Conjunctivitis is a common inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body's defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation of the bulbar and/or palpebral conjunctiva Palpebral Conjunctiva Blepharitis. It can be classified into infectious (mostly viral) and noninfectious conjunctivitis, which includes allergic causes. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship commonly present with red eyes, increased tearing, burning, foreign body Foreign Body Foreign Body Aspiration sensation, and photophobia Photophobia Abnormal sensitivity to light. This may occur as a manifestation of eye diseases; migraine; subarachnoid hemorrhage; meningitis; and other disorders. Photophobia may also occur in association with depression and other mental disorders. Migraine Headache. Itching is a chief symptom in allergic conjunctivitis. Treatment depends on the underlying cause and includes antibiotic and antiviral Antiviral Antivirals for Hepatitis B therapy, glucocorticoids Glucocorticoids Glucocorticoids are a class within the corticosteroid family. Glucocorticoids are chemically and functionally similar to endogenous cortisol. There are a wide array of indications, which primarily benefit from the antiinflammatory and immunosuppressive effects of this class of drugs. Glucocorticoids, and antihistamines Antihistamines Antihistamines are drugs that target histamine receptors, particularly H1 and H2 receptors. H1 antagonists are competitive and reversible inhibitors of H1 receptors. First-generation antihistamines cross the blood-brain barrier and can cause sedation. Antihistamines.
Last updated: Dec 15, 2025
Infectious conjunctivitis
Noninfectious conjunctivitis
Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship can present with some or all of the following symptoms:
| Viral conjunctivitis | Bacterial conjunctivitis | Allergic conjunctivitis | |
|---|---|---|---|
| Discharge | Clear, watery discharge | Thick, purulent yellow, white, or green discharge with severe crusting | Clear, watery discharge |
| Eye involvement | Begins unilateral, but usually progresses to bilateral (highly infectious) | Unilateral, can rarely progress to bilateral | Bilateral |
| Conjunctival appearance | Mostly peripheral injection with conjunctival follicles (small swollen papules usually on the palpebral and bulbar conjunctiva Conjunctiva The mucous membrane that covers the posterior surface of the eyelids and the anterior pericorneal surface of the eyeball. Eye: Anatomy) | Diffuse injection, non-follicular | Diffuse injection with chemosis and conjunctival follicles |
| Other symptoms | Extraocular signs of viral infection ( fever Fever Fever is defined as a measured body temperature of at least 38°C (100.4°F). Fever is caused by circulating endogenous and/or exogenous pyrogens that increase levels of prostaglandin E2 in the hypothalamus. Fever is commonly associated with chills, rigors, sweating, and flushing of the skin. Fever, lymphadenopathy Lymphadenopathy Lymphadenopathy is lymph node enlargement (> 1 cm) and is benign and self-limited in most patients. Etiologies include malignancy, infection, and autoimmune disorders, as well as iatrogenic causes such as the use of certain medications. Generalized lymphadenopathy often indicates underlying systemic disease. Lymphadenopathy, pharyngitis Pharyngitis Pharyngitis is an inflammation of the back of the throat (pharynx). Pharyngitis is usually caused by an upper respiratory tract infection, which is viral in most cases. It typically results in a sore throat and fever. Other symptoms may include a runny nose, cough, headache, and hoarseness. Pharyngitis, rash Rash Rocky Mountain Spotted Fever) | Signs of bacterial infection, depending on etiology | Sneezing Sneezing The sudden, forceful, involuntary expulsion of air from the nose and mouth caused by irritation to the mucous membranes of the upper respiratory tract. Rhinovirus, itching, atopic dermatitis Dermatitis Any inflammation of the skin. Atopic Dermatitis (Eczema) |
| Complications |
|
|
|

Patient with bacterial conjunctivitis presenting with characteristic thick yellow purulent discharge
Image: “A swollen, pus-filled eye with conjunctivitis” by Tanalai at English Wkipedia. License: CC BY 3.0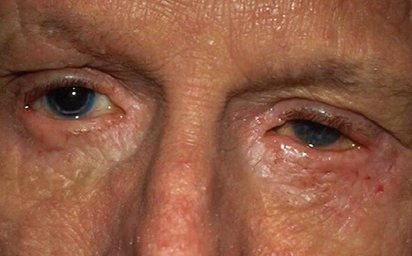
Patient with allergic conjunctivitis presenting with clear, watery discharge and chemosis
Image: “Atopic keratoconjunctivitis” by U.S. National Library of Medicine. License: CC BY 2.0, edited by Lecturio.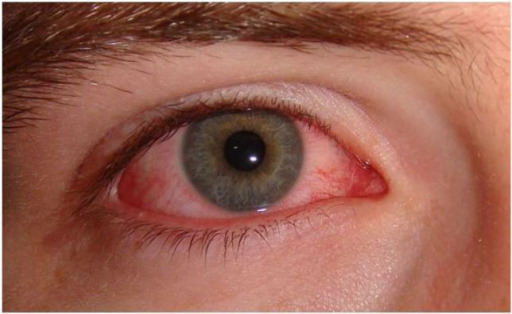
Patient with viral conjunctivitis presenting with significant peripheral injection and no visible discharge
Image: “Acute viral conjunctivitis” by Wikimedia Creative Commons. License: CC BY 4.0
Newborn presenting with gonococcal ophthalmia neonatorum, caused by a maternally transmitted gonococcal infection
Image: “Gonococcal ophthalmia neonatorum” by CDC/J. Pledger. License: Public DomainThe diagnosis is mainly clinical.
Viral conjunctivitis
Bacterial conjunctivitis
Allergic conjunctivitis
The following conditions enter into the differential diagnoses of conjunctivitis: