Playlist
Show Playlist
Hide Playlist
Intracranial Hemorrhage and Trauma
-
Slides Intracranial Hemorrhage.pdf
-
Download Lecture Overview
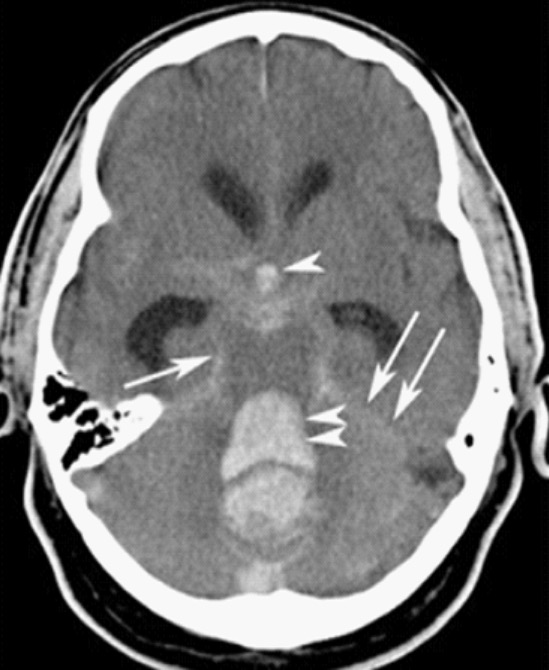
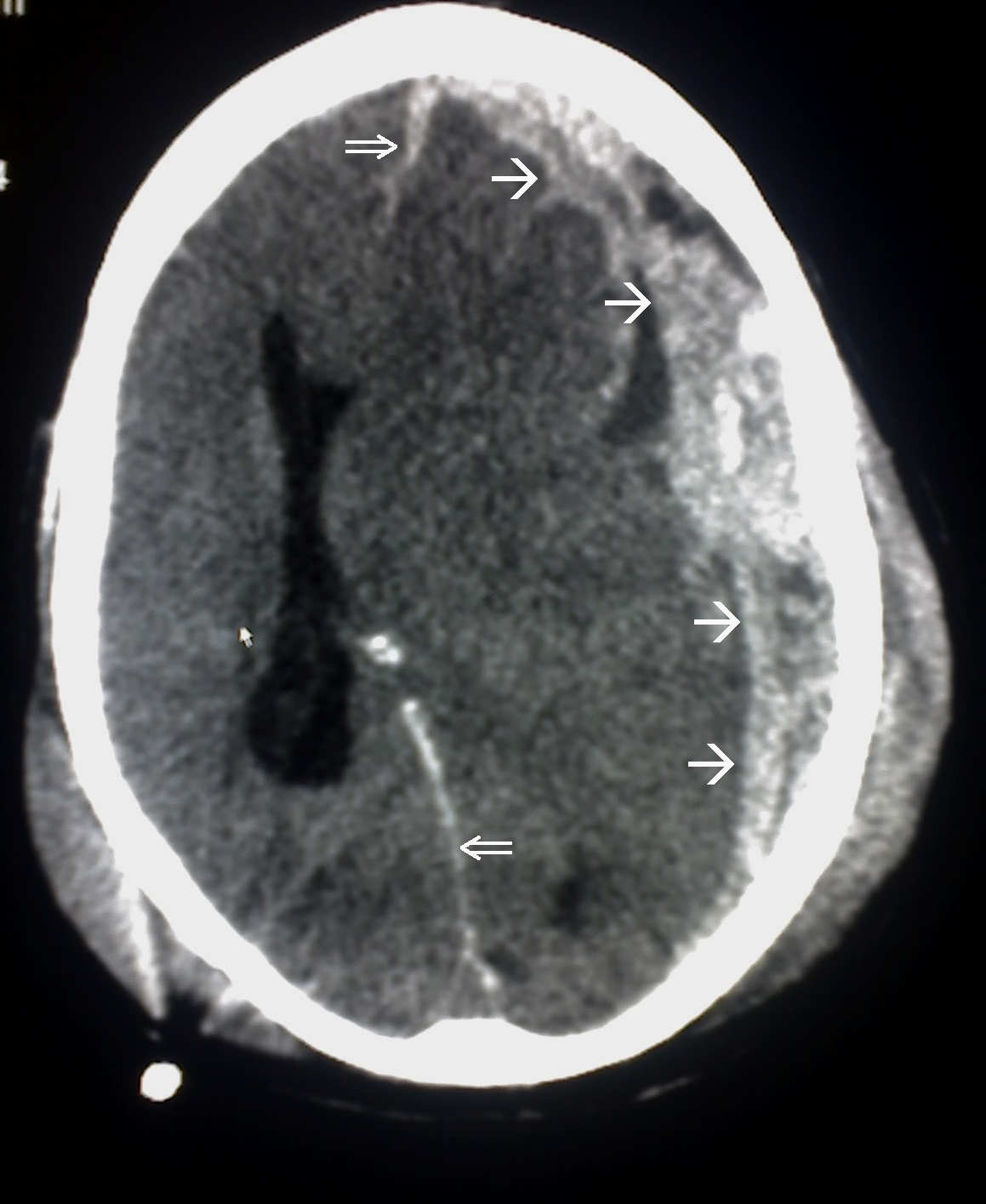
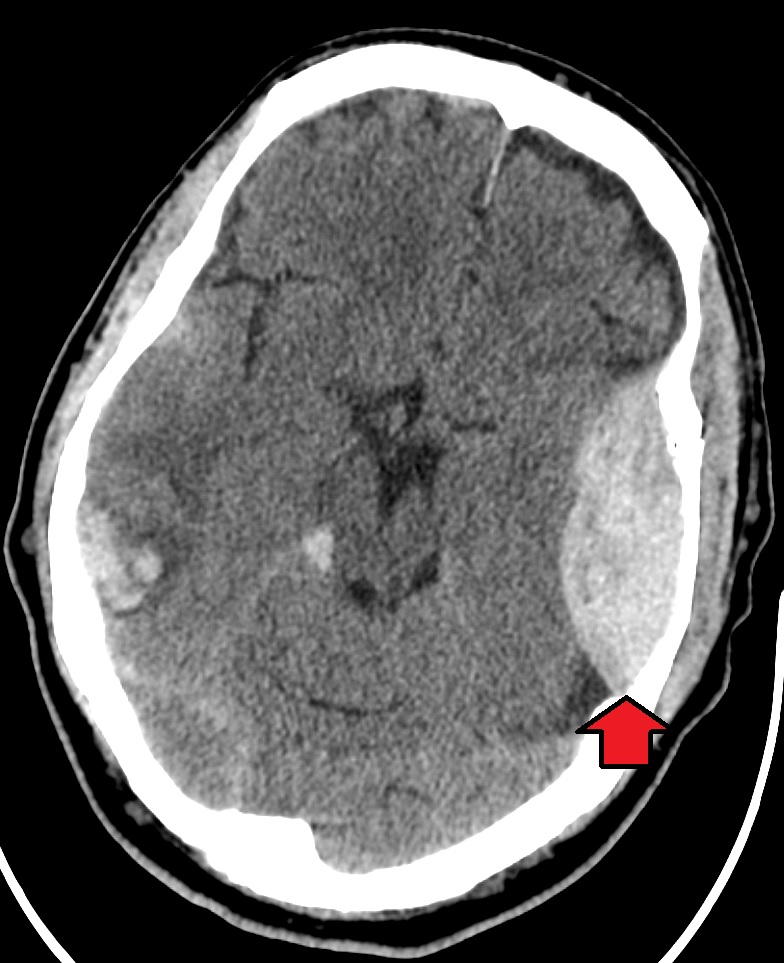
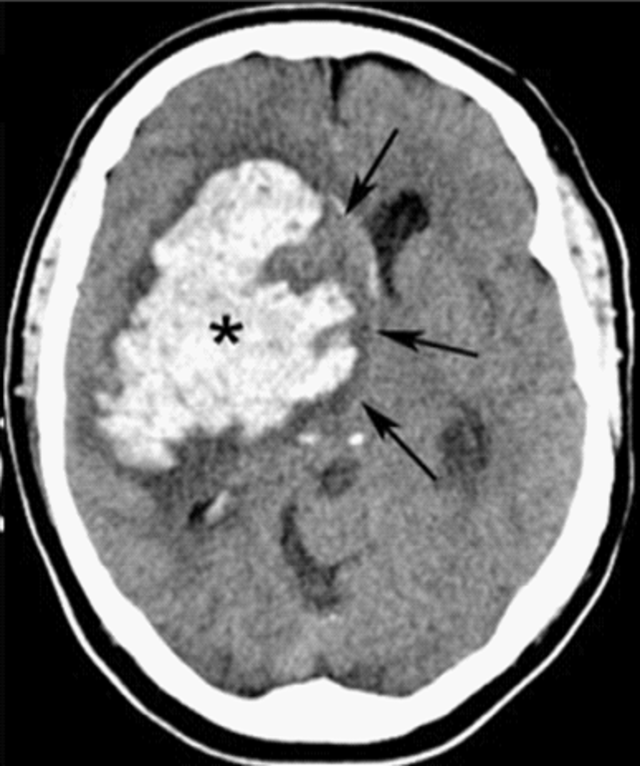
00:01 So in this lecture we'll be discussing intracranial hemorrhage and traumatic injury to the brain. 00:06 Let's start off by reviewing some normal brain anatomy. 00:10 Here we have an axial CT scan through the head and you can see the 2 temporal lobes here. 00:18 We have the pons, which is a portion of the brain stem back here and then we have the cerebellum seen most posteriorly and inferiorly within the brain. 00:28 We have the frontal lobes anteriorly and then we have the 2 sylvian fissures. 00:32 Posteriorly, we see a portion of the fourth ventricle and then the center we see the suprasellar cistern. 00:41 These are the frontal horns of the lateral ventricles and then adjacent to them we see the caudate nucleus. 00:48 This is the sagittal MRI scan which shows us the corpus callosum, the pons which is part of the brain stem, the cerebellum seen posteriorly and inferiorly, and the medulla, again, part of the brain stem. 01:04 So this is an axial T2 image of the brain. 01:07 You can see here anteriorly are the frontal lobes and we have the sylvian fissures. 01:11 Just behind the sylvian fissures are the temporal lobes and then posteriorly are the 2 occipital lobes. 01:19 Here we have the occipital horns of the lateral ventricles. 01:22 On this axial T2 weighted image, we have the frontal horns of the lateral ventricles and then again the occipital lobes posteriorly. 01:29 So MRI is usually the most sensitive examination at detecting brain abnormalities. 01:36 However, because MRI does take a long time being required, CT is usually used as the first line of diagnosis. 01:43 It's very easy to obtain and it's quick and it does have a relatively high sensitivity in detecting hemorrhage and mass effect. 01:49 We always start off with a non-contrast CT of the head. 01:53 If we administer contrast, contrast can be mistaken for hemorrhage so a non-contrast CT of the head is really the first line of imaging to look for hemorrhage. 02:02 There are 4 major types of hemorrhage. 02:05 There's epidural, subdural, subarachnoid, and intracerebral. 02:10 So let's take a look at each of these a little bit further. 02:13 This is the diagram that helps you differentiate how each one should look. 02:17 So we have an epidural hematoma here, which is located outside of the dura. 02:22 We have a subdural hematoma which is located just beneath the dura, so you see a dural line right here, and we have an intracerebral hematoma here which is within the brain parenchyma. 02:34 This is an example of a cause of a subarachnoid hemorrhage. 02:37 You can have a small aneurysm here that can cause a subarachnoid hemorrhage which can fill the sulci. 02:43 So an epidural hematoma is a hemorrhage that's located between the dura and the skull. It's usually caused by an injury to the middle meningeal artery, it can be caused by trauma, and it can be caused by skull fractures that often result in an injury to the middle meningeal artery. 03:01 Much less commonly so less than about 10% of the cases are caused by an injury to the middle meningeal vein. 03:07 So epidural hematomas present as a high density, extra axial lens-shaped collection. 03:12 It cannot cross suture line because the dura is connected to the skull at the sutures, however, it can cross the midline. 03:19 So subdural hematoma is hemorrhage that is located between the dura and to the brain. This is commonly caused by an injury to the bridging veins that go from the cerebral cortex to the venous sinuses and it is often related to trauma but it's not often associated with skull fractures. 03:35 This is an example of a subdural hematoma, it's a high density, crescent shaped collection and this can actually cross suture lines but this cannot cross the midline which different from an epidural hematoma which is able to cross midline but is not able to cross the suture lines. 03:51 So as subdural hematomas become subacute, they may develop a fluid-fluid level and they become hypodense overtime. 03:58 So this is a comparison of a subdural and an epidural hematoma. 04:02 In a subdural hematoma, the dura is attached to the skull and the blood is underneath the dura, so between the dura and the brain. 04:10 In an epidural hematoma, the dura is peeled off of the skull and the hemorrhage is between the skull and the dura and it's usually caused by a fracture. 04:19 Subdural hematomas predominantly consist of venous blood while epidural hematomas consist of arterial blood and a subdural hematoma is usually caused by a rupture of the bridging vein while an epidural hematoma is usually caused by rupture of a middle meningeal artery. 04:35 Let's take a look at this case here. 04:37 Which type of hemorrhage do you think this is? So this is a high density, biconvex collection in the temporal-parietal region right here. 04:53 You have adjacent soft tissue swelling and there's an adjacent skull fracture which was later found, it's not visible on this images, so this is an example of an epidural hematoma. 05:06 This is an example of a subdural hematoma. 05:09 We have an acute subdural hematoma along the right convexity. 05:13 It presents as a high density, crescentic collection. 05:16 This is an example of a chronic subdural hematoma that presents as a low density crescentic collection along the right hemisphere. 05:25 In this case, you can see that there's persistent mass effect. 05:28 So if you take a look at the midline, the midline is still shifted to the left, slowly this will resolve. 05:34 So subarachnoid hemorrhage is a high density fluid between the pia and the arachnoid space. You can see blood within the sulci and within the basal cisterns and common causes include trauma, ruptured aneurysm, or an AV malformation. 05:49 Usually patients present with what's called a thunderclap headache, it's kind of like getting hit on the head with a hammer and then patients often complain of it being the worst headache of their life. 05:59 So let's take a look at these 3 CT axial images. 06:02 So can you see the abnormality here? You can actually see blood within the basal cisterns and within the sylvian fissures. 06:17 Here we have an example of blood within the fissures. 06:20 You can see blood within the sulci and you can also see blood within the falx. 06:28 This subarachnoid hemorrhage was caused by ruptured aneurysm. 06:32 Let's take a look at this image. 06:35 So what kind of hemorrhage is this? How would you characterize this? So this is an example of an intracerebral hematoma. 06:49 You have hemorrhage within the brain parenchyma here and the hemorrhage is extended into the ventricular system which can often happen with an intracerebral hematoma. 06:59 This is commonly caused by trauma, aneurysm rupture, amyloidosis, or hypertension. There are many, many, other causes but these are some of the more common ones. 07:10 Intracerebral hematomas present as small areas of high density with surrounding edema. The edema, as we've talked about, appears hypodense. 07:20 It can also cause blood to enter the ventricular system and it may displace or compress the surrounding structures because of mass effect from the collection. 07:29 These can also result in herniation. 07:31 This is another example an intracerebral hematoma. 07:35 As you can see here, there are areas of high density within the brain parenchyma with a surrounding area of low density representing edema.
About the Lecture
The lecture Intracranial Hemorrhage and Trauma by Hetal Verma, MD is from the course Neuroradiology.
Included Quiz Questions
Which is NOT true of a subarachnoid hemorrhage?
- It is caused by rupture of the middle meningeal artery.
- Patients often present with the worst headache of their life.
- It appears on imaging as a high density between the pia and the arachnoid space.
- It can be caused by a ruptured aneurysm.
- There is blood is seen within the sulci.
A patient presents to the emergency department with the worst headache of his life and rates it as 10/10 intensity. What is the next best step in the management of this patient?
- Non-contrast CT scan of the head
- Contrast CT scan of the head
- Non-contrast MRI of the brain
- Contrast MRI of the brain
- Ultrasound of brain
What is TRUE regarding subdural hematoma?
- It is crescent-shaped on CT imaging.
- It crosses the midline.
- It cannot cross the suture line.
- It lies between the dura and the skull.
- It is commonly caused by injury to the bridging arteries.
With a subarachnoid hematoma, blood can be seen within which of the following structures?
- Sylvian fissure
- Fourth ventricle
- Caudate lobes
- Cerebral aqueduct
- Spinal canal
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |