Playlist
Show Playlist
Hide Playlist
HIV Infection and HIV Life Cycle– Secondary Immunodeficiency Diseases
-
Slides Secondary Immunodeficiency.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
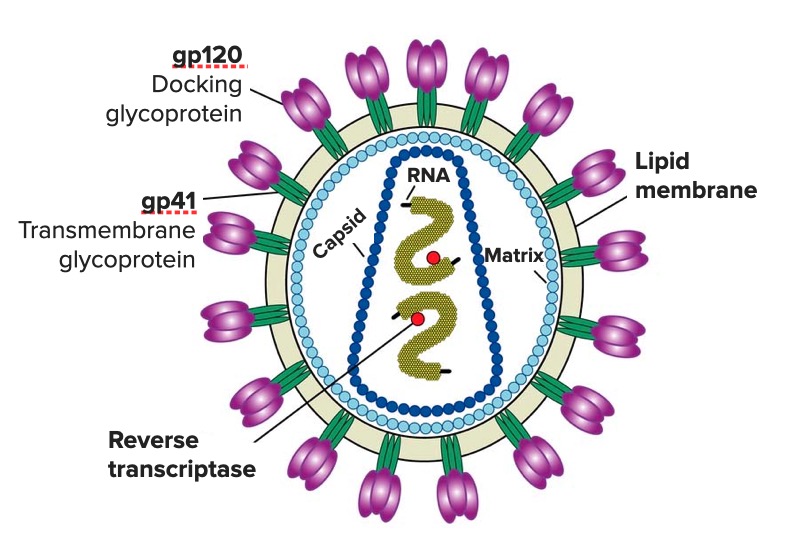
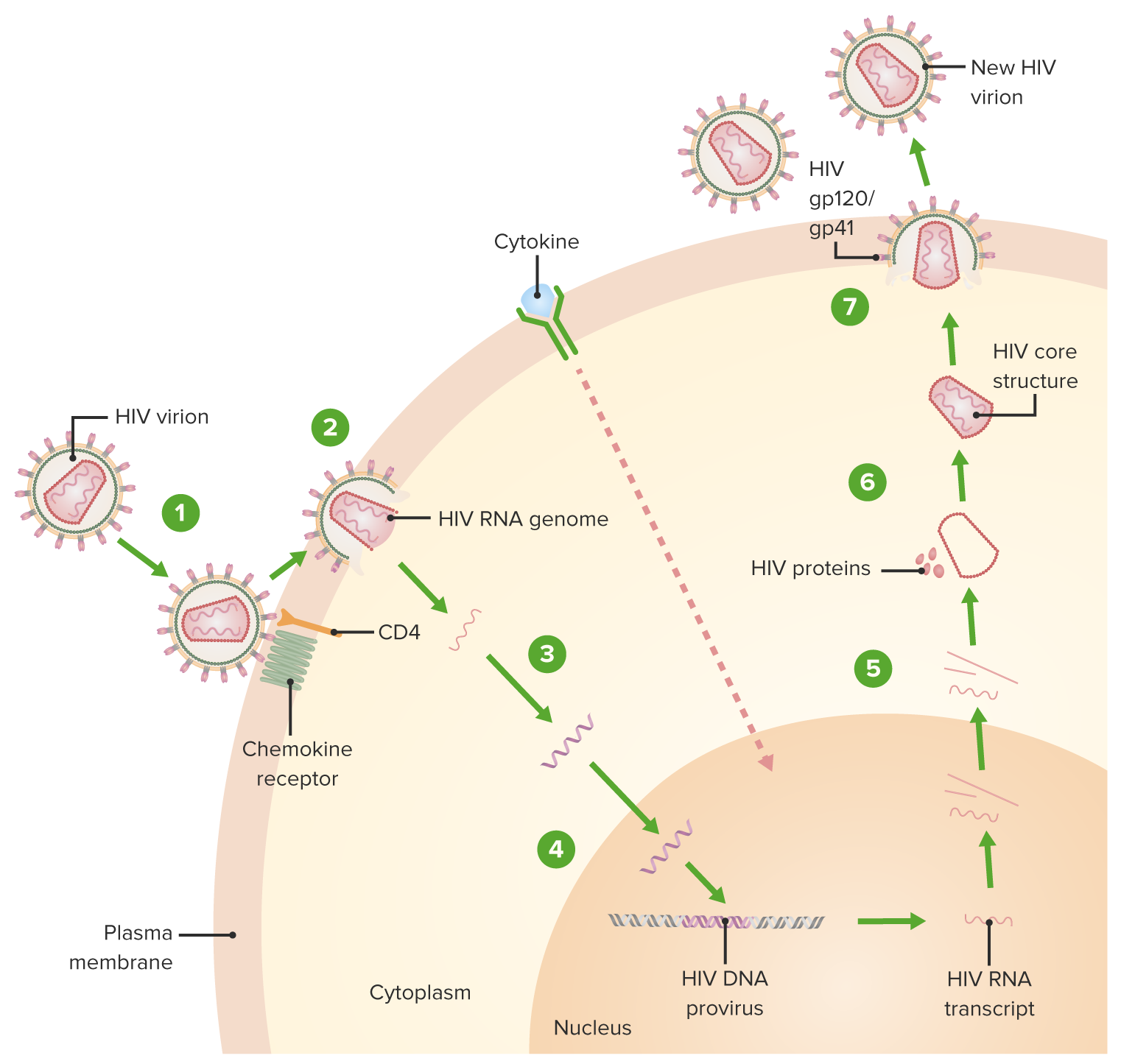
00:01 So let’s now focus on the HIV virus and the Acquired Immune Deficiency Syndrome. 00:09 HIV is a retrovirus and it can infect CD4+ T-cells, macrophages and dendritic cells. 00:24 The HIV binds to CD4 and also to a chemokine receptor. 00:31 We often use the term co-receptor for the chemokine receptor, it needs to bind to both. 00:37 Here we can see on the surface of a helper T-cell, the CD4 molecule and also the chemokine receptor, CXCR4. 00:47 And the HIV virus is binding to both of those receptors. 00:53 The same applies to macrophages that can become infected with HIV, but here the chemokine receptor that is utilized is different. 01:01 Instead of using CXCR4, the chemokine receptor CCR5 is employed as the co-receptor in addition to CD4. 01:18 So in HIV infection, there is depletion of CD4+ T-cells. 01:26 And this is due to a direct cytopathic effect of the virus, due to HIV gp120-mediated cytotoxicity, due to activation-induced apoptotic cell death of the infected cells, and also due to CD8+ T-cell killing of infected CD4+ cells due to recognition of peptide MHC Class I, with the peptides being derived from proteins in the HIV virus. 02:00 Here we have the HIV virus bound to the surface of a T-lymphocyte. 02:07 You really just need to focus on a couple of points on this slide, and they are illustrated here. 02:15 The gp120 molecule on the surface of a virus; remember, when you come across these kind of designations such as gp120, it means that it’s a glycoprotein, that’s what the gp stands for, and it has molecular weight of 120,000 Daltons. 02:31 That’s why it’s called gp120. 02:33 And gp120 is essential for the virus to bind to the surface of the cell that it’s going to infect. 02:40 And as we’ve already heard, the molecule CD4 plus a chemokine receptor are essential because the gp120 needs to bind to both of these receptors in order to infect the cell. 02:55 Virion binding to CD4 and the chemokine receptor will lead to infection of the cell. 03:03 There is fusion of the HIV membrane with the cell membrane, and entry of the viral genome into the cytoplasm of the cell that is being infected. 03:17 The enzyme reverse transcriptase mediates synthesis of proviral DNA. 03:24 Remember the HIV virus is a retrovirus, which is an RNA virus, so it needs to turn its RNA into DNA in order to replicate in the host cell. 03:35 There is integration of provirus into the cell genome, followed by cytokine activation of the cell, with transcription of HIV genome, transport of spliced and unspliced RNAs to the cytoplasm. 03:52 Followed by synthesis of the HIV proteins and assembly of virion core structure. 03:58 Expression of gp120 and gp41 on the cell surface occurs, with budding of the mature virion. 04:07 The acute phase of HIV infection involves death of memory CD4+ T-cells in mucosal tissues. 04:18 There is then dissemination of virus to lymph nodes, and the virus then becomes latent. 04:25 And during latency, there is low level replication of the virus in lymphoid tissues. 04:31 There is a slow progressive T-cell depletion over time. 04:36 And in the chronic phase, the ongoing activation of T-cells results in extensive death of CD4+ T-cells, resulting in profound immunodeficiency. 04:51 So here we can see the infection of mucosal tissues, the death of mucosal memory CD4 T-cells occurs, the virus is transported to the lymph nodes, and infection is established in lymphoid tissues such as the lymph nodes. 05:12 There is a spread of infection throughout the body with viremia. 05:16 There is a partial control of replication, as the immune response kicks in. 05:24 A stage of clinical latency is established with chronic infection, the virus is concentrated in lymphoid tissues, there is a low level of virus production. 05:36 But following other events such as other microbial infections, the production of cytokines and so forth, virus replication becomes increased. 05:47 And ultimately there is destruction of lymphoid tissue, and crucially a depletion of those all important CD4+ helper T-cells. 05:57 And once they are depleted below a certain level, the patient will go on and develop full blown AIDS.
About the Lecture
The lecture HIV Infection and HIV Life Cycle– Secondary Immunodeficiency Diseases by Peter Delves, PhD is from the course Immunodeficiency and Immune Deficiency Diseases. It contains the following chapters:
- HIV Infection
- HIV Structure
- HIV Life Cycle
- Progression of HIV Infection
Included Quiz Questions
Which of the following is a receptor for human immunodeficiency virus (HIV)?
- C-X-C motif chemokine receptor 4 (CXCR4)
- C-X-C motif chemokine receptor 3 (CXCR3)
- C-C motif chemokine receptor type 7 (CCR7)
- C-C motif chemokine receptor type 8 (CCR8)
- Cluster of differentiation 8 (CD8)
The human immunodeficiency virus (HIV) targets which of the following immune cells?
- CD4+ T cells, macrophages, dendritic cells
- CD4+ T cells, macrophages, natural killer cells
- CD4+ T cells, CD8+ T cells, natural killer cells
- CD8+ T cells, macrophages, dendritic cells
- CD8+ T cells, plasma cells, B cells
Depletion of CD4+ T cells is due to all of the following EXCEPT...?
- Enhanced phagocytosis by macrophages
- Direct cytopathic effects of HIV
- Gp120-mediated cytotoxicity
- Activation-induced cell death by apoptosis
- Killing by HIV-specific cytotoxic T cells
Which of the following properly depicts the progression of HIV infection?
- Acute phase, latency, profound immunodeficiency
- Latency, acute phase, profound immunodeficiency
- Acute phase, profound immunodeficiency, latent phase
- Low level replication, acute phase, profound immunodeficiency
- Latency, low level replication, acute phase
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |