Perianal and perirectal abscesses are collections of pus in the enclosed space near the perirectal tissues. These infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease originate from obstruction of anal crypt glands. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship present with severe pain Pain An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons. Pain: Types and Pathways in the anal or rectal area. Finding a tender, fluctuant Fluctuant Dermatologic Examination mass Mass Three-dimensional lesion that occupies a space within the breast Imaging of the Breast on physical exam can provide the diagnosis. Management requires prompt surgical incision and drainage Incision And Drainage Chalazion, which may be followed by a course of antibiotics in some cases. Untreated, these abscesses can lead to the formation of fistulas.
Last updated: Dec 15, 2025
Anal glands, found in the intersphincteric plane, drain into crypts found along the circumference of the dentate/ pectinate line Pectinate line Rectum and Anal Canal: Anatomy. Infection of an obstructed glandular crypt may occur due to:
Common bacteria Bacteria Bacteria are prokaryotic single-celled microorganisms that are metabolically active and divide by binary fission. Some of these organisms play a significant role in the pathogenesis of diseases. Bacteriology:
The classification of anorectal abscesses is based on their location.
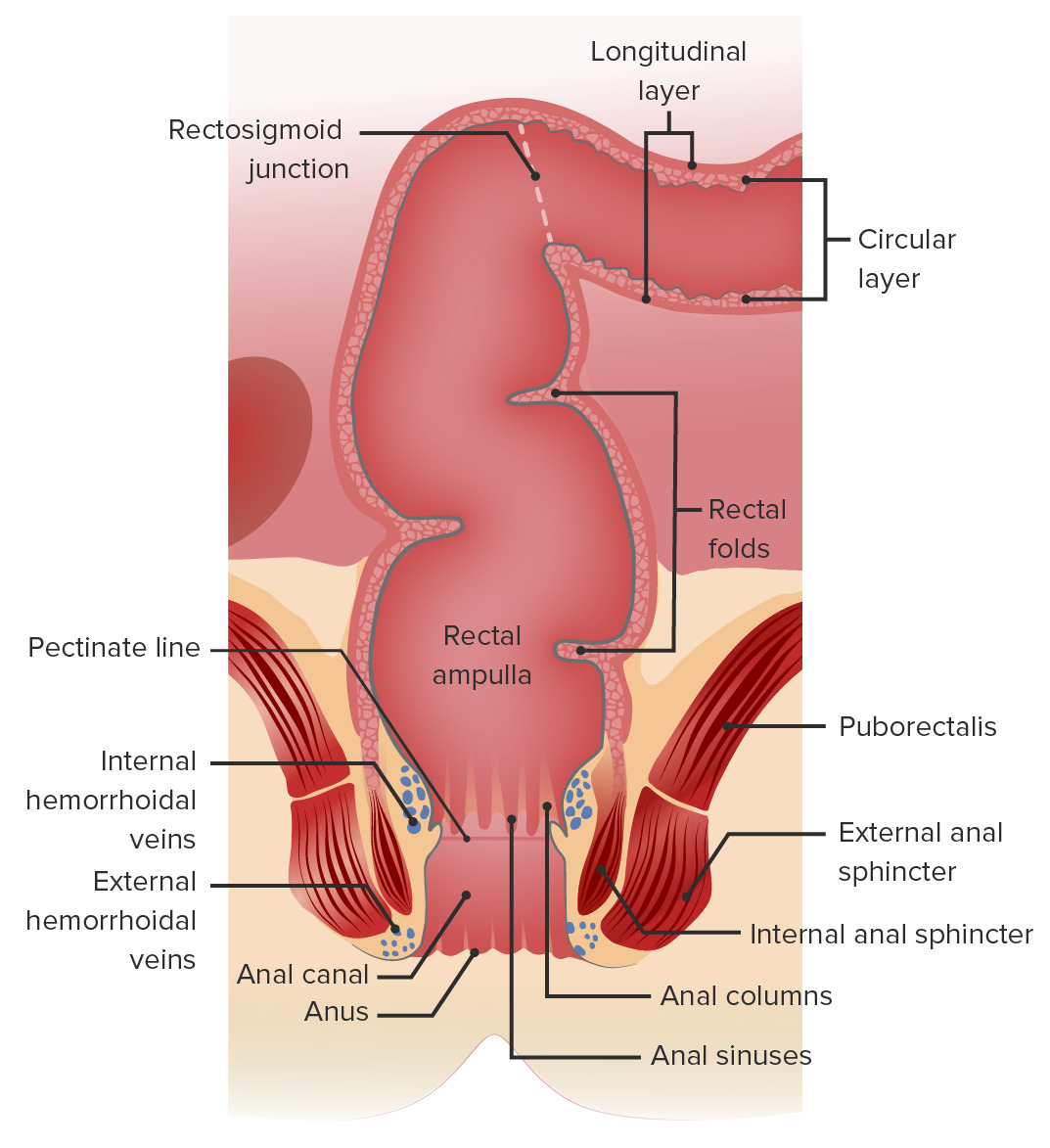
Relevant anatomy of the anus and rectum:
The perianal space surrounds the anus. The ischiorectal space extends laterally from the external sphincter to the ischium. The intersphincteric space is the area between the external and internal anal sphincters. The supralevator space is above the levator ani (the puborectalis is part of the levator ani complex).
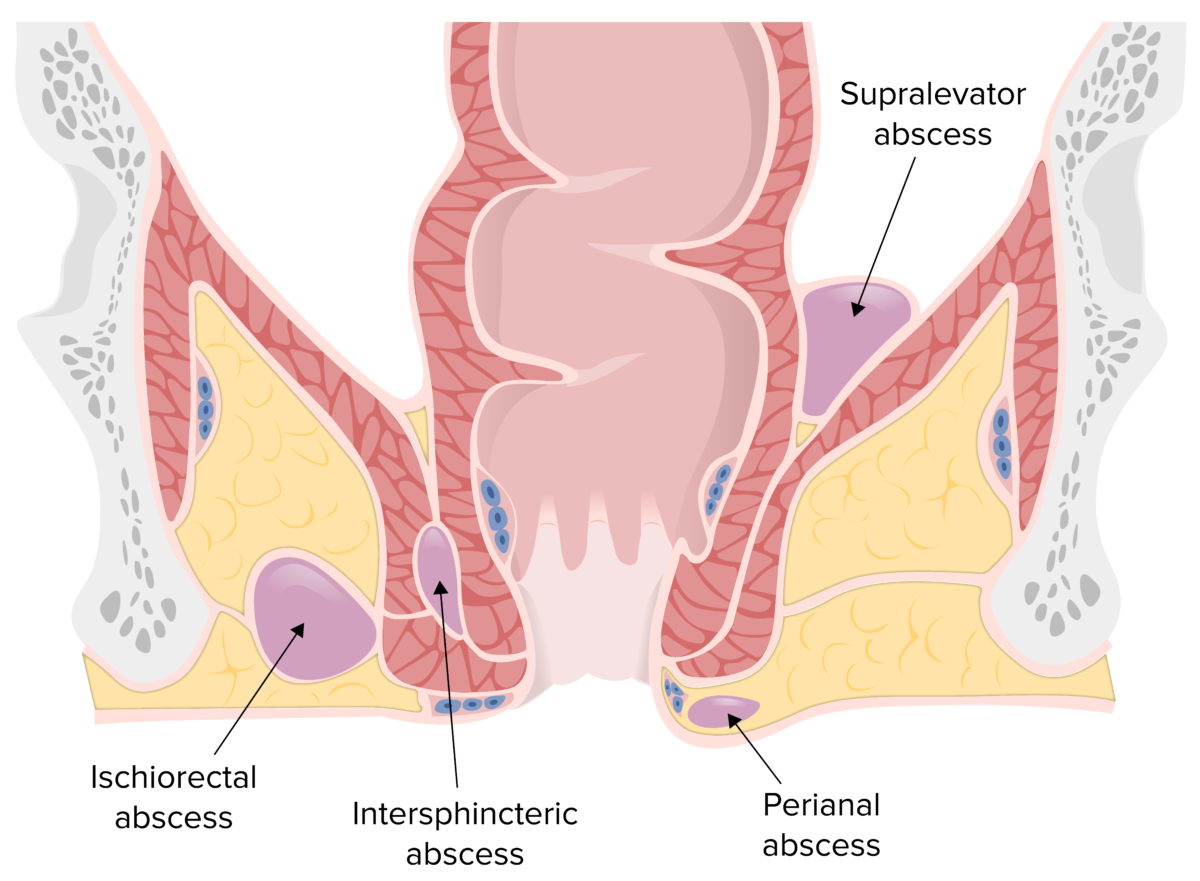
Locations of perianal, ischiorectal, intersphincteric, and supralevator abscesses
Image by Lecturio.The symptoms of a perirectal or perianal abscess Abscess Accumulation of purulent material in tissues, organs, or circumscribed spaces, usually associated with signs of infection. Chronic Granulomatous Disease can vary based on its location, but may include:
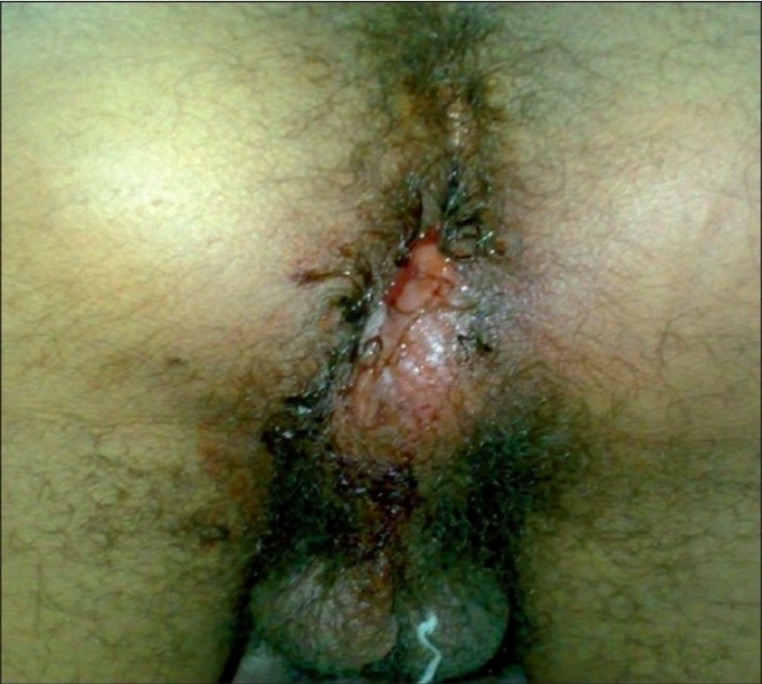
Perianal swelling, erythema, and drainage due to a perianal abscess
Image: “Localization of the perianal abscess” by Department of Urology, University Hospital Center, Fez, Morocco. License: CC BY 2.0The diagnosis of a perianal or ischiorectal abscess Abscess Accumulation of purulent material in tissues, organs, or circumscribed spaces, usually associated with signs of infection. Chronic Granulomatous Disease is usually made clinically. However, CT, MRI, or ultrasonography may be useful for identifying:
Surgical drainage:
Antibiotic therapy:
Postoperative care Postoperative care After any procedure performed in the operating room, all patients must undergo close observation at least in the recovery room. After larger procedures and for patients who require hospitalization, observation must continue on the surgical ward. The primary intent of this practice is the early detection of postoperative complications. Postoperative Care: