Playlist
Show Playlist
Hide Playlist
Acute and Chronic Diabetes Complications
-
Slides AcuteChronicDiabetesComplications EndocrinePathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
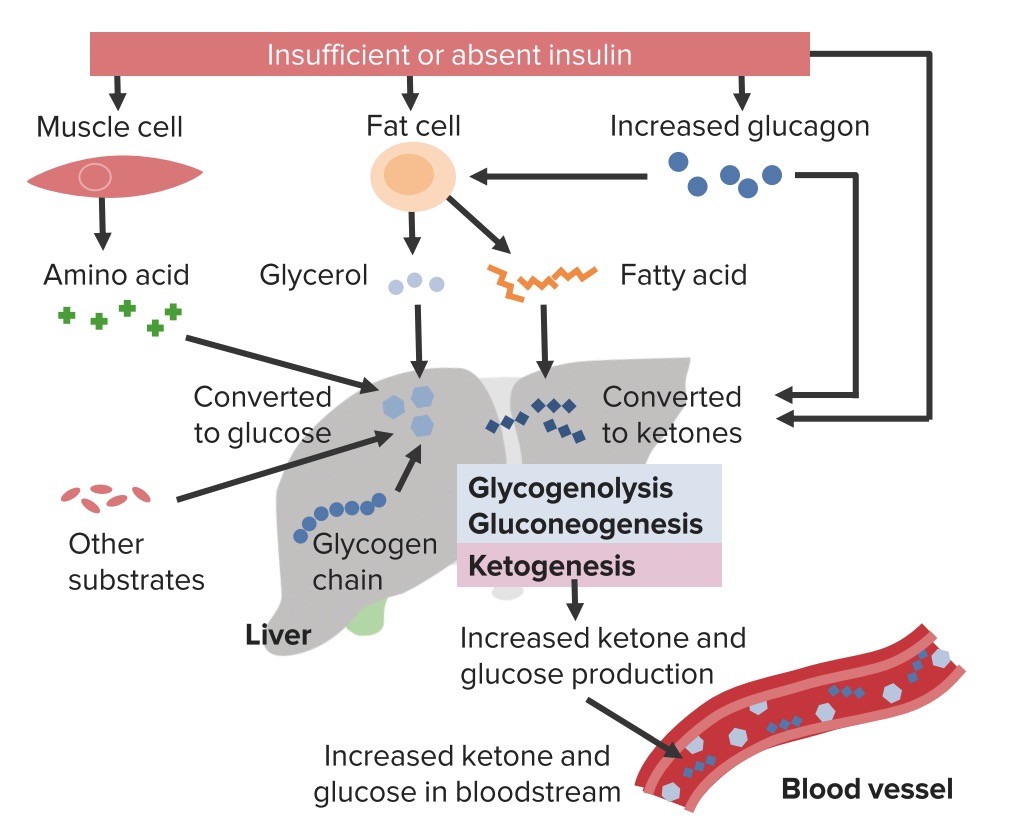
00:00 Now that we established the definition of hyperglycemia and all the differentials we’ve looked at, let us now take a look at complications specifically for type I and type II diabetes. 00:14 We will organize our complications initially with acute and chronic and as we move forward, we will then take a look at some of these issues and complications in much greater detail. 00:26 With acute complication type I diabetes, if not controlled properly, the patient maybe in a state of ketoacidosis. 00:36 Remember that this would be an endogenous production of keto acids, therefore would be referred to as being or experiencing metabolic acidosis with an anion gap, which we shall refer to. 00:50 Type II diabetes mellitus, if untreated, complications here acutely rarely would it be diabetic ketoacidosis, but it would be hyperosmolar, hyperglycemic state or sometimes worst case scenario hyperosmolar, hyperglycemic type of coma, but it would be non-ketotic. 01:12 The reason in type II diabetes to be non-ketotic is because there might be residual amounts of insulin and just enough insulin and make sure that your biochemistry is strong here, that if you have just enough insulin that you may not be forced to break down your lipid and have beta oxidation taking place. 01:32 So, therefore, the hyperosmolar is being caused by the hyperglycaemia in type II diabetes if it’s uncontrollable. 01:42 Remember all these mellitus and now that we’re doing medicine, let’s be a little bit more technical versus insipidus. 01:48 Remember that in insipidus, you will have and mellitus, you would have both polydipsia and polyuria. 01:57 However, in insipidus, you would not have polyphagia. 02:02 Our focus beyond acute is chronic complications. 02:09 The chronic complications would be quite similar for both type I and type II diabetes mellitus if left untreated or poorly controlled. 02:18 If it’s type I diabetes, then the complications chronically would be accelerated only because remember the glycemic control in type I, if uncontrolled, can be quite variable. 02:32 Whereas in type II diabetes mellitus, the one that we see quite a bit is chronic complications and here refer to decades; the microvascular diseases you may then end up having diabetic retinopathy, diabetic nephropathy and diabetic neuropathy and we call this stock and glove The macrovascular disease will be coronary arterial disease, peripheral vascular disease or stroke being caused by what’s known as atherosclerosis in your arteries and referred to cerebrovascular accident or cerebrovascular disease. 03:09 Now, keep in mind that you want to know in great detail what kind of complications are taking place within these blood vessels. 03:17 So, therefore, if it’s macrovascular, you are referring to arterial or arteriole thus more commonly you would find atherosclerosis. 03:27 If you’re referring to microvascular, then you are referring to arterioles. 03:34 Would you please tell me what kind of... what sort of arteriolosclerosis will be taking place within arterioles in diabetes? It would be hyaline arteriolosclerosis. 03:48 Lastly, just to make sure that we are completely comfortable with our complications within our blood vessel, more commonly within your capillaries with the pathogenesis causing damage to your capillary and that was our discussion earlier with non-enzymatic glycosylation. 04:07 Make sure that those sets of blood vessels are well organized in your head before we move on otherwise you’re confusing all of the complications that are taking place on a vascular level.
About the Lecture
The lecture Acute and Chronic Diabetes Complications by Carlo Raj, MD is from the course Pancreatic Disease and Diabetes.
Included Quiz Questions
Why doesn't hyperosmolar hyperglycemic state progress to diabetic ketoacidosis (DKA)?
- Lack of production of ketone bodies
- Increased acidosis
- Decreased insulin
- Lack of production of insulin
- Reduced anion gap
What is NOT a microvascular complication of diabetes mellitus?
- Cerebrovascular disease
- Neuropathy of the entire hand
- Retinopathy
- Nephropathy
- Neuropathy of the entire foot
Which statement about vasculature damage and pathogenesis is CORRECT?
- Microvascular - hyaline arteriolosclerosis
- Medium-large vessel - hyaline arteriolosclerosis
- Microvascular - atherosclerosis
- Macrovascular - non-enzymatic glycosylation
- Microvascular - sorbitol depletion
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |