Bowen disease and erythroplasia of Queyrat are 2 related entities that describe squamous cell carcinoma Squamous cell carcinoma Cutaneous squamous cell carcinoma (cSCC) is caused by malignant proliferation of atypical keratinocytes. This condition is the 2nd most common skin malignancy and usually affects sun-exposed areas of fair-skinned patients. The cancer presents as a firm, erythematous, keratotic plaque or papule. Squamous Cell Carcinoma (SCC) (SCC) in situ of the skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions. Bowen disease usually presents in sun-exposed areas (e.g., face and forearms) as a red, scaly skin Skin The skin, also referred to as the integumentary system, is the largest organ of the body. The skin is primarily composed of the epidermis (outer layer) and dermis (deep layer). The epidermis is primarily composed of keratinocytes that undergo rapid turnover, while the dermis contains dense layers of connective tissue. Skin: Structure and Functions lesion. The lesion can occur in other areas as well. The genital region, particularly the penile shaft, is also affected. When the glans penis Glans Penis Penis: Anatomy is involved, the lesion is called erythroplasia of Queyrat, with uncircumcised males being at high risk. Both genital lesions have HPV HPV Human papillomavirus (HPV) is a nonenveloped, circular, double-stranded DNA virus belonging to the Papillomaviridae family. Humans are the only reservoir, and transmission occurs through close skin-to-skin or sexual contact. Human papillomaviruses infect basal epithelial cells and can affect cell-regulatory proteins to result in cell proliferation. Papillomavirus (HPV) infection as a risk factor. Pathologic findings show full-thickness atypia Atypia Fibrocystic Change without basement membrane Basement membrane A darkly stained mat-like extracellular matrix (ecm) that separates cell layers, such as epithelium from endothelium or a layer of connective tissue. The ecm layer that supports an overlying epithelium or endothelium is called basal lamina. Basement membrane (bm) can be formed by the fusion of either two adjacent basal laminae or a basal lamina with an adjacent reticular lamina of connective tissue. Bm, composed mainly of type IV collagen; glycoprotein laminin; and proteoglycan, provides barriers as well as channels between interacting cell layers. Thin Basement Membrane Nephropathy (TBMN) invasion. Both entities may progress to invasive SCC. Thus, local destruction via surgical excision or topical chemotherapy Chemotherapy Osteosarcoma should be performed.
Last updated: Dec 15, 2025
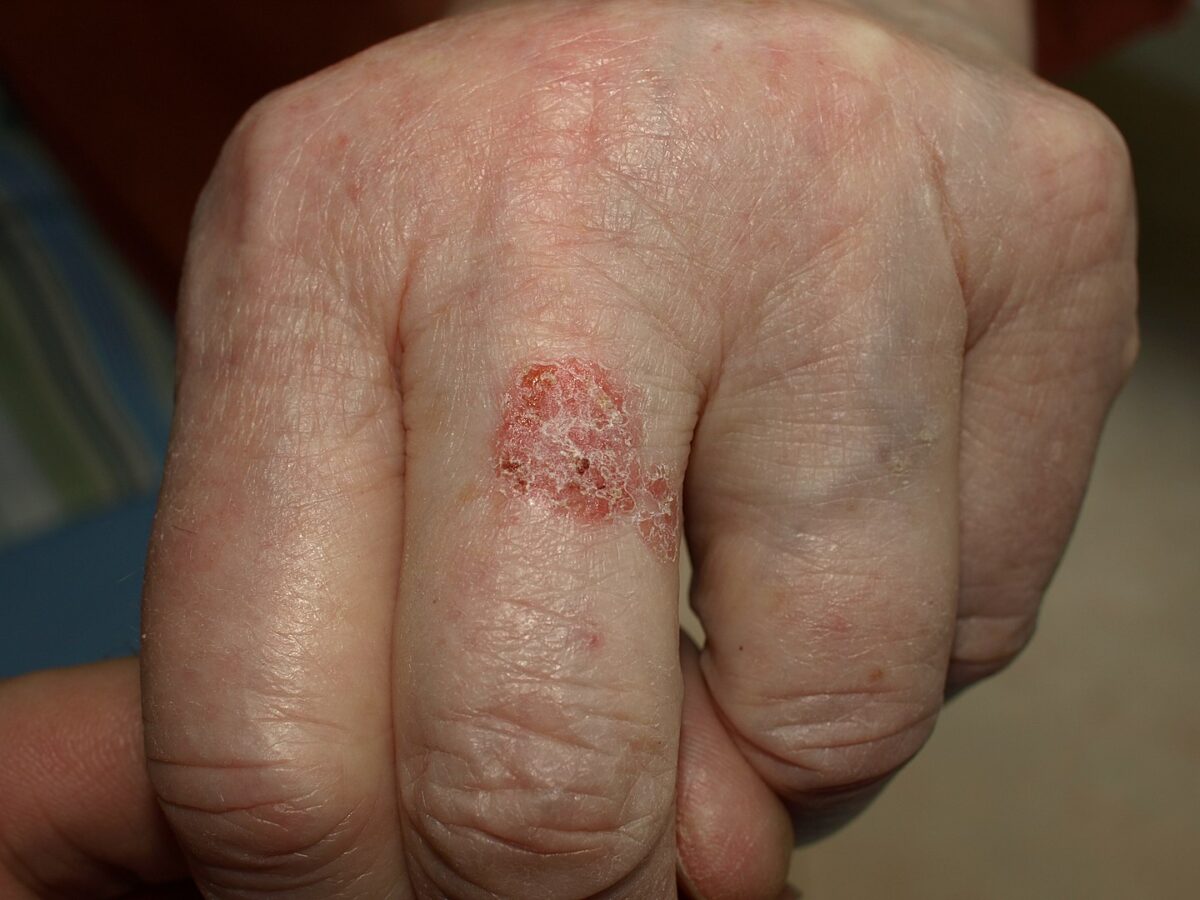
Bowen disease in an 81-year-old-woman
Image: “Bowen11” by Klaus D. Peter. License: CC BY 3.0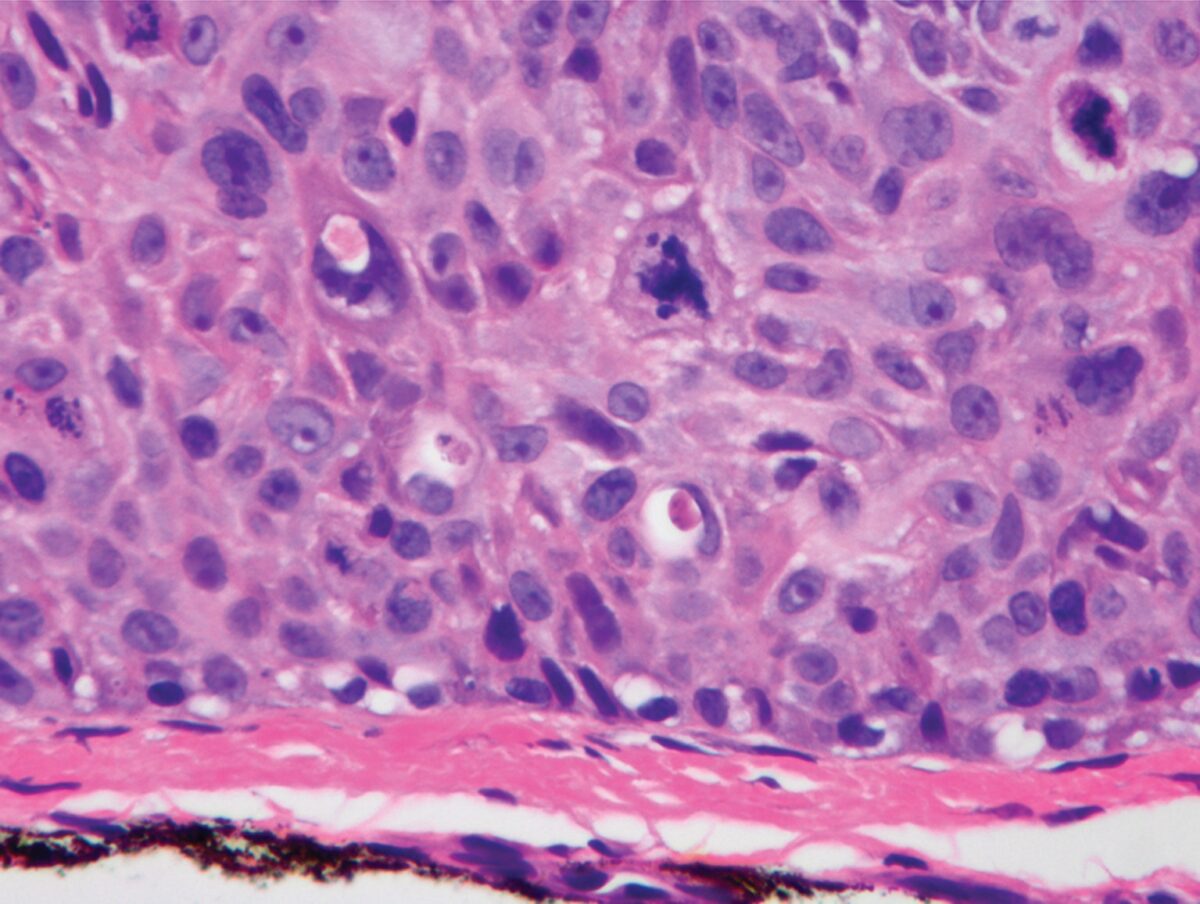
Bowen disease:
There is full-thickness atypia with intact basement membrane.
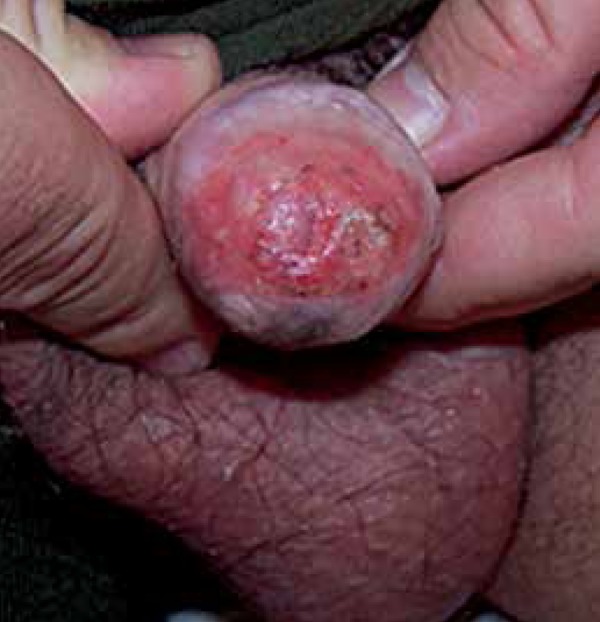
Erythroplasia of Queyrat
Image: “Figure 1” by João Roberto Antônio et al. License: Public Domain