Playlist
Show Playlist
Hide Playlist
Localized Rashes: Impetigo, Cellulitis and Herpes Zoster
-
Slides LocalizedRashes AcuteCare.pdf
-
Download Lecture Overview
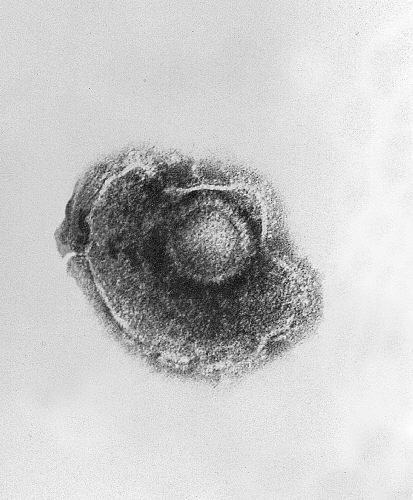
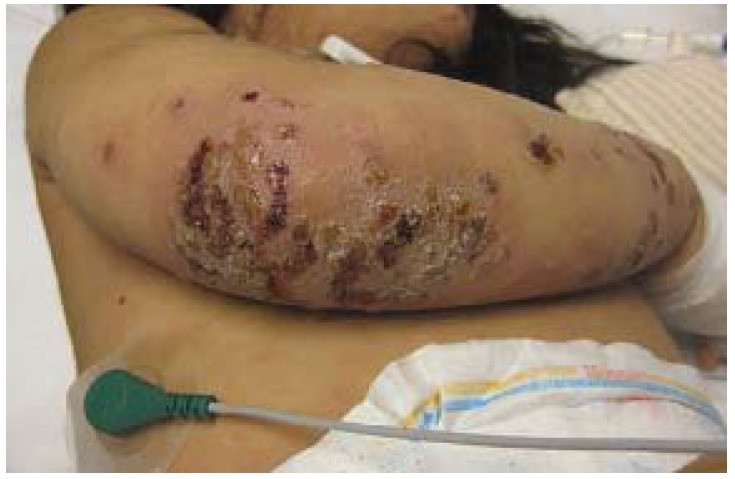
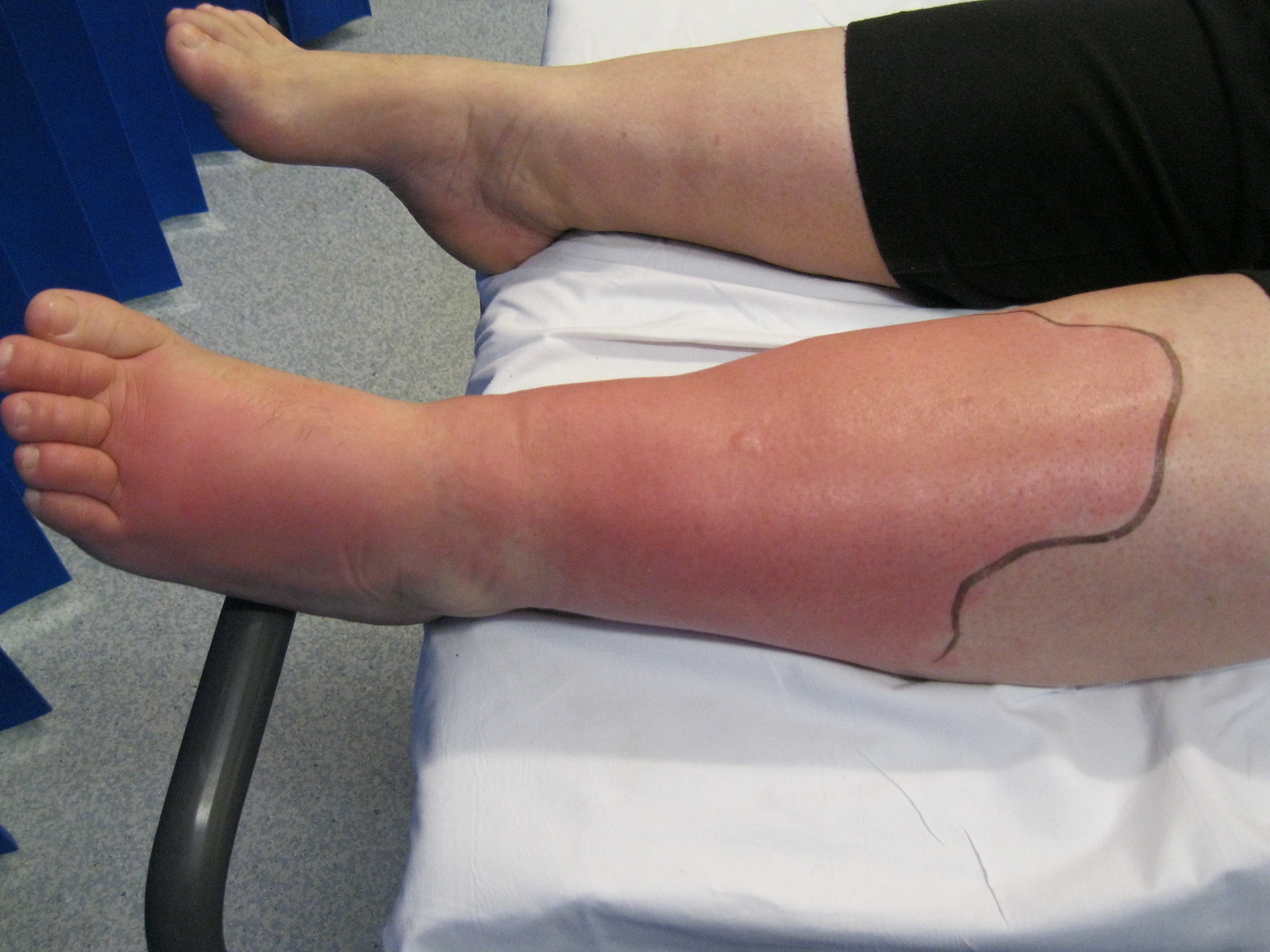
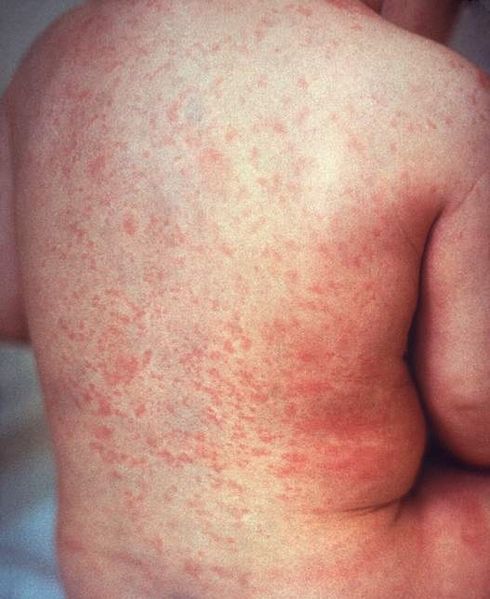
00:01 Erysipelas and cellulitis, so this is an infection of the superficial skin structure down into the dermis. 00:07 That’s the difference but they appear very similarly. Pain, tenderness, calor, erythema - those are the hallmarks of both of these. 00:16 But erysipelas is more superficial and sometimes you'll have a hard time differentiating between the two just based on what you are saying in front of you in clinic. 00:26 Aggressive when it comes to the potential for methicillin-resistant Staph aureus or MRSA. 00:32 If there is somebody who has frequent health care contact or certainly with a history of MRSA in the past, I'm gonna treat them with a different set of antibiotics. 00:41 It may be for a patient who’s naïve, for a child for example that child might be -- receive a cephalosporin using first generation, but for the patients like mine who have all those comorbidities, goes to the doctor a lot, get admitted to the hospital, sometimes you're in a rehabilitation center or a nursing home; clindamycin, trimethoprim-sulfamethoxazole could be good options for them because that will handle the MRSA more effectively. 01:08 And just a warning, always be cognizant of the fact that cellulitis can progress into a necrotizing fasciitis and necrotizing fasciitis can masquerade initially as just a simple cellulitis so patients who feel really sick, who have a rapid progression of their rash, who have other evidence like neurovascular or neurological changes that suggests infection in deeper layers, compartment syndrome, those are patients you want to stay on top of and refer urgently, don’t wait to send them to the emergency department for a surgical referral -- do it right now. 01:47 Just moving on to zoster, and this is just the figure there shows the progression of shingles or zoster. 01:55 It’s related of course to the varicella virus which sits in your dendrites dormant and once its awakened it travels up nerve fibers and creates its blistering rash. 02:08 Again, just like I did when the kid got chicken pox, like many years ago, the herpes zoster comes back. 02:16 So the key with herpes zoster is the dermatome of distribution because it’s related to those nerve fibers so that’s what separates it from other types of blistering rashes. 02:26 It’s usually found over those thoracic dermatome but one important factor is that if it -- don’t be shocked if it crosses the midline about one in five cases, too, but it should have stay dermatomal as well. 02:38 Post-herpetic neuralgia can be absolutely debilitating. 02:42 Luckily it is still uncommon but certainly it does happen, about 13% of cases of herpes zoster develop post-herpetic neuralgia more common as patients grow older. 02:55 So luckily we can prevent both herpes zoster and post-herpetic neuralgia as well, and that’s what the application of the varicella vaccine or the shingles vaccine. 03:06 Now it’s a one dose vaccine given at age 60, it’s recommended by the US Centers for Disease Control and Prevention and it is a fact they’ve been preventing zoster, it’s actually more effective though in preventing post-herpetic neuralgia, so it can cut the case of post-herpetic neuralgia by about two thirds compared with no vaccination. 03:25 Once you see a case of zoster in your clinic prescribe antiviral agents there, there are a number out they're all effective so it’s really based on dosing as to which one you prefer that can reduce the duration of symptoms. 03:39 It also reduces viral shedding but it’s important to get it on board early. 03:44 Most patients I've -- in my experience, do come in fairly early with this because they are concerned; it hurts for one thing and therefore they want pain relief from the pain of the shingles but they also wanna get treated and that improves things. 03:58 Very important to keep these patients while they have the active lesions away from young children, away from pregnant women who could be at special risk if they contract varicella; and also anybody who is immunocompromised. 04:13 Corticosteroids have been used for the management of herpes zoster, they don’t seem to be effective and because they have a lot of side effects even the short course, they're not routinely recommended. 04:25 Alright, so that just took you through some localized rashes and hopefully you have a good sense of how to treat them and I guess my question is, how itchy do you feel right now? Don’t worry, you'll be fine. Just use some emollients and we’ll see you next time.
About the Lecture
The lecture Localized Rashes: Impetigo, Cellulitis and Herpes Zoster by Charles Vega, MD is from the course Acute Care. It contains the following chapters:
- Impetigo and Cellulitis
- Herpes Zoster
Included Quiz Questions
A 69-year-old man presents with an itchy and painful rash along his waistline for the past 2 days. On physical examination, he is afebrile and has a vesicular rash that does not cross the midline. Which of the following is the most appropriate pharmacotherapy at this time?
- Systemic antiviral therapy
- Topical steroids
- Systemic antibiotics
- Topical antibiotics
- Systemic steroids
Which of the following regarding herpes zoster is INACCURATE?
- It never extends beyond a single dermatome.
- It follows dermatomal distribution.
- It spread down the sensory nerve to cause the typical rash.
- The thoracic and lumbar dermatomes are most commonly involved.
- It is predominantly vesicular.
Which of the following has been shown to decrease the risk of post-herpetic neuralgia?
- Live attenuated herpes zoster vaccine
- Immunosuppression
- Topical corticosteroids
- Older age
- Topical lidocaine
Which of the following is a treatment option for cellulitis in patients with chronic healthcare contact or history of MRSA?
- Systemic clindamycin
- Vancomycin
- Topical clindamycin
- Amoxicillin
- No therapy is required.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |