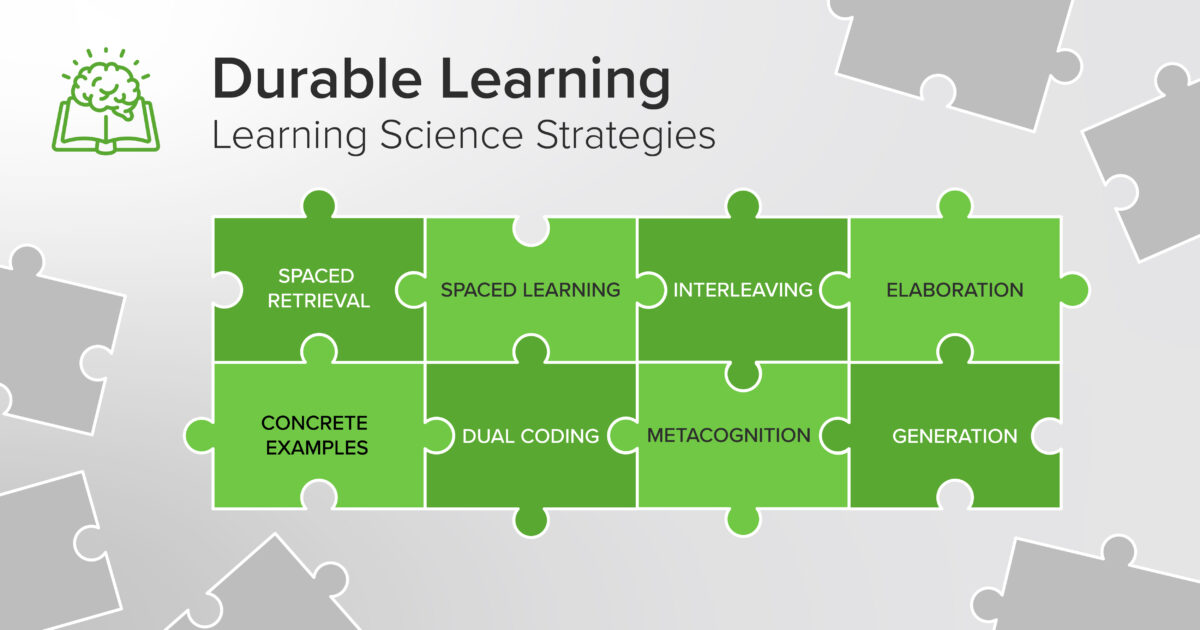
What is Durable Learning?
Durable learning refers to deep and lasting knowledge retention. While fostering durable learning might be the desired outcome of many teaching methods, some methods are better suited for it than others.
Durable learning is best fostered by integrating learning strategies backed by evidence, which support the efficient acquisition, retention, and retrieval of medical knowledge. Implementing these strategies into medical schools’ teaching methods can result in learning outcomes that move beyond familiarity with new material and lead to deeper, long-term retention and mastery of key concepts.
The Roles of Medical Schools and Educators Need to Change, as Do Their Tools
Medical education is a continuously evolving field. Evidence-based medicine has been a global standard for a long time but evidence-based medical education has only recently begun to gain broader acceptance and popularity. Incorporating the latest findings of learning science research into medical education is key, not only in basic sciences but also in clinical learning, as the latter directly impacts patient care.
Placed within this context, the imperative to foster durable learning among medical students gains acute relevance due to several challenges faced by medical schools worldwide:
- The demands placed on educators by the exponential increase in the amount of medical knowledge that needs to be transferred to students
- The demands placed on students in terms of efficient knowledge management throughout medical school (spanning 4 to 8 years)
- The long-term ability of students to acquire, retain, and apply accumulated knowledge, due in part to the widespread use of suboptimal study methods
Shifting to evidence-based teaching implies a change in roles for medical educators. The role of a medical educator becomes more that of a curator, creator, and moderator of online content and that of a coach rather than being the key channel of information transfer as for example in the traditional lecture approach.
Moreover, the influx of digital native medical students and the ever-changing knowledge landscape point toward the adoption of digital platforms as a way forward. These platforms allow for the deployment of evidence-based learning strategies, which can foster durable learning and guide medical students on their journey to becoming skilled health care providers.
Medical Education Needs to Keep Pace with an Ever-Changing Knowledge Landscape
Why is studying medicine today more challenging than ever before?
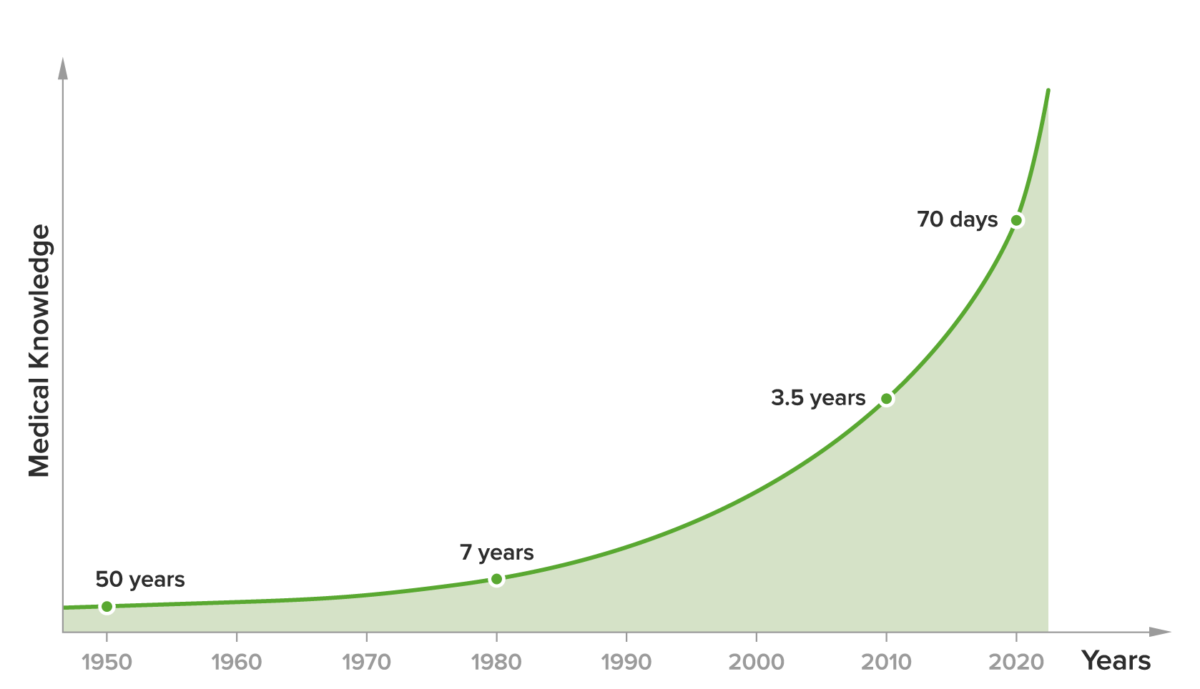
In 1950, medical knowledge doubled at an approximate rate of every 50 years; by 1980, that rate had increased to every 7 years, and 3.5 years in 2010. Today, the doubling time of medical knowledge is approximately 70 days.(1) Due to this exponential increase in the amount of knowledge medical students must learn and retain, they run the risk of “cognitive overload,“ which can negatively impact learning outcomes.(2)
The Doubling Time of Medical Knowledge(1)
Studying medicine is a marathon, not a sprint
The typical duration of medical education ranges from 4 to 8 years, which means that the amount of medical knowledge students need to learn will have doubled multiple times before they graduate. During this time, medical students must retain information from the basic sciences and then be able to practically apply it within a clinical setting. Therefore, fostering students’ durable learning is critical in order for them to become competent physicians after graduation. The challenge of long-term knowledge retention across the medical school curriculum and beyond has been extensively discussed in the literature.(3,4,5,6)
Medical students rely on common, yet inefficient, study methods
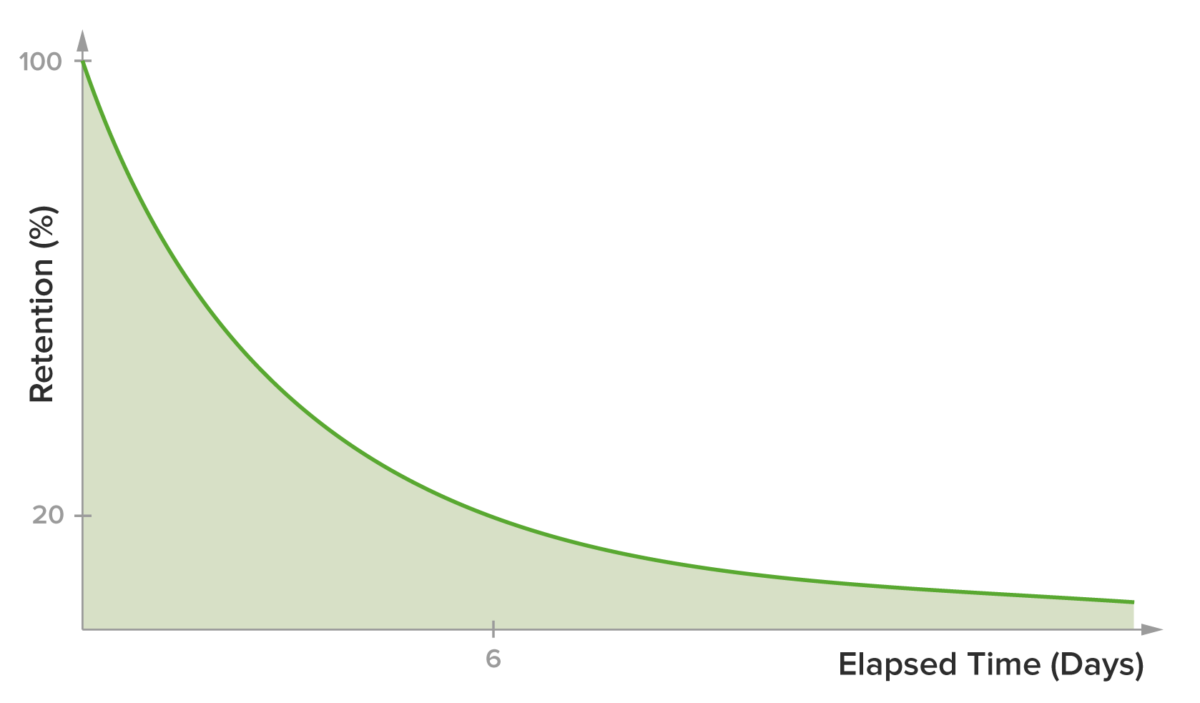
Medical students’ main job is learning, yet they predominantly rely on study practices that are far from optimal, such as massed learning (or “cramming”).(7,8) The popular belief that information can be embedded in a student’s long-term memory by massed practice leads students to use this inefficient study technique. While massed practice does provide students with a sense of familiarity with the material or even mastery of the subject(8), the information is in fact rapidly forgotten, as shown by the Ebbinghaus forgetting curve.(9,10)
Typical Representation of the Ebbinghaus Forgetting Curve(10)
Keeping Pace Requires a New Approach to Medical Education
Being a good educator is more than being a good clinician
Teaching methods used by medical schools and educators can play a key role in fostering durable learning. Established approaches to medical education, such as traditional lectures(11), still dominate the modern medical school landscape, despite being inefficient.(12,13) At the same time, medical educators rarely have a background in instructional design or regularly advance their teaching skills.(14) Therefore, becoming a good educator requires an effort that goes beyond being a good clinical expert.
Emerging online teaching methods impose new requirements on medical educators
The medical educator’s role has been gradually changing with the increasing prevalence of teaching approaches such as problem-based learning, team-based learning, and more. The emergence of the COVID-19 pandemic in early 2020 catalyzed this change. The current environment is continuing to accelerate the transition from traditional instructional methods to increasingly online-based approaches. This translates into new required roles for medical educators:
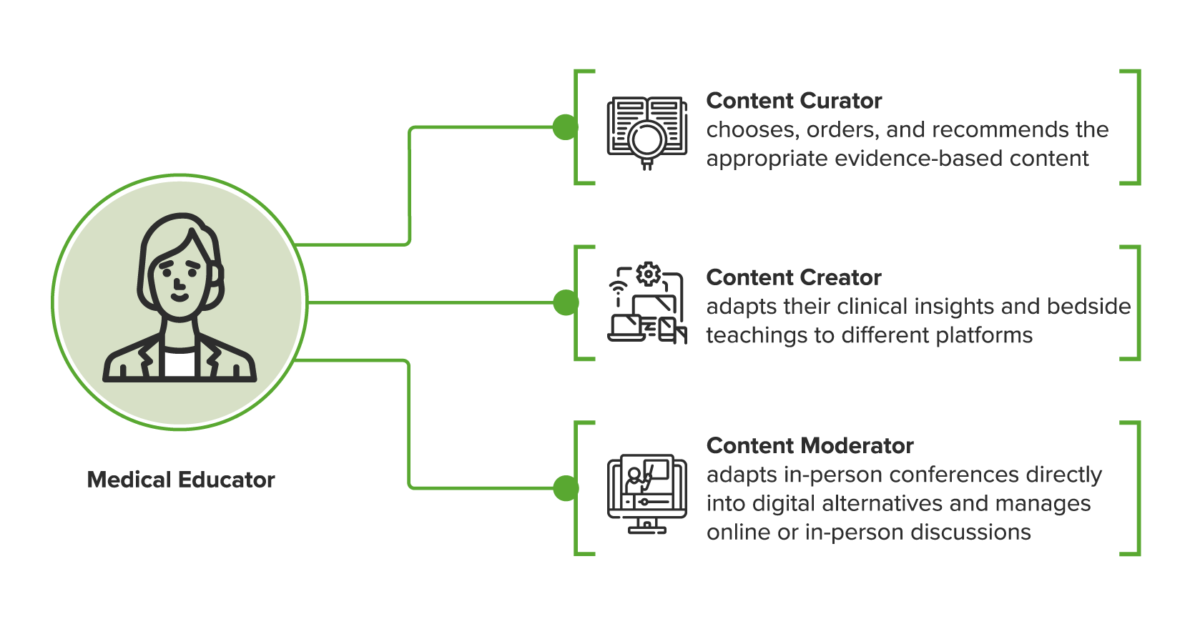
- Content curators, who choose, order, and recommend the appropriate evidence-based content at the right time and place for their students.
- Content creators, who adapt their clinical insights and bedside teachings to different platforms (in the form of tweets and short messages).
- Content moderators, who adapt typical in-person conferences directly into digital alternatives (online webinars, classes, or problem-based learning (PBL) tutorials) by becoming proficient in the tools of digital platforms and adept in managing online discussions.
These new roles of medical educators present different and significant challenges than their offline counterparts.(15)
The Evolving Role of Medical Educators(15)
Role of a coach remains essential in the post-pandemic era
A medical educator’s broader role as a coach, rather than a lecturer, gained relevance in the pre-pandemic era and should be further advanced post-pandemic.(16) Being a coach is being a “guide on the side” rather than a “sage on the stage.”(17) By guiding and empowering students’ self-directed learning based on strategies validated by learning science, medical educators use their time more effectively. Moreover, by leveraging innovative digital tools, educators enable students to access new material according to their individual needs and at their own pace.(18,19)
Evidence-Based Medical Education is the Way Forward
Implementation of learning science strategies is key
Critical clinical expertise and reasoning are built upon the foundational knowledge students acquire early on in medical school. The lack of durable learning in these first years thus impacts students and junior doctors around the globe and poses a challenge to medical education.(20)
This challenge can be addressed by implementing the validated findings of learning and cognitive science in the instructional design and assessment methodologies of medical schools. These evidence-based learning strategies are most powerful when applied in combination:
- Spaced Retrieval
- Spaced Learning
- Interleaving
- Dual Coding
- Concrete Examples
- Metacognition
- Elaboration
- Generation
Most of these evidence-based learning techniques can be implemented through the use of a digital learning platform and help to increase the knowledge acquisition and retention rates of medical students without compromising teaching models essential in a clinician’s journey to becoming a good health care provider.
Digital platforms have emerged as a response to new challenges
The evolving global knowledge landscape and the new generation of digital native learners necessitate the adoption of digital platforms, such as Lecturio, as a response to the accelerating growth of medical knowledge and the long-term retention thereof. Digital learning platforms provide medical students with effective tools to quickly and continuously access, acquire, and retain ever-changing knowledge, allowing them “to learn anything, from anyone, at any time.”(21,22)
Would you like to learn more about this topic? Read the in-depth article, “Durable Learning in Medical Education.”
Online Seminar
This first online seminar from Lecturio’s Durable Learning series focuses on challenges faced by medical schools worldwide, the changing roles of medical educators and aims to help them understand the science behind evidence-based learning strategies.
Watch the seminar recording:
Would you like to learn more? Explore the Pulse Seminar Library.