Playlist
Show Playlist
Hide Playlist
Hypersensitivity: Types
-
Slides Hypersensitivity Introduction and Types.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
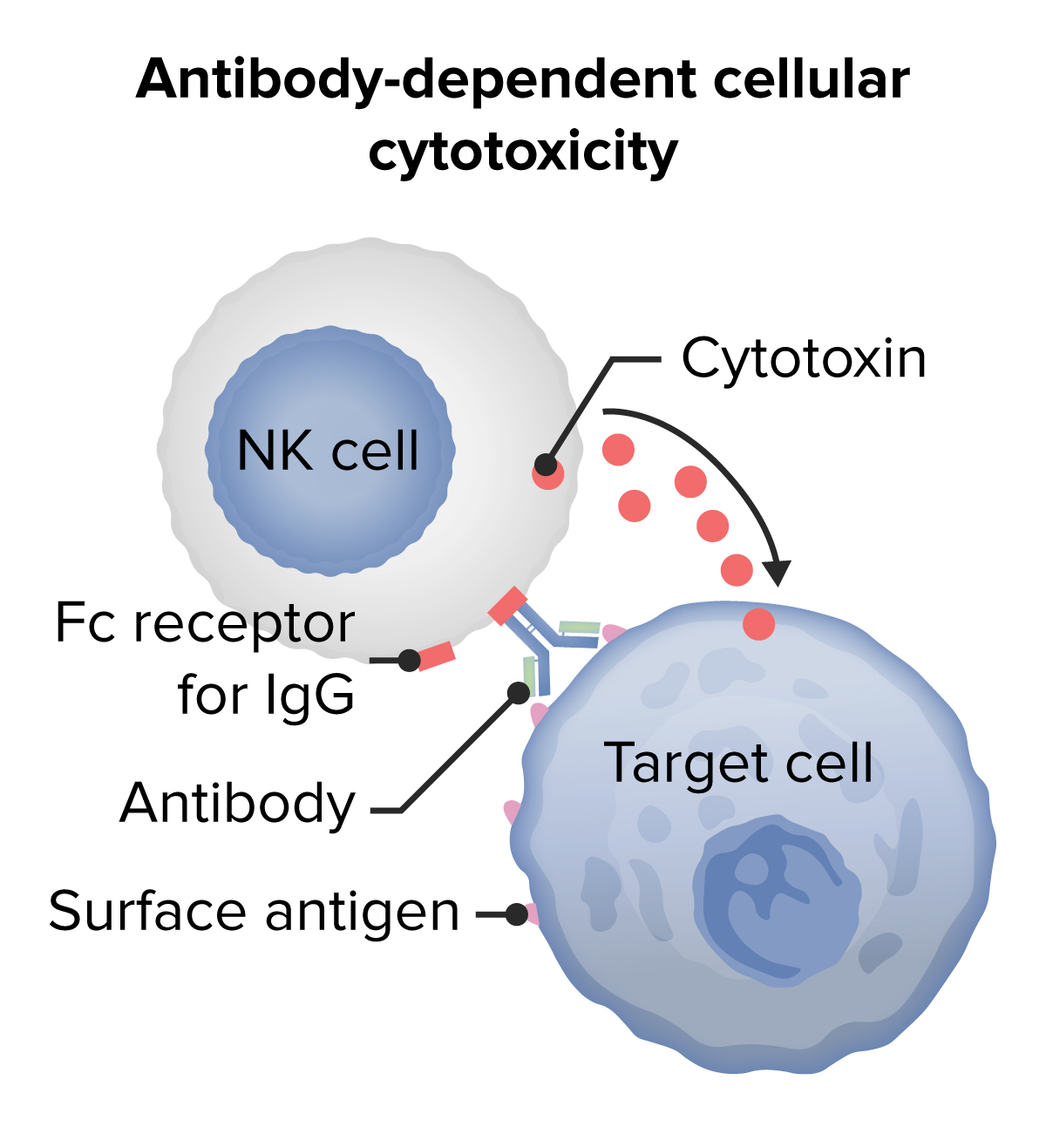
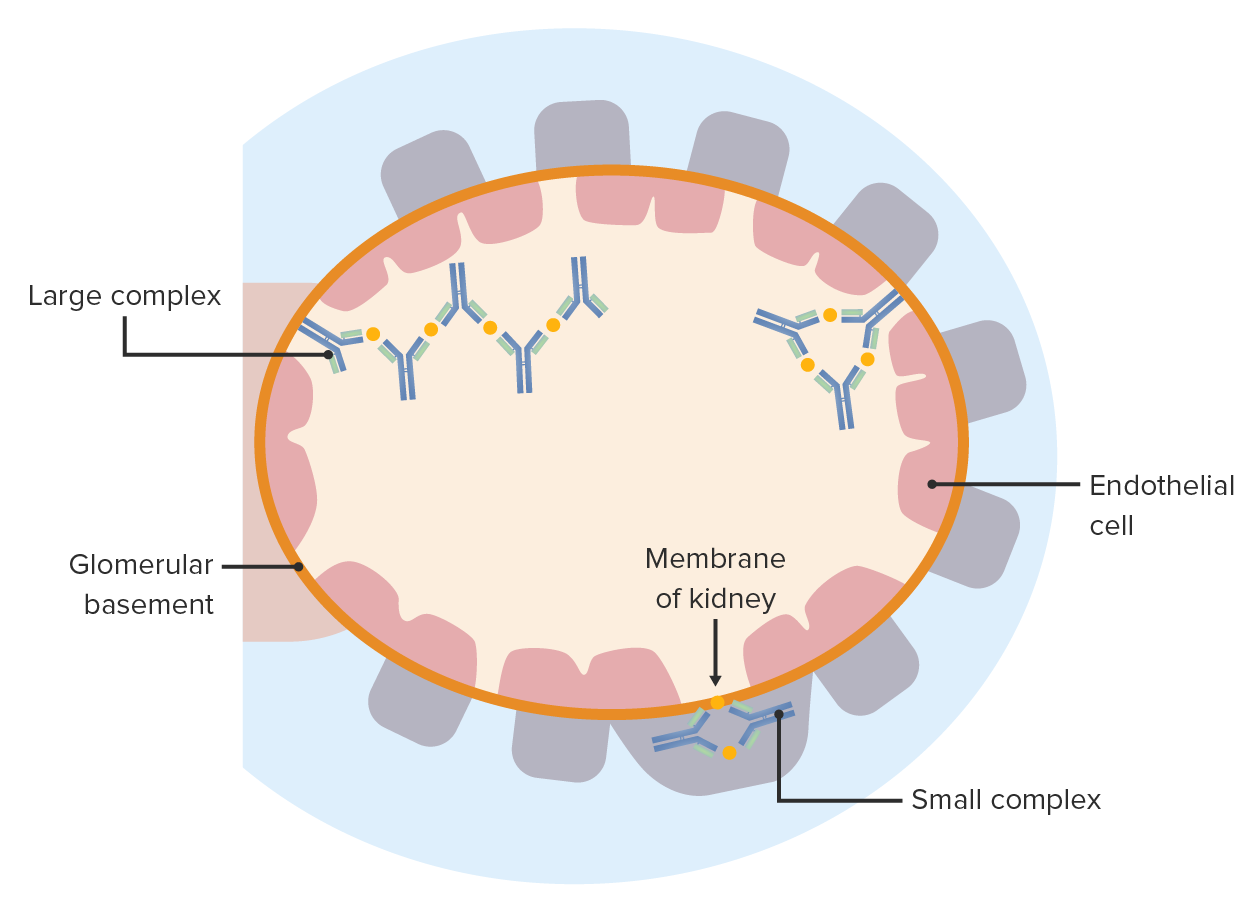
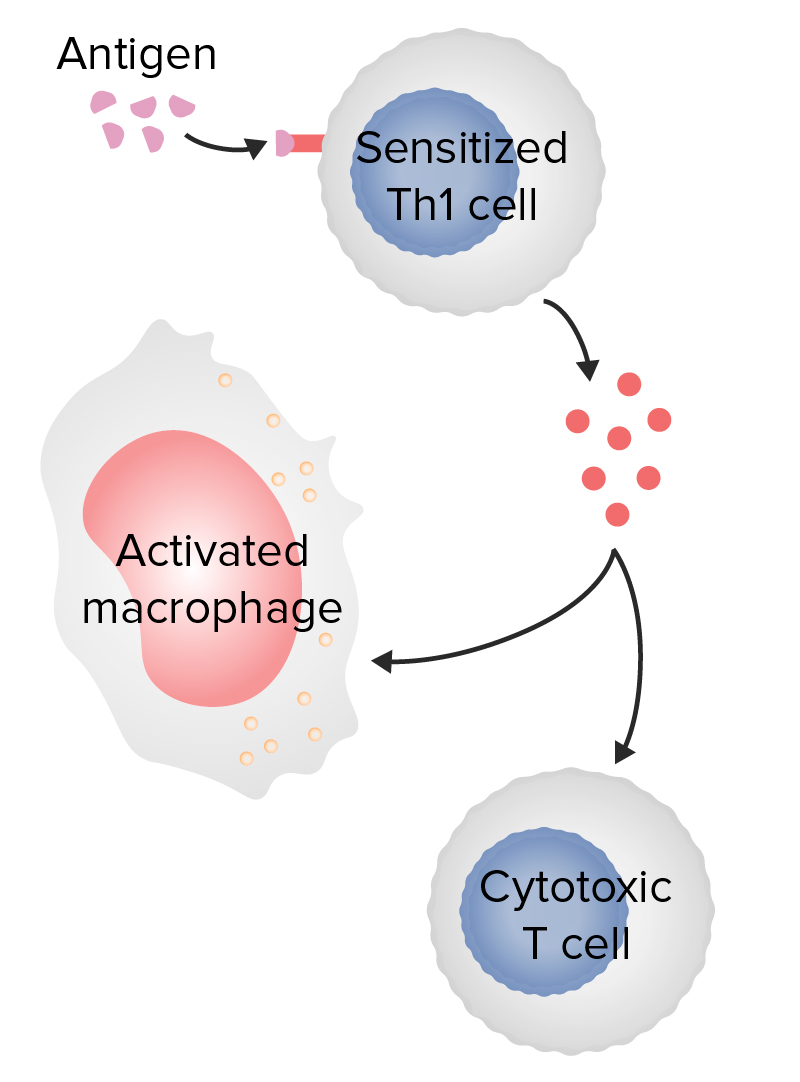
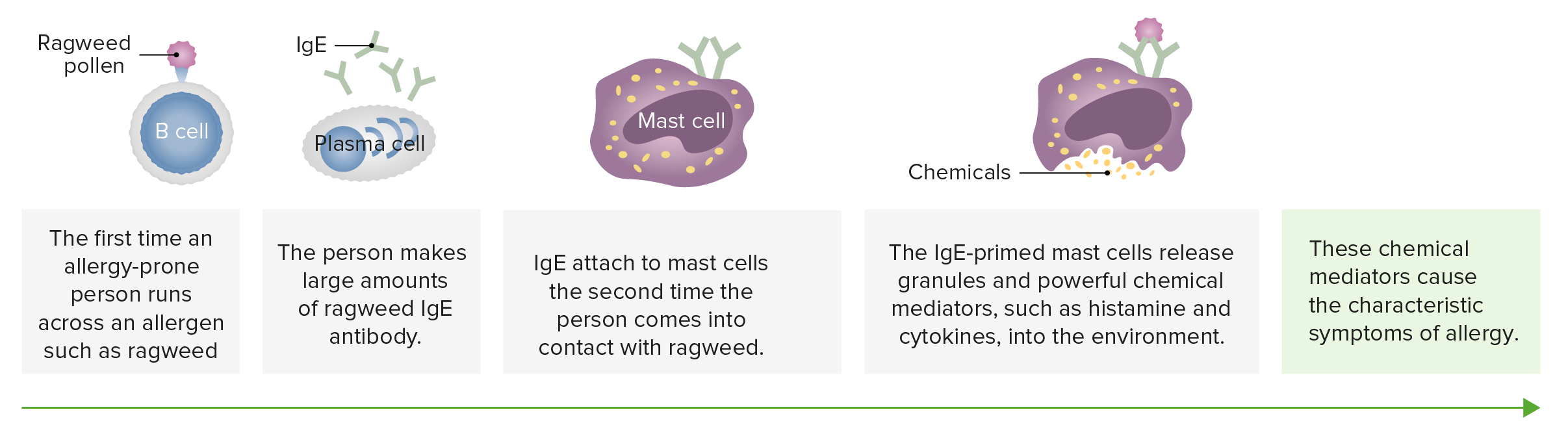
00:01 So we’re going to look at each of these four different types, and I’ll explain to you exactly what’s involved in these different types of hypersensitivity reaction. 00:11 So Type I - IgE mediated mast cell degranulation. 00:16 So here we have a mast cell, and on the surface of mast cells are Fc receptors that are specific for the IgE class of antibody. 00:26 This is in fact the high affinity IgE receptor that’s called FcεR1. 00:34 So this will bind IgE antibodies by the Fc region of the antibody. 00:39 That’s why it’s called an Fc receptor. 00:42 And we all have mast cells sitting in our tissues that have IgE on their cell surface. 00:48 And it doesn’t cause any problems at all. 00:50 The problem arises, is if an antigen comes in which the IgE is specific for, and that antigen binds to the IgE. 01:02 Because what happens then, is that the IgE antibodies on the surface of the mast cell get linked together; we use the term cross-linked. 01:10 And if this substance is a completely innocuous substance, for example grass pollen, we refer to it as an allergen. 01:19 It’s going to generate allergy. 01:24 And the consequence of the IgE antibodies being linked together by the allergen is that the mast cells release their granules, they degranulate. 01:42 Type II hypersensitivity is cytotoxic antibodies against cell surface antigen. 01:50 So here we have a cell surface, with some antigens present on the cell surface, and antibodies are bound to those antigens. 01:59 Sometimes the antibodies can be directly toxic to the cell. 02:05 However, in most cases, other components of the immune response are required in order for these antibodies to actually damage the cell. 02:15 So for example, the classical pathway of complement may become activated, leading to the production of the membrane attack complex. 02:25 Or killer cells, that is any cell that is able to participate in ADCC. 02:32 So this term K-cell is used as a generic description of cells able to participate in ADCC. 02:40 There’s only two things you need from a cell to do that. 02:43 You need it to have an Fc receptor, and you need it to be able to produce toxic molecules. 02:50 Or macrophages that again have Fc receptors on their surface and are able to attack the coated cell. 03:07 Type III hypersensitivity is immune complex mediated hypersensitivity. 03:12 Now, all that term means, immune complex, is simply an antibody bound to an antigen, and you know that’s what antibodies do isn’t it? They bind to antigens. 03:21 But in this situation, there is a binding to an inappropriate antigen or immune complexes are becoming trapped in small tissue spaces in the body and causing pathology. 03:33 So for example, macrophages can become activated, complement can become activated. 03:40 There will be recruitment of neutrophils if complement component C5a is generated, because that’s a very potent chemotactic factor for neutrophils, and pathology will ensue. 03:53 And then finally, Type IV hypersensitivity, delayed type hypersensitivity. 03:58 It’s called delayed type hypersensitivity because it takes a little while to get going. 04:02 The other three types, you can have antibody that's already present, and as soon as the antigen comes into the body, the response will happen immediately. 04:10 For T-cells, you need them to expand up in number, to proliferate, to differentiate, and to start secreting cytokines. 04:18 So typically, type IV hypersensitivity takes two or three days before you actually see any effects. 04:26 And there is recognition of peptide MHC Class II by the T-cell receptor on a T-cell that is going to mediate this hypersensitivity reaction, most commonly by producing excessive amounts of cytokines.
About the Lecture
The lecture Hypersensitivity: Types by Peter Delves, PhD is from the course Hypersensitivity and Autoimmune Disease. It contains the following chapters:
- Hypersensitivity - Type I
- Hypersensitivity – Type II
- Hypersensitivity – Type III
- Hypersensitivity – Type IV
Included Quiz Questions
Which of the following types of hypersensitivity reaction is often referred to as delayed type hypersensitivity reaction?
- Type IV
- Type I
- Type II
- Type III
- Type V
Which receptor binds to immunoglobulin E and mediates mast cell degranulation in type I hypersensitivity reactions?
- Fc epsilon RI (FcεRI)
- Peptide-major histocompatibility complex class II (pMHCII)
- T-cell antigen receptors
- Cluster of differentiation 5a
- Complement receptor
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Hypersentivity types I choose that rating because the lecture is nice basing on the slides, it is well explained