Playlist
Show Playlist
Hide Playlist
Cervical Cancer (HPV)
-
Slides CervicalCancer PathologyInfectionsNeoplasmsandScreening.pdf
-
Download Lecture Overview
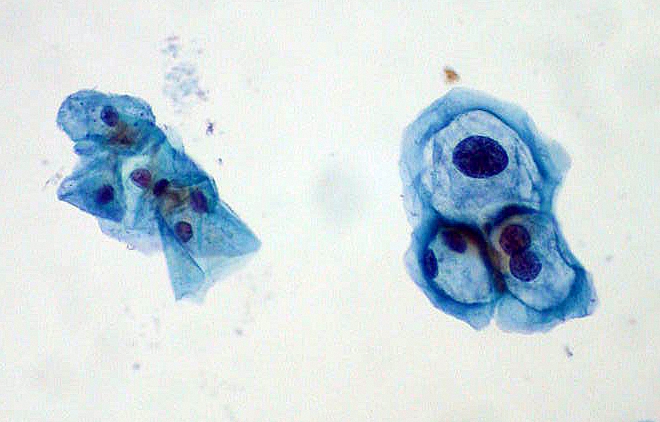
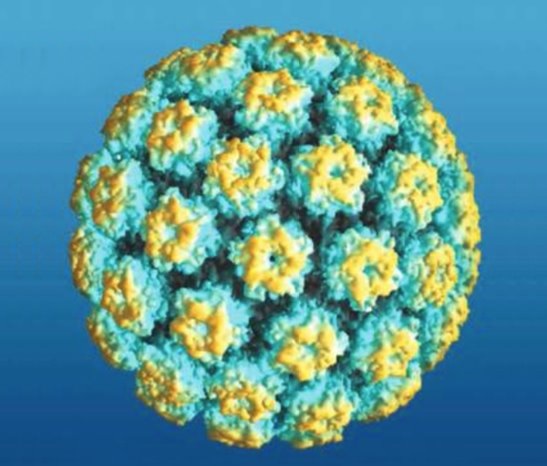
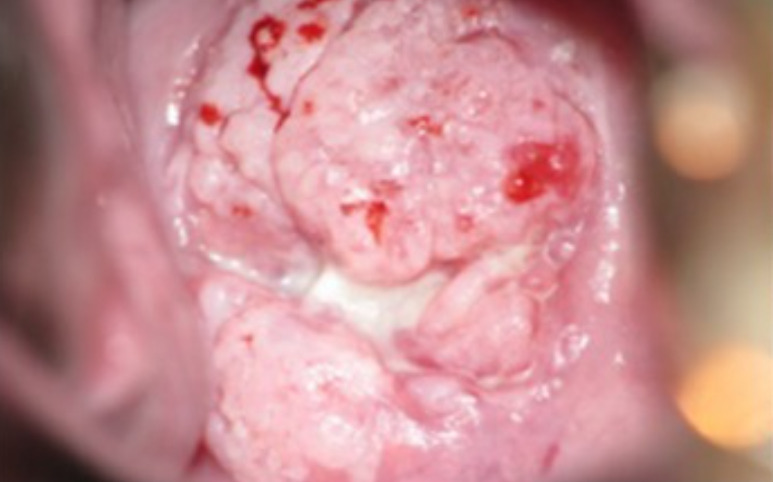
00:01 Hi. 00:02 Today I'd like to talk to you about HPV (human papilloma virus), cervical cancer and screening. 00:09 Let's talk a little bit about human papilloma virus, HPV for short. 00:14 The HPV genotype appears to be the most important determinant for the persistence and progression of disease. 00:22 There are two different oncogenic types. 00:24 One type is human papilloma virus 16 or HPV-16. 00:29 It has the highest carcinogenic potential and this is very important to remember for your test. 00:35 It accounts for about 55 to 60% of all cases of cervical cancer worldwide. 00:41 The next most carcinogenic type of HPV is HPV-18. 00:46 It's responsible for a lot less, 10 to 15% of all cases of cervical cancer. 00:53 There are risk factors for cervical cancer besides just HPV infection. 00:58 The known risk factors increase the likelihood of persistence of HPV infection which is normally cleared by a young, healthy woman. 01:05 However, if you're a smoker, that incidence of clearing is reduced. 01:12 Also, if you have a compromised immune system, that is with years of taking glucocorticoids, you can potentially have an increased persistence of HPV. 01:23 Also, we know that HIV infection can also increase the persistence of human papilloma virus leading to cervical cancer. 01:33 Let's talk a little bit about the molecular pathogenesis of HPV. 01:37 HPV belongs to the papillomavirus family and is a group of double-stranded DNA viruses. 01:45 HPV 6 and 11 which I have not mentioned yet causes genital warts while 16 and 18 are more likely to cause cervical cancer. 01:54 The progression to invasive cervical cancer is characterized by the viral DNA integrating into the host DNA. 02:01 HPV is very common. 02:04 It's usually an infection that occurs in teenagers and women in their twenties. 02:09 Although the prevalence is not quite known, it decreases as women age. 02:14 The lifetime cumulative risk though of acquiring it is about 80%. 02:20 Most young women, especially those under 21 have a very effective immune system that can clear the infection in about an average of eight months. 02:30 There's some guidelines that we now need to review. 02:33 They're from the United States Preventive Service Task Force, and they only apply to certain women. 02:40 So this is important to remember. 02:41 They apply to women who have a cervix and who are of age, greater than 21 years old, regardless of their sexual history. 02:51 It does not apply to women who have already received a pre-cancer cervical lesion diagnosis or have frank cervical cancer. 02:58 It does not apply to women who've been exposed to DES or diethylstilbestrol It does not apply to women who are immunocompromised such as women who are HIV-positive. 03:09 Here are the guidelines. 03:10 Again, women ages 21 to 65 should be screened with cytology every three years. 03:16 Women who are 30 to 65 who want to lengthen the screening can have intervals of five years with a combination of cytology and HPV screening. 03:26 And there are other recommendations that we no longer follow which are grade D recommendations. 03:32 So if you are younger than 21 or older than 65 or you already have had a hysterectomy due to cancer, or you are younger than 30, we don't do HPV testing alone or in combination with cytology in women again who are younger than 30. 03:50 What about prevention? So how can we prevent all of this morbidity and potentially mortality with HPV. 03:56 Well, now there is a vaccine that protects women against nine strains of HPV. 04:02 While it protects women, both boys and girls should receive the vaccine between the ages of 9 and 26 years old. 04:10 Thank you for listening.
About the Lecture
The lecture Cervical Cancer (HPV) by Lynae Brayboy, MD is from the course Gynecologic Pathology: Infections, Neoplasms and Screening.
Included Quiz Questions
Which of the following HPV strain is having the highest carcinomatous potential?
- HPV 16
- HPV 18
- HPV 11
- HPV 33
- HPV 35
Which of the following patients does USPSTF current recommendation for cervical cancer apply to?
- Women who are above 21 regardless of sexual history.
- Women who do not have a cervix.
- Women who are received a diagnosis of a high-grade precancerous cervical lesion or cervical cancer.
- Women with in utero exposure to diethylstilbestrol.
- Women who are immunocompromised.
Which of the following HPV strains cause genital warts?
- HPV 11
- HPV 16
- HPV 18
- HPV 33
- HPV 35
Which of the following statements are TRUE regarding HPV vaccination?
- HPV vaccination is recommended in boys and girls between the age of 9 to 26 years
- HPV vaccination is recommended for girls between the age of 9 to 26 years
- HPV vaccination is recommended for boys between the age of 9 to 26 years
- HPV vaccination is recommended for ladies between the age of 27 to 45 years
- HPV vaccination is recommended for men between the age of 27 to 45 years
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Straight to the point! Thi lecture gives you basic need to know info
I liked this lecture, it was short and very to point