Playlist
Show Playlist
Hide Playlist
B-Cell Development in the Bone Marrow – Lymphocyte Development
-
19 Slides B-Cell Development in the Bone Marrow.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
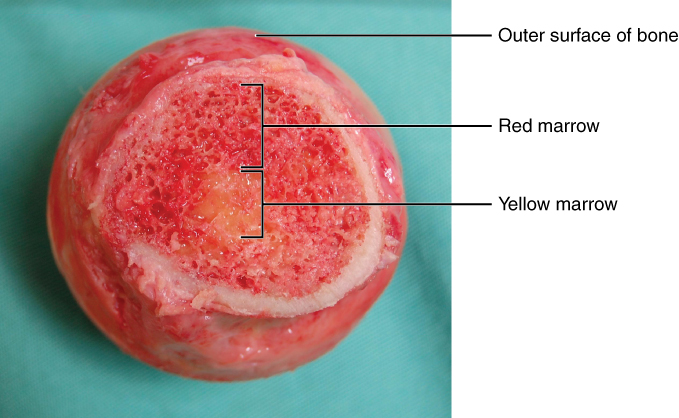
00:01 So, B cells, as their name suggests B developed in the bone marrow. 00:09 So the bone marrow is where B cells develop. 00:11 And in fact, virtually all the cells of the immune system start off from multipotent hematopoietic stem cells in the bone marrow. 00:22 So let's have a look at how B cell development in the bone marrow occurs and the stages in B cell maturation in the bone marrow. 00:32 I've already mentioned they start off from hematopoietic stem cells. 00:37 These develop into pro-B cells, those hematopoietic stem cells that instead of becoming a mast cell line, instead of becoming a dendritic cell, those that are going to become B cells initially become Pro-B cells. 00:53 The next stage in their development is to become a Pre-B cell. 01:00 Then they develop into immature B cells, and of course, eventually into mature B cells. 01:07 There are two stages in this development process where these B cells undergo very, very extensive cell division in other words proliferation. 01:16 That's at a very early stage in their maturation at the stem cell, pro-B cell stage. 01:22 And then later on at the pre-B, Immature B cell stage, they undergo further massive rounds of proliferation. 01:30 They dividing all the time. 01:31 But these two stages in their development are characterized by particularly extensive cell proliferation. 01:41 There are two genes that are called RAG1 and RAG2. 01:45 Stands for Recombination Activating Genes. 01:49 Already mentioned that the immunoglobulin genes in the B cell undergo recombination to create diversity. 01:58 These recombination activating genes, obviously play a role and that as the name suggests. 02:03 And these genes are also expressed two different points in the development and maturation of B cells that the Pro-B, Pre-B stage, and then they can become reexpressed later on in immature B cells to fine tune the antigen receptor on the B cell. 02:24 There's another molecule which we'll hear about shortly called TdT, Terminal deoxynucleotidyl transferase Bit of a mouthful that isn't it? We normally just refer to this TdT because terminal deoxynucleotidyl transferase, it's quite long word to say, so TdT. 02:44 And that's expressed again, at the stage between pro-B cells and pre-B cells. 02:51 If we look at the immunoglobulin gene DNA in the B cell, and the RNA that's producing that DNA in the stem cell stage, and the pro B cell stage, these immunoglobulin genes are what we call in the germline configuration. 03:12 That means how these genes are inherited through the sperm and the egg, the germline, and every single cell in the body will have this DNA just like you have genes for all the different genes you have in all the different cells. 03:26 And in all the cells in the body, they will be in the germline, orientation or configuration. 03:32 And it's only once cells developed to become B cells that these immunoglobulin genes recombine. 03:42 And this recombination initially starts off at the Pre-B cell stage, and some segments within the heavy chain genes for the immunoglobulins. 03:53 Because immunoglobulins consists of a heavy chain, and a light chain. 03:57 The first event that says, "Hmm, that cell is going to become a B cell." is when the B cell recombines its heavy chain genes. 04:08 And it recombines three gene segments as we'll see shortly, they're called V, D, and J Variable, Diversity, and Joining. 04:18 Once that the combination processes occurred in the pre-B cell, messenger RNA is produced for the heavy chain and that includes a segment that is from the constant region called mu. 04:34 So you get mu mRNA in the pre-B cell, As that cell then develops to the final stage, before full maturity, in other words, the immature B cell, the recombined heavy chain gene, associates the product of that gene associates with the product of a recombined light changing Then the light chains, the V gene segments and J gene segments that recombine, produce a light chain protein. 05:11 So now we have Ig for the DNA that's recombined in the heavy chain and the light chain, we have a mu heavy chain protein, and either a kappa or lambda light chain protein produced from the capital lambda messenger RNA. 05:30 And then finally, we end up via alternative splicing of the V, D, and J with a constant region of the IgM antibody which is encoded by a Cmu gene or the IgD antibody encoded by a C Delta gene. 05:52 So the stage of maturation early on the immunoglobulin genes are notly combined, so there's no expression in order to express these genes, they need to be recombined, they only recombine in B cells, and they only recombine at the pre-B cell stage. 06:10 So you start off at the pre-B cell stage with the first indication that this cell is going to become a B cell. 06:17 It has cytoplasmic mu heavy chain. 06:20 And on the surface, it has what is called the Pre-B cell receptor, which is a surrogate light chain. 06:27 It's not the proper light chain, but it's a sort of intermediate light chain that's produced to put together with the mu heavy chain. 06:34 And then once the light chain genes have been recombined, you get the full mature antibody molecule on the surface of this immature B cell. 06:44 So it's a mature antibody, but it's on the surface of an immature B cell, and this is membrane IgM. 06:52 And then, as well as IgM, another class of antibody, the IgD class is put on the surface of the mature B cell. 07:03 As well as having antibodies on their cell surface B cells have thousands of other molecules on their cell surface just like every cell does. 07:10 And we can use certain molecules on the surface of B cells to identify which stage in maturation they are. 07:18 So for example, the molecule CD34 is present on the surface of the stem cells. 07:25 It's also present on the surface of the pro-B cell. 07:29 But additional molecules become expressed such as CD19, and CD10. 07:35 And then, as those pro-B cells develop into pre-B cells, there is low expression of a molecule called B220. 07:45 But as that pre-B cell develops into an immature B cell, the expression of CD34 is lost. 07:52 So if a cell has a molecule on its surface, we describe it as a CD, whatever positive cell, if it doesn't have expression, we describe it as a CD, whatever negative cell. 08:04 So in other words, the stem cells, the Pro-B cells, and the pre-B cells are CD34 positive, whereas the immature B cell is CD34 negative. 08:16 At that stage, of the immature B cell there is a low level expression of IgM antibodies on the surface of the B cell. 08:24 And then as the B cell further matures to become a fully mature B cell, the level of expression of IgM increases. 08:33 So, where are these different types of B cell these different stages of maturation found? Well, the stem cells, the pro-B cells, the pre-B cells are all within the bone marrow. 08:44 And then as these cells develop into immature B cells, they can leave the bone marrow and enter what immunologists refer to as the periphery rather strange term that the periphery simply means anywhere outside of the primary lymphoid tissues. 09:01 So anywhere in the body that isn't the bone marrow or the thymus, immunologists refer to as the periphery. 09:07 And the mature B cells are found in the periphery or move to the periphery. 09:14 The response to antigen clearly, if the B cell doesn't have an antigen receptor on the surface, it can't respond it, it has no way of responding to antigen. 09:22 So because there is no surface antibody on stem cells, pro-B cells, or pre-B cells, there's no response to antigen. 09:31 At the immature B cell stage when there is low level expression of IgM. 09:36 the B cells can undergo what is called negative selection or deletion. 09:41 And this refers to the fact that if those B cells encounter molecules from our own body, what we call self antigen, then they become deleted because we don't want B cells that can attack our own body components. 09:55 We want B cells that can fight infection coming from outside the body. 09:59 So they'll be deletion of B cells that recognize self antigen, and there can be receptor editing. 10:05 And this is why RAG1 and RAG2 get reexpressed at this stage so that the receptor can be changed. 10:11 If it reacts itself, it can be changed to a different receptor that reacts with a foreign pathogen rather than reacting itself. 10:19 And then, once they're mature, of course the B cells are fully able to respond to antigen I mean, that's how it should be obviously, you need the B cells to be able to respond And they can become activated, they can proliferate, divide up in number, and they can differentiate and become specialized, particularly become specialized to produce a progeny of a B cell that is called a plasma cell. 10:42 And what plasma cells do is they secrete very large amounts of antibody of the same specificity that acts as the B cell receptor on the surface of the B cell. 10:53 So in the bone marrow, we have these pre-B cells, this early stage of development, and they have on their cell surface, not a mature form of the antibody molecule, but a preliminary version, if you like the antibody molecule, where you have the normal version of the IgM heavy chain, which is called mu heavy chain. 11:17 But it's not a mature version of the light chain. 11:20 They have what we refer to as a surrogate light chain, and this is made up of two components. 11:24 One is called V pre-B, and the other is called lambda 5. 11:30 And then as the pre-B cell matures into an immature B cell, it swaps the surrogate light chain for a proper, a real light chain, and that can either be the kappa light chain, or the lambda light chain. 11:46 So the mature B cell now has on its cell surface, a proper mature version of the antibody molecule. 11:55 And initially, these mature B cells that have not yet encountered antigen we call them naive B cells. 12:02 They're not yet met antigen at all. 12:04 They express on their cell surface two different classes of antibody IgM, surface IgM, and surface IgD. 12:14 And these cells have left the bone marrow and travel to the secondary lymphoid tissue. 12:20 And they sit in wait in the secondary lymphoid tissue in case their particular antigen the antigen they recognize comes along.
About the Lecture
The lecture B-Cell Development in the Bone Marrow – Lymphocyte Development by Peter Delves, PhD is from the course Adaptive Immune System. It contains the following chapters:
- B-Cell Development in the Bone Marrow
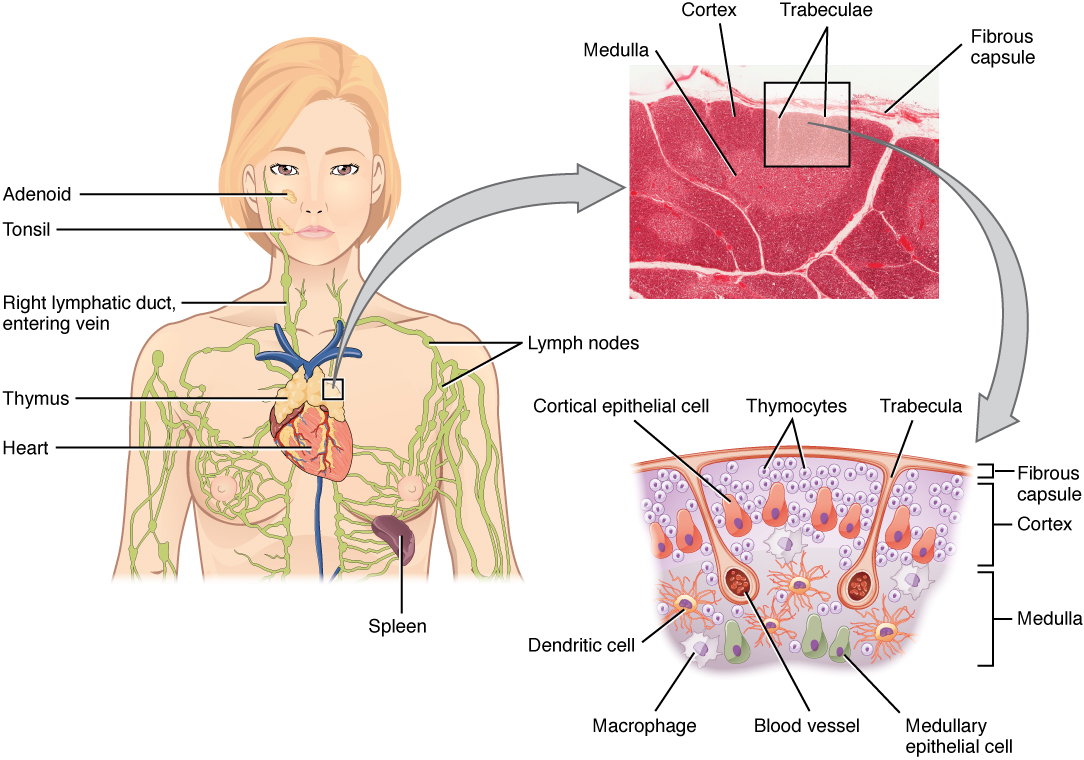
- Anatomic Site of the B-Cell Development
Included Quiz Questions
What is one of the components of the surrogate light chain on a pre-B cell?
- λ5
- λ
- κ
- μ
- κ3
Expression of recombination activating genes (RAG) mainly occurs in which stages of B-cell development?
- Pro-B, pre-B, Immature B
- Stem cell and pro-B
- Pre-B and mature B
- Immature B and mature B
- Mature B
Which immunoglobulin chains join to form the membrane IgM, expressed on the surface of the immature B cell?
- Two μ heavy chains and two λ light chains
- Two λ light chains
- κ and λ light chains
- Two κ light chains
- Two μ heavy chains
Which of the following correctly represents the recombination complex of heavy chains and light chains, respectively?
- VDJ and VJ
- VDJ and VDJ
- VJ and VDJ
- VJ and VJ
Which of the following stages of the B-cell development in the bone marrow are CD34 deficient?
- Immature and mature B cells
- Stem cell and pro-B cells
- Stem cell and pre-B cells
- Pro-B cells and immature B cells
- Pro-B cells and mature B cells
Which of the following stages in the process of B-cell development occur in the bone marrow and periphery, respectively?
- Pro-B cell formation, plasma cell formation
- Pre-B cell formation, pre-B cell formation
- Immature B cell formation, pre-B cell formation
- Plasma cell formation, mature B cell formation
- Mature B cell formation, plasma cell formation
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Simple and easy to understand. Thanks Professor Peter for explaining the concepts well and clear.
Very good slides and explanation in this important and beautiful chapter of immunology