Renal Na+ and water regulation work in tandem to control how fluid is distributed throughout the compartments of the body. Sodium Sodium A member of the alkali group of metals. It has the atomic symbol na, atomic number 11, and atomic weight 23. Hyponatremia is the body’s dominant extracellular solute, and is responsible for the osmotic force that keeps differing amounts of water in each compartment. Changes in Na+ balance are sensed by the body through changes in blood volume. Changes in water balance are sensed by the body through changes in plasma osmolality Plasma osmolality Volume Depletion and Dehydration. Both ultimately send feedback signals to the kidneys Kidneys The kidneys are a pair of bean-shaped organs located retroperitoneally against the posterior wall of the abdomen on either side of the spine. As part of the urinary tract, the kidneys are responsible for blood filtration and excretion of water-soluble waste in the urine. Kidneys: Anatomy to ensure that homeostasis Homeostasis The processes whereby the internal environment of an organism tends to remain balanced and stable. Cell Injury and Death is maintained. Abnormalities in these processes can result in problems in volume status Volume Status ACES and RUSH: Resuscitation Ultrasound Protocols (e.g., hypertension Hypertension Hypertension, or high blood pressure, is a common disease that manifests as elevated systemic arterial pressures. Hypertension is most often asymptomatic and is found incidentally as part of a routine physical examination or during triage for an unrelated medical encounter. Hypertension, pulmonary edema Pulmonary edema Pulmonary edema is a condition caused by excess fluid within the lung parenchyma and alveoli as a consequence of a disease process. Based on etiology, pulmonary edema is classified as cardiogenic or noncardiogenic. Patients may present with progressive dyspnea, orthopnea, cough, or respiratory failure. Pulmonary Edema, pitting edema Pitting edema Edema caused by excess fluid without excess colloid. Leaves “pits” due to fluid displacement when pressure is applied to the area Edema) and dysnatremias ( hyponatremia Hyponatremia Hyponatremia is defined as a decreased serum sodium (sNa+) concentration less than 135 mmol/L. Serum sodium is the greatest contributor to plasma osmolality, which is very tightly controlled via antidiuretic hormone (ADH) release from the hypothalamus and by the thirst mechanism. Hyponatremia and hypernatremia Hypernatremia Hypernatremia is an elevated serum sodium concentration > 145 mmol/L. Serum sodium is the greatest contributor to plasma osmolality, which is very tightly controlled by the hypothalamus via the thirst mechanism and antidiuretic hormone (ADH) release. Hypernatremia occurs either from a lack of access to water or an excessive intake of sodium. Hypernatremia).
Last updated: Jul 21, 2023
To understand renal sodium Sodium A member of the alkali group of metals. It has the atomic symbol na, atomic number 11, and atomic weight 23. Hyponatremia and water regulation, it is important to understand how water is normally distributed in the body.
Total body water Total body water Body Fluid Compartments ( TBW TBW Body Fluid Compartments):
Intracellular fluid Intracellular fluid The fluid inside cells. Body Fluid Compartments ( ICF ICF The fluid inside cells. Body Fluid Compartments):
Extracellular fluid Extracellular fluid The fluid of the body that is outside of cells. It is the external environment for the cells. Body Fluid Compartments (ECF):
Plasma osmolality Plasma osmolality Volume Depletion and Dehydration refers to the combined concentration of all solutes in the blood.
Plasma Plasma The residual portion of blood that is left after removal of blood cells by centrifugation without prior blood coagulation. Transfusion Products tonicity refers to the concentration of only the osmotically active Osmotically Active Osmotic Diuretics solutes in blood and is often referred to as effective osmolality.
A nephron Nephron The functional units of the kidney, consisting of the glomerulus and the attached tubule. Kidneys: Anatomy is the functional unit of the kidney through which fluid and solutes, including Na+, are filtered, reabsorbed, and secreted.
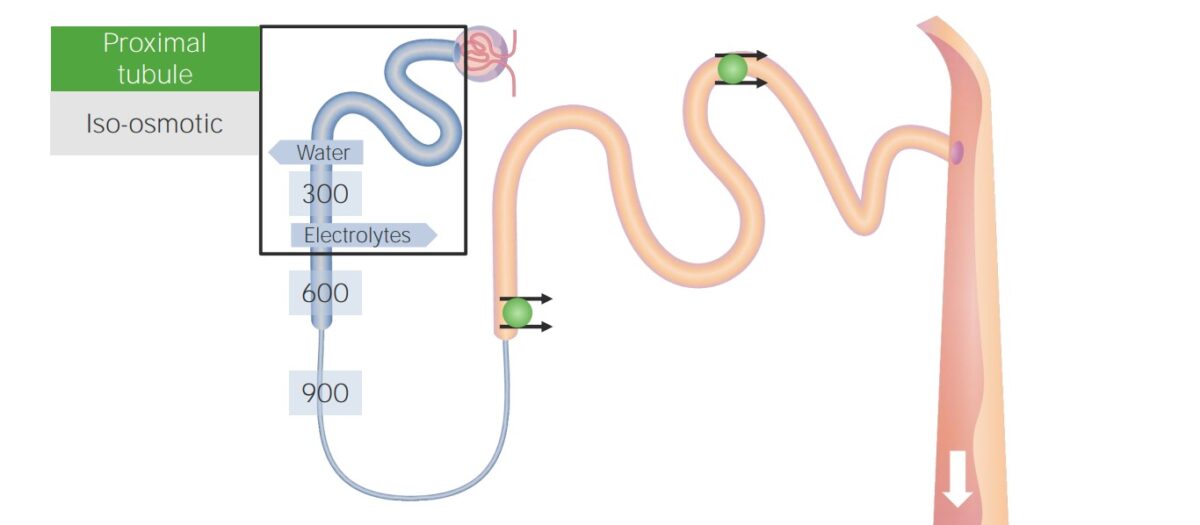
Reabsorption in the proximal tubule:
The numbers overlying the tubules represent the osmolality of the surrounding tissue.
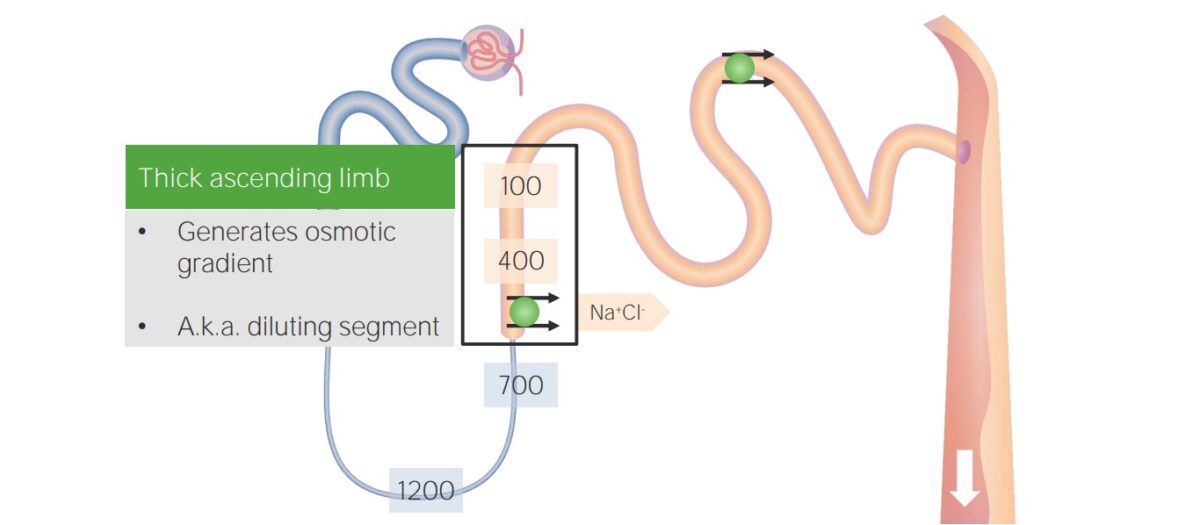
Reabsorption in the thick ascending limb:
Sodium, potassium, and chloride are reabsorbed through the NKCC2 cotransporter, but the thick ascending limb is not permeable to water. The thick ascending limb is a diluting segment of the nephron.
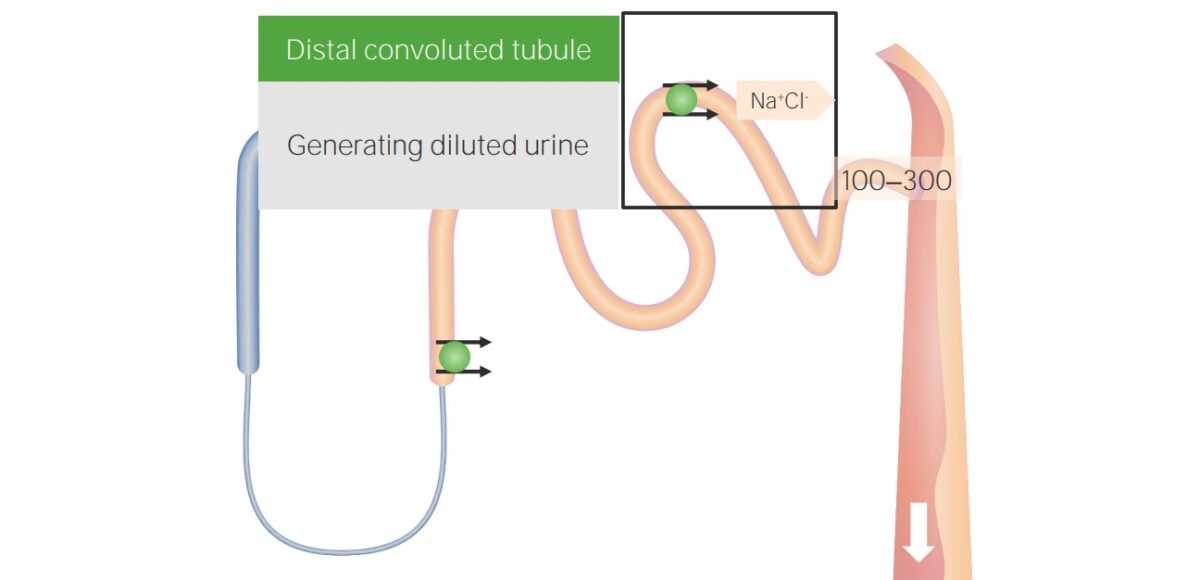
Reabsorption in the distal convoluted tubule (DCT):
Sodium and chloride are reabsorbed in the DCT, but the DCT is not permeable to water. The DCT is another diluting segment.
The body regulates Na+ balance by sensing changes in the effective circulating volume ( ECV ECV A procedure in which the physician attempts to manually rotate the fetus from a breech to a cephalic presentation by pushing on the maternal abdomen Fetal Malpresentation and Malposition), which is also known as the effective arterial blood volume (EABV).
The RAAS RAAS A blood pressure regulating system of interacting components that include renin; angiotensinogen; angiotensin converting enzyme; angiotensin i; angiotensin ii; and angiotensinase. Renin, an enzyme produced in the kidney, acts on angiotensinogen, an alpha-2 globulin produced by the liver, forming angiotensin I. Angiotensin-converting enzyme, contained in the lung, acts on angiotensin I in the plasma converting it to angiotensin II, an extremely powerful vasoconstrictor. Angiotensin II causes contraction of the arteriolar and renal vascular smooth muscle, leading to retention of salt and water in the kidney and increased arterial blood pressure. In addition, angiotensin II stimulates the release of aldosterone from the adrenal cortex, which in turn also increases salt and water retention in the kidney. Angiotensin-converting enzyme also breaks down bradykinin, a powerful vasodilator and component of the kallikrein-kinin system. Adrenal Hormones is stimulated by a low ECV ECV A procedure in which the physician attempts to manually rotate the fetus from a breech to a cephalic presentation by pushing on the maternal abdomen Fetal Malpresentation and Malposition:
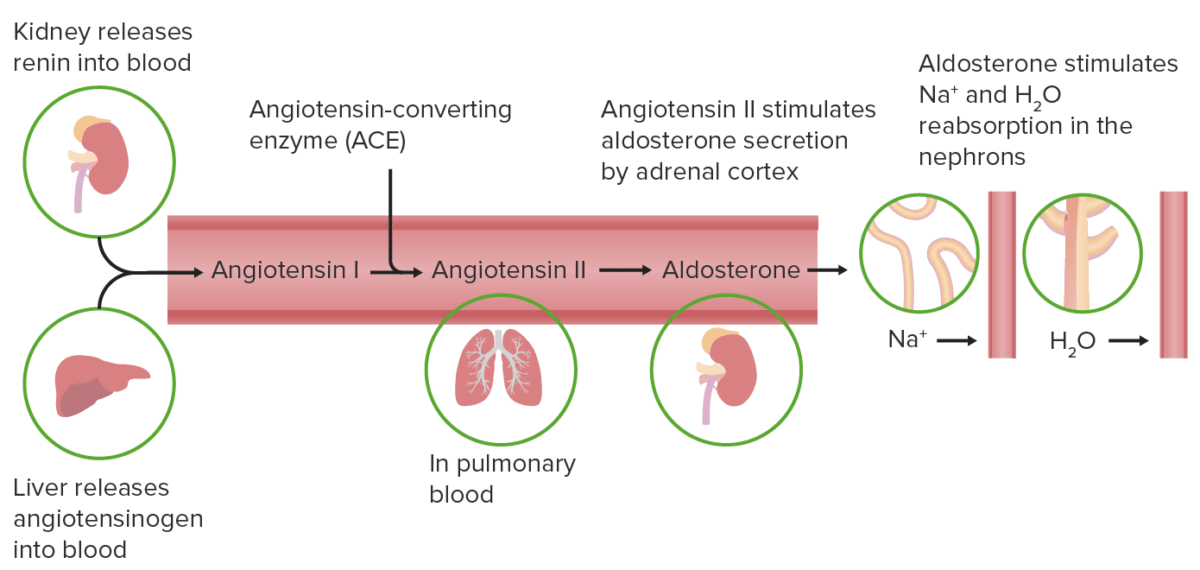
The renin-angiotensin-aldosterone system
Image by Lecturio.Effects of aldosterone Aldosterone A hormone secreted by the adrenal cortex that regulates electrolyte and water balance by increasing the renal retention of sodium and the excretion of potassium. Hyperkalemia:
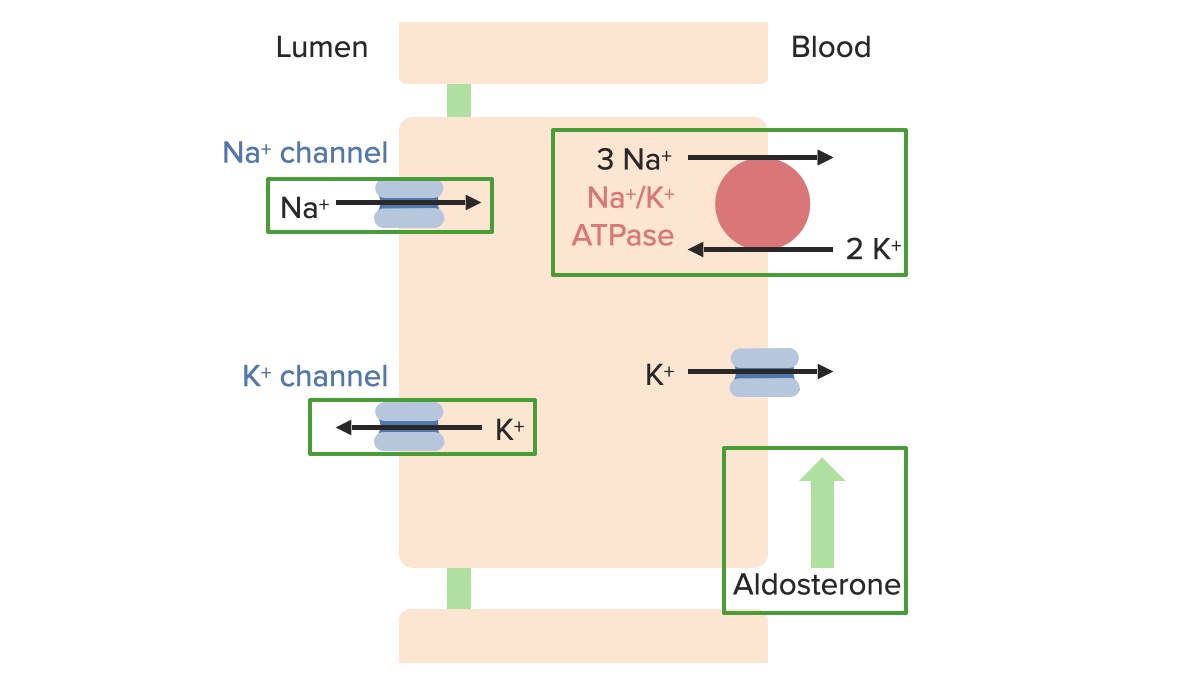
Effects of aldosterone on sodium and potassium regulatory transport proteins in the principal cells of the collecting ducts
Image by Lecturio.Changes in ECV ECV A procedure in which the physician attempts to manually rotate the fetus from a breech to a cephalic presentation by pushing on the maternal abdomen Fetal Malpresentation and Malposition are sensed by the juxtaglomerular apparatus, carotid-sinus and aortic-arch baroreceptors Baroreceptors Receptors in the vascular system, particularly the aorta and carotid sinus, which are sensitive to stretch of the vessel walls. Diabetes Insipidus, and cardiac baroreceptors Baroreceptors Receptors in the vascular system, particularly the aorta and carotid sinus, which are sensitive to stretch of the vessel walls. Diabetes Insipidus.
Water regulation is primarily controlled by osmoreceptors in the hypothalamus Hypothalamus The hypothalamus is a collection of various nuclei within the diencephalon in the center of the brain. The hypothalamus plays a vital role in endocrine regulation as the primary regulator of the pituitary gland, and it is the major point of integration between the central nervous and endocrine systems. Hypothalamus, which maintain plasma osmolality Plasma osmolality Volume Depletion and Dehydration very tightly. Very small changes in plasma osmolality Plasma osmolality Volume Depletion and Dehydration result in changes in ADH release and the sensation of thirst.
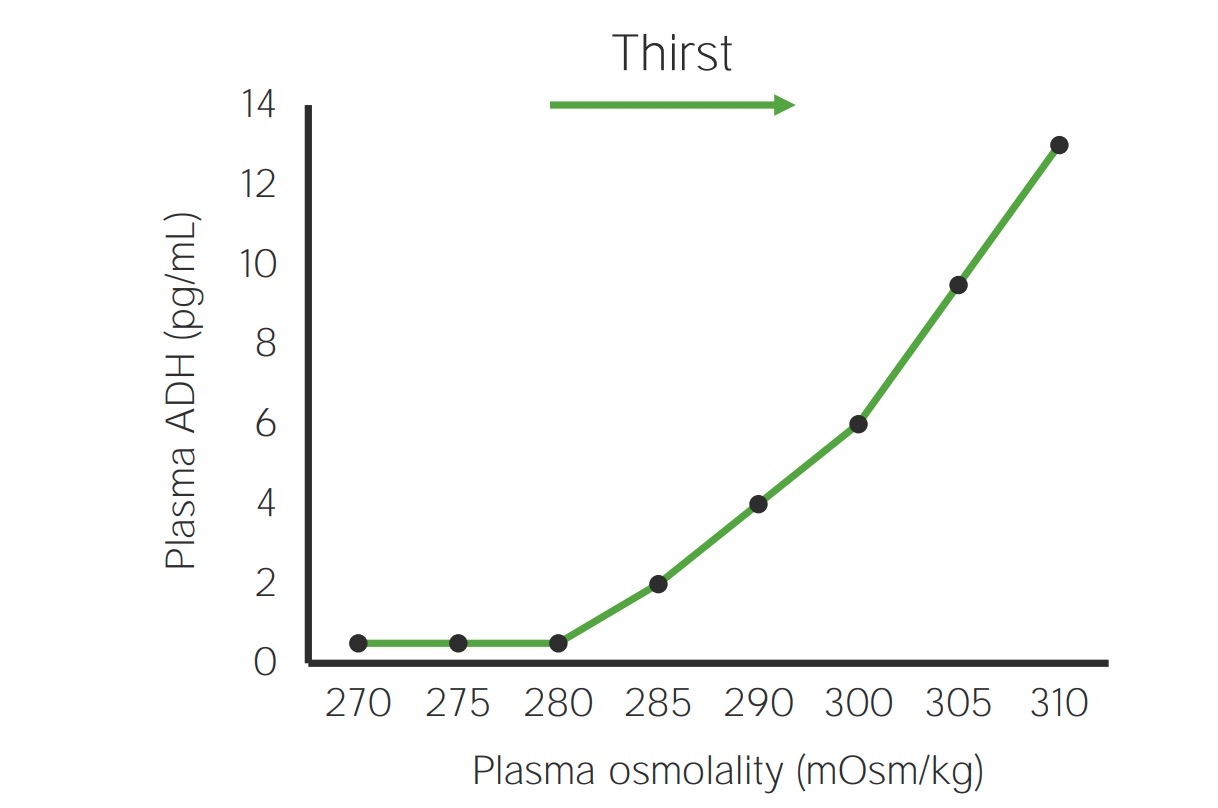
Osmotic antidiuretic hormone (ADH) regulation:
Slight increases in plasma osmolality stimulate ADH release in a linear fashion.
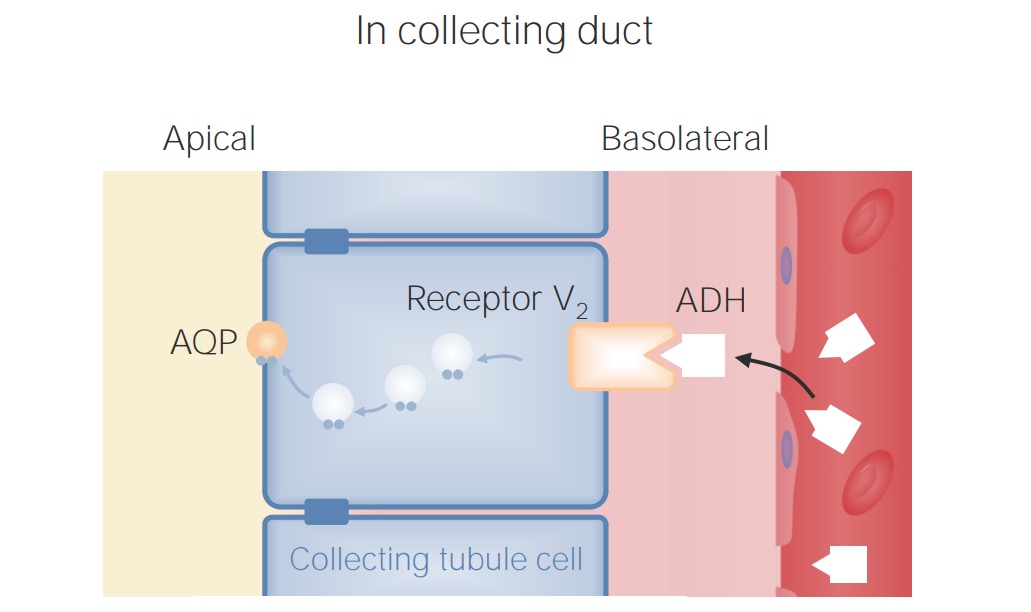
Location and function of the antidiuretic hormone (ADH) V2 receptor in the collecting ducts
AQP: AquaporinVery large decreases in the ECV ECV A procedure in which the physician attempts to manually rotate the fetus from a breech to a cephalic presentation by pushing on the maternal abdomen Fetal Malpresentation and Malposition can independently cause ADH release in an attempt to preserve volume.
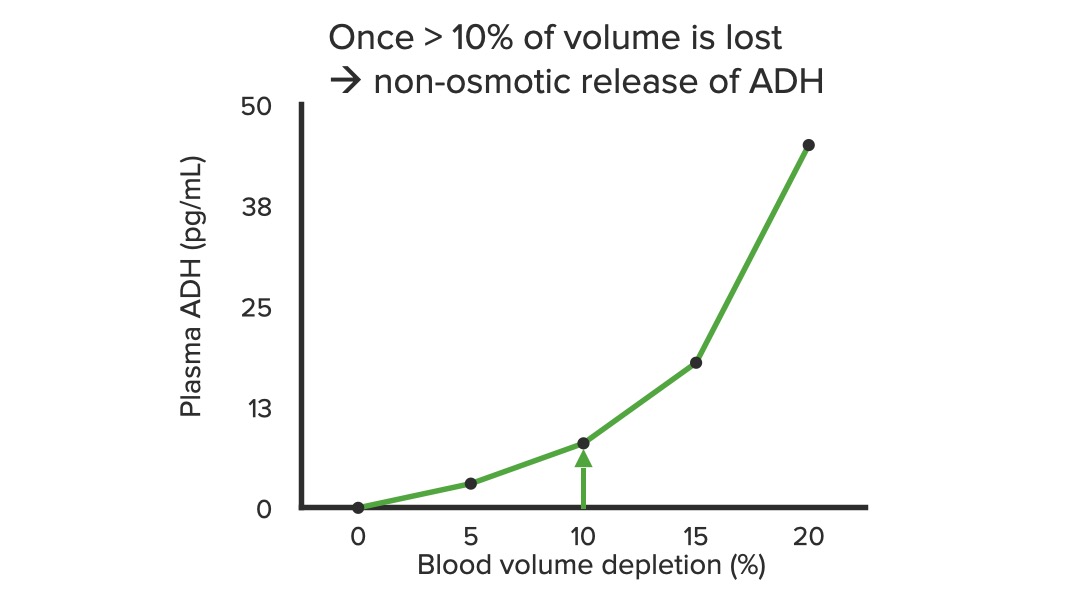
Severe decreases in blood volume stimulate ADH release.
ADH: antidiuretic hormone
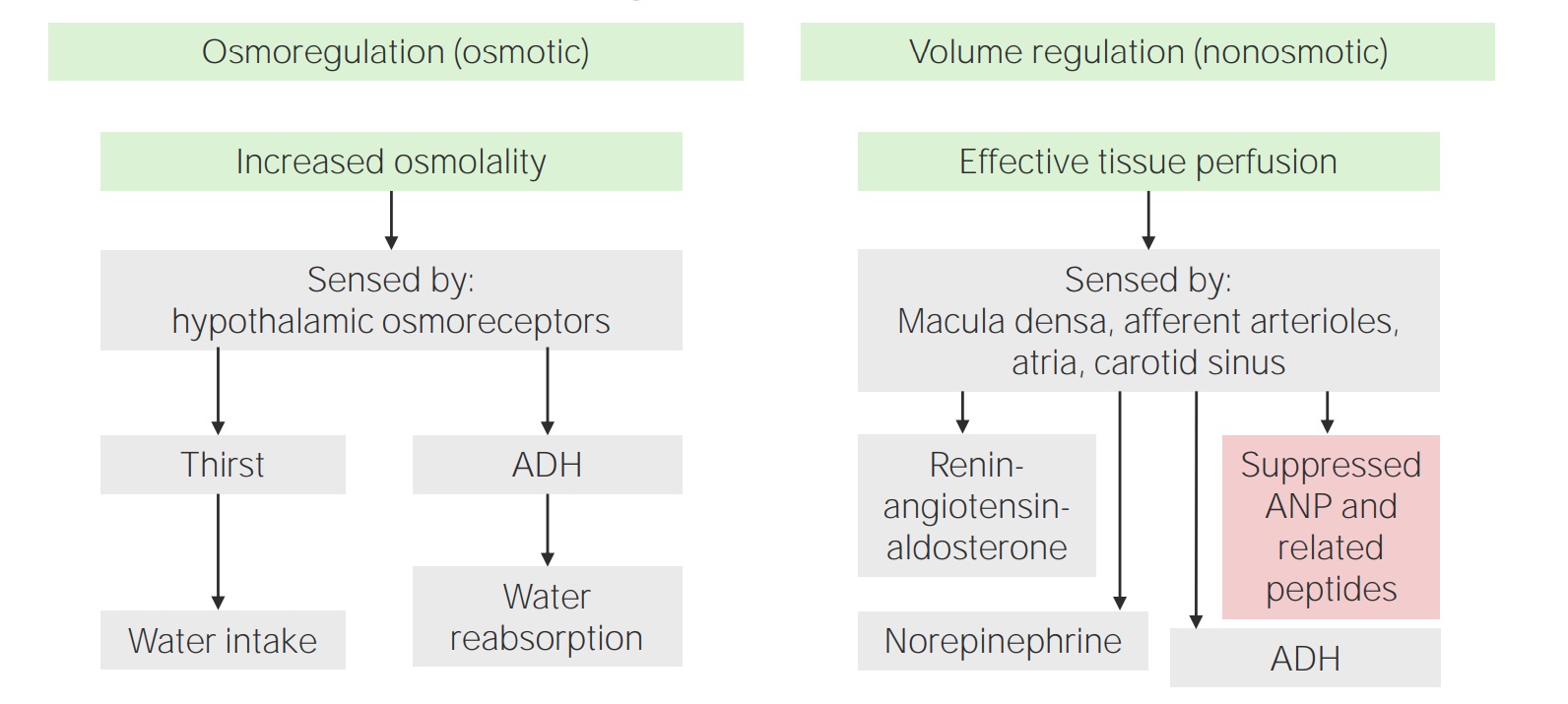
Osmotic and non-osmotic regulation of antidiuretic hormone (ADH)
ANP: Atrial natriuretic peptide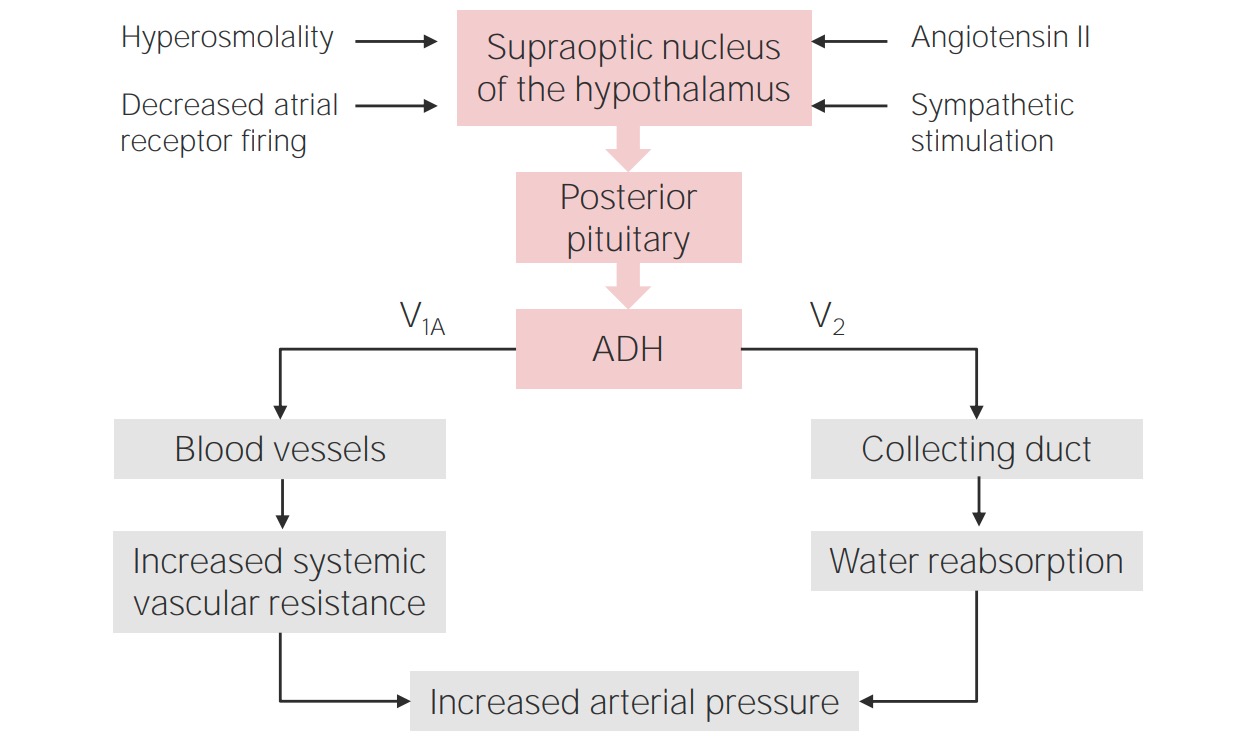
Regulation of antidiuretic hormone
Image by Lecturio.