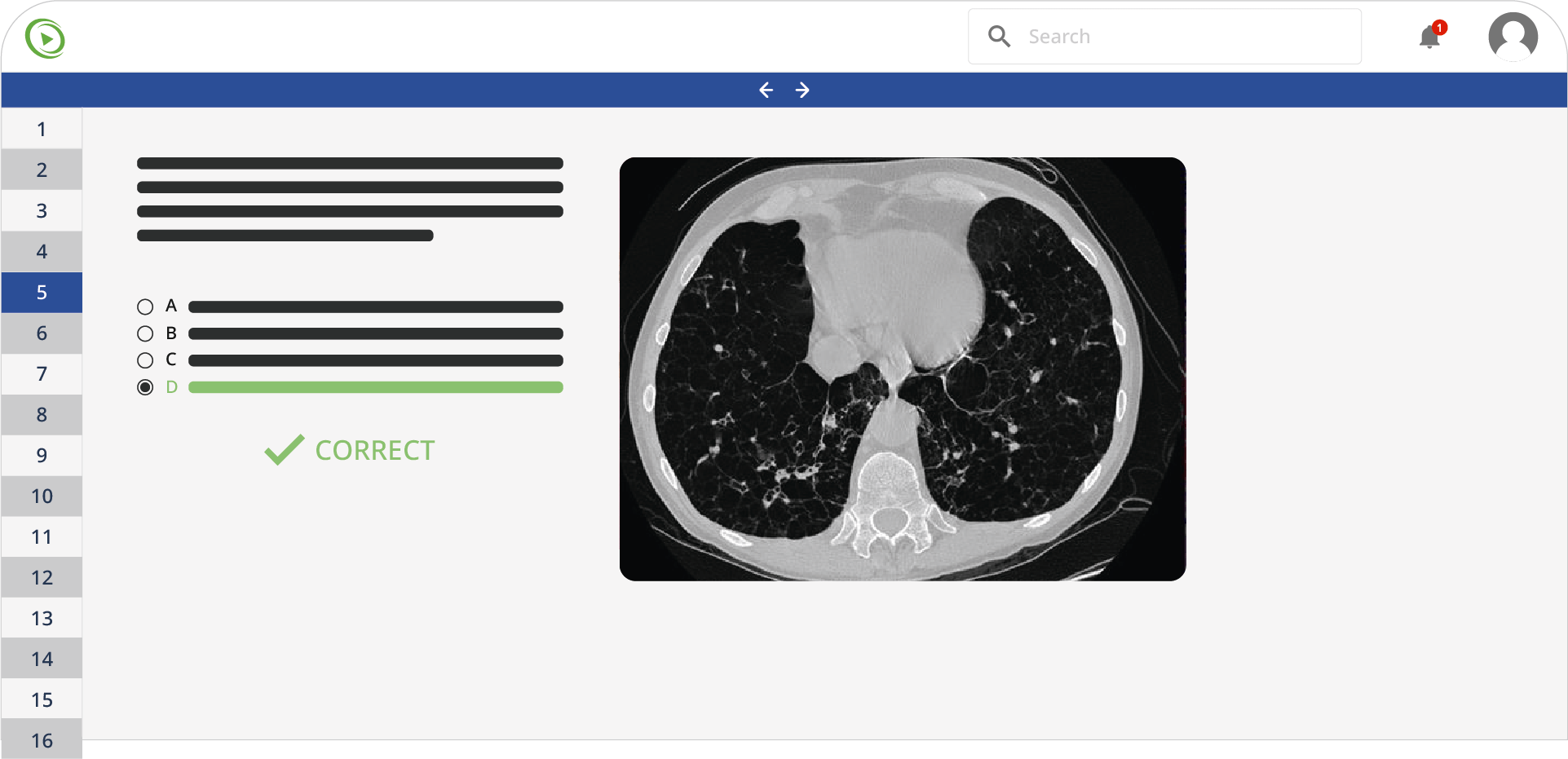
A 70-year-old man presents to a medical clinic reporting blood in his urine and lower abdominal pain for the past few days. He is also concerned about urinary frequency and urgency. He states that he recently completed a cycle of chemotherapy for non-Hodgkin lymphoma. Which medication in the chemotherapy regimen most likely caused his symptoms?
A. Cytarabine
B. Methotrexate
C. Rituximab
D. Cyclophosphamide
E. Prednisone
A 22-year-old man presents with abdominal cramps and diarrhea over the last few weeks. He notes that several of his bowel movements have a small amount of blood. Past medical history is significant for an intermittent cough that has been persistent since returning from Mexico last month. The patient takes no current medications. On physical examination, there is diffuse tenderness to palpation. Which of the following medications is indicated for this patient’s condition?
A. Mebendazole
B. Ivermectin
C. Albendazole
D. Pyrantel
E. Praziquantel
A 25-year-old G1P0 woman at an estimated gestational age of 9 weeks presents for her first prenatal visit following a positive home pregnancy test. She says she missed 2 periods but assumed it was due to stress at work. She has decided to continue with the pregnancy. Her past medical history is significant for migraine headaches, seizures, and asthma. She takes multiple medications for her condition. Physical examination is unremarkable. An ultrasound confirms a 9-week-old intrauterine pregnancy. Which of these following medications poses the greatest risk to the fetus?
A. Acetaminophen
B. Sumatriptan
C. Valproic acid
D. Albuterol
E. Budesonide
A 35-year-old man who works in a shipyard presents with a sharp pain in his left big toe for the past 5 hours. He says he had similar pain a few weeks ago after an evening of heavy drinking with his friends. He denies any recent history of trauma or fever. There is no significant past medical history and he takes no medications. Family history is significant for a mother who has type 2 diabetes mellitus and a father who has hypertension. He reports regular drinking and the occasional binge on weekends, but denies any smoking history or recreational drug use. The vital signs include: pulse 86/min, respiratory rate 14/min, and blood pressure 130/80 mm Hg. On physical examination, the patient is slightly overweight and in obvious distress. The 1st metatarsophalangeal joint of the left foot is erythematous, severely tender to touch, and swollen. No obvious deformity is seen. Arthrocentesis of the 1st left metatarsophalangeal joint reveals sodium urate crystals. Which of the following would be the most appropriate next step in management?
A. Probenecid
B. Morphine
C. Aspirin
D. Allopurinol
E. Naproxen
A 59-year-old man presents with intense, sharp pain in his toe for the past hour. He reports similar symptoms in the past and this is his 2nd visit to the emergency department this year with the same complaint. The patient is afebrile and the vital signs are within normal limits. On physical examination, there is significant erythema, swelling, warmth, and moderate pain on palpation of the right 1st toe. The remainder of the examination is unremarkable. A plain radiograph of the right foot reveals no abnormalities. Joint arthrocentesis of the inflamed toe reveals urate crystals. Laboratory studies show:
| Serum glucose (random) | 170 mg/dL |
| Sodium | 140 mEq/L |
| Potassium | 4.1 mEq/L |
| Chloride | 100 mEq/L |
| Uric acid | 7.2 mg/dL |
| Serum creatinine | 0.8 mg/dL |
| Blood urea nitrogen | 9 mg/dL |
| Cholesterol, total | 170 mg/dL |
| HDL-cholesterol | 43 mg/dL |
| LDL-cholesterol | 73 mg/dL |
| Triglycerides | 135 mg/dL |
HDL: high-density lipoprotein; LDL: low-density lipoprotein
Ibuprofen is prescribed for the acute treatment of this patient’s symptoms. He is also put on chronic therapy to prevent the recurrence of future attacks. Which of the following drugs is 1st-line for chronic therapy of gout?
A. Methotrexate
B. Colchicine
C. Allopurinol
D. Indomethacin
E. Probenecid
A 30-year-old woman came to her OBGYN for an infertility consultation. The patient reports having intercourse with her husband at least 3 times per week with increasing frequency during the periods. The lab reports of her husband revealed an adequate sperm count. After the work-ups was complete, her OBGYN prescribed a medication similar to GnRH to be administered in a pulsatile manner. Which drug is prescribed to the patient?
A. Danazol
B. Leuprolide
C. Anastrazole
D. Clomiphene
E. Mestranol
A 20-year-old man is found lying unconscious on the floor of his room by his roommate. The paramedics arrive at the site and find him unresponsive with cold, clammy extremities and constricted, non-reactive pupils. He smells of alcohol and his vital signs show the following: blood pressure 110/80 mm Hg, pulse 100/min, and respiratory rate 8/min. Intravenous access is established and dextrose is administered. The roommate suggests the possibility of drug abuse by the patient. He says he has seen the patient sniff a powdery substance, and he sees the patient inject himself often but has never confronted him about it. After the initial assessment, the patient is given medication and, within 5–10 minutes of administration, the patient regains consciousness and his breathing improves. He is alert and cooperative within the next few minutes. Which of the following drugs was given to this patient to help alleviate his symptoms?
A. Ethanol
B. Methadone
C. Naloxone
D. Atropine
E. Dextrose
On the 3rd day post-anteroseptal myocardial infarction (MI), a 55-year-old man who was admitted to the intensive care unit is undergoing an examination by his physician. The patient complains of the new onset of precordial pain which radiates to the trapezius ridge. The nurse informs the physician that his temperature was 37.7°C (99.9°F), 2 hours ago. On physical examination, the vital signs are stable, but the physician notes the presence of a triphasic pericardial friction rub on auscultation. A bedside electrocardiogram (ECG) shows persistent positive T waves in leads V1–V3 and an ST-segment: T wave ratio of 0.27 in lead V6. Which of the following is the drug of choice to treat the condition the patient has developed?
A. Aspirin
B. Colchicine
C. Clarithromycin
D. Furosemide
E. Prednisone
A 40-year-old man presents with left hip pain. He says that symptoms started a month ago and have progressively worsened. He says the pain has rendered him unable to report to work for the last 2 weeks. The pain was initially 4/10 in intensity, dull with no radiation and was aggravated to 5/10 in intensity upon weight-bearing. Initially, it improved with rest and Tylenol. He initially attributed it to heavy work and took a few days off work, but he did not seek medical attention. However, it worsened over time to its present 8/10 intensity and does not respond to Tylenol anymore. The patient denies any history of injury, weight loss, change in appetite, or recent travel. His past medical history is significant for Crohn’s disease, managed with a combination of prednisone and mesalamine and presently in remission. On physical examination, there is limited flexion and extension at the left hip. The rest of the examination, including a complete neurological examination, is unremarkable. On abdominal imaging of the left hip joint, a transcervical fracture is noted in the left hip with surrounding bony sclerosis. A DEXA scan shows a T-score of -2.5 at the hips and -1.5 at the lumbar spine (normal T-score ≥ -1.0). Which of the following is most likely to be the underlying cause for the fracture in this patient?
A. Trauma
B. Chronic steroid use
C. Pott’s disease
D. Metastatic lesion
E. Sciatica
A 49-year-old man seeks evaluation at an urgent care clinic with a complaint of palpitations for the past few hours. He denies any chest pain, shortness of breath, or sweating. He is anxious and appears worried. His medical history is unremarkable with the exception of mild bronchial asthma. He only uses medications during an asthma attack and has not used medications since last week. He is a former smoker and drinks a couple of beers on weekends. His heart rate is 136/min, the respiratory rate is 16/min, the temperature is 37.6°C (99.7°F), and the blood pressure is 120/80 mm Hg. The physical examination is unremarkable, and an electrocardiogram is ordered. Which of the following groups of drugs should be given to treat his symptoms?
A. α1-receptor antagonist
B. Selective β1-receptor antagonist
C. Non-selective β-receptor antagonist
D. α-receptor agonist
E. β-receptor agonist
A 38-year-old man presents to his physician with recurrent episodes of facial swelling and abdominal pain. He reports that these episodes started when he was approx. 16 years of age. His mother also has similar episodes of swelling accompanied by the swelling of her extremities. The vital signs include: blood pressure 140/80 mm Hg, heart rate 74/min, respiratory rate 17/min, and temperature 36.6°C (97.8°F). His physical examination is unremarkable. The laboratory workup shows the following findings:
| Test | Result | Normal range |
| C1 esterase inhibitor | 22% | > 60% |
| Complement C4 level | 9 mg/dL | 14–40 mg/dL |
| Complement C2 level | 0.8 mg/dL | 1.1–3.0 mg/dL |
| Complement component 1q | 17 mg/dL | 12–22 mg/dL |
Which of the following antihypertensive medications is contraindicated in this patient?
A. Amlodipine
B. Valsartan
C. Fosinopril
D. Atenolol
E. Indapamide
A 48-year-old woman underwent a thyroidectomy with central neck dissection due to papillary thyroid carcinoma. On day 2 postoperatively, she developed irritability, dysphagia, difficulty breathing, and spasms in different muscle groups in her upper and lower extremities. The vital signs include blood pressure 102/65 mm Hg, heart rate 93/min, respiratory rate 17/min, and temperature 36.1℃ (97.0℉). Physical examination shows several petechiae on her forearms, muscle twitching in her upper and lower extremities, expiratory wheezes on lung auscultation, decreased S1 and S2 and the presence of an S3 on cardiac auscultation, and positive Trousseau and Chvostek signs. Laboratory studies show:
| Ca2+ | 4.4 mg/dL |
| Mg2+ | 1.7 mEq/L |
| Na+ | 140 mEq/L |
| K+ | 4.3 mEq/L |
| Cl– | 107 mEq/L |
| HCO3– | 25 mEq/L |
Administration of which of the following agents could prevent the patient’s condition?
A. Anticonvulsants prior to and for 1 week after the operation
B. Magnesium sulfate intraoperatively
C. Vitamin D and ionic calcium prior to and 2 weeks after the operation
D. Calcium gluconate intraoperatively
E. Potassium supplementation prior to and 2 weeks after the operation
Do you want to practice more Pharmacology questions?
Create a free Lecturio account and you’ll have access to the Lecturio question bank, with more than 2,200 USMLE Step 1 practice questions.