Snakebites are a rare cause of morbidity Morbidity The proportion of patients with a particular disease during a given year per given unit of population. Measures of Health Status and mortality Mortality All deaths reported in a given population. Measures of Health Status, as the majority of snakes are nonvenomous. Viperidae (which includes rattlesnakes) and Elapidae (which includes coral snakes) are 2 families of venomous snakes in the United States. Envenomation results in increased capillary permeability, hemolysis, tissue necrosis Necrosis The death of cells in an organ or tissue due to disease, injury or failure of the blood supply. Ischemic Cell Damage, and allergic reactions Allergic Reactions Type I hypersensitivity reaction against plasma proteins in donor blood Transfusion Reactions. Evidence of envenomation at the bite site includes edema Edema Edema is a condition in which excess serous fluid accumulates in the body cavity or interstitial space of connective tissues. Edema is a symptom observed in several medical conditions. It can be categorized into 2 types, namely, peripheral (in the extremities) and internal (in an organ or body cavity). Edema, erythema Erythema Redness of the skin produced by congestion of the capillaries. This condition may result from a variety of disease processes. Chalazion, warmth, bullae Bullae Erythema Multiforme, and necrosis Necrosis The death of cells in an organ or tissue due to disease, injury or failure of the blood supply. Ischemic Cell Damage. Systemic symptoms such as nausea Nausea An unpleasant sensation in the stomach usually accompanied by the urge to vomit. Common causes are early pregnancy, sea and motion sickness, emotional stress, intense pain, food poisoning, and various enteroviruses. Antiemetics, diaphoresis, paresthesias Paresthesias Subjective cutaneous sensations (e.g., cold, warmth, tingling, pressure, etc.) that are experienced spontaneously in the absence of stimulation. Posterior Cord Syndrome, and altered sensorium may be present. In addition, coral snake venom can cause flaccid muscles. The diagnosis is clinical. Management includes supportive care, pain Pain An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons. Pain: Types and Pathways control, hydration, and antivenom. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship are monitored closely for shock Shock Shock is a life-threatening condition associated with impaired circulation that results in tissue hypoxia. The different types of shock are based on the underlying cause: distributive (↑ cardiac output (CO), ↓ systemic vascular resistance (SVR)), cardiogenic (↓ CO, ↑ SVR), hypovolemic (↓ CO, ↑ SVR), obstructive (↓ CO), and mixed. Types of Shock, coagulopathy, respiratory failure Respiratory failure Respiratory failure is a syndrome that develops when the respiratory system is unable to maintain oxygenation and/or ventilation. Respiratory failure may be acute or chronic and is classified as hypoxemic, hypercapnic, or a combination of the two. Respiratory Failure, and renal failure Renal failure Conditions in which the kidneys perform below the normal level in the ability to remove wastes, concentrate urine, and maintain electrolyte balance; blood pressure; and calcium metabolism. Renal insufficiency can be classified by the degree of kidney damage (as measured by the level of proteinuria) and reduction in glomerular filtration rate. Crush Syndrome.
Last updated: Apr 7, 2025
Some important venomous snakes in the United States include:

Western diamondback rattlesnake:
a highly excitable, aggressive rattlesnake responsible for a significant portion of the venomous snake bites and most of the snakebite fatalities reported in the United States each year

A Texas coral snake
Image: “8141” by U.S. Department of Health & Human Services. License: Public Domain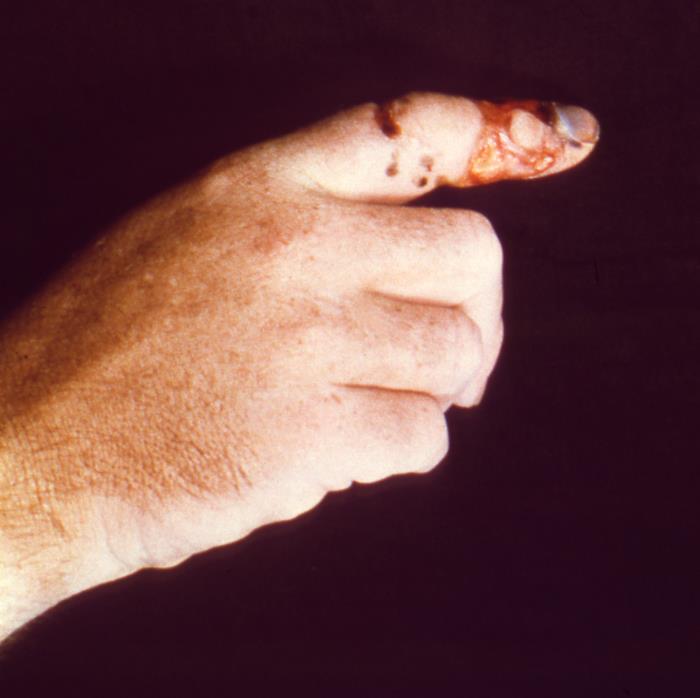
Index finger of a patient’s right hand displaying an area of focal necrosis following a bite from a snake in the Crotalinae subfamily
Image: “21010” by U.S. Department of Health & Human Services. License: Public Domain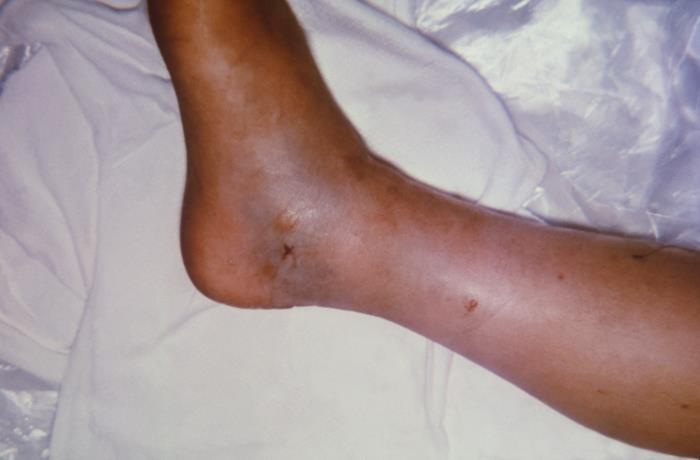
Medial view of a patient’s right foot where the patient sustained a copperhead rattlesnake bite:
Note the swelling exhibited in the ankle region and the broken skin surface at the snake bite site.
The diagnosis of a snake bite is clinical and aided by the identification Identification Defense Mechanisms of the snake. Photos of the snake (if able to be taken safely) help expedite the diagnosis and management.