Playlist
Show Playlist
Hide Playlist
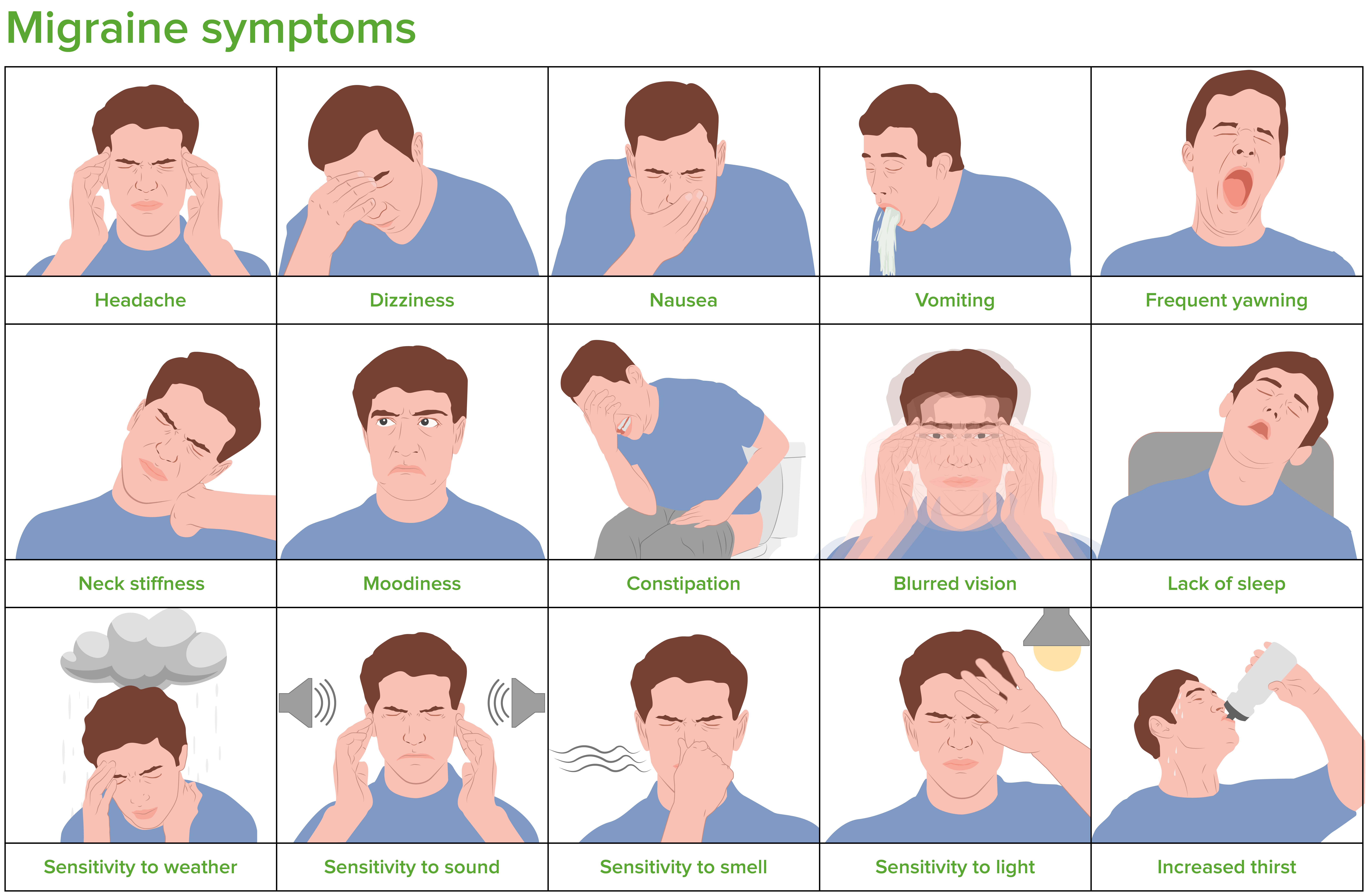
Case: Just Another Migraine?
-
Slides ApproachtoAcuteProblems AcuteCare.pdf
-
Download Lecture Overview
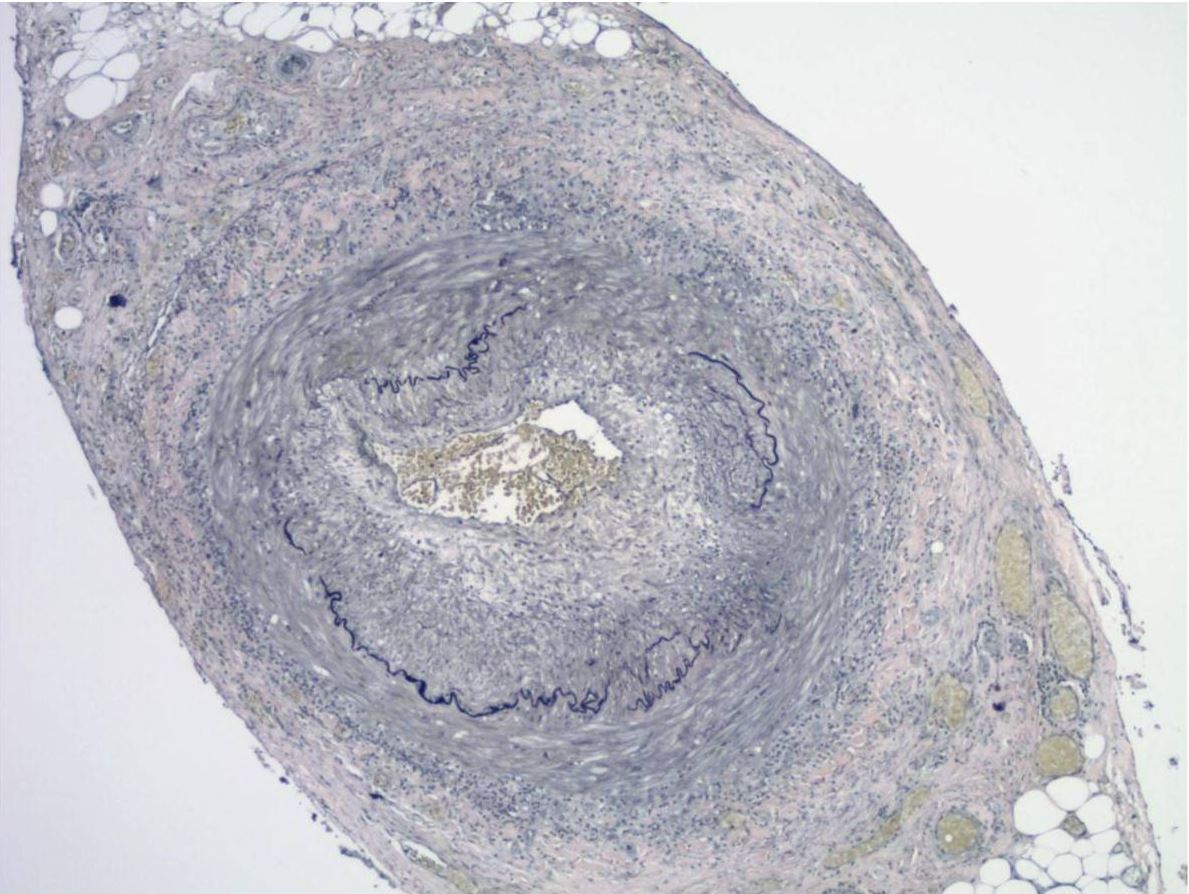
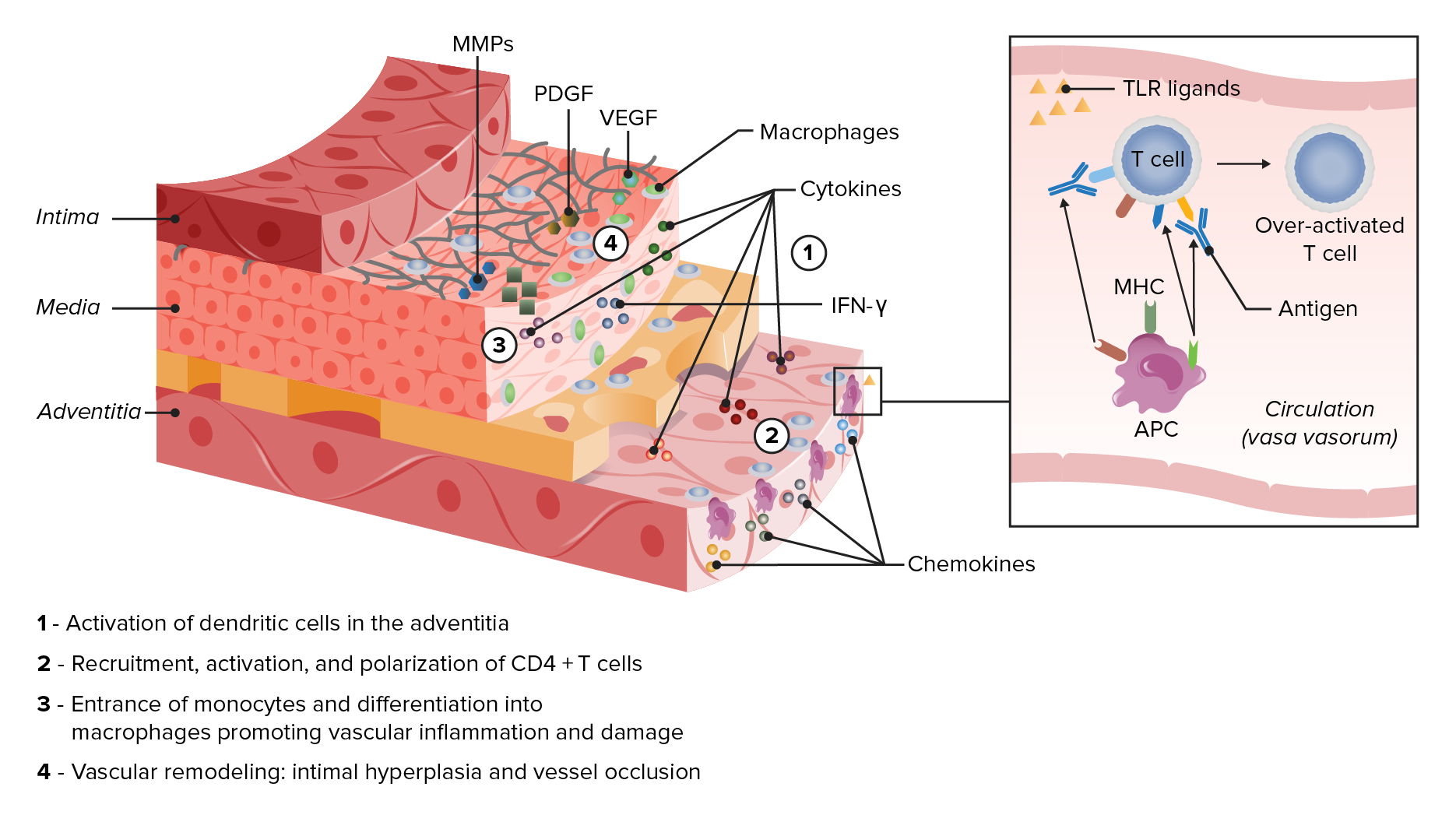
00:01 Okay, last case. 00:03 So, we’ve got an older patient here. 00:05 I’ve got a 75-year-old woman. 00:06 She has a one-day history of headache. 00:08 Well, it’s just one of my migraines, she explains. 00:11 Sounds pretty benign. 00:12 Let’s get a little bit more. 00:15 So, she has a long history of unilateral migraine headaches, which previously resolved with just a high-dose non-steroidal anti-inflammatory drugs. 00:24 However, the character of this pain is different. 00:26 It’s very concentrated over her temple specifically and it's actually tender to palpation there. 00:34 So, just with that limited history alone, what's the next best step in the management for this patient? And again, you could pause and think about this for a second. 00:44 So, is it, A, just change the type of NSAID she is taking? Maybe that will make a difference. 00:49 Just reassurance. 00:50 She's right, it’s probably just a recurrent migraine and just continue with that expectant management that’s been working for a while. 00:56 Do you initiate maybe a new drug, like a triptane instead of giving her an NSAID? Maybe that’ll be more effective for a migraine headache? Or, D, do we send her to the laboratory immediately and we also initiate corticosteroids? So, this one is to throw you off. 01:11 Indeed, not every case of acute management just needs reassurance and it will probably resolve with time because this is unusual. 01:21 New headaches and different types of headaches always should raise attention for potential red flags. 01:27 In this case, you're seeing unilateral temporal-based pain in a 75-year-old woman with the area actually tender to palpation. 01:35 All of that is very concerning for the diagnosis of…temporal arteritis. 01:41 Very good. 01:42 So, temporal arteritis can have severe complications, particularly in terms of risk of thrombosis and ischemia immediately, so she could lose her vision, she can have a stroke. 01:54 Therefore, immediate laboratory evaluation for simple things like a Sed rate and a CBC for the potential for temporal arteritis and she should not leave your clinic without a prescription for corticosteroids because the application of corticosteroids can dramatically reduce that risk of complication. 02:12 So, she’ll need close follow-up and an initiation of treatment right away. 02:17 So, this is just an example, but I thought it was a keen example to give you an idea that not every case can be managed just with expectant management and reassurance. 02:27 But, certainly, I think for USMLE exam and the way I think about patient care, the answer many times, it's not every answer, and so the trick for you is to watch for high-risk conditions. 02:38 Now, what do those conditions include? I think headache is a high-risk condition. 02:43 So, always pay attention to it. 02:44 Chest pain, while it’s usually benign, still a high-risk condition. 02:48 New neurological symptoms. 02:50 This isn’t the patient with diabetes for 20 years, who has bilateral tingling in the feet, but I’m talking about somebody who has monocular blindness or a left facial droop, something new going on that's acute. 03:05 Think about stroke, you think about masses or other severe CNS disorders. 03:11 Or – and these are often found incidentally – new lesions or masses in organs such as the skin or the breasts. 03:17 I’ve got this mole and, yeah, it seems to be growing and changing. 03:20 Then it bleeds and falls off and then it comes back again. 03:23 The first thing I'm worried about is cancer. 03:25 Now, that's – is it going to be cancer? Unlikely. 03:29 But the first thing I'm going to worry about is cancer. 03:32 And anytime somebody comes in with a – I feel a new mass in my breast, particularly if they’re over 50 and particularly if they are higher risk for breast cancer because of a family history or something like that. 03:43 These are the high-risk conditions just to name a few. 03:46 But some of the more common ones that we see should alert you to the fact that you might need to really go and perform a more thorough workup here. 03:55 You may need to order advanced therapy for this patient right from the get-go, not everything can just be a wait-and-see approach. 04:02 So, hopefully, you found these cases beneficial. 04:05 Now, we’ll move into the acute care module and you can see how this plays out with some real cases. 04:10 Thank you.
About the Lecture
The lecture Case: Just Another Migraine? by Charles Vega, MD is from the course Acute Care.
Included Quiz Questions
What is NOT a high-risk presentation in primary care?
- Abdominal pain
- Headache
- Chest pain
- New neurologic symptoms
- New breast lesion
What is a high-risk presentation in primary care?
- New neurologic symptom
- Leg pain
- Muscle soreness
- Fatigue
- Congestion
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |