A 5-year-old boy presents to his pediatrician for a well-child visit. His mother reports that he is doing well and that she has no concerns. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. On physical examination, the patient is noted to have a right upper extremity blood pressure of 150/80 mm Hg. In addition, 2+ radial pulses and trace femoral pulses are felt. Cardiac auscultation reveals a regular heart rate and rhythm with normal S1 and S2. A 2/6 long systolic murmur with a systolic ejection click is heard over the left sternal border and the back. The point of maximal impact is normal. Which of the following is the most likely diagnosis in this patient?
A. Takayasu arteritis
B. Interrupted aortic arch
C. Pheochromocytoma
D. Coarctation of the aorta
E. Essential hypertension
A healthy, full-term 1-day-old girl is being evaluated after birth and is noted to have a cleft palate and a systolic ejection murmur at the second left intercostal space. A chest radiograph is obtained that reveals a boot-shaped heart and the absence of a thymus. An echocardiogram is done that shows pulmonary stenosis with a hypertrophic right ventricular wall, ventricular septal defect, and overriding of the aorta. Which of the following additional features is expected to be seen in this patient?
A. Seizures due to hypocalcemia
B. Catlike cry
C. Hyperthyroidism from transplacental antibodies
D. Webbing of the neck
E. Increased phenylalanine in the blood
A 3-month-old baby died suddenly at night while asleep. His mother noticed that he had died only after she awoke in the morning. No cause of death was determined based on the autopsy. He had no known medical problems and took no medications. The mother’s pregnancy was uneventful, and the baby was born at full term. There was no family history of any similar events. Which of the following precautions would most likely have prevented the death of the baby?
A. Placing the infant in a supine position on a firm mattress while sleeping
B. Routine postnatal electrocardiogram (ECG)
C. Keeping the infant covered and maintaining a high room temperature
D. Application of a device to maintain the sleeping position
E. Home respiratory, cardiac, and oxygen (O2) saturation monitoring
F. Avoiding pacifier use during sleep
An 18-month-old boy is brought to the emergency department after losing consciousness. His mother states that he was running with other kids in the park when he suddenly fell down and became unresponsive for less than 1 minute. He has not had any immunizations due to their religious beliefs. The parents report that he plays with other children, but tires easily. He has had difficulty feeding, but there was no follow-up with a pediatrician. The heart rate was 120/min and the oxygen saturation was 91%. The height is in the 40th percentile and the weight is in the 50th percentile. On examination, the boy is crying with perioral cyanosis. The lung sounds are clear. S-1 is normal and there is a single S-2. A grade 2/6 systolic ejection murmur is appreciated at the left upper sternal border. When the child squats, the murmur is intensified and the cyanosis improves. What is the most appropriate next step in the management of this patient?
A. Diazepam
B. Morphine, oxygen, nitroglycerin, and aspirin
C. Morphine, oxygen, IV fluids, and beta blockers
D. Observation and reassurance
E. Antibiotics and supportive care
A 9-month-old male infant is brought to his pediatrician by his mother with lethargy and decreased oral intake for one day. His mother also mentions that he did not sleep well the previous night. A review of the medical record reveals several missed appointments and that the boy was born at 36 weeks gestation via spontaneous vaginal delivery. At the clinic, his temperature is 37.2ºC (99.0ºF), pulse rate is 140/minute, respirations are 44/minute, and blood pressure is 92/60 mm Hg. On physical exam the infant is awake but irritable and the rest of the physical is within normal limits for his age. On ophthalmologic examination, there are multiple retinal hemorrhages that extend to the periphery in both eyes. Which of the following investigations is most likely to be helpful in the management of the infant?
A. Hemoglobin electrophoresis
B. Peripheral blood smear
C. Noncontrast computed tomography of head
D. Lumbar puncture
E. Bone marrow aspiration
A 14-year-old boy is brought to the office for slight weakness when running or walking up the stairs. The weakness is occasionally associated with cramps and muscle pain. He also mentions having one episode of red-colored urine after a particularly difficult workout with his track team. His vital signs and physical examination are within normal limits. He has no significant past medical or family history. Laboratory studies show the following:
- CPK: 1864 U/L
- LDH: 421 U/L
- AST: 490 U/L
- ALT: 280 U/L
EEG, electromyography, and MRI show no abnormalities. Which of the following is most likely to be deficient in this patient?
A. GLUT-2
B. Glucose-6-phosphatase
C. Liver phosphorylase
D. Lysosomal acid maltase
E. Muscle phosphorylase
A 2-year-old girl presents to the emergency department with a 3-minute episode of a tonic-clonic seizure. The parents deny any previous history of seizure involving the patient or the family. Physical examination reveals an afebrile, well-groomed, and playful appearance, with normal vital signs. The patient carries a pink birthmark on the right side of her face extending from the forehead to the zygomatic arch. Which of the following findings is most likely on a head CT of this patient?
A. A non-enhancing hemispheric lesion
B. Intraparenchymal hemorrhage
C. Prominent intraparenchymal white matter calcification
D. Subependymal giant cell astrocytoma
E. Subependymal nodule
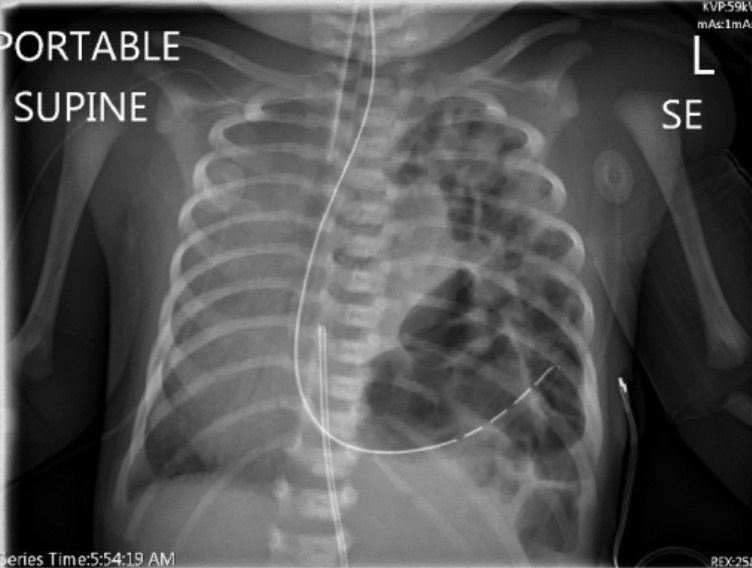
Twenty-four hours after delivery, a 2.4 kg (5.3 lb) newborn develops respiratory distress. She was born at 38 weeks gestation. Her pulse is 136/min, respiratory rate is 60/min, and blood pressure is 60/30 mm Hg. Examination shows a scaphoid abdomen. The heart sounds are heard in the right hemithorax, and the lung sounds are absent on the left side. The umbilical artery blood gas analysis on 60% oxygen shows:
| pH | 7.30 |
| pCO2 | 48 mm Hg |
| pO2 | 52 mmHg |
A nasogastric tube is inserted. A chest X-ray is shown. Which of the following is the most likely diagnosis?
A. Bochdalek hernia
B. Kartagener’s syndrome
C. Midgut volvulus
D. Pneumothorax
E. Situs inversus
A 10-year-old boy is brought to the office by his mother because of jerking movements of his arms for the past 6 months. These jerking movements are more frequent the morning after he stays up late playing video games. He also had 2 tonic-clonic seizures 5 months and 2 months ago. A physical examination shows no abnormalities, and there are no jerking movements during the examination. EEG shows a 4- to 6-Hz bilateral polyspike and slow-wave discharges with frontal predominance over a normal background activity. Which of the following drugs would be most appropriate for treating this patient?
A. Lamotrigine
B. Levetiracetam
C. Topiramate
D. Valproate
E. Zonisamide
A 2-month-old is brought to the physician for a well-child examination. She was born at 39 weeks gestation via spontaneous vaginal delivery and is exclusively breastfed. She weighed 3,400 g (7 lb 8 oz) at birth. At the physician’s office, she appears well. Her pulse is 136/min, respiratory rate is 41/min, and blood pressure is 82/45 mm Hg. She weighs 5,200 g (11 lb 8 oz) and measures 57.5 cm (22.6 in) in length. The remainder of the physical examination is normal. Which of the following developmental milestones has this patient most likely met?
A. Absence of asymmetric tonic neck reflex
B. Monosyllabic babble
C. Reaches for objects
D. Smiles in response to face
E. Stares at own hand
Do you want to practice more Pediatrics questions?
Create a free Lecturio account and you’ll have access to the Lecturio question bank with more than 1,200 USMLE Step 2 CK practice questions.