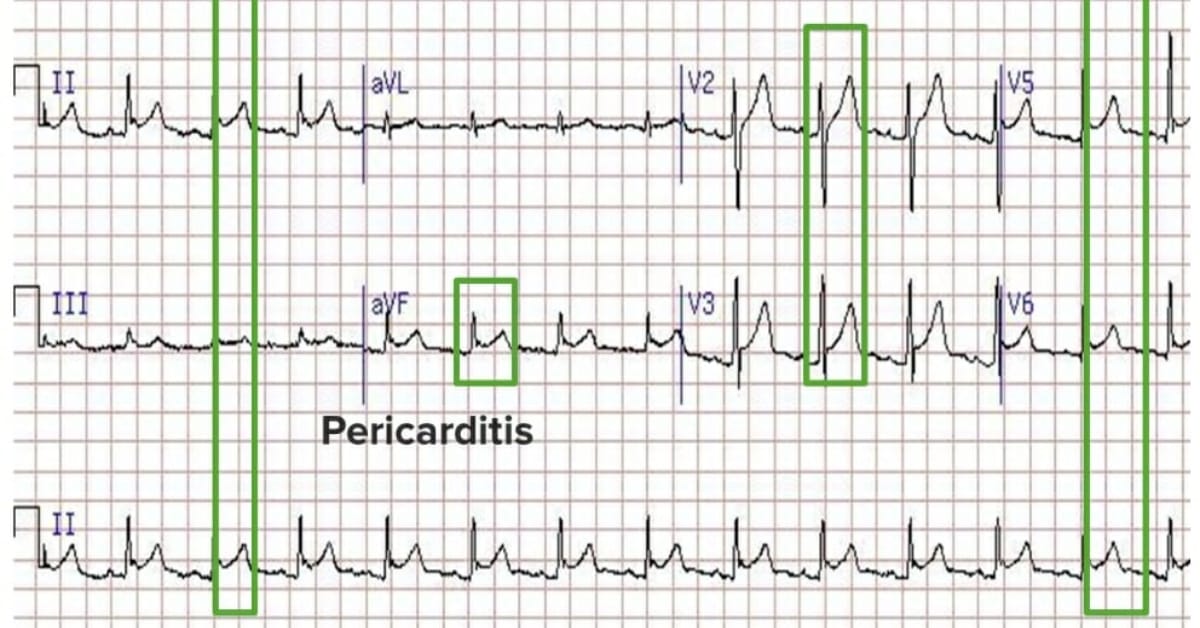
The most common locations for placing ECG leads are in the operating room or the emergency room. It’s important to know where to place them because in the ER, you have to be able to place them quickly and accurately. This can be difficult because the wires can tangle themselves and figuring out which color goes where can be confusing. While most machines come with a guide, it’s faster to just remember where the leads should go.
In this article, I’ll tell you about the indications for an ECG, outline where the leads should be placed, and offer a quick mnemonic to help you remember the lead placements. Before we get into that, let’s talk about the ECG itself!
Take the Course: Cardiology
Cover all cardiology essentials with the complete online class.
What Is an ECG?
Almost everyone’s seen an ECG once in their life. It’s the heart monitor you see with squiggly lines that go flat when someone dies in movies. But it’s more complicated than that. An ECG is a common diagnostic and monitoring device that tracks the electrical activity of the heart. The purpose of the leads is to measure this electrical activity at different angles of the heart.
So, what exactly does an ECG measure?
It measures the direction and magnitude of electrical activity in the heart. As you may know, the heart is a muscle that requires electrical conduction to contract. All these muscle contractions must be coordinated to pump blood properly through its 4 chambers and into the rest of the body. That’s what keeps the heart in a normal rhythm. However, if those contractions aren’t coordinated, an arrhythmia can occur, impeding proper blood flow. This can have fatal consequences.
What do the ECG results tell us?
You can view the squiggly lines from an ECG as patterns that reflect the electrical signals going through the heart. Each lead measures those signals from different walls of the heart. For example, if a heart wall is ischemic, the ECG should indicate the affected areas and, consequently, which coronary artery is occluded. Using the device, you should also be able to infer other cardiac problems like cardiac hypertrophy and arrhythmias.
When Will I Need to Attach an ECG?
Indications for an ECG
For a medical student, the answer is, “Whenever you’re told to do so.”
But of course, knowing the indications will help you anticipate the necessity of an ECG and to act more quickly and reliably. The main indication for using an ECG is based on a patient’s history and symptoms. Hook the patient to an ECG if:
- They present with dizziness, chest pain, syncope, seizure, or poisoning
- If the vital signs related to the heart like blood pressure and heart rate are abnormal
- If they need CPR
Patients with cardiac diseases like rheumatic heart disease, coronary heart disease, and congenital heart diseases, or other diseases like metabolic disorders, electrolyte imbalance, and blunt trauma to the chest should always have an ECG ordered. You will also need it for screening patients who have installed pacemakers, are athletes (for cardiomyopathy), or with hypertension. You’ll also be asked to hook up patients undergoing surgery to monitor their vital signs.
There are 3 main types of ECG:
- Resting ECG: This is the most common one you’ll find around the hospital. This is for when the patient is lying down comfortably and not moving.
- Stress/exercise ECG: This is used for treadmill stress tests to see if cardiac-related symptoms or abnormal ECG results arise from extraneous activities.
- Ambulatory ECG/Holter monitor: This is used to monitor a patient’s heart rhythm for a longer period of time. It’s basically a small ECG attached to a patient where it can monitor them at home, as the patient can go about their day.
When to NOT place an ECG?
What are the contraindications for an ECG? Since it’s a non-invasive procedure, there’s very little reason to not conduct an ECG unless the patient is allergic to the adhesive of the leads or the leads themselves. Of course, if the patient refuses to undergo an ECG procedure, you can’t proceed without their consent. So, make sure to inform your patients about the benefits of undergoing an ECG and the potential risks of not doing so.
How to Place ECG Leads
Different ECG machines require different placements, with some machines utilizing 3 or 5 leads. For this article, we’ll focus on the 12-lead resting ECG. Some ECG machines use an adhesive for the leads, while others use suction cups. Adhesive leads are a lot easier to place, but remember to always check if the patient is allergic to the adhesive. If so, you’ll have to look for another device.
The patient must be in a comfortable position when you place the leads. Have them lie down flat. Don’t forget to reassure the patient that this is a non-invasive procedure and they shouldn’t experience any discomfort throughout the whole process. If you’re using the suction cups for chest leads, they can feel a bit cold and there’s a minor pinching sensation. Apart from that, the patient shouldn’t be feeling anything.
If you end up with a device that uses suction cups, you might have trouble placing the leads because they can come loose with any slight movement. Before placing the leads, sterilize the patient’s chest with alcohol. For patients with chest hair, it may be harder to place the leads, and shaving the area may be necessary (with patient’s permission). Since the procedure is related to electric currents, make sure the patient removes any metallic accessories to avoid interference with or artifacts on the readings.
Before you start, explain to the patient what you will be doing. Make sure the area is private, because they’ll be baring their chest. Ask them for any allergies and any underlying cardiac conditions they may have. Finally, ask for their consent.
Placing the leads
Every ECG machine includes a guide on the device itself to help with proper placement. They’re even color-coded for your convenience. However, I highly recommend you don’t memorize based on colors, because there are two different color-coding standards for a 12-Lead ECG.
Instead, memorize where each bipolar and unipolar lead goes and just use the guide on the ECG to double check if your placement is correct. A normal 12-Lead ECG has 6 limb leads and 6 precordial leads. These are all organized into 10 wires. Each lead is labeled accordingly.
Personally, I always place the limb leads first because they’re the easiest to place. That’s because they’re all labeled according to their side and body part (RA – right arm, LA – left arm, RL – right leg, LL – left leg). These limb leads refer to the I, II, III, aVL, aVR, and aVF leads on the ECG result.
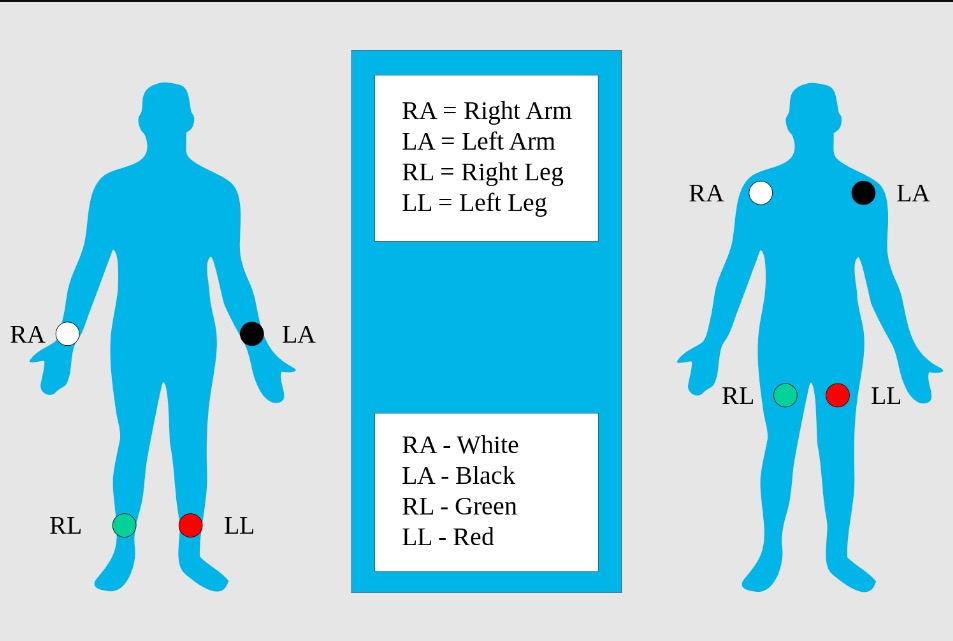
Limb electrodes: standard placement of the limb electrodes (left image) and modified placement (right image) for ECG
Image: “Limb leads, standard placement of the limb leads for electrocardiography” by MoodyGroove. License: Public DomainNext are the precordial leads. This is where medical students get stumped because they’re all simply labeled V1 to V6. What makes it more complicated is that they’re not meant to be placed in order. The location of V3 depends on where you placed the other leads. You’ll also have to palpate for the intercostal spaces (ICS), so learning how to palpate a patient’s ribs is crucial. For example, when I say 4th ICS, it means you have to palpate for the area below the 4th rib.
Also, remember that the V2–6 leads go on the left side, oriented towards the direction of the heart’s apex. Many students make the common mistake of placing the leads in reverse!
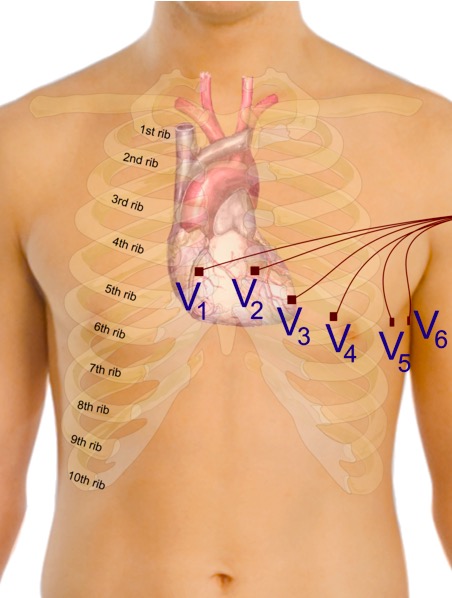
Proper placement of the precordial electrodes for ECG
Image: “Precordial leads in ECG” by Mikael Häggström. License: CC0 1.0Here is the recommended order for placing the leads:
- Place V1 and V2 on the RIGHT and LEFT margins of the sternum, respectively. This is the edge of the hard part (the sternum bone) in the middle of the chest. They should be on the same level at the 4th intercostal space (ICS).
- Skip V3 for now. Place V4 at the 5th ICS at the left midclavicular line. This is aligned with the middle of the left collarbone.
- Place V5 at the 5th ICS at the anterior axillary line. This is defined as the imaginary line down your frontmost armpit fold (anterior axillary fold).
- Place V6 at the 5th ICS at the midaxillary line. This is the imaginary line that follows down the middle of your armpit. Note that the ribs move in a curved line, so V5 and V6 will be a bit higher than V4. Just trace the ribs properly and you’ll get the correct area.
- Lastly, place V3 in the middle of V2 and V4.
How to remember ECG lead placement: mnemonics
While I don’t have a mnemonic for ECG placement per se, I do have associated ideas that help me associate the lead numbers with where they’re supposed to be placed:
- V3 comes later, so put that aside.
- V1 and V2 are one group at the 4th ICS. V4–6 are another group at the 5th ICS. Keep them in their separate groups so they don’t get tangled.
- V1 and V2 go first so they go on either side of the middle of the chest.
- Remember that V4–6 are located down and left because that’s where the apex of the heart is pointing.
- V4 is placed around one fourth (¼) of the way from the left of the chest.
- V6 is placed down the armpit because “armpit” has 6 letters.
- Then, just place V3 and V5 in the middle of their neighboring numbers, where they belong.
For the limb leads, this mnemonic is a lot easier, but it only works for ECGs that follow the American Heart Association (AHA) color system:
- Right-side: Snow over grass (white lead (RA) above the green lead (RL))
- Remember that white is on the right!
- Left-side: Smoke over fire (black lead (LA) above the red lead (LL))
Apart from these memorization techniques, you can always come up with your own. Regardless, I hope this guide helped because I fumbled a lot when I was an intern in the hospital when I would try to place the leads properly. But after a lot of practice and memorization, I’m now able to do it just by referencing the lead labels. So practice and take every opportunity to use the ECG machine when you can!