Helicobacter pylori is a gram-negative bacterium that causes gastric infection. It is the most well known and clinically significant species of Helicobacter. Transmission is believed to occur by ingestion of contaminated food or water; therefore, a higher prevalence Prevalence The total number of cases of a given disease in a specified population at a designated time. It is differentiated from incidence, which refers to the number of new cases in the population at a given time. Measures of Disease Frequency of infection is seen in areas with poor sanitation Sanitation The development and establishment of environmental conditions favorable to the health of the public. Hepatitis E Virus. Certain bacterial features contribute to the pathogenicity of H. pylori: urease Urease An enzyme that catalyzes the conversion of urea and water to carbon dioxide and ammonia. Nocardia/Nocardiosis production (allowing survival in an acidic environment), motility Motility The motor activity of the gastrointestinal tract. Gastrointestinal Motility (permitting movement to the gastric epithelium Epithelium The epithelium is a complex of specialized cellular organizations arranged into sheets and lining cavities and covering the surfaces of the body. The cells exhibit polarity, having an apical and a basal pole. Structures important for the epithelial integrity and function involve the basement membrane, the semipermeable sheet on which the cells rest, and interdigitations, as well as cellular junctions. Surface Epithelium: Histology), and several toxins (creating local damage and inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body's defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation). Chronic infection with H. pylori can lead to peptic ulcer Peptic ulcer Peptic ulcer disease (PUD) refers to the full-thickness ulcerations of duodenal or gastric mucosa. The ulcerations form when exposure to acid and digestive enzymes overcomes mucosal defense mechanisms. The most common etiologies include Helicobacter pylori (H. pylori) infection and prolonged use of non-steroidal anti-inflammatory drugs (NSAIDs). Peptic Ulcer Disease disease or even gastric cancer Gastric cancer Gastric cancer is the 3rd-most common cause of cancer-related deaths worldwide. The majority of cases are from adenocarcinoma. The modifiable risk factors include Helicobacter pylori infection, smoking, and nitrate-rich diets. Gastric Cancer in severe cases.
Last updated: Apr 2, 2025
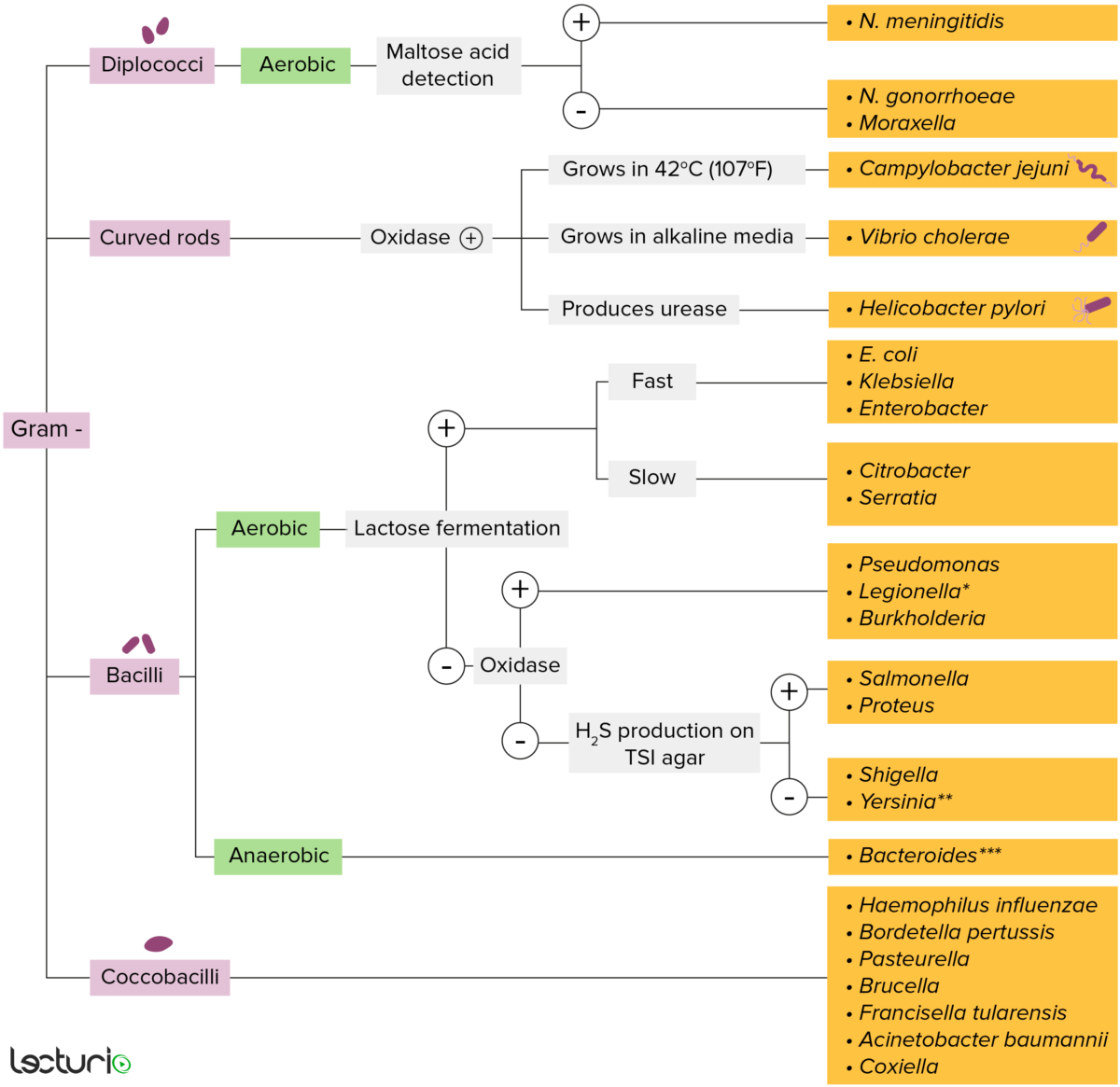
Gram-negative bacteria:
Most bacteria can be classified according to a lab procedure called Gram staining.
Bacteria with cell walls that have a thin layer of peptidoglycan do not retain the crystal violet stain utilized in Gram staining. These bacteria do, however, retain the safranin counterstain and thus appear as pinkish-red on the stain, making them gram negative. These bacteria can be further classified according to morphology (diplococci, curved rods, bacilli, and coccobacilli) and their ability to grow in the presence of oxygen (aerobic versus anaerobic). The bacteria can be more narrowly identified by growing them on specific media (triple sugar iron (TSI) agar) where their enzymes can be identified (urease, oxidase) and their ability to ferment lactose can be tested.
* Stains poorly on Gram stain
** Pleomorphic rod/coccobacillus
*** Require special transport media
Features:
Helicobacter genus contains about 35 species, with H. pylori being the most well-known.
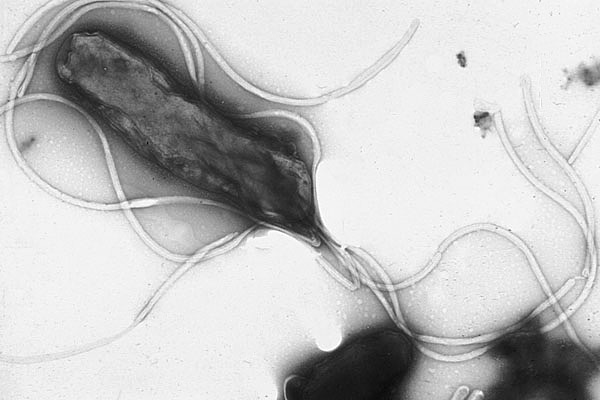
Electron micrograph of Helicobacter pylori possessing multiple flagella (negative staining)
Image: “Electron micrograph of helicobacter pylori” by Yutaka Tsutsumi, M.D. License: Public Domain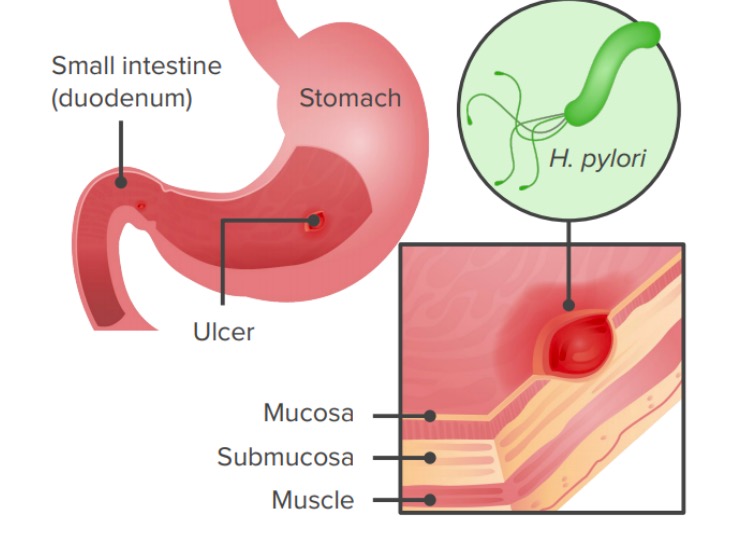
Infection by Helicobacter pylori via ingestion of a pathogen results in gastric ulcers or gastritis.
Image by Lecturio.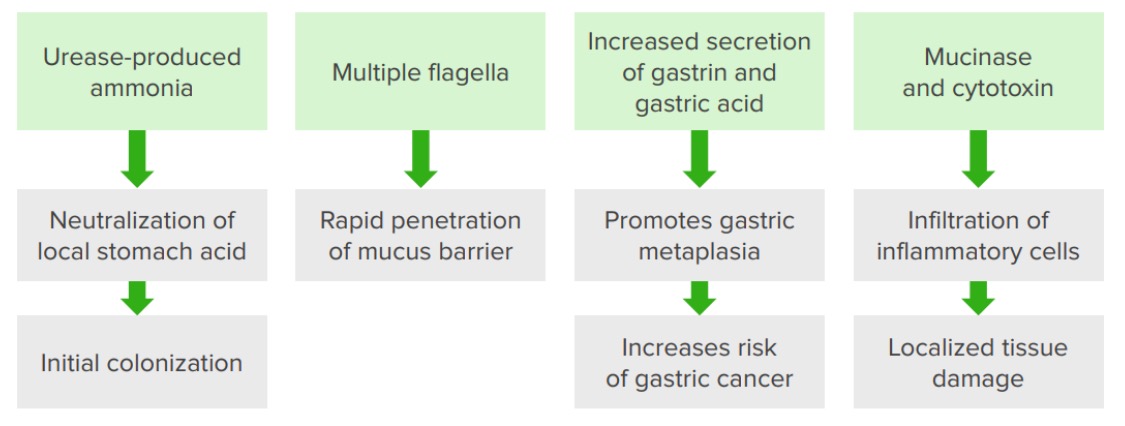
Pathogenic features of Helicobacter pylori
Image by Lecturio.In H. pylori infection: