Playlist
Show Playlist
Hide Playlist
Hypersensitivity: Type 1 – Causes
-
Slides Hypersensitivity.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
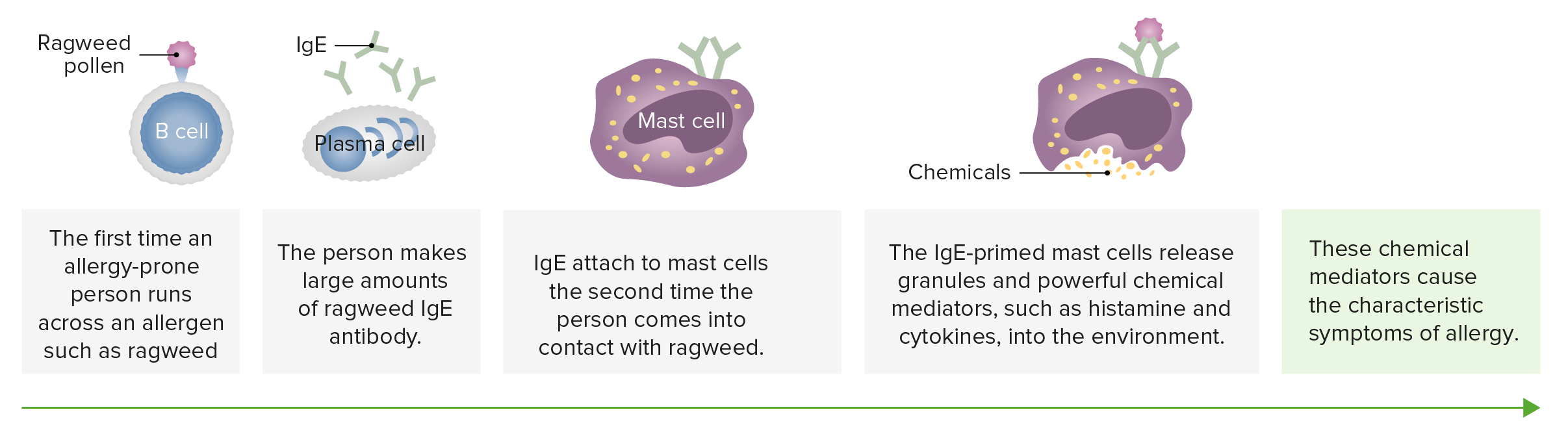
00:01 Right, now having given you a little overview of those four different types, let’s now look in a bit more detail at each one. So Type I hypersensitivity - IgE-mediated mast cell degranulation. 00:15 You’ve already seen this picture. 00:17 So these Type I hypersensitivity reactions, IgE-mediated mast cell degranulation. 00:22 That’s what we usually think of as allergic types of responses, allergy. 00:27 And this type of response often referred to as atopy, an inappropriate production of IgE antibodies is caused by a multitude of different factors. 00:38 Genetics is important, but other factors also are important. 00:43 Regarding the genes, there is not a single dominant allergy gene; it’s rather that several genes contribute to the development of the allergic process. 00:54 Amongst them, the gene encoding the FcεR1, the gene encoding the cytokine interleukin-4 which is very important in causing B-cells to class switch to IgE production, CD14, HLA-DR, there are a number of different genes. 01:11 So it’s really the combination of genes that’s important, not any one single specific gene. 01:17 And of course the environment is also very important, it’s not a purely genetic situation we have here. 01:23 And early microbial exposure, and early allergen exposure perhaps in the uterus seem to play an important role. 01:31 Immune responsiveness overall is abnormal, with a decreased production of gamma interferon, and perhaps overall a more Th2 type of environment with those Th2 cells that secrete cytokines such as interleukin-4 and interleukin-5 and interleukin-6. They’re the more dominant population. 01:53 And remember, all of these responses are normal responses. 01:56 So a Type I hypersensitivity reaction is based upon something that is a normal protective immune response. 02:01 For example against a parasitic worm infection. 02:04 If you have a parasitic worm infection in your gut for example, you’d be very grateful to having this sort of response because it would help expel the worms from the gut. 02:15 However in a substantial minority of individuals, IgE-mediated mast cell degranulation occurs in response to what should be a harmless environmental antigen. 02:25 And afterall, grass pollen is not going to cause you any harm, but in a significant number of people, there’s a response to this that actually leads to pathology. 02:34 Maybe you yourself suffer from allergies. 02:36 You’ll certainly know people that do, because it’s a very common affliction of people to suffer from these allergic reactions. 02:45 In Type I hypersensitivity, there’s an immediate IgE response, but this resolves within around about an hour. 02:55 However it is frequently followed by what is referred to as the late phase reaction. 03:01 This occurs around about 4-12 hours later. 03:03 And it involves CD4+ helper T-cells, monocytes and eosinophils becoming activated. 03:14 So there are a number of different types of atopic allergy, that is allergy caused by excessive production of IgE. 03:22 Rhinoconjunctivitis which you may know as hay fever, affects around about 20-35% of individuals. 03:30 Asthma affects around about 10-20% of individuals, atopic eczema again around about 20% of individuals, urticaria similar kinds of numbers, food allergy maybe around about 3-5% of individuals develop food allergy, and insect venom hypersensitivity in about one in a hundred people. 03:57 We use the term anaphylaxis to describe a severe systemic hypersensitivity to allergen in an injection, a sting or by epithelial exposure, for example in the gut mucosa. 04:13 It involves a rapid vasodilation which leads to a substantial drop in blood pressure. 04:21 There is constriction of the airways, edema and anaphylactic shock can result that is often fatal. 04:32 However, immediate administration of epinephrine can reverse the bronchoconstriction and vasodilation and rescue the patient. 04:45 Let’s have a look at some of the mediators that mast cells produce that contribute towards the inflammatory process. 04:53 We can divide these mediators into two groups. 04:56 Ones that have already been made by the mast cell and are stored within granules within the mast cell. 05:03 And then newly synthesized mediators that are made from arachidonic acid. 05:10 Histamine is the classical mast cell inflammatory mediator. 05:14 It causes smooth muscle contraction and an increase in vascular permeability. 05:20 Heparin is produced and stored in granules, and this is an anticoagulant. 05:26 And eosinophil chemotactic factor is a third example of a pre-made mediator stored in the granules, and this as its name suggests mediates eosinophil chemotaxis. 05:39 So all these substances are ready to go, and the second the mast cell degranulates, they can mediate their effects. 05:46 Regarding the newly synthesized mediators, prostaglandin D2, prostaglandin E2 and prostaglandin F2α can mediate smooth muscle contraction and increase vascular permeability just like histamine. 06:01 Leukotriene B4 is a chemotactic factor for neutrophils. 06:08 And leukotriene C4, D4 and E4 cause smooth muscle contraction and vascular permeability again just like the prostaglandins and the histamine. 06:19 Let’s look at how the leukotrienes and prostaglandins are synthesized. 06:25 They are both produced from phospholipids, by the use of phospholipase A2 to generate arachidonic acid. 06:34 Then either via the lipoxygenase pathway which produces leukotrienes or via the cyclooxygenase pathway involving COX1 and COX2 which produces prostaglandins, these mediators are generated within the mast cell. 06:56 This is a list of allergens. 06:59 You’ll be very familiar with many of these I am sure. 07:02 So they include things like pollens, things associated with animals like animal dander, house dust mites and so forth, molds, various chemicals, and a number of food allergens.
About the Lecture
The lecture Hypersensitivity: Type 1 – Causes by Peter Delves, PhD is from the course Hypersensitivity and Autoimmune Disease. It contains the following chapters:
- A Closer Look on Type I Hypersensitivity
- Anaphylaxis
- Mast Cell Mediators
- Synthesis of Leukotrienes and Prostaglandins
Included Quiz Questions
Which of the following statements regarding atopy/allergy is most accurate?
- It is mainly a type 1 hypersensitivity reaction.
- A single gene mutation is involved.
- The risk is increased with early microbial exposure.
- In utero exposure to allergens is not associated with the condition.
Which of the following regarding the phases of type I hypersensitivity reaction is most accurate?
- Immediate phase reaction is IgE mediated.
- Late phase reaction is IgE mediated.
- Late phase reaction mainly involves cytotoxic T cells.
- Immediate phase reaction mainly involves helper T cells.
- There is no late phase reaction in type I hypersensitivity reaction.
Which of the following statements regarding anaphylaxis is most accurate?
- It is a serious hypersensitivity reaction that is rapid in onset and may cause death.
- Severe vasoconstriction is often seen.
- The airways are not affected.
- Immediate epinephrine administration could worsen vasodilation.
- Edema is not observed.
Inhibition of cyclooxygenase (COX) reduces the production of which of the following mediators?
- Prostaglandins
- Leukotrienes
- Phospholipids
- Lipoxygenase
- Arachidonic Acid
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
3 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
clearly explained ,great way to understand the mechanism, body language is really effective
Very understandable and practical! Dr. Delves is able to convey all the important info easily enough.
Best lecture on immunology .thanks sir for it.l am glad and confident.