Playlist
Show Playlist
Hide Playlist
Linezolid, Streptogramins and Chloramphenicol – Bacterial Protein Synthesis Inhibitors (Antibiotics)
-
Slides Linezolid Streptogramins Chloramphenicol Antibiotics.pdf
-
Reference List Pharmacology.pdf
-
Download Lecture Overview
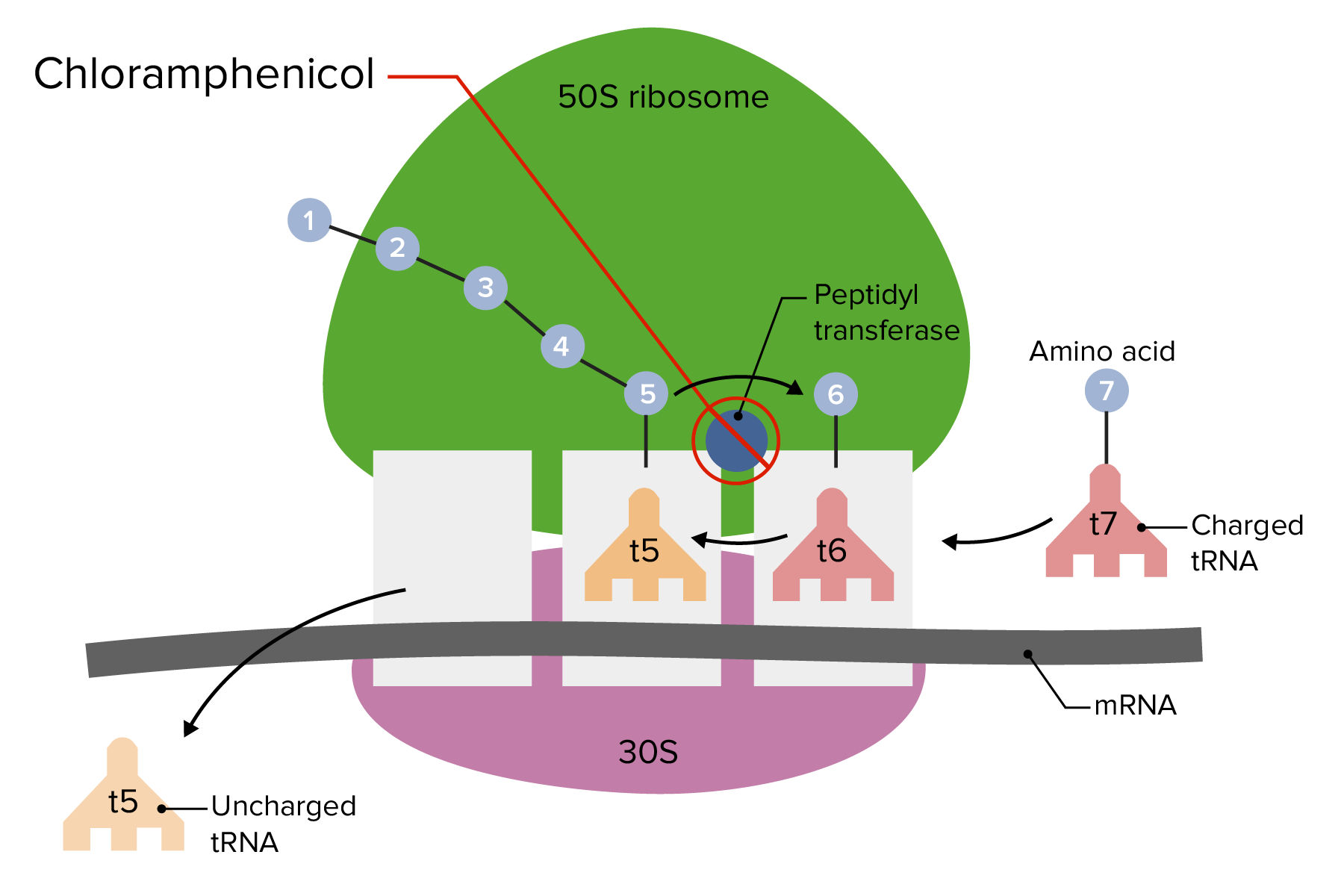
00:01 So, let's talk about that last one linezolid. 00:04 They're used in drug-resistant gram-positive cocci infections like, Methicillin-Resistant Staph Aureus, Penicillin Resistant Strep-Pneumo and Vancomycin-Resistant Enterococcus. 00:16 They bind to the 50 S ribosomal unit as I had mentioned before, there is no cross resistance with other protein synthesis inhibitors and they're reserved for multi-drug resistant agents. 00:27 Now, I want to just show you a picture from an echocardiogram. 00:31 This is a tricuspid valve, so on the left side you can see the tricuspid valve and you can't really see any kind of vegetation. 00:40 On the right where the green arrow is pointing, you can see a large vegetation on one of the tricuspid valves. 00:46 This person has obviously, a fairly severe endocarditis and a valvular vegetation, because it's the tricuspid valve, you know, it's the right side, it's probably involved with some kind of intravenous drug abuse. 01:00 This patient had multiple resistant infection was actually treated quite successfully with this drug. 01:07 Now, in terms of toxicity. 01:09 Toxicity of this drug include thrombocytopenia and neutropenia. 01:12 This particular patient developed thrombocytopenia, which was managed conservatively. 01:18 Unfortunately, you can also have serotonin syndrome. 01:21 So, remember that, if you know, your IV drug abusers also tend to be on antidepressants, there's a high correlation there and if you're using this antibacterial agent you may actually induce a serotonin syndrome. 01:33 So, please go back to your psychiatry lectures and take a good look at serotonin syndrome, so, that you understand it. 01:41 The streptogramins are a combination of two medications, they tend to be bactericidal, with really good post-antibiotic effects. 01:51 They are active against MRSA, VRSA and other resistant enterococci. 01:56 Now, E. faecalis is resistant to these agents, because they have a very unique efflux transport mechanism. 02:04 Which is kind of cool, these organisms have actually evolved a way of getting rid of streptogramins from the inside of their cytoplasm. 02:12 In terms of toxicity and adverse events. 02:16 You often get a very painful injection site, you can get myalgia and arthralgias. 02:21 Remember that these agents are potent inhibitors of CYP450 3A4, so therefore if you remember your other lectures, they will increase plasma levels of drugs like, cyclosporine, diazepam and warfarin. 02:36 Chloramphenicol has a very distinct structure. 02:39 There's actually no other drugs in its class, so, it's on its own. 02:43 It has wide distribution, it's a non-polar molecule as you can see, so, it crosses the blood-brain barrier and the blood uterine barrier. 02:52 It's inactivated in the liver and it is excreted in the urine. 02:56 It's bacteriostatic against Haemophilus, Neisseria, the Bacteroides species. 03:01 It's also used as a backup drug against Salmonella, pneumococcal disease and meningococcus. 03:07 It can also be used topically quite often as well. 03:10 It is not active against chlamydia species. 03:14 The resistance is through a plasmid-mediated formation of an enzyme, called an acetyltransferase, that inactivates that drug. 03:23 The toxicity especially for topical use, is direct irritation, you can also get super infections like candidiasis, remember that chloramphenicol does not work against candida. 03:35 Aplastic anemia, is a potential side effect, that's relatively rare about 2.5 per 100,000, it is irreversible and can be fatal though. 03:46 The one thing that i want you to remember about chloramphenicol, is something called, “Gray baby syndrome,” It is going to be on your exams, at some point in your career. 03:54 That is where you get anemia, cyanosis, cardiovascular collapse, it affects neonates, especially those who are premature and it may be linked to a deficiency in the hepatic glucuronyltransferase. 04:08 So, it's something important to be aware of and to know.
About the Lecture
The lecture Linezolid, Streptogramins and Chloramphenicol – Bacterial Protein Synthesis Inhibitors (Antibiotics) by Pravin Shukle, MD is from the course Antimicrobial Pharmacology. It contains the following chapters:
- Linezolid
- Streptogramins
- Chloramphenicol
Included Quiz Questions
What statement about linezolid is INCORRECT?
- It is a potent inhibitor of CYP450 3A4.
- There is no cross-resistance with other protein synthesis inhibitors.
- When combined with SSRIs, it may lead to serotonin syndrome.
- It is associated with thrombocytopenia and neutropenia.
- It may be used against MRSA and VRE.
What statement about Gray baby syndrome is INCORRECT?
- It is the result of streptogramin toxicity.
- It may be linked to an insufficiency of hepatic glucuronyltransferases.
- It primarily affects newborns.
- It presents with anemia, cyanosis, and cardiovascular collapse.
- It is associated with prematurity.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |