Estudia para el ENARM con Lecturio
Prepárate para el ENARM con las lecciones en video, preguntas de casos clínicos y las páginas de concepto de Lecturio.
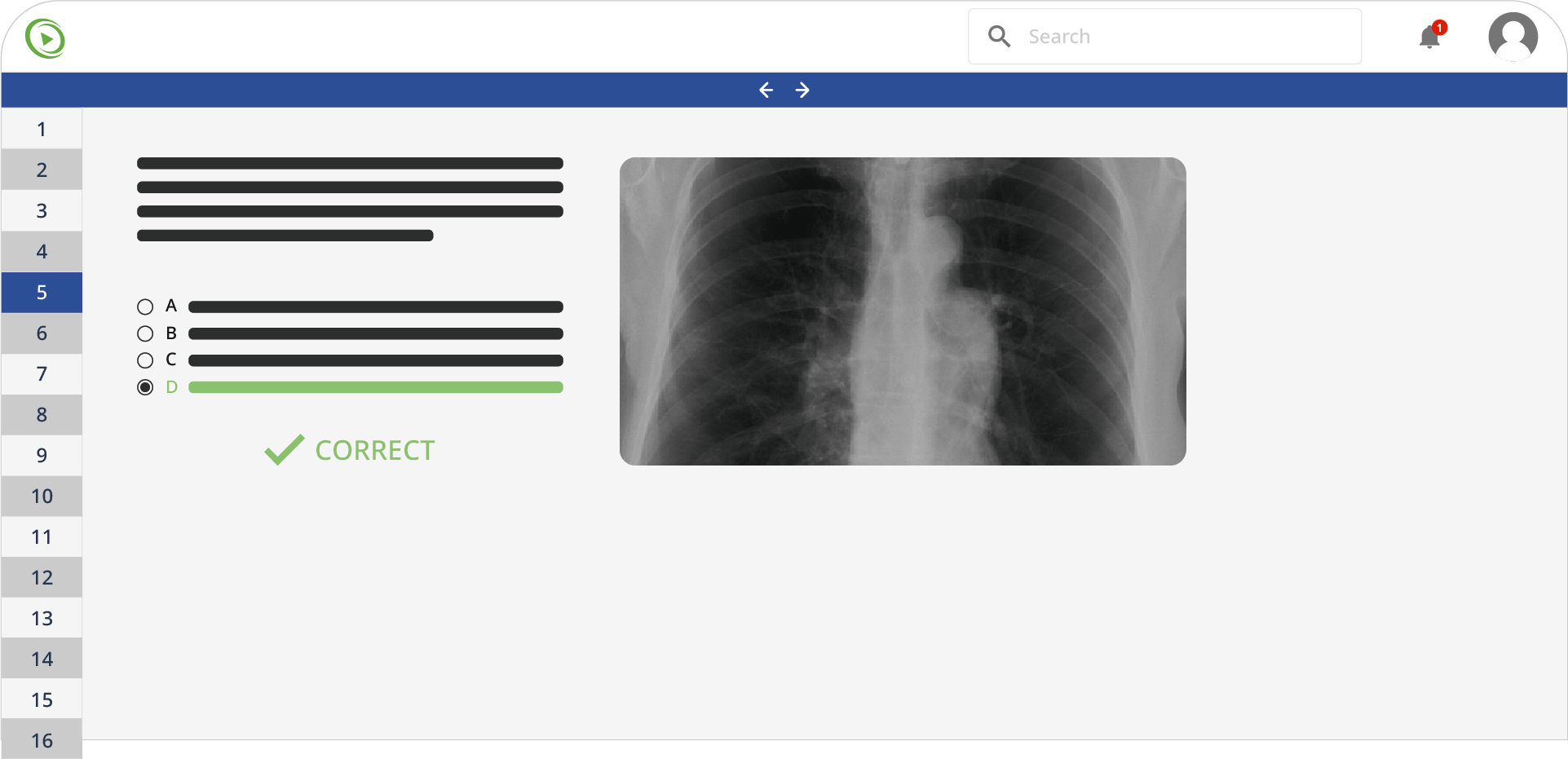
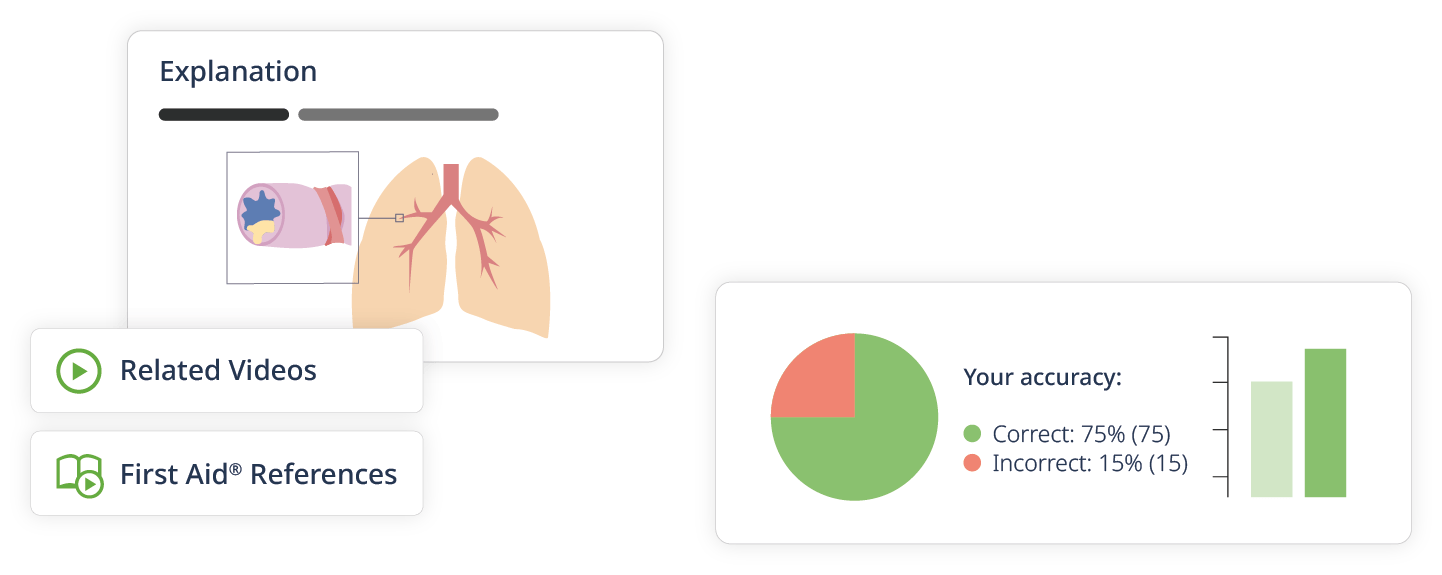


Banco de preguntas impulsado con inteligencia artificial (IA)
Tests de repetición espaciada
Lecciones en Video
Páginas de Concepto
El ENARM es el primer paso para ingresar al Sistema Nacional de Residencias Médicas (SNRM)
El objetivo del Examen Nacional para Aspirantes a Residencias Médicas (ENARM) es seleccionar a los médicos más preparados para realizar una residencia médica en México. Lecturio es una herramienta de estudio la cual ayuda a los estudiantes a prepararse y aprobar dominar el ENARM.
- El ENARM se compone de 280 preguntas, estructuradas en forma de casos clínicos que tienen de una a tres preguntas cada uno; con una sola opción correcta basada en la modalidad de la mejor respuesta y tres distractores. Es importante resaltar que 250 de las preguntas son en español y 30 en inglés.
- El ENARM dura 5 horas con dos turnos matutino y vespertino
- El examen se aplica en formato electrónico con una computadora para cada sustentante
- El ENARM explora las competencias cognitivas en casos clínicos enfocados en Salud Pública, Urgencias, Medicina Familiar y de las cuatro especialidades troncales Medicina Interna, Pediatría, Ginecología-Obstetricia y Cirugía General
- El examen ENARM se presenta cada año en el mes de septiembre en diferentes ciudades de México. Se ofertan alrededor de 8.000 plazas y cerca de 500 para extranjeros en cada convocatoria.
- Los y las sustentantes podrán elegir la especialidad de su interés posterior a la presentación del examen
Practica tu camino al éxito
Domina el ENARM con las potentes preguntas de Lecturio sobre casos clínicos y los tests de repetición espaciada elaborados por expertos.
- Más de 2,000 casos clínicos reales
- Videos y textos explicativos a detalle
- Asistencia del Tutor IA
- Ilustraciones de alta calidad
- Seguimiento del progreso con revisión adaptativa
Al integrar todas las funciones en tu práctica o recuperación, podrás experimentar la preparación de exámenes más eficiente posible y tener las herramientas adecuadas para el día del examen.







- 9,000 preguntas
- Plan de estudio personalizado
- Recordatorios automáticos para un aprendizaje óptimo
- Mayor retención de conocimientos
- Algoritmo adaptativo para repasos específicos
- Mejora de la eficiencia del aprendizaje
Retén la información más importante y mejora tu capacidad para recordar conceptos clave con la ayuda de un algoritmo adaptativo, que te dice exactamente lo que tienes que repetir y cuándo.
Aumentaron su confianza
en su preparación para presentar el ENARM
Prefirieron la flexibilidad y comodidad que ofrece la plataforma
en la preparación de exámenes
Recomendarían Lecturio a un amigo
Un gran número de estudiantes encuentra Lecturio como un recurso inteligente y confiable
Maximiza tu preparación para el ENARM
Con las lecciones en video y páginas de concepto con los temas más relevantes
- 220 horas de lecciones en video
- Preguntas de recuperación integradas
- Diapositivas descargables de alta calidad
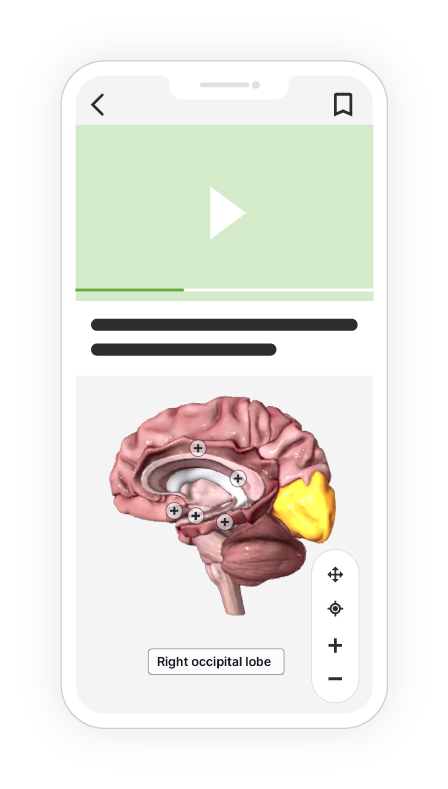
- Ilustraciones detalladas y modelos en 3D
- Resúmenes de apoyo para tu estudio
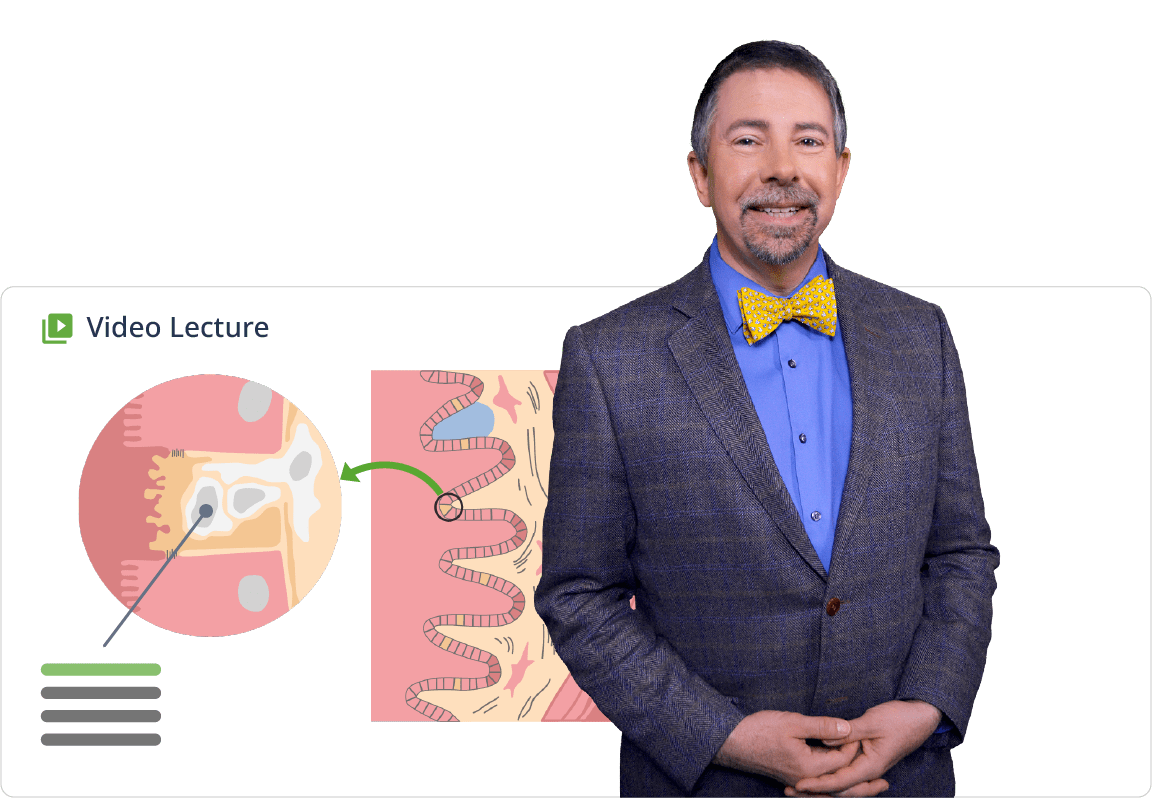
Lecturio se encarga de simplificar los complejos temas del ENARM mediante atractivas lecciones en vídeo impartidas por educadores expertos, quiénes ofrecen una amplia cobertura para una comprensión integral.






- Más de 1,450 páginas de conceptos detallados
- Videolecciones enlazadas y tests Qbank
- De alto rendimiento y actualizadas
- Imágenes, gráficos y tablas detallados
Domina nuevos conceptos médicos y refuerza tus conocimientos sobre temas difíciles utilizando nuestras completas Páginas de Conceptos, creadas y revisadas por médicos formados en EE. UU.

Accede hoy a Lecturio Medical Premium
Prueba gratis de 7 días
El recurso de estudio todo en uno para MD, DO, PA, NP y otros estudiantes de medicina clínica.
Preguntas y Respuesta
El ENARM es un examen nacional en México que evalúa los conocimientos y habilidades de los aspirantes a residencias médicas. Es un requisito para acceder a programas de especialización en instituciones de salud del país.
El ENARM está abierto a médicos mexicanos y extranjeros que deseen postularse para residencias médicas en México. Se requiere cumplir con los requisitos específicos establecidos por la convocatoria oficial.
El ENARM se lleva a cabo anualmente en fechas y sedes determinadas por la Comisión Interinstitucional para la Formación de Recursos Humanos para la Salud (CIFRHS) de México.
La convocatoria oficial con los requisitos se publica en abril y el examen se aplica cada año a finales de septiembre en varias sedes a lo largo de la República Mexicana.
El ENARM consta de una serie de preguntas de opción múltiple que evalúan el conocimiento práctico en las cuatro especialidades troncales Medicina Interna, Pediatría, Ginecología-Obstetricia y Cirugía General. El ENARM se presenta por turnos, matutino o vespertino, cada turno dura 5 horas.
El ENARM abarca una amplia gama de temas médicos relevantes para la práctica clínica y la especialización. Incluye áreas como diagnóstico, tratamiento, farmacología, procedimientos médicos, ética médica y otros aspectos esenciales para la atención de los pacientes.
Lecturio ofrece un enfoque integral y personalizado para la preparación del ENARM. Nuestro contenido de alta calidad, incluyendo lecciones en video, preguntas de práctica y materiales de estudio, está diseñado específicamente para ayudar a los estudiantes a adquirir los conocimientos necesarios para superar el examen. Además, Lecturio proporciona una plataforma en línea accesible y flexible, que permite a los estudiantes estudiar a su propio ritmo y de acuerdo con sus necesidades individuales. Nuestro enfoque en la comprensión profunda y el refuerzo constante garantiza que los estudiantes estén preparados de manera efectiva para enfrentar el desafío del ENARM.