Playlist
Show Playlist
Hide Playlist
Subarachnoid Hemorrhage (SAH): Diagnosis
-
Emergency Medicine Bord Intracranial Hemorrhage.pdf
-
Download Lecture Overview
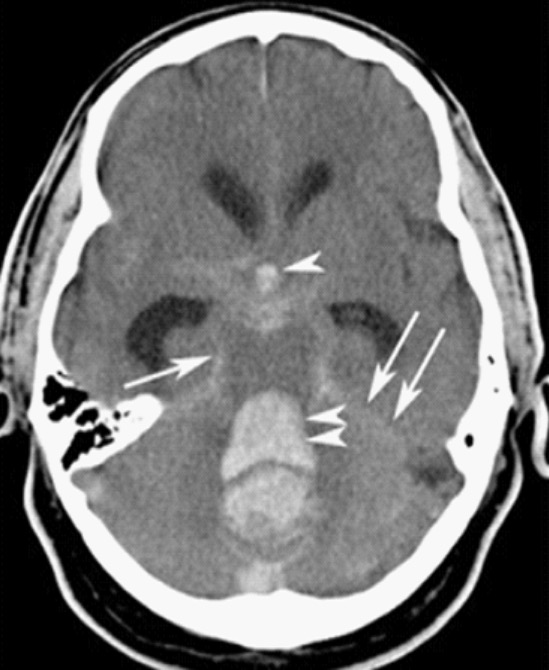
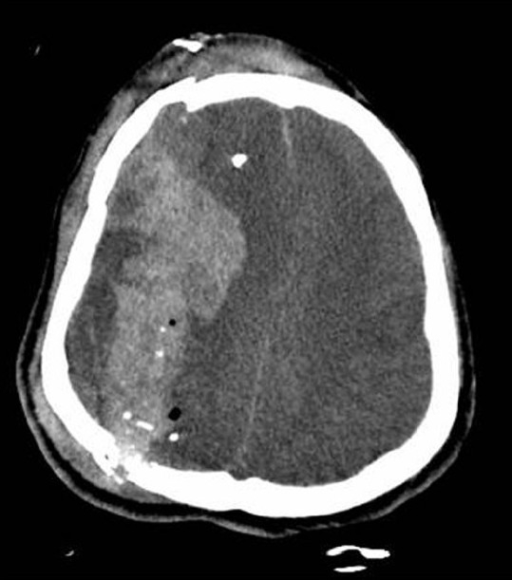
00:01 How do we diagnose subarachnoid hemorrhage? A non-contrast head CT is the first test that you wanna get. 00:09 Non-contrast head CT is better the sooner you get it after the headache starts. 00:15 If you get a non-contrast head CT within the first 6 hours in a 64 slice CT scanner in one of the newer generation CT scan machines, the sensitivity and specificity approaches almost 100% for subarachnoid hemorrhage so it’s really a great test to get. 00:33 Within the first 24 hours actually, it’s still pretty good, it’s about 90% but as the time goes on and as the time ticks away, the sensitivity and specificity does go down significantly. 00:47 So you wanna make sure that if someone presents with these symptoms and you’re worried, get that CT as quickly as you possibly can because as time goes by, you don’t want them waiting for that test to get less and less good. 00:59 So let’s say you have a patient and your patient presents with classic symptoms for subarachnoid hemorrhage, and you very astutely go and you get them that non-contrast head CT very early on or within the timeframe that they present to the Emergency Department and that scan is negative, are you done? Unfortunately, the answer there is no. 01:21 So if the head CT is negative, the patient still needs additional testing in order to 100% rule out subarachnoid hemorrhage. 01:28 The reason that this is one of those diagnosis in Emergency Medicine that we like to get as close to 100% to rule it out as possible, is because it has such a high morbidity and mortality associated with it. 01:39 So this isn’t something where you wanna be like, “We’re pretty sure you don’t have it, you can go home.” We wanna be as close to 100% as we possibly can be. 01:47 So we look at our gold standard test for subarachnoid hemorrhage, and the gold standard here is lumbar puncture. 01:54 And when you do your lumbar puncture, what it looks for is it looks for the cell count and it looks for Xanthochromia. 01:59 When you’re doing the lumbar puncture, you generally send a cell count on tube one and tube four, you’re generally getting four tubes of cerebrospinal fluid when you do that test. 02:10 And the reason that we do it on two tubes, that we do it on tube one and tube four, is because sometimes what can happen is you can have what’s called a traumatic tap, and what that is, is when you’re gonna do your lumbar puncture, you hit a small blood vessel, and you get a little bit of blood in your sample. 02:25 So by sending it on tube one and tube four, ideally what would happen is that the blood would be greater in tube one if it is was a traumatic tap and then decrease in tube four. 02:36 So you’re looking at the trend between those two tubes because tube one you get in the beginning, so tube one is the first CSF that comes out, and tube four is the last CSF that you’re collecting. 02:46 Xanthochromia is a slight yellow discoloration of the cerebrospinal fluid, and the reason that that develops is because there are red blood cells in the CSF and as those red blood cells degrade, they can turn a yellow color. 03:01 Now, that’s something that the lab test is for, but it’s not a fancy test. 03:04 For the most part, what people do is they take the CSF and they hold the tube of cerebrospinal fluid up and they put a white piece of paper behind and if that fluid looks to be a little bit yellow, that is positive for Xanthochromia, and that’s looking for those broken down red blood cells. 03:21 Now, a lumbar puncture is definitely a somewhat invasive test but I always, especially in patients who are very concerned that they could have a subarachnoid hemorrhage, I always explain to them that this is the best test. 03:34 As of right now, this is the gold standard where we can most definitively figure out whether or not this is a subarachnoid hemorrhage. 03:42 There are other options, and a CT angiography which is a CT scan of the brain that looks at the blood vessels has actually a relatively good sensitivity and specificity as well, and eventually these might change and a CT angiography may actually become the gold standard for looking at this. 04:01 The advantage of the CT angiography is that that can detect or show you where there is an aneurysm, if it’s in fact present. 04:08 So that’s an advantage of getting the CT angiography whereas your lumbar puncture doesn’t give you that information. 04:14 So CT angiography is the test that can be done and it’s a CT scan with IV contrast that can help give you more information. 04:22 So it’s another option that we have for evaluating these patients and it’s potentially something that may replace lumbar puncture as the gold standard.
About the Lecture
The lecture Subarachnoid Hemorrhage (SAH): Diagnosis by Sharon Bord, MD is from the course Neurologic and Psychiatric Emergencies.
Included Quiz Questions
Which of the following statements regarding the early evaluation of subarachnoid hemorrhage (SAH) is FALSE?
- A negative non-contrast CT rules out SAH.
- Non-contrast CT scan has a very high sensitivity and specificity.
- Lumbar puncture is indicated with strong suspicion of SAH and a normal CT scan.
- Cerebral spinal fluid is collected in 4 tubes.
- CT angiography is also a reasonable option for diagnosing SAH.
What is the additional advantage of CT angiography over non-contrast CT or lumbar puncture in the diagnosis of subarachnoid hemorrhage?
- It may point out the etiology.
- It is less invasive.
- It is easier to perform.
- It has fewer side effects.
- It is less expensive.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |