Playlist
Show Playlist
Hide Playlist
Sexually Transmitted Infections (STIs): Sores/Ulcers, Syphilis, and Genital Herpes Simplex
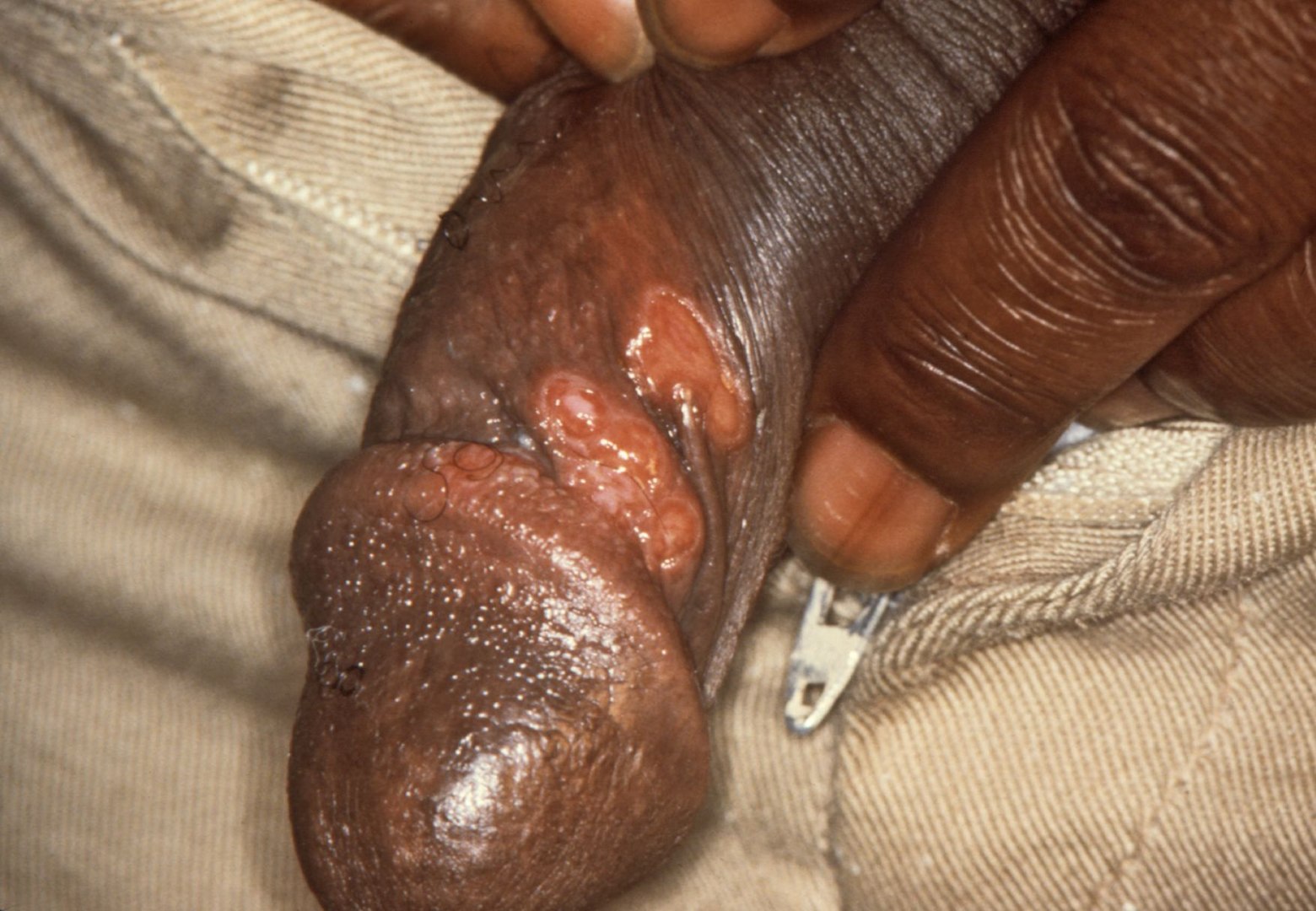
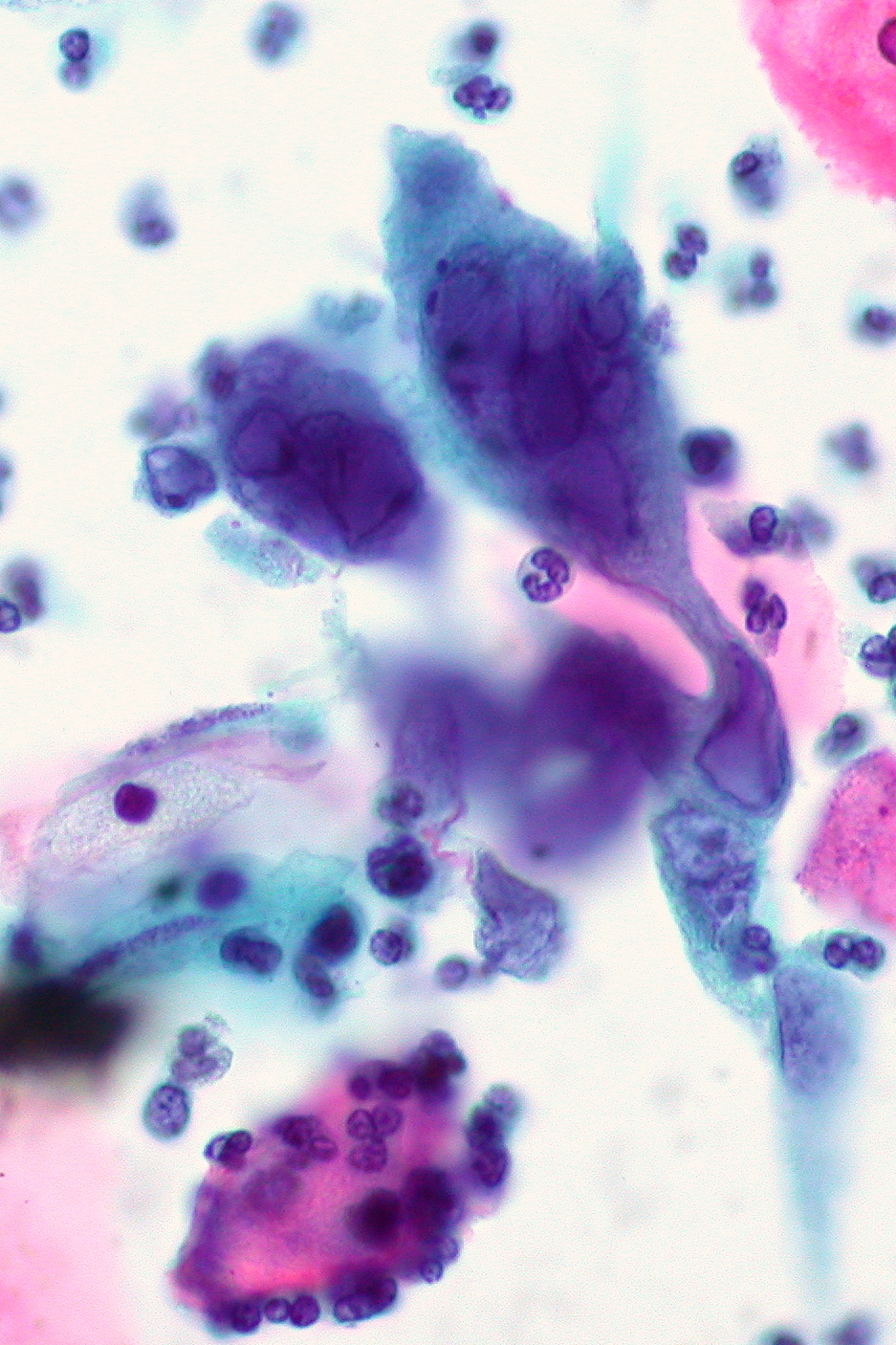
00:00 Hello, in this lecture, we'll be discussing sexually transmitted infections in women. 00:08 In the United States, sexually transmitted infections traditionally called STDs, now called STIs, are a problem. 00:17 You can see here, that we have high rates of human papilloma virus as well as HSV or herpes simplex virus-2 Half of the infections are in men and about half are in women which make up about a hundred million types of infections. 00:37 Why are STIs so important to discuss? Well, they facilitate HIV transmission. 00:44 They do this by disrupting the epithelial mucosal barriers that are important in protecting the body. 00:52 They can also increase the number of HIV targets in the genital tract. 00:57 They also increase expression of HIV co-receptors. 01:02 They induce secretion of cytokines and increase HIV shedding and also, HIV alters the natural history of some STIs. 01:13 So essentially, STIs and HIV work together to make the patient sicker. 01:18 I now want to bring your attention to two classifications recommended by the CDC or the Centers for Disease Control. 01:26 Sores or ulcers are actually caused by syphillis, HSV-1 and HSV-2. 01:34 As you might have read, HSV-1 is traditionally oral while HSV-2 is traditionally genital but they can affect each body part. 01:43 Other uncommon causes of sores in the US include LGV, chancroid or granuloma inguinale. 01:55 Now let's talk about drips, the second classification. 01:59 These are discharges, so women usually would present with some type of vaginitis or an abnormal discharge. 02:06 Commonly, gonorrhea and chlamydia are the culprits. 02:10 You can also have nongonococcal urethritis or cervicitis. 02:15 Trichomonas vaginitis or urethritis also cause an abnormal discharge. 02:20 You can get a discharge with a yeast infection or Candidiasis, this is non-STD. 02:26 You can also have bacterial vaginosis which is not sexually transmitted but can be sexually associated. 02:33 We'll discuss that in a little bit. 02:35 The major concerns though are genital HPV especially type 16 and 18 and cervical, anal and oral cancer. 02:45 Let's now talk about a case. 02:48 A 30-year old woman presents to your clinic with the following physical finding: What's your diagnosis? We'll, if you've read here, it's herpes simplex. 02:59 Well, what else do we need to know? It could be syphillis. 03:03 It could be a zipper cut but unlikely, or it could be granuloma inguinale. 03:10 What do you need to do to differentiate? Additional testing. 03:14 So you need to ask the patient if the sores are painful. 03:18 This is usually indicative of chancroid. 03:21 or it could be very painful, associated with herpes. 03:25 Typically, syphillis presents as a painless sore. 03:29 LGV is also traditionally painless as well as granuloma inguinale. 03:35 Let's talk about primary syphillis. 03:38 This is rare to see but in any immunocompromised patient, this may be present, especially a patient with HIV or AIDS. 03:47 Primary syphillise has a 10-90 day incubation, On average, three weeks. 03:53 You can see a chancre on examination and early on you may see a macule or papule that tends to lead to erosion around the edges. 04:03 Usually, the base is clean, painless and indurated with smooth, firm borders. 04:09 It can go unnoticed in a large percentage of the population and it typically resolves on one to five weeks. 04:17 This stage is highly infectious and therefore, their sexual partners are at risk. 04:24 Let us now review what it looks like in a female. 04:27 If you were to do a speculum exam, you should always wear gloves. 04:31 In the clinical setting of syphilis, you may see the characteristic chancre on the labia as shown in this image. 04:38 Externally, you may see a sore on the outside, on the labia minora or majora. 04:46 Here you see it pictured on the labia minora, on both sides or bilaterally. 04:53 Let's now talk about secondary syphillis. 04:56 This represents a dissemination of the spirochetes throughout the blood. 05:01 This usually takes two to eight weeks after the initial presentation of the chancre. 05:08 The rash is usually a whole body rash and does include the palms and the soles, which is unusual for rashes as the palms and the soles are usually spared. 05:20 You sometimes can have mucus patches in the mouth and you may see a condyloma lata which is highly infectious. 05:28 This is not to be confused with condyloma accuminata which is seen on the cervix and other scenarios. 05:35 The patient may have constitutional symptoms such as fever and usually signs and symptoms resolve in two to ten weeks. 05:45 Early diagnosis of syphillis is very important especially in a reproductive age woman as she is at risk for pregnancy. 05:53 Clinical presentation should alert you to the diagnosis of syphillis but you can use skin lesions to obtain spirochetes to do darkfield microscopy also serology with an RPR is important in diagnosing syphillis. 06:07 These are often tested on your exam and you may wanna go over these in some detail. 06:14 Let's now talk about the treatment. 06:16 Especially in a pregnant woman, Benzathine Penicillin 2.4 million units is very important. 06:24 If a patient has an allergy, then she would need to be desensitized but that's beyond the scope of the USMLE. 06:31 But just remember, penicillin is the treatment. 06:35 Let's now discuss genital herpes. 06:38 This is usually caused by HSV-2 but can be caused by HSV-1. 06:43 Transmission is usually through direct contact, usually during asymptomatic shedding. 06:49 That means, the partner may not have any lesions but can still shed virus. 06:54 Primary infection is commonly asymptomatic. 06:58 Symptomatic cases sometimes can be very severe, prolonged and have systemic manifestations. 07:05 Vesicles errupt and cause painful ulcerations and crusting. 07:10 There is a definitive recurrence potential and patient should be made aware of this. 07:17 Let's now talk about the diagnosis of HSV-1 or HSV-2. 07:22 Typically, we do PCR. 07:24 Culture was an older method that we did utilize, and we also do serology. 07:30 Typically you will do PCR from a lesion that you see upon presentation. 07:36 Culture was done traditionally but serology can be done quickly in the office with just a blood test. 07:44 Let's now talk about treatment. 07:46 Since herpes simplex virus is a virus, we need to use antivirals. 07:51 We typically use acyclovir, valcyclovir and famciclovir. 07:56 These may potentially show up on some of your examination questions. 08:01 Just to remind you, we had a case from earlier in the lecture. 08:05 This patient did in fact have herpes simplex. 08:09 These are what the ulcerations may look like. 08:11 These can be very painful and lead to dysuria.
About the Lecture
The lecture Sexually Transmitted Infections (STIs): Sores/Ulcers, Syphilis, and Genital Herpes Simplex by Lynae Brayboy, MD is from the course Gynecologic Pathology: Infections, Neoplasms and Screening. It contains the following chapters:
- Symptoms - Sores/Ulcers
- Syphilis - Clinical Manifestation
- Genital Herpes Simplex
Included Quiz Questions
Which of the following presents as discharge in patients with sexually transmitted diseases?
- Trichomonas vaginalis
- Syphilis
- Genital herpes
- Chancroid
- Granuloma inguinale
Which of the following presents as ulcers in patients with sexually transmitted diseases?
- Genital herpes
- Trichomonas vaginalis
- Bacterial vaginosis
- Gonorrhea
- Chlamydia
Which of the following presents as painful ulcers?
- Chancroid
- Secondary Syphilis chancre
- Lymphogranuloma venerum
- Granuloma inguinale
- Primary syphilis chancre
Which of the following is NOT a part of the secondary syphilis features?
- Aortitis
- Rash
- Mucus patch
- Condyloma lata
Which of the following is used for confirmatory diagnosis of syphilis except for clinical presentation?
- Darkfield microscopy and serological tests
- Culture
- Microscopic examination
- Biopsy
- Immunofluorescence
Which of the following is the treatment of choice in patients with early syphilis?
- Benzathine Penicillin G 2.4 million units
- Procaine penicillin 1.2 million units
- Amoxicillin 500 mg
- Azithromycin 500mg
- Metronidazole 500mg
Which of the following is NOT used in the diagnosis of herpes simplex?
- Gram stain
- PCR
- serology
- Culture
- Western blot
Which of the following is used in the treatment of herpes simplex?
- Acyclovir
- Ribavarin
- Gemcitimab
- Lamivudine
- Interferon beta
Customer reviews
3,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
2 |
I felt Dr. Brayboy did an amazing job with this lecture. I greatly appreciate her clear explanation.
Just reading the slides. Poor lecturing ability had to study this from another source. And lecturer is constantly mentioning whether the topic is on usmle or not.
she modulates her voice that keeps you engaged and divides the content into easy to understand packages of knowledge
just reading the screen in front of her but that's not the big deal.. her pauses are horrible misleading and ruining the focus .. so instead of focusing on the subject im focusing on understanding whenever she pauses in a wrong place one repeating voice rhythm circling again and again sorry but i had to find some other resource to study this subject from