture
Image by Lecturio.
Horizontal mattress suture
Image by Lecturio.There are 2 basic types of surgical knots:
Knot-tying techniques:
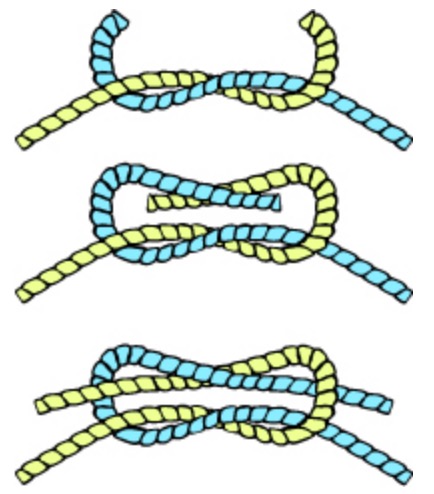
Tying a square knot
Image: “Knot square” by Jazzmanian. License: Public Domain
Surgeon’s knot
Image: “Surgical knot” by Werneuchen. License: Public Domain