Moraxella is a genus of gram-negative diplococci Gram-negative diplococci Neisseria, with M. catarrhalis being the most clinically relevant species. M. catarrhalis is part of the normal flora of the upper respiratory tract, but it can cause infection in susceptible individuals. The infection is transmitted through respiratory droplets Droplets Varicella-Zoster Virus/Chickenpox and can lead to chronic obstructive pulmonary disease Pulmonary disease Diseases involving the respiratory system. Blastomyces/Blastomycosis ( COPD COPD Chronic obstructive pulmonary disease (COPD) is a lung disease characterized by progressive, largely irreversible airflow obstruction. The condition usually presents in middle-aged or elderly persons with a history of cigarette smoking. Signs and symptoms include prolonged expiration, wheezing, diminished breath sounds, progressive dyspnea, and chronic cough. Chronic Obstructive Pulmonary Disease (COPD)) exacerbations in adults and otitis media in children. Moraxella species are catalase- and oxidase-positive, allowing them to resist damage from reactive oxygen species Reactive oxygen species Molecules or ions formed by the incomplete one-electron reduction of oxygen. These reactive oxygen intermediates include singlet oxygen; superoxides; peroxides; hydroxyl radical; and hypochlorous acid. They contribute to the microbicidal activity of phagocytes, regulation of signal transduction and gene expression, and the oxidative damage to nucleic acids; proteins; and lipids. Metabolic Dysfunction-associated Steatotic Liver Disease (MASLD) in the highly oxygenated environment of the respiratory tract.
Last updated: Dec 15, 2025
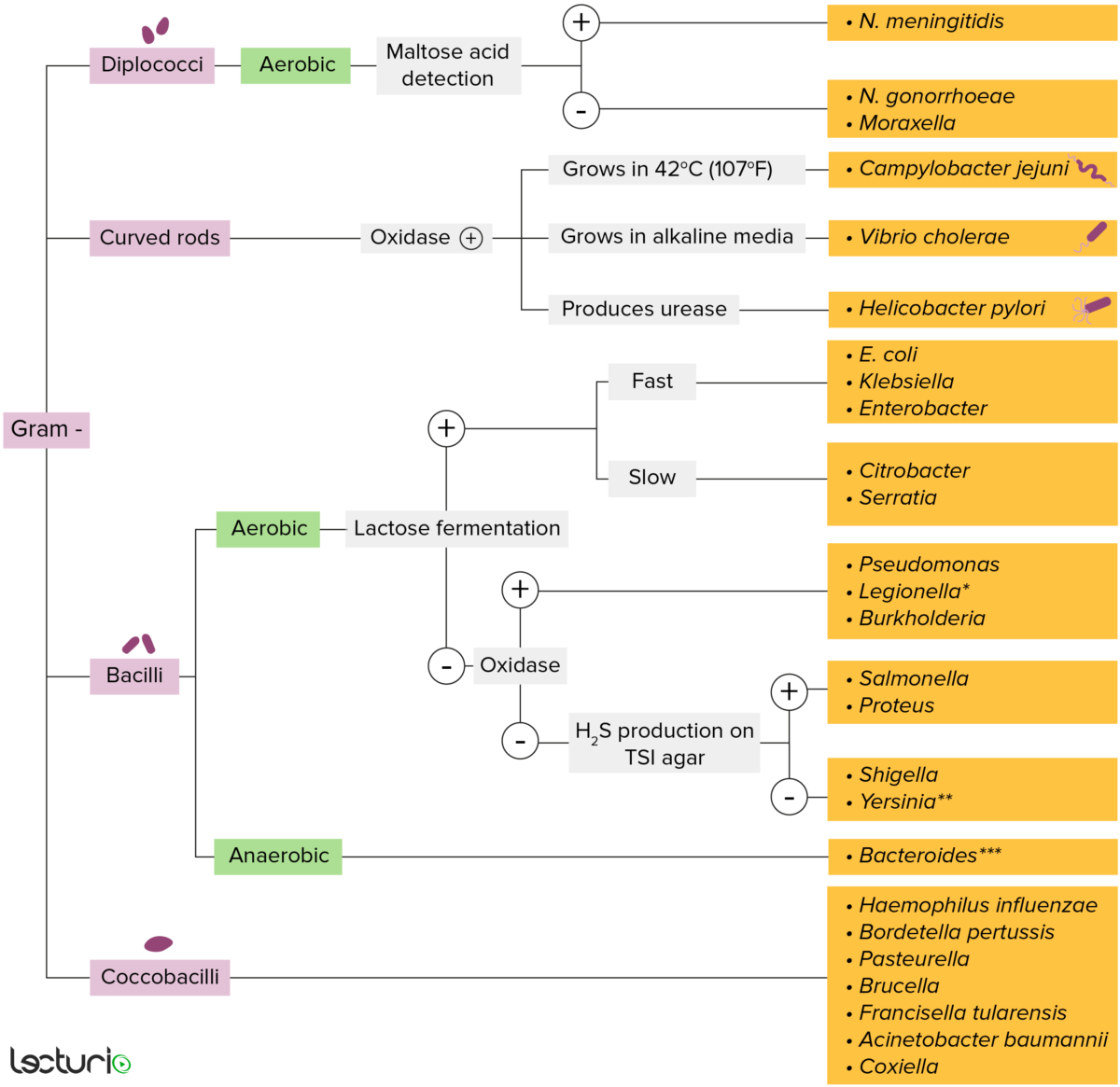
Gram-negative bacteria:
Most bacteria can be classified according to a lab procedure called Gram staining.
Bacteria with cell walls that have a thin layer of peptidoglycan do not retain the crystal violet stain utilized in Gram staining. These bacteria do, however, retain the safranin counterstain and thus appear as pinkish-red on the stain, making them gram negative. These bacteria can be further classified according to morphology (diplococci, curved rods, bacilli, and coccobacilli) and their ability to grow in the presence of oxygen (aerobic versus anaerobic). The bacteria can be more narrowly identified by growing them on specific media (triple sugar iron (TSI) agar) where their enzymes can be identified (urease, oxidase) and their ability to ferment lactose can be tested.
* Stains poorly on Gram stain
** Pleomorphic rod/coccobacillus
*** Require special transport media
Features:
M. catarrhalis and M. lacunata are the most clinically relevant species within this genus.
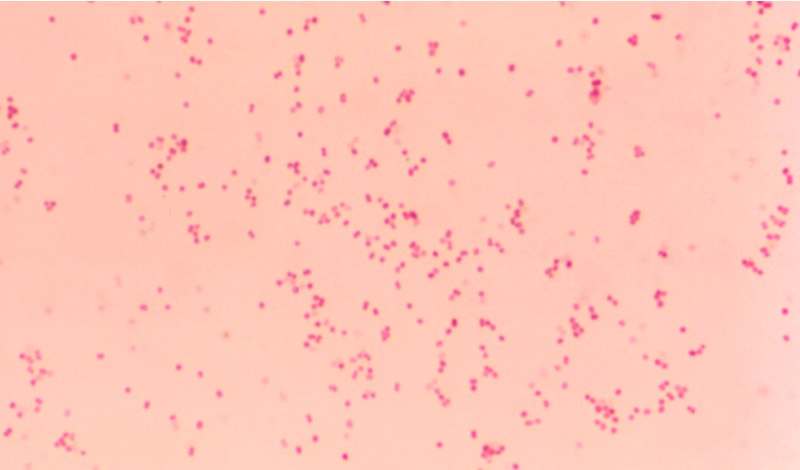
Moraxella catarrhalis (diplococcus formation)
Image: “Moraxella Catarrhalis” by CDC/Dr. W.A. Clark. License: Public DomainM. lacunata is a common cause of chronic angular blepharoconjunctivitis in humans.
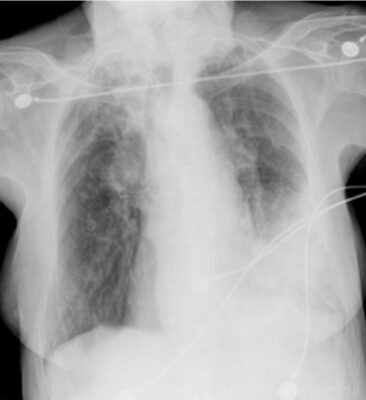
Pneumonia secondary to Moraxella catarrhalis:
Chest X-ray shows a left lower lobe infiltrate secondary to Moraxella catarrhalis, a gram-negative diplococcus that can be an etiologic agent for lung infections in immunocompromised patients and in those with chronic obstructive pulmonary disease (COPD).