Playlist
Show Playlist
Hide Playlist
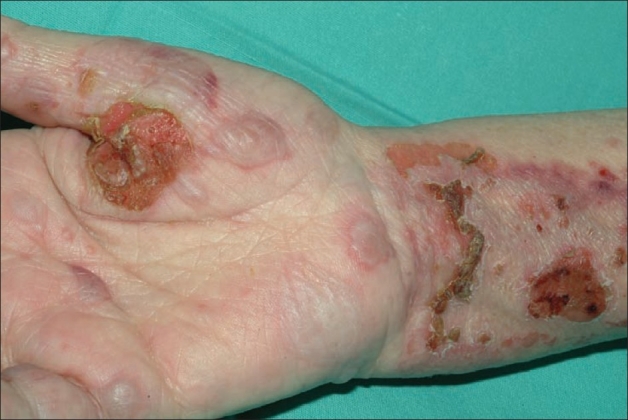
Pemphigus Vulgaris
-
Slides Bullous Diseases.pdf
-
Reference List Dermatology.pdf
-
Download Lecture Overview
00:02 Next up, pemphigus vulgaris. So, pemphigus vulgaris, in contrast to bullous pemphigoid. 00:08 It's important to try and make sure we separate those 2 disease process. 00:11 Pemphigus vulgaris, much more significant, and potentially can be a fatal disease process. 00:17 Both of them are autoimmune diseases, but where the immune-mediated attack occurs is very important. 00:24 It's most common in somewhat younger ages, those 40-60 years of age, with an equal predilection for men and for women. 00:32 And it is essentially caused by anti-desmoglein IgG antibodies that are attacking the keratinocytes within the epidermis. 00:41 So, since the epidermis itself is being attacked, it's going to break up and be thin, and for that reason, you're going to have fragile, flaccid bullae on normal skin. Oftentimes, when a patient presents, you may not see any bullae whatsoever, even though this is a lecture about bullous diseases, the bullae are so thin-walled that they're very prone to rupture before you even see the patient. 01:01 These lesions are painful, they may be bleeding and definitely, you're going to have a positive Nikolsky sign by just, again, rubbing that skin. You'll see the skin slough right off. 01:10 Extensive mucosal involvement, just like we saw with Stevens-Johnson syndrome. 01:15 Patients may report odynophagia, pain with swallowing, epistaxis, through the nosebleeds and these ulcerative lesions within the nasopharynx, conjunctiva may be involved. 01:27 And as you might imagine, this can be complicated by secondary infections. 01:31 Malnutrition can occur, mostly because they have trouble eating due to all that discomfort if they don't get some parenteral nutrition. 01:37 If you were to biopsy any one of these lesions, and that is often recommended to ensure that you've got the right diagnosis, you'll see acantholysis, which just simply means separation and well, peeling apart of the different keratinocytes in the skin. 01:52 Immunofluorescence will identify those anti-desmoglein immunoglobulins that I mentioned. Again, you'll find them right within the epidermis rather than at the epidermis-dermis junction. 02:03 And of course, with this disease since it is such a severe disease with a relatively high fatality rate, you're going to have to send that person to a specialized burn unit where they can really manage all those potential complications of having your skin not functioning. 02:17 They're oftentimes treated with high-dose IV glucocorticoids, along with rituximab at least initially, to control the disease process, and then over time, you may add on some steroid-sparing agents such as azathioprine or mycophenolate mofetil.
About the Lecture
The lecture Pemphigus Vulgaris by Stephen Holt, MD, MS is from the course Allergic and Immune-mediated Skin Disorders.
Included Quiz Questions
Which of the following is true regarding pemphigus vulgaris?
- Immunofluorescence microscopy shows IgG antidesmoglein antibodies.
- Light microscopy shows a thickening of the stratum corneum.
- Mucous membrane involvement is not commonly observed in patients with pemphigus vulgaris.
- It is caused by T-cell–mediated keratinocyte destruction.
- It is more common in patients older than 60 years.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |