Playlist
Show Playlist
Hide Playlist
Conjunctivitis: Introduction and Etiologies
-
Slides External Eye Diseases Conjunctivitis.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
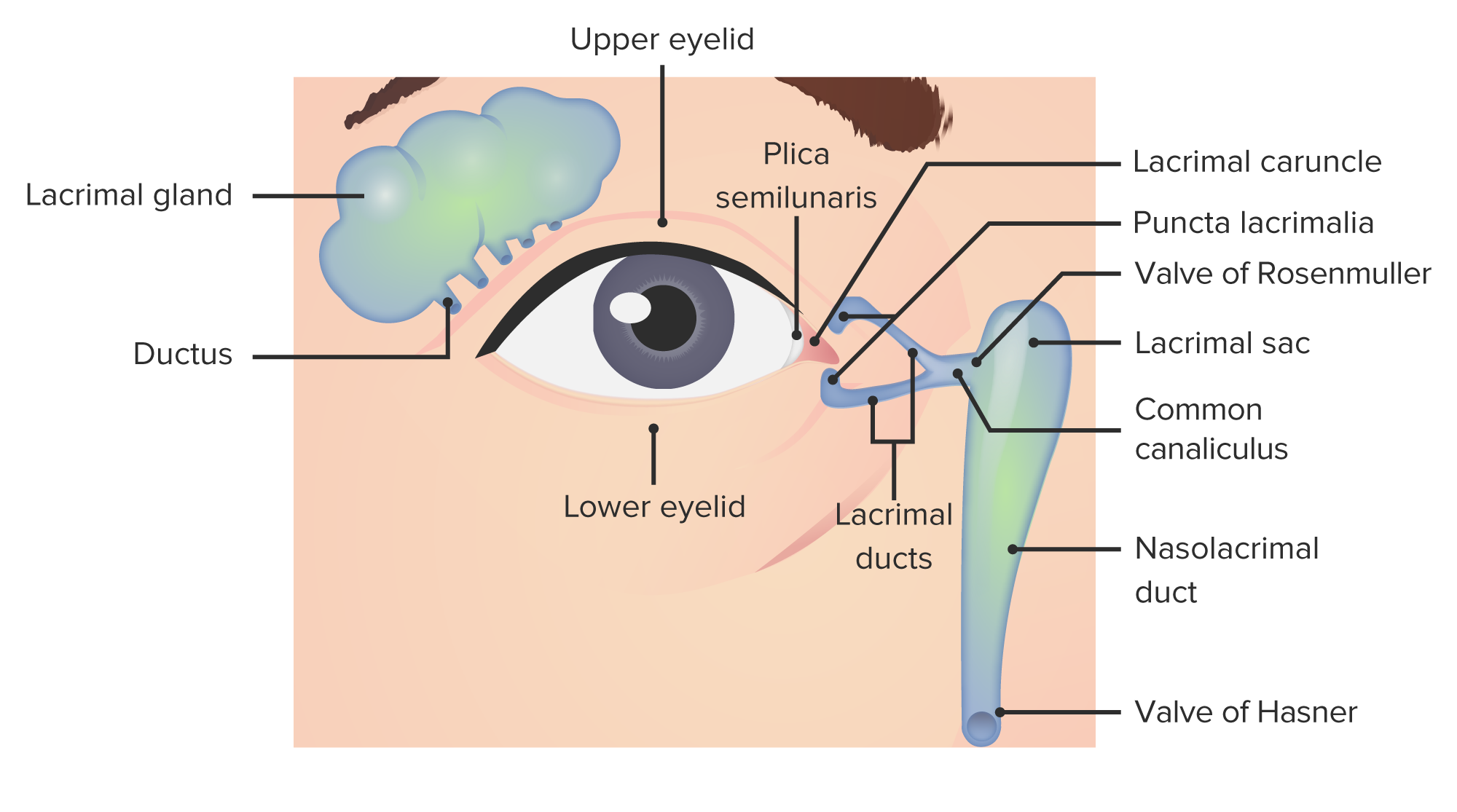
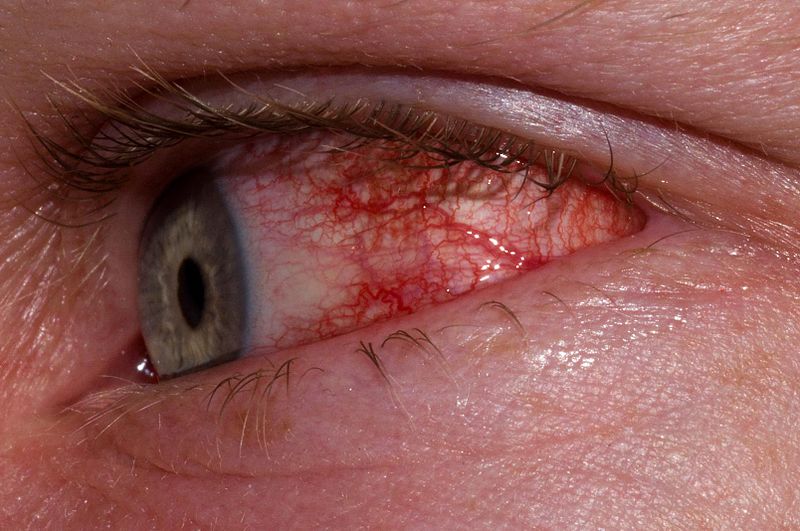
00:02 Welcome back. 00:04 Previously, we've talked about other inflammatory processes that involve other structures of the external eye. 00:11 We've talked about blepharitis, we've talked about hordeolums. 00:16 Today we're going to go one layer deeper and look at the conjunctiva. 00:20 We're going to look at inflammation of that, or conjunctivitis, more colloquially known as "pink eye". 00:28 As always, I want to acknowledge the help and the assistance in the great job that was done on this slide presentation of Dr. José Mata. 00:37 Let's talk about inflammation of the conjunctiva. 00:39 It overlies the sclera, and it's going to be that vasculature, that vascularized membrane that provides additional lubrication to the front of the eye. 00:48 Usually the vessels are not apparent and we normally have nice wide eyes, but when that gets inflamed, we'll have conjunctivitis And we'll continue that into our next session. 00:59 The conjunctiva has two components. 01:02 There is the bulbar conjunctiva that's associated with the eye orbit, with the eye itself and the palpebral conjunctiva that's on the inside of the eyelid. 01:11 And both of those can become inflamed. 01:14 And typically, when we do have conjunctivitis, both are involved. 01:18 So conjunctivitis or pink eye is inflammation of the conjunctiva. 01:22 Remember, conjunctiva is this highly vascularized membrane that sits over kind of the whites of the eye, over the sclera. 01:30 And this is going to be an important, highly vascularized membrane that will allow more fluid production or allow the transudation of fluid to help kind of keep the external part of the eye well liquefied, not liquefied, but well lubricated. 01:49 And you can have inflammation of this as you can have inflammation of almost anything. 01:54 And it can involve either the bulbar conjunctiva, which is what we see there over the whites of the eye or over the orbit of the eye, or it can involve the conjunctiva that sits on the inside of the eyelid or the palpebral conjunctiva. 02:08 Either one will work and frequently everything is involved. 02:14 Two kind of major flavors in terms of the cause of conjunctivitis. 02:18 So we can have a noninfectious conjunctivitis which will be non-allergic or allergic. 02:24 And clearly, if you have a noninfectious conjunctivitis, we must have an infectious one and that will be either bacterial or viral. 02:31 Okay, let's get into a little bit more detail. 02:34 Of the infectious causes, viruses are going to be quite common. 02:39 And of the viruses, adenovirus is going to be the vast majority of the causal organism. 02:45 These are quite diffusely out there in the environment. 02:50 And so 65%-90% of the conjunctivitis that's associated with virus is going to be an adenovirus. 02:57 And we're just seeing a couple eyes that are showing you the characteristic inflammation of the conjunctiva, again, inflammation of conjunctiva is no different than inflammation anywhere else. 03:07 This is vasodilation and increased vascular permeability with the recruitment of inflammatory cells. 03:14 It just seems to be happening here in the conjunctiva of the eye. 03:19 Okay, so that's most common cause. 03:22 The second one is herpes simplex virus, it's going to be more common in the pediatric population. 03:27 And then in the geriatric population, varicella zoster is going to be the most common virus. 03:33 So depending on the face in front of you, whether it's kind of a very young face, a very old face or the rest of the world, you can make an educated guess about which virus is likely to be causing this. 03:46 Because it's a viral infection, we are not bringing in many neutrophils. 03:50 It's going to be predominantly kept in check or eventually eliminated by actions of T-cells and some macrophages. 03:58 So it's going to be overall a sparse mucus discharge. 04:01 There will be inflammation that also extends up into the lacrimal gland in the lateral part of the eyes, as well as involving the lacrimal caruncle at the medial canthus. 04:13 In both of those cases, because of inflammation of that part of the apparatus, there will be increased lacrimation, there will be a tendency to have tearing. 04:22 Important part about viral etiologies for conjunctivitis is that they are mostly self-resolving. 04:28 We try to prevent a secondary bacterial infection but usually, given enough time and an intact immune system, we can eventually make them go away. 04:39 Bacteria, on the other hand, are going to need a little bit of help. 04:42 So the most common bacterial cause of conjunctivitis is Staph aureus, very common skin pathogen, and it's also going to be very common around the orbit of the eye. 04:53 And if it gets into the conjunctiva, it can wreak a significant amount of damage. 05:03 In kids, the most common is probably Haemophilus influenzae. 05:08 In the newborn population, it's Neisseria, and we actually even administer eyedrops in many neonatal situations to prevent the spread or the bacterial expression of the Neisseria in the eye. 05:25 In developing countries, it'll be Chlamydia trachomatis So, again, kind of depending on who's staring back at you and, and or whether you're in a developing country or in an industrialized country, you can make an educated guess about the infectious agent. 05:44 You're going to know that it's bacteria because of the presence of pus. 05:47 so because now this is a bacterial infection, we are recruiting neutrophils. 05:52 And neutrophils are going to have a characteristic yellow kind of color, and there will be much more of an exudate. 06:01 We're going to need to... 06:02 When we recognize that pus, we're going to need to treat with antibiotics because that sort of bacterial infection is unlikely to spontaneously resolve. 06:12 Those are the infectious causes. 06:13 On the other side of the equation are the non-infectious causes, and you can have allergic or non-allergic. 06:18 Of the non-allergic, these are autoimmune diseases. 06:21 Dry eye syndrome or sicca syndrome and Sjogren syndrome involve inflammation, autoimmune-derived or driven inflammation of either the conjunctiva proper or of the lacrimal system. 06:35 And so we can have an immune-based response that isn't driven by extrinsic allergens. 06:42 On the other hand, allergic conjunctivitis is due to airborne allergens. 06:47 and because we're getting mast cell degranulation, and a variety of other things, that's how we're getting the inflammation. 06:53 And obviously it's going to be bilateral.
About the Lecture
The lecture Conjunctivitis: Introduction and Etiologies by Richard Mitchell, MD, PhD is from the course External Eye Diseases.
Included Quiz Questions
What is the common name for conjunctivitis?
- Pink or red eye
- Brown eye
- Yellow eye
- Gray eye
- Blue eye
What structure lies underneath the conjunctiva?
- Sclera
- Cornea
- Tarsus
- Choroid
- Iris
What organism most commonly causes viral conjunctivitis?
- Adenovirus
- Varicella-zoster
- Herpes simplex
- Retrovirus
- HPV
What organism is associated with conjunctivitis in newborns in developed countries?
- Neisseria
- Staphylococcus
- Chlamydia
- Treponema
- Streptococcus
What syndrome is usually associated with noninfectious conjunctivitis?
- Sjogren's syndrome
- Horner's syndrome
- Down syndrome
- Heerfordt syndrome
- Turner's syndrome
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Dr.Mitchell is very good at teaching. his hand gestures capture my attention as he speaks and keeps me actively listening. the visuals repressenting the eye stractures are also very pleaseant to see