Playlist
Show Playlist
Hide Playlist
Red Eye and Orbital Trauma
-
Slides The Red Eye.pdf
-
Download Lecture Overview
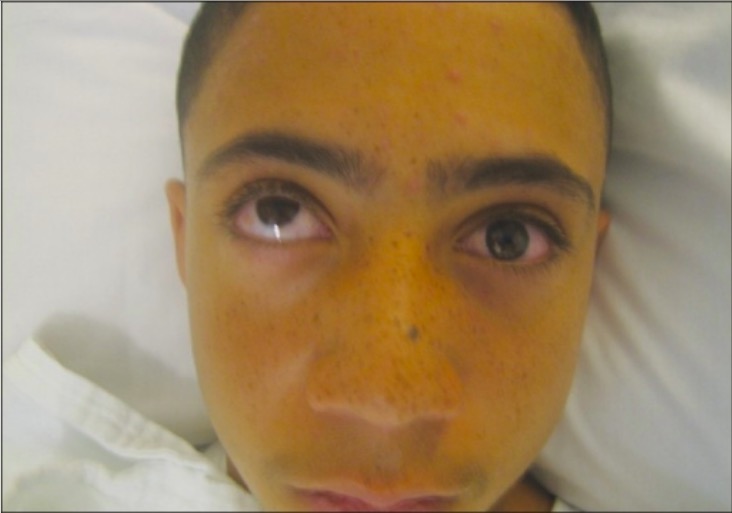
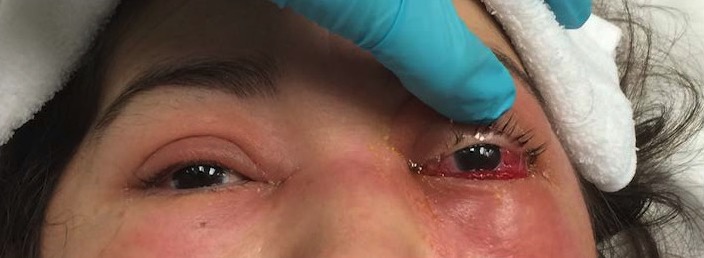
00:01 In this lecture, we’ll review the red eye in children and orbital trauma. 00:06 So let’s start with some infections. 00:08 Blepharitis is an inflammation of the eyelid margin that is due to infection. 00:13 This in turn can result in styes which include the hordeolum which is acute and the chalazion which is chronic. 00:22 So antibiotics are really only needed in these sorts of things if it spreads and becomes are preseptal cellulitis, which is quite rare. 00:30 In general, we can treat these with warm compresses until resolution. 00:34 We recommend about 10 minutes four times a day of warm compresses. 00:40 So the next potential complication, which is actually fairly common in infants, is the blocked tear duct which can result in dacryocystitis. 00:49 This is an infection and inflammation of the nasolacrimal duct. 00:53 If you recall, tears are generated laterally. 00:55 They sweep across the eye and then they drain down in the nasolacrimal duct into the nose. 01:01 This will present with redness and tearing and often excessive tearing, but the sclera typically looks normal. 01:08 This is more common in infants. 01:11 Again, antibiotics are really not necessary unless it spreads into a preseptal cellulitis. 01:17 I might use antibiotics in some of these cases. 01:20 And generally, warm compresses, once again, are the way to go for this, 10 minutes four times a day. 01:28 Moving on to conjunctivitis. 01:30 Conjunctivitis is an infection of the conjunctiva of the eyes. 01:36 So generally, this is what we typically call pink eye. 01:40 It’s usually caused by viruses. 01:42 It’s rare for this to be bacteria. 01:45 We really probably over treat this. 01:48 Viral is the most common entity and classically, we're taught if it’s one side, it’s bacterial or viral. 01:55 If it’s both, it’s bacterial or viral, that’s just not true. 01:58 It’s very hard to predict whether something is bacterial or viral, but generally they’re almost all viral. 02:04 A bacterial conjunctivitis is very severe with purulence and drainage. 02:09 So antibiotics are probably overused in substantial portion of patients with conjunctivitis. 02:15 Generally, watchful waiting is appropriate unless it’s bilateral and severe and then probably, we’ll start with some antibiotics. 02:22 It’s also highly contagious when it’s viral, so we recommend people avoid rubbing and touching their eyes as much as they can and washing their hands frequently. 02:33 If we are to cover with antibiotics, we can usually do topical drops, although rarely we may do something systemic like high dose amoxicillin. 02:43 There is one exception, actually a few exceptions in infants. 02:47 So infants, gonorrhea of the eye is common in infants who are born to mothers with active gonorrhea. 02:55 It generally will show up in two or three days and will be a very vigorous and aggressive bacterial conjunctivitis of the eye. 03:03 We can test it with a PCR of the eye, which then is sent to the lab, and they look for genetic material of the gonococcus. 03:11 This, we need to treat with ceftriaxone. 03:14 We need to admit these infants to the hospital and if treated, the prognosis is outstanding. 03:20 Chlamydia is a bit different than gonorrhea in the eye of infants. 03:25 While gonorrhea grows quickly and will show up in two to three days, chlamydia appears later in two to three weeks. 03:33 So any infant with a delay in eye response, two to three weeks of age, you have to worry about chlamydia. 03:40 Another alternative is they’re having a toxic reaction to some of the antimicrobial ion that was applied at birth that can also show up at two to three weeks. 03:50 To test, we do a PCR of the eye and then we will treat these infants with azithromycin. 03:58 The problem is this is sometimes hard to cure and it can recur. 04:02 This is a major cause of blindness worldwide in infants, so we just need to be aware of this, that if untreated, this can result in blindness or trachoma. 04:15 Another sexually transmitted infection for an infant that can be exposed in utero or it can also happen later on in life is HSV of the eye. 04:27 This typically in infants will present in the first month of life as skin, eye, mouth disease. 04:33 This, we have to aggressively treat. 04:35 We test it with an HSV culture, which grows very quickly, usually within a day. 04:41 For these infants, we will treat them with IV acyclovir for 14 days. 04:46 These infants really need to be hospitalized and an ophthalmologist should be consulted. 04:51 This can cause vision defects. 04:53 If you can see here, the eye is actually aggressively infected and if that infection goes over the area where the pupil is, you can have defects in vision. 05:04 So we really want to aggressively treat these infants. 05:10 Another thing you will see frequently which really isn't much of a problem is subconjunctival hemorrhage. 05:17 This is when patients have bleeding just under the conjunctiva. 05:22 It usually is caused by acute cough or sneeze or vomiting and it’s really just a little hemorrhage that can happen there. 05:29 It self-resolves and there’s really no therapy needed, but sometimes patients will show up and be worried about this. 05:37 This is an unusual one that we see really more often in the American Southwest which is caused by very dry or sunny climates. 05:48 This is called pterygium. 05:49 And this pterygium can grow out from the corners of the eye and very rarely can actually even obstruct vision, though usually they don’t and therapy is really usually unnecessary. 06:01 Usually, they’re asymptomatic. 06:04 If it grows into the field of vision, surgery may be indicated and you should consult an ophthalmologist. 06:11 Another one we see fairly frequently is the corneal abrasion. 06:15 This is in a differential diagnosis for a child who is crying and you can’t figure out why. 06:19 Sometimes, they just scratch their own eye or anyone who has had eye trauma. 06:24 Usually in older children that were called a trauma and you’re worried about it, the way you check for it is do a fluorescein exam. 06:31 So while the patient is looking away, you put some fluorescein drops in the eye and then you hold up a Wood’s lamp and if you see that fluorescein pulling over the eye, you know they had a corneal abrasion. 06:42 So it arises from direct eye trauma. 06:45 It’s painful and persistent and is usually worse with blinking. 06:49 They may have no exam finding without the fluorescein dye. 06:52 So you really have to do that fluorescein dye exam and that requires a little bit of practice, have someone show you how to do it. 06:59 The pain resolves usually in a day or two. 07:01 There’s really not much you need to do, although I do recommend following up with ophthalmology if the lesion goes over the pupil just to make sure the vision is okay. 07:10 Sometimes, folks will treat this with topical erythromycin just to prevent superinfection, although that’s very rare. 07:18 The clinical evidence behind this is not strong but it is often done in practice and provides lubrication to the eye. 07:25 This is a result of anterior chamber eye trauma. 07:30 So a hyphema is an acute bleed as a result of direct blunt force trauma to the eye in the anterior chamber of the eye. 07:39 And what you can see if you look carefully is this blood sort of layered out, about half way up the eye. 07:44 When you see that layering of blood, you know that’s a hyphema. 07:49 It usually happens right in front of the iris. 07:51 So it’s basically a result of direct trauma, say a baseball to the eye. 07:56 This is an orbital emergency and we generally want to call ophthalmology to get them to come and check things out. 08:04 The blood can interfere with drainage of fluid and result in glaucoma. 08:09 Generally, this is usually either in or outpatient treatment. 08:14 We used to treat them more inpatient, now more outpatient. 08:17 We do admit these infants and children if they’re expected poor compliance or if they have an underlying problem like sickle cell disease, which in general they do much worse with. 08:29 So, patients with sickle cell or patients where they're not likely to stay still and generally, we don’t want them running around too much with this. 08:36 And they often will recommend bed rest until it’s healed up. 08:42 So how do we treat it? We’ll put a shield patch over their eye and aminocaproic acid can reduce the incidence of rebleed. 08:52 You may need an inpatient experience for that because of the toxicity of the drug which causes nausea, vomiting or hypotension. 09:01 Sometimes, often, I will just recommend a topical steroid and dilating drops and they may or may not require glaucoma meds depending on how the blood is interfering with the drainage of the fluid from the anterior chamber of the eye. 09:16 So that’s my review of causes of red eye in children. 09:21 Thanks for your time.
About the Lecture
The lecture Red Eye and Orbital Trauma by Brian Alverson, MD is from the course Pediatric Emergency Medicine. It contains the following chapters:
- The Red Eye and Orbital Trauma
- Neonatal Conjunctivitis
- Pterygium
- Corneal Abrasion
- Hyphema
Included Quiz Questions
Where does blood collect in a patient with a hyphema?
- The anterior chamber
- The iris
- The conjunctivae
- The retina
- The vitreous
A 12-year-old child is diagnosed with acute blepharitis. Which of the following is the most appropriate treatment at this point in time?
- Warm compresses
- Cryotherapy
- Incision and drainage
- Antibiotics
- Acyclovir
A 10-year-old girl presents with excessive tearing of her right eye. Physical examination shows erythema over the medial lacrimal punctum of the ipsilateral eyelid. What is the most likely diagnosis?
- Dacryocystitis
- Chalazion
- Hordeolum
- Conjunctivitis
- Trachoma
A toddler is brought to the physician because of red eyes for 2 days and is diagnosed with mild bilateral conjunctivitis. Physical examination is otherwise normal. Which of the following is the most appropriate next step in management?
- Watchful waiting
- Systemic antibiotics
- Topical antibiotics
- Systemic acyclovir
- Topical acyclovir
A neonate is diagnosed with gonorrheal conjunctivitis. Which of the following is the most appropriate antibiotic treatment for this patient?
- Intravenous ceftriaxone
- Topical eythromycin
- Intravenous vancomycin
- Oral erythromycin
- Topical ciprofloxacin
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |