Guillain-Barré syndrome ( GBS GBS An acute inflammatory autoimmune neuritis caused by t cell- mediated cellular immune response directed towards peripheral myelin. Demyelination occurs in peripheral nerves and nerve roots. The process is often preceded by a viral or bacterial infection, surgery, immunization, lymphoma, or exposure to toxins. Common clinical manifestations include progressive weakness, loss of sensation, and loss of deep tendon reflexes. Weakness of respiratory muscles and autonomic dysfunction may occur. Polyneuropathy), once thought to be a single disease process, is a family of immune-mediated polyneuropathies Polyneuropathies Diseases of multiple peripheral nerves simultaneously. Polyneuropathies usually are characterized by symmetrical, bilateral distal motor and sensory impairment with a graded increase in severity distally. The pathological processes affecting peripheral nerves include degeneration of the axon, myelin or both. The various forms of polyneuropathy are categorized by the type of nerve affected (e.g., sensory, motor, or autonomic), by the distribution of nerve injury (e.g., distal vs. Proximal), by nerve component primarily affected (e.g., demyelinating vs. axonal), by etiology, or by pattern of inheritance. Mononeuropathy and Plexopathy that occur after infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease (e.g., with Campylobacter jejuni Campylobacter jejuni A species of bacteria that resemble small tightly coiled spirals. Its organisms are known to cause abortion in sheep and fever and enteritis in man and may be associated with enteric diseases of calves, lambs, and other animals. Campylobacter). Typical GBS GBS An acute inflammatory autoimmune neuritis caused by t cell- mediated cellular immune response directed towards peripheral myelin. Demyelination occurs in peripheral nerves and nerve roots. The process is often preceded by a viral or bacterial infection, surgery, immunization, lymphoma, or exposure to toxins. Common clinical manifestations include progressive weakness, loss of sensation, and loss of deep tendon reflexes. Weakness of respiratory muscles and autonomic dysfunction may occur. Polyneuropathy is characterized by acute monophasic neuromuscular paralysis, which is symmetric and ascending in progression. If the paralysis reaches the respiratory muscles, GBS GBS An acute inflammatory autoimmune neuritis caused by t cell- mediated cellular immune response directed towards peripheral myelin. Demyelination occurs in peripheral nerves and nerve roots. The process is often preceded by a viral or bacterial infection, surgery, immunization, lymphoma, or exposure to toxins. Common clinical manifestations include progressive weakness, loss of sensation, and loss of deep tendon reflexes. Weakness of respiratory muscles and autonomic dysfunction may occur. Polyneuropathy can progress into respiratory failure Respiratory failure Respiratory failure is a syndrome that develops when the respiratory system is unable to maintain oxygenation and/or ventilation. Respiratory failure may be acute or chronic and is classified as hypoxemic, hypercapnic, or a combination of the two. Respiratory Failure, which requires prolonged hospitalization Prolonged Hospitalization Surgical Infections. Management is mostly supportive and may require either plasma exchange Plasma exchange Removal of plasma and replacement with various fluids, e.g., fresh frozen plasma, plasma protein fractions (ppf), albumin preparations, dextran solutions, saline. Used in treatment of autoimmune diseases, immune complex diseases, diseases of excess plasma factors, and other conditions. Thrombotic Thrombocytopenic Purpura or IV immunoglobulin Iv Immunoglobulin Dermatomyositis.
Last updated: Nov 12, 2024
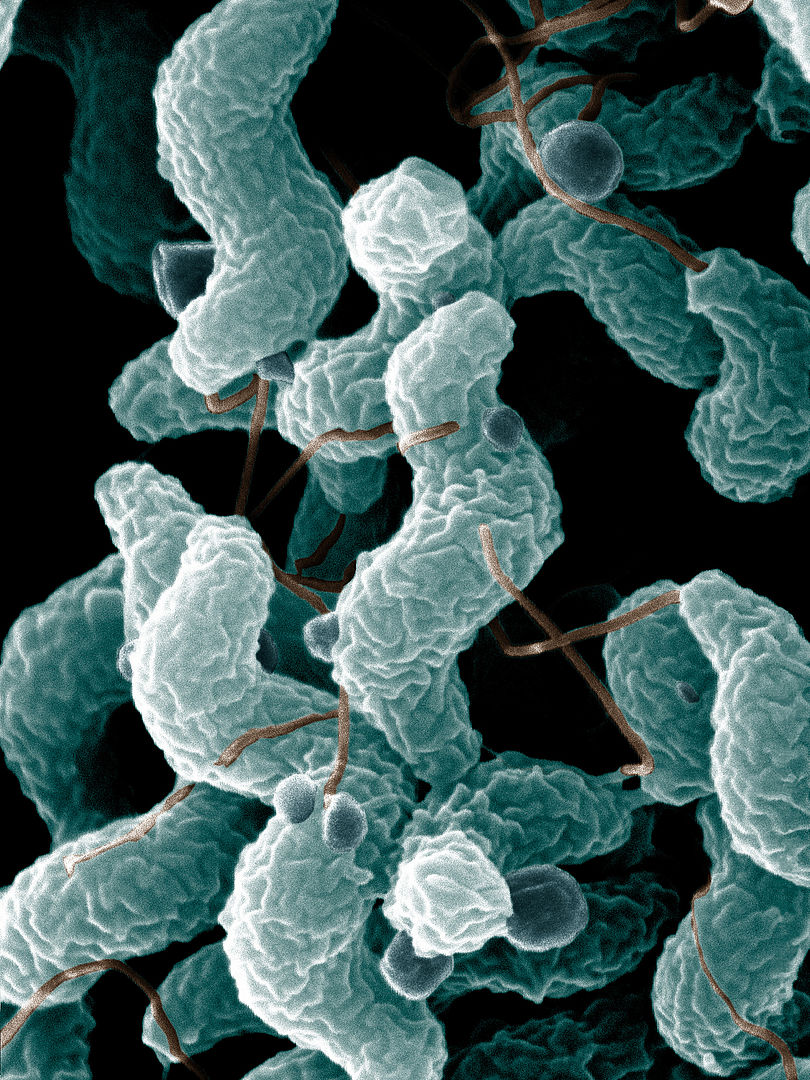
Campylobacter jejuni
This scanning electron micrograph depicts the S-shaped organism with a single, polar flagella.
Clinical symptoms vary based on the subtype of GBS GBS An acute inflammatory autoimmune neuritis caused by t cell- mediated cellular immune response directed towards peripheral myelin. Demyelination occurs in peripheral nerves and nerve roots. The process is often preceded by a viral or bacterial infection, surgery, immunization, lymphoma, or exposure to toxins. Common clinical manifestations include progressive weakness, loss of sensation, and loss of deep tendon reflexes. Weakness of respiratory muscles and autonomic dysfunction may occur. Polyneuropathy. Individuals may have a history of respiratory or GI symptoms 1–4 weeks prior to the appearance of GBS GBS An acute inflammatory autoimmune neuritis caused by t cell- mediated cellular immune response directed towards peripheral myelin. Demyelination occurs in peripheral nerves and nerve roots. The process is often preceded by a viral or bacterial infection, surgery, immunization, lymphoma, or exposure to toxins. Common clinical manifestations include progressive weakness, loss of sensation, and loss of deep tendon reflexes. Weakness of respiratory muscles and autonomic dysfunction may occur. Polyneuropathy.
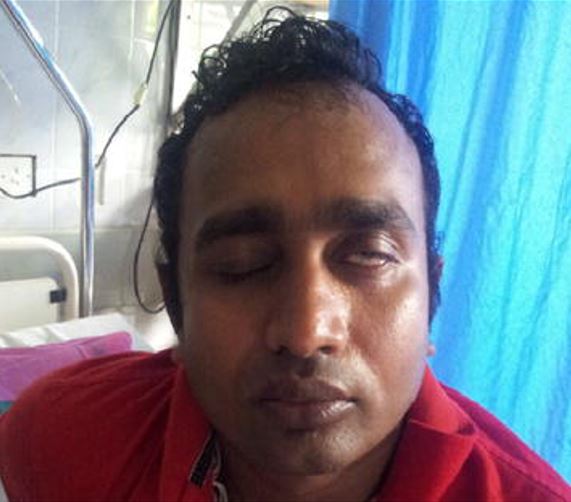
Clinical symptoms of Guillain-Barré syndrome:
Bell palsy (facial nerve palsy) in an individual with GBS following an acute dengue fever infection