Start your online rheumatology video course
with Steven Holt, MD from the Yale School of Medicine
Rheumatology works towards improving long-term health outcomes of patients affected by rheumatic disorders that profoundly affect mobility and quality of life. The complexity of autoimmune and non-autoimmune joint diseases, combined with their overlapping symptoms and the need for precise treatment strategies, poses a significant challenge.
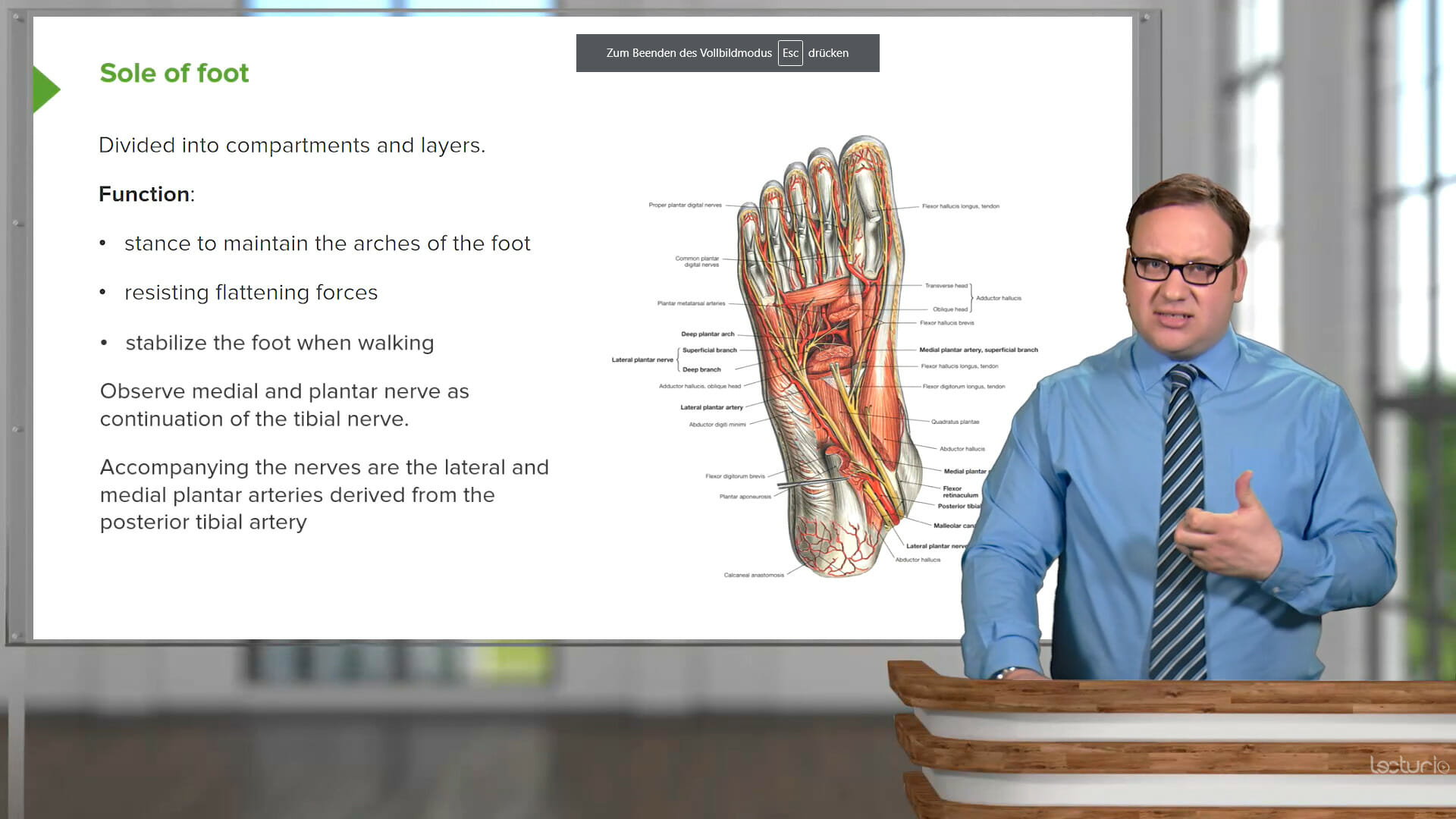
This course will provide you with an in-depth understanding of the pathophysiology, diagnosis, and management of key rheumatic diseases, including arthritis, connective tissue diseases, spondyloarthritides, non-autoimmune arthritis, and vasculitides. Dr. Stephen Holt, MD, from the Yale School of Medicine leads this course with case-based presentations that not only illustrate the theory but show how to practically apply it in the approach to patients with joint pain.
The combination of Video Lessons with interactive quiz questions, downloadable study materials, and a USMLE-style Qbank makes it easy to understand and retain the topics. By the end of this course, you will be equipped with the foundational knowledge and skills needed to effectively identify and manage rheumatic diseases, helping you make a lasting impact on their quality of life.