Hereditary angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema (HAE), also known as C1 esterase inhibitor (C1-INH) deficiency, is an autosomal dominant Autosomal dominant Autosomal inheritance, both dominant and recessive, refers to the transmission of genes from the 22 autosomal chromosomes. Autosomal dominant diseases are expressed when only 1 copy of the dominant allele is inherited. Autosomal Recessive and Autosomal Dominant Inheritance disorder characterized by recurrent episodes of severe swelling Swelling Inflammation ( angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema). Hereditary angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema commonly affects the limbs, face, intestinal tract, and upper airway Airway ABCDE Assessment. Swelling Swelling Inflammation in the airway Airway ABCDE Assessment can restrict breathing and lead to a life-threatening airway Airway ABCDE Assessment obstruction. Hereditary angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema has 3 subtypes distinguished by their underlying etiologies and levels of C1 inhibitor C1 inhibitor An endogenous 105-kda plasma glycoprotein produced primarily by the liver and monocytes. It inhibits a broad spectrum of proteases, including the complement C1r and the complement C1s proteases of the classical complement pathway, and the mannose-binding protein-associated serine proteases. C1-inh-deficient individuals suffer from hereditary angioedema types I and II. Angioedema in the blood. Management includes treatment with danazol Danazol A synthetic steroid with antigonadotropic and anti-estrogenic activities that acts as an anterior pituitary suppressant by inhibiting the pituitary output of gonadotropins. It possesses some androgenic properties. Danazol has been used in the treatment of endometriosis and some benign breast disorders. Antiestrogens, kallikrein inhibitors, and C1-INHs. Hereditary angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema is self-limiting Self-Limiting Meningitis in Children, but may be fatal if the airway Airway ABCDE Assessment becomes compromised.
Last updated: Mar 28, 2025
Hereditary angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema (HAE) is a hereditary condition featuring recurrent episodes of swelling Swelling Inflammation ( angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema), usually of the mucosa of the respiratory and gastrointestinal (GI) systems, without urticaria Urticaria Urticaria is raised, well-circumscribed areas (wheals) of edema (swelling) and erythema (redness) involving the dermis and epidermis with associated pruritus (itch). Urticaria is not a single disease but rather is a reaction pattern representing cutaneous mast cell degranulation. Urticaria (Hives) or itching.
Genetic mutations Genetic Mutations Carcinogenesis are the cause of HAE:
The basic pathophysiology of swelling Swelling Inflammation in HAE has to do with the overproduction of bradykinin.
| HAE type I | HAE type II | HAE type III | |
|---|---|---|---|
| Prevalence Prevalence The total number of cases of a given disease in a specified population at a designated time. It is differentiated from incidence, which refers to the number of new cases in the population at a given time. Measures of Disease Frequency | 80%–85% of cases | 15%–20% | Very rare; usually in women |
| Cause | Reduced secretion Secretion Coagulation Studies of C1-INHs | Production of non-functional C1-INH |
|
| Pathophysiology | Excess production of inflammatory anaphylatoxins Anaphylatoxins Serum peptides derived from certain cleaved complement proteins during complement activation. They induce smooth muscle contraction; mast cell histamine release; platelet aggregation; and act as mediators of the local inflammatory process. The order of anaphylatoxin activity from the strongest to the weakest is C5a, C3a, C4a, and C5a des-arginine. Innate Immunity: Barriers, Complement, and Cytokines that affect the flow Flow Blood flows through the heart, arteries, capillaries, and veins in a closed, continuous circuit. Flow is the movement of volume per unit of time. Flow is affected by the pressure gradient and the resistance fluid encounters between 2 points. Vascular resistance is the opposition to flow, which is caused primarily by blood friction against vessel walls. Vascular Resistance, Flow, and Mean Arterial Pressure of body fluids between the vascular system and body tissues | Excess production of inflammatory anaphylatoxins Anaphylatoxins Serum peptides derived from certain cleaved complement proteins during complement activation. They induce smooth muscle contraction; mast cell histamine release; platelet aggregation; and act as mediators of the local inflammatory process. The order of anaphylatoxin activity from the strongest to the weakest is C5a, C3a, C4a, and C5a des-arginine. Innate Immunity: Barriers, Complement, and Cytokines that affect the flow Flow Blood flows through the heart, arteries, capillaries, and veins in a closed, continuous circuit. Flow is the movement of volume per unit of time. Flow is affected by the pressure gradient and the resistance fluid encounters between 2 points. Vascular resistance is the opposition to flow, which is caused primarily by blood friction against vessel walls. Vascular Resistance, Flow, and Mean Arterial Pressure of body fluids between the vascular system and body tissues |
|
Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship with HAE have recurrent attacks:
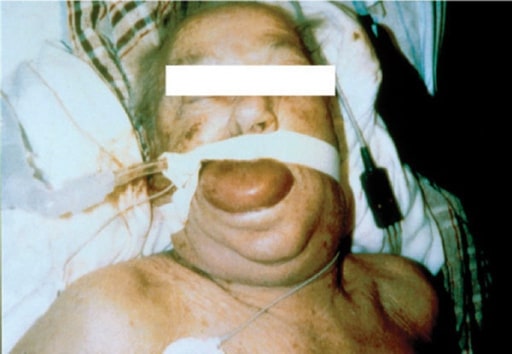
Severe face, tongue, and pharyngeal edema in a patient treated with an angiotensin- converting-enzyme (ACE) inhibitor
Image: “F3” by the National Allergy, Asthma, and Urticaria Centers of Charleston, Charleston, SC. License: CC BY 2.0.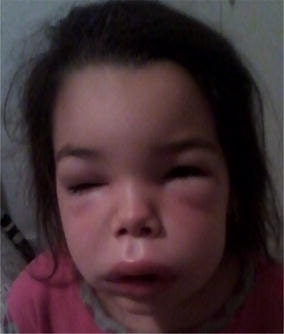
Angioedema of the face
Image: “Angioedema of the face” by S. Tolga Yavuz et al. License: CC BY 4.0.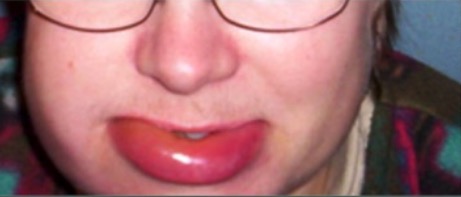
Hereditary angioedema
Image: “Typical features” by the Department of Bacteriology and Immunology, Haartman Institute, University of Helsinki, Helsinki, Finland. License: CC BY 4.0.Recognizing HAE is often difficult due to a wide variability in disease expression:
Blood tests often used to confirm the diagnosis:
| Type of angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema without urticaria Urticaria Urticaria is raised, well-circumscribed areas (wheals) of edema (swelling) and erythema (redness) involving the dermis and epidermis with associated pruritus (itch). Urticaria is not a single disease but rather is a reaction pattern representing cutaneous mast cell degranulation. Urticaria (Hives) | C1-INH protein | C1q | C4 & C2 |
|---|---|---|---|
| HAE type I | ↓ | Normal | ↓ |
| HAE type II | N or ↑ (but dysfunctional) | Normal | ↓ |
| Acquired angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema with C1-INH deficiency (type I) | ↓ | ↓ | ↓ |
| Acquired angioedema Angioedema Angioedema is a localized, self-limited (but potentially life-threatening), nonpitting, asymmetrical edema occurring in the deep layers of the skin and mucosal tissue. The common underlying pathophysiology involves inflammatory mediators triggering significant vasodilation and increased capillary permeability. Angioedema with C1-INH deficiency (type II) | ↓ | ↓ | ↓ |
Management focuses on treating attacks based on specific symptoms: