Playlist
Show Playlist
Hide Playlist
Opioid Analgesics – Drugs of Abuse
-
Slides Opioid Analgesics Drugs of Abuse.pdf
-
Slides Opioid Analgesics Fentanyl .pdf
-
Slides Opioid Analgesics Fentanyl .pdf
-
Reference List Pharmacology.pdf
-
Download Lecture Overview
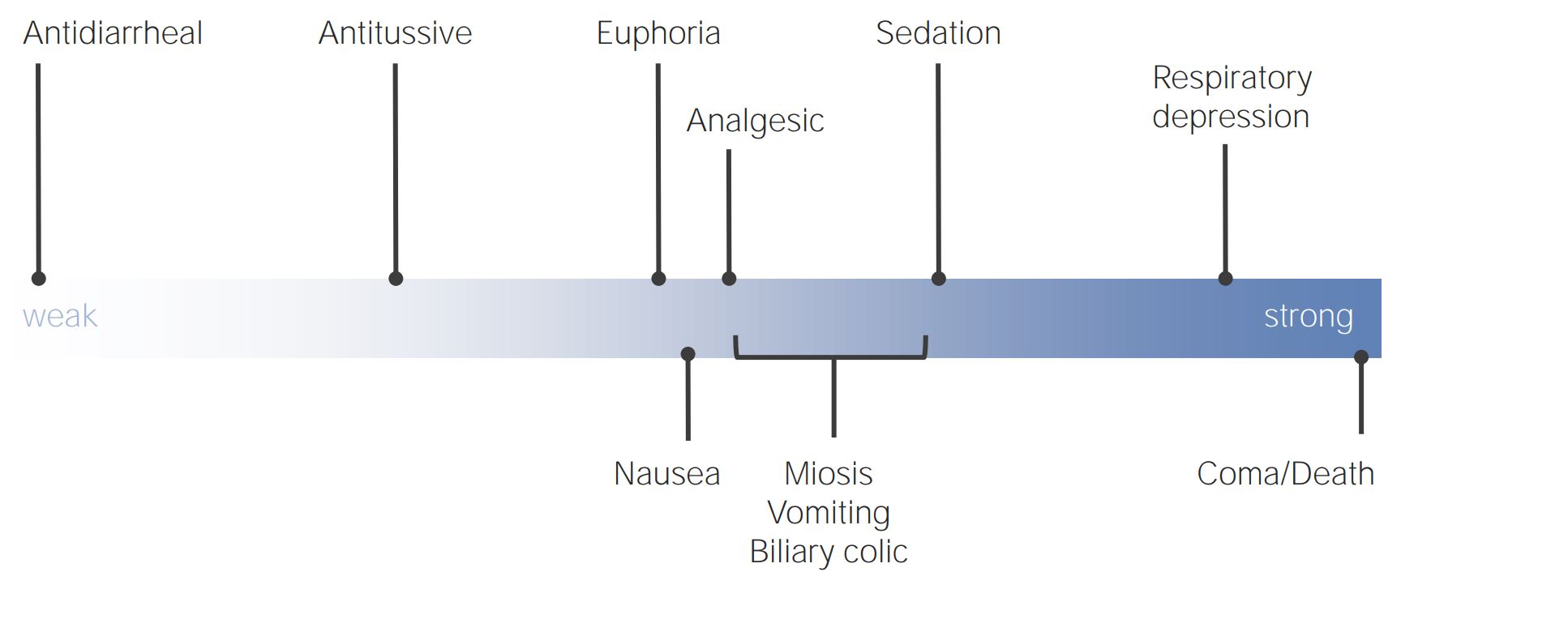
00:01 Welcome to pharmacology by Lecturio. 00:03 Today we're going to be talking about opioids. 00:06 Specific to toxicology, we expand the definition of opioids not just to include those drugs that are prescribed by physicians but also those medications that are taken illegally. 00:17 This includes drugs like heroin or even morphine. 00:21 Sometimes this will include illegal ingestion of oxycodone and codeine. 00:26 This can also include meperidine. 00:28 And more recently we've seen a spike in the use of illicit fentanyl, carfentanyl and sufentanil. 00:35 Now remember that the antidote for all of these medications is Naloxone. 00:41 We also use a partial agonist called methadone in the treatment of patients who have addiction to opioids. 00:48 Now opioids in general will work through either the mu, the kappa or the lambda receptors in the opioid subclass. 00:58 They also may disinhibit the dopaminergic pathways in the central nervous system. 01:05 And finally, it should be noted that there is a biphasic component to the response of opioids. 01:11 You'll have an initial rush of euphoria followed later by sedation and even a coma. 01:17 I wanna talk quickly about fentanyl. 01:20 Fentanyl is now the new epidemic in North America. 01:24 It is 100 times more potent than morphine. We use to initially sell it as a patch so patients would often get chronic pain prescriptions with fentanyl patches. 01:35 Then we started to see pharmacy thefts. 01:37 Now we start to see fentanyl being sold on the street. 01:41 This first started in 2013 where we saw upswings in some US cities including Chicago, New York, Detroit and Philadelphia. 01:51 By 2015, we started to see an upswing in areas of Canada as well. 01:56 And this was associated with organized crime. 01:59 By 2016, it was the most overdosed drug in America. 02:03 By 2016 as well we started to see it being cut in illicit labs with MDMA, with cocaine, with heroin and with ecstasy. 02:13 And more recently, we're starting to see street cuts with -- cuts with marijuana or liquid fentanyl where it's being mixed with drinks including things like syrup, like cough syrup or even over-the-counter pop and sodas. 02:29 Now here's a graphical representation of the toxicity of the different agents. 02:35 On the left you see heroin. In the middle you see fentanyl. 02:40 So you can see that a smaller amount of fentanyl will give you the same amount of high. 02:45 And finally on the far right you can see carfentanyl and how incredibly toxic it is. 02:51 I've put a pen there for a comparison of size. 02:54 So barely a speck of carfentanyl will give you as much of a medical effect as a large amount of heroin. 03:02 Lately on the market we started to see sufentanil. 03:08 Now sufentanil is 10 times more potent than fentanyl and 1000 times more potent than morphine. 03:15 Carfentanyl is 100 times more potent than fentanyl and it's 10,000 times more potent than morphine. 03:23 Now, just because carfentanyl is so much more potent doesn't necessarily mean it's more dangerous because it has a very short half-life. 03:31 Where does this come into relevance for you? Well first of all, this is going to be relevant for you when you are working as emergency personnel. 03:41 Remember that you do not wanna eat or drink or smoke, referring to putting the cigarette in your mouth or use the bathroom while working in an area with suspected fentanyl use. 03:54 So this includes if you're working with EMS on your ride along programs and you go into a home where there's suspected fentanyl use, be very careful of what you touch and where you go. 04:06 Do not touch your eyes, nose or mouth during these circumstances. 04:11 It's incredibly hard to do, believe me because when you're dealing with patients and you're -- you know intellectually that you're not supposed to touch your eyes, nose and mouth. 04:20 You invariably wanna scratch yourself in the nose or you get a twitch in your eye. 04:24 It's just psychological. 04:26 Remember that field testing of these products should be avoided. 04:33 We wanna do the tests in the lab. The problem with field testing is wind. 04:37 You can have wind whip up the product into your face and that could be potentially lethal. 04:43 Avoid aerosolization of any of these products. 04:48 So even, you know, flapping a bedsheet as you're trying to get to a patient who might be comatosed with fentanyl overdose can release fentanyl into the air and then you ingest it. 04:59 Wash your hands with soap and water after each run. 05:02 Make sure you're wearing gloves and do not use latex gloves. 05:06 Latex gloves do not provide protection against fentanyl overdose and exposure. 05:11 You should use nitrile gloves. 05:14 Finally, masks are recommended for first responders and code teams when you're going in to places where there is suspected fentanyl abuse. 05:26 Okay. Take care of yourselves out there. Make sure that you're playing it safe. 05:31 This will probably be on your exams as well, so it's important to know the risks associated with fentanyl and carfentanyl in the real world and then on the street. And show them what you know on your exam.
About the Lecture
The lecture Opioid Analgesics – Drugs of Abuse by Pravin Shukle, MD is from the course Toxicology. It contains the following chapters:
- Toxicology: Opipoid Analgesics
- Fentanyl
Included Quiz Questions
Which statement is correct about the potency of morphine and fentanyl?
- Fentanyl is 80-100x as potent as morphine.
- Fentanyl is 10-20x as potent as morphine.
- Fentanyl is as potent as morphine.
- Morphine is 10-20x as potent as fentanyl.
- Morphine is 80-100x as potent as fentanyl.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
me gusto mucho. es muy facil de comprender y muy interactivo con el estudiante
1 customer review without text
1 user review without text