Playlist
Show Playlist
Hide Playlist
Pemphigus Vulgaris
-
Slides Dermatology Inflammatory Skin Diseases.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
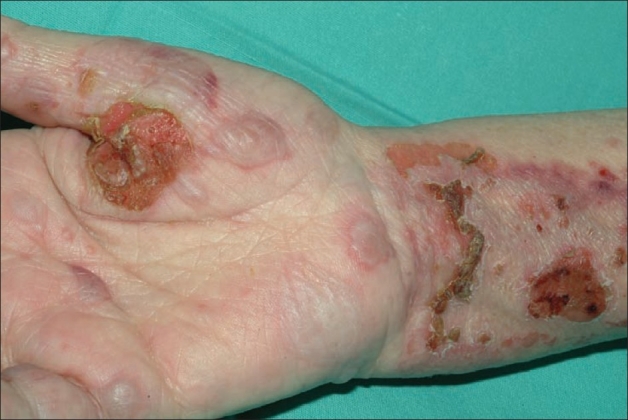
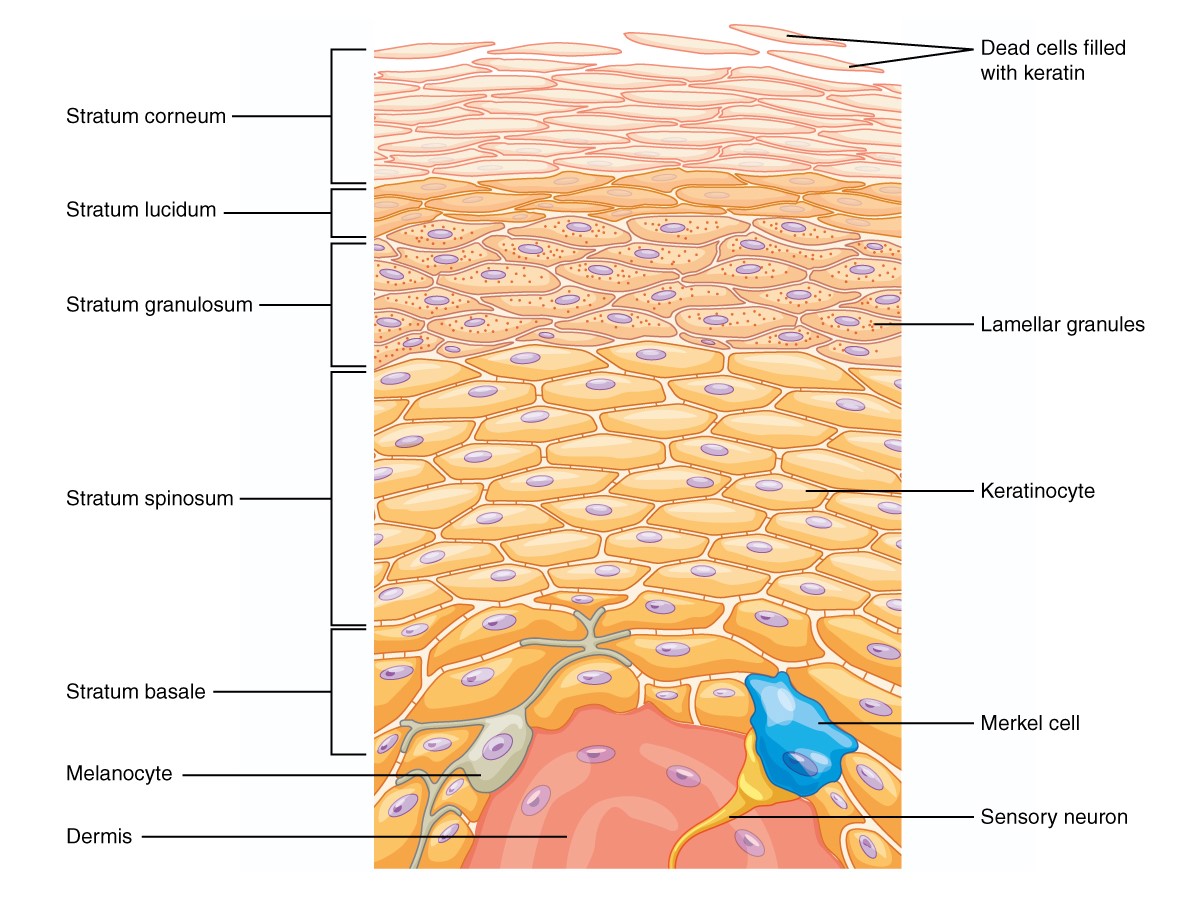
00:01 Our topic here is pemphigus vulgaris. 00:04 I want you to hone in on vulgar. 00:09 Why? Because there are two conditions that I’m going to walk you through, and students tend to get this confused, but not any longer because you’re with me. 00:18 And the two conditions include pemphigus vulgaris, and then subsequently, I’m going to walk you through bullous pemphigoid. 00:27 Of these two, which ones are more dangerous? So, pemphigus vulgaris is the one that has an increased risk of killing you. 00:37 So therefore, increased risk of mortality. 00:40 And we talked about the skin, where if you took a tongue depressor and you scrape the skin, there’s one condition in which the skin would remain intact, there’s one in which it would then come right off, split. 00:54 Could you imagine as to how, perhaps, traumatic that would be for the patient? So guess which one this would be in which skin would then come off. 01:04 Pemphigus vulgaris. 01:07 Why do students get this confused? It’s this point. 01:11 In other words, the pathogenesis or the etiology. 01:15 Both are type 2 hypersensitivities. 01:18 What does that mean to you? It means that the antibodies are then -- autoantibodies are attacking a particular target or protein. 01:28 What you need to memorize is which protein is involved and which type of disease as being a target for that particular IgG. 01:36 In pemphigus vulgaris, it is the skin which is then being scraped off. 01:40 It’s the vulgar, dangerous one. 01:43 I’ll tell you what this means. 01:44 It means acantholysis, and we call this positive Nikolsky′s sign. 01:50 That’s to come. 01:52 So now, you start thinking about the two different junctions or two different bridges. 01:58 The one bridge is going to be the one that then connects one keratinocyte to another. 02:04 And then you have another bridge which is then going to connect the dermis with the epidermis. 02:10 I’ll tell you right now, it’s the one that we’re focusing upon in vulgaris in which it’s connecting one keratinocyte to another. 02:17 And this, ladies and gentlemen, please focus on desmo-, desmo-, desmosome. 02:23 You see anything about desmoglein, desmosome, or perhaps even the family of E-cadherin. 02:32 Remember that way back when in neoplasia. 02:35 These are the bridges that you want to keep in mind between keratinocyte to keratinocyte, or from cell to cell. 02:42 Your focus here will be on desmosome. 02:45 If you lose this bridge, in other words, the function of the desmosome hasn’t been compromised due to bombing taking place by these IgGs attacking it. 02:56 If the desmosomes are gone, then what do you think the fate of the keratinocyte is? Comes right off. 03:05 Scary. 03:07 Autoimmune antibody-mediated attack on desmosome, a type 2 hypersensitivity. 03:12 The desmosomes are the ones that are the bridge or allow for the keratinocyte to -- I don’t want to say communicate -- attach or anchor through the other keratinocyte. 03:22 If this is gone, then therefore, as is the epidermis. 03:27 There is the foundation that you want to know for vulgaris, and I’ll quickly describe to you, bullous pemphigoid. 03:34 Spend a minute, make sure you repeat me a few times to make sure that you comprehend everything that I just delivered. 03:44 Vulgaris, demographics, who is it? Where do you see it? Often seen in middle-aged men and women. 03:52 Usually presents first in the oral mucosa. 03:54 Isn’t that dangerous? So yes, within your mouth, you can have pemphigus vulgaris resulting in the same issue, attacking the desmosome, so therefore, the integrity of your mucosa has now been compromised. 04:09 The loss of the keratinocyte adhesion yields superficial blisters. 04:14 Stop. 04:16 Both of these are going to have blisters. 04:18 What do you mean both? Pemphigus vulgaris and the other one, bullous pemphigoid. 04:23 Are there other variants? Of course, there are, but I have to at least give you the foundation and the fundamentals so that you know at least what you’re working with. 04:32 Both of these conditions are going to give you blisters, but the blister that we then call in bullous pemphigoid are bullae, right? Bullae, bullous pemphigoid. 04:43 Now, blisters here, pay attention to description, are going to be superficial. 04:49 A blister is not as big as bullae, but yet, which condition is vulgar? Uh-huh, good! Pemphigus vulgaris. 04:57 So, loss of keratinocyte adhesion will then yield a fluid-filled structure which we then call a superficial blister. 05:05 Guess what, it will easily rupture. 05:08 This description is not the case with bullous pemphigoid. 05:12 Let’s continue. 05:16 What are we looking for? Superficial blisters. 05:18 Where? Everywhere up and down the body, huh? You have keratinocytes in your skin everywhere. 05:23 It is the biggest organ that we have in our body, for Pete’s sakes. 05:26 So, scalp, face, trunk, arm, groin, whatever. 05:30 The point is wherever this problem occurs, everywhere, we have loss of integrity of either the mucosa or the epidermis. 05:40 Pemphigus vulgaris, if you were to take a look at this picture here, you have superficial blisters. 05:45 And then what happens on your right is that histologically, if you will take a section, literally, you'll find that the keratinocytes are going to come right off. 05:55 And when they do so, what is the bottom most layer of your epidermis? I’m sorry, what did you say? Good. 06:02 Basale. 06:04 So, say that you have your stratum basale, your stratum basale which is left behind after the skin is scraped off. 06:15 It looks like a row of tombstones. 06:20 A row of tombstones. 06:23 So for example, if you were to bury the dead, and then maybe perhaps, you’re going to leave behind a tombstone, and that’s what the stratum basale is going to look like once your skin comes right off. 06:36 Keep that in mind. 06:37 This is the vulgar disease. 06:41 Management: Well, you want to try to mitigate effect of the autoantibodies. 06:48 Think of immunosuppressant agents.
About the Lecture
The lecture Pemphigus Vulgaris by Carlo Raj, MD is from the course Inflammatory Skin Diseases.
Included Quiz Questions
Autoantibodies to desmogleins, integral structures for cell-to-cell adhesion, cause intraepithelial cleavage with acantholysis (detached keratinocytes) primarily localized to the suprabasal region. This is a histopathologic description of which of the following conditions?
- Pemphigus vulgaris
- Bullous pemphigoid
- Stevens-Johnson syndrome
- Toxic epidermal necrolysis
- Erythema marginatum
Pemphigus vulgaris is classified as which of the following types of hypersensitivity reactions?
- Type II
- Type I
- Type III
- Type IV
- Type V
Which of the following statements regarding pemphigus vulgaris is FALSE?
- It primarily affects children.
- The bullae of pemphigus vulgaris are more fragile than those of bullous pemphigoid.
- It is characterized by intraepidermal acantholysis.
- IgG autoantibodies detect desmosomes as antigens.
- Oral mucosa is often involved.
Which of the following histological features is most characteristic of pemphigus vulgaris?
- Retention of basal keratinocytes along the basement membrane zone, resembling a "row of tombstones"
- Antibodies deposited at the dermal-epidermal junction
- Linear eosinophilic deposition
- Subepidermal blisters with eosinophil-rich infiltrate
- Damage to hemidesmosomes
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Taken lot of effort to explain the details of the topic and to make us understand the difference between the two conditions: pemphigous vulgaris and bullous pemphigoid. it was a beautiful lecture.....